Abstract
Background
Obesity is a chronic complex disease, consequence of an unbalance between energy intake and expenditure and of the interaction between predisposing genotype and facilitating environmental factors. The aim of the study was to evaluate body composition, abdominal fat, and metabolic changes in a group of severely obese patients before and after laparoscopic gastric bypass (LGBP) at standardized (10% and 25%) total weight loss.
Methods
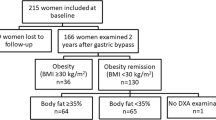
Twenty-eight patients (14 M, 14 F; age 41.71 ± 6.9 years; body mass index (BMI) 49.76 ± 5.8 kg/m2) were treated with laparoscopic gastric bypass. All evaluations before surgery and after achieving ~10% and ~25% weight loss (WL). Body composition was assessed by bioimpedance analysis; resting metabolic rate (RMR) was measured by indirect calorimetry.
Results
Body weight, BMI, and waist circumference significantly decreased at 10% and 25% WL. We observed a significant reduction of both RMR (2,492 ± 388 at entry vs. 2,098 ± 346.6 at 10% WL vs. 2,035 ± 312 kcal per 24 h at 25% WL, p = 0.001 vs. baseline) as well as of RMR corrected for fat-free mass (FFM; 35.7 ± 6.7 vs. 34.9 ± 9.0 at 10% WL vs. 33.5 ± 5.4 at 25% WL kilocalorie per kilogram FFM × 24 h, p = 0.041 vs. baseline). Body composition analysis showed a relative increase in FFM and a reduction of fat mass at 25% WL. A significant reduction in blood glucose, insulin, homeostasis model assessment index was observed. Ultrasonography showed a marked decrease in the signs of hepatic steatosis.
Conclusion
In conclusion, our study confirms that LGBP is a safe procedure in well-selected severely obese patients and has early favorable effects on both metabolic parameters and body composition. Longer-term observations are required for in-depth evaluation of body composition changes.
Similar content being viewed by others
References
Renehan AG, Tyson M, Egger M, et al. Body mass index and incidence of cancer: a systematic review and metabolic prospective observational studies. Lancet. 2008;371:569–78.
Hsu IR, Kim SP, Kabir M, et al. Metabolic syndrome, hyperinsulinemia, and cancer. Am J Clin Nutr. 2007;86:867–71.
Olshansky SY, Passaro DJ, Hershow RC, et al. A potential decline in life expectancy in the United States in the 21st century. N Engl J Med. 2005;352(11):1138–45.
Hamilton MT, Hamilton DG, Zderic TW. Role of low energy expenditure and sitting in obesity, metabolic syndrome, type 2 diabetes, and cardiovascular disease. Diabetes. 2007;56:2655–67.
Contaldo F, Pasanisi F, Finelli C, et al. Obesity, heart failure and sudden death. Nutr Metab Cardiovasc Dis. 2002;12(4):190–7.
Marchesini G, Bugianesi E, Forlani G, et al. Nonalcoholic fatty liver, steatohepatitis, and the metabolic syndrome. Hepatology. 2003;37:917–23.
Bugianesi E, Leone N, Vanni E, et al. Expanding the natural history of nonalcoholic steatohepatitis: from cryptogenic cirrhosis to hepatocellular carcinoma. Gastroenterology. 2002;123:134–40.
Colicchio P, Tarantino G, del Genio F, et al. Nonalcoholic fatty liver disease in young adult severely obese non-diabetic patients in South Italy. Ann Nutr Metab. 2005;49:289–95.
Stampfer MJ, Maclure KM, Colditz GA, et al. Risk of symptomatic gallstones in women with severe obesity. Am J Clin Nutr. 1992;55:652–8.
NIH. Third report of the National Cholesterol Education Program Expert Panel (Adult Treatment Panel III). Bethesda: NIH Publication; 2001. p. 01-3670.
Bedogni G, Bellentani S, Miglioli L, et al. The Fatty Liver Index: a simple and accurate predictor of hepatic steatosis in the general population. BMC Gastroenterol. 2006;6:33.
del Genio F, Alfonsi L, Marra M, et al. Metabolic and nutritional status changes after 10% weight loss in severely obese patients treated with laparoscopic surgery vs integrated medical treatment. Obes Surg. 2007;17(12):1592–8.
Saverymuttu SH, Joseph AEA, Maxwell JA. Ultrasound scanning in the detection of hepatic fibrosis and steatosis. Br Med J. 1986;292:13–5.
Ricci C, Longo R, Gioulis E, et al. Noninvasive in vivo quantitative assessment of fat content in human liver. J Hepatol. 1997;27:108–13.
Osawa H, Mori Y. Sonographic diagnosis of fatty liver using a histogram technique that compares liver and renal cortical amplitude. J Clin Ultrasound. 1996;24:25–9.
Ribeiro-Filho FF, Faria AN, Azjen S, et al. Methods of estimation of visceral fat: advantages of ultrasonography. Obes Res. 2003;11:1488–94.
Cignarelli M, DePergola G, Picca G, et al. Relationship of obesity and body fat distribution with ceruloplasmin serum levels. Int J Obes Relat Metab Disord. 1996;20:809–13.
Targher G, Tonoli M, Agostino G, et al. Ultrasonographic intra-abdominal depth and its relation to haemostatic factors in healthy males. Int J Obes Relat Metab Disord. 1996;20:882–5.
Rissanen P, Makimattila S, Vehmas T, et al. Effect of weight loss and regional fat distribution on plasma leptin concentration in obese women. Int J Obes Relat Metab Disord. 1999;23:645–9.
Kinoshita T, Ittoh M. Longitudinal variance of fat mass deposition during pregnancy evaluated by ultrasonography: the ratio of visceral fat to subcutaneous fat in the abdomen. Gynecol Obstet Invest. 2006;61(2):115–8.
Anonymous. Gastrointestinal surgery for severe obesity: National institutes of health consensus development conference draft statement. Obes Surg. 1991;1:257–65.
Buchwald H, Williams SE. Bariatric surgery worldwide 2003. Obes Surg. 2004;14(9):1157–64.
Sjöström L, Narbro K, Sjöström CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52.
Harris ML, Flegal KM, Cowie LL, et al. Prevalence of diabetes, impaired fasting glucose, and impaired glucose tolerance in US adults: the Third National Health and Nutrition Examination Survey 1988–94. Diabetes Care. 1998;21:518–24.
Colditz GA, Willet WC, Rotnitky A, et al. Weight gain as a risk factor for clinical diabetes in women. Ann Intern Med. 1995;122:481–6.
Pories WJ, Swanson MS, MacDonald KG, et al. Who would have thought it? An operation proves to be the most effective therapy for adult-onset diabetes mellitus. Ann Surg. 1995;222(3):339–50.
Despres JP. The insulin-resistance-dyslipidemic syndrome of visceral obesity: effect on patient’s risk. Obes Rev. 1998;6(1):8–17.
Rubino F, Gagner M, Gentileschi P, et al. The early effect of the Roux-en-Y gastric bypass on hormones involved in body weight regulation and glucose metabolism. Ann Surg. 2004;240:236–42.
Hoene M, Weigert C. The role of interleukin-6 in insulin-resistance, body fat distribution and energy balance. Obes Rev. 2008;9:20–9.
Benedetti G, Mingrone G, Marcoccia S, et al. Body composition and energy expenditure after weight loss following bariatric surgery. J Am Coll Nutr. 2000;19:270–4.
Carey DG, Pliego GJ, Raymond RL. Body composition and metabolic changes following bariatric surgery: effects on fat mass, lean mass and basal metabolic rate: six months to one-year follow-up. Obes Surg. 2006;16:1602–8.
de Boer JO, van Es AJH, Roovers LCA, et al. Adaptation of energy metabolism of overweight women to low-energy intake, studied with whole body calorimeters. Am J Clin Nutr. 1986;44:585–95.
Kushner RF, Schoeller DA, Field CR, et al. Is the impedance index (ht2/R) significant in predicting total body water? Am J Clin Nutr. 1992;56(5):835–9.
Marra M, Caldara A, Montagnese C, et al. Bioelectrical impedance phase angle in constitutionally lean females, ballet dancers and patients with anorexia nervosa. Eur J Clin Nutr. 2008; in press
Armellini F, Zamboni M, Rigo L, et al. The contribution of sonography to the measurement of intra abdominal fat. J Clin Ultrasound. 1990;18:563–7.
Vlachos IS, Hatziioannou A, Perelas A, et al. Sonographic assessment of regional adiposity. Am J Roentgenol. 2007;189:1545–53.
Koda M, Senda M, Kamba M, et al. Sonographic subcutaneous and visceral fat indices represent the distribution of body fat volume. Abdom Imaging. 2007;32:387–92.
Armellini F, Zamboni M, Robbi R, et al. Total and intra-abdominal fat measurements by ultrasound and computerized tomography. Int J Obes Relat Metab Disord. 1993;17:209–14.
Tornaghi G, Raiteri R, Pozzato C, et al. Anthropometric or ultrasonic measurements in assessment of visceral fat? A comparative study. Int J Obes Relat Metab Disord. 1994;18:771–5.
Abe T, Kawakami Y, Sugita M, et al. Use of B-mode ultrasound for visceral fat mass evaluation: comparisons with magnetic resonance imaging. Appl Human Sci. 1995;14:133–9.
Pontiroli AE, Pizzocri P, Giacomelli M, et al. Ultrasound measurement of visceral and subcutaneous fat in morbidly obese patients before and after laparoscopic adjustable gastric banding: comparison with computerized tomography and with anthropometric measurements. Obes Surg. 2002;12:648–51.
Stolk RP, Meijer R, Mali WP, et al. Ultrasound measurements of intra abdominal fat estimate the metabolic syndrome better than do measurements of waist circumference. Am J Clin Nutr. 2003;77:857–60.
Minocci A, Savia G, Lucantoni R, et al. Leptin plasma concentrations are dependent on body fat distribution in obese patients. Int J Obes Relat Metab Disord. 2000;24:1139–44.
Ribeiro-Filho FF, Faria AN, Kohlmann O Jr, et al. Ultrasonography for the evaluation of visceral fat and cardiovascular risk. Hypertension. 2001;38:713–7.
Kim SK, Kim HJ, Hur KY, et al. Visceral fat thickness measured by ultrasonography can estimate not only visceral obesity but also risks of cardiovascular and metabolic diseases. Am J Clin Nutr. 2004;79:593–9.
Leite CC, Wajchenberg BL, Radominski R, et al. Intra-abdominal thickness by ultrasonography to predict risk factors for cardiovascular disease and its correlation with anthropometric measurements. Metab. 2002;51:1034–40.
Busetto L, Tregnaghi A, De Marchi F, et al. Liver volume and visceral obesity in women with hepatic steatosis undergoing gastric banding. Obes Res. 2002;10(5):408–11.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
del Genio, F., del Genio, G., De Sio, I. et al. Noninvasive Evaluation of Abdominal Fat and Liver Changes Following Progressive Weight Loss in Severely Obese Patients Treated with Laparoscopic Gastric Bypass. OBES SURG 19, 1664–1671 (2009). https://doi.org/10.1007/s11695-009-9891-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-009-9891-x