Abstract
Background
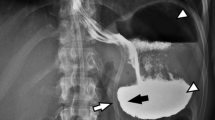
Laparoscopic adjustable gastric banding (LAGB) has commonly been complicated by the problem of band slippage or prolapse. Since popularization of the pars flaccida approach and improved anterior fixation, it is our impression that the problem of symmetrical dilatation of the proximal gastric pouch has become more important.
Methods
We have reviewed the results of a series of 425 LAGB all performed by the pars flaccida approach from June 2003 to October 2007 to analyze the incidence and implications of this new pattern.
Results
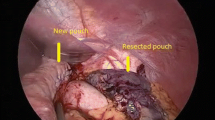
There were no posterior prolapses, 2 anterior prolapses, and 17 cases of symmetrical pouch dilatation (SPD) (revision rate 4.4%). Teenage patients had a 22% revision rate for SPD. All revisions were completed laparoscopically with no mortality, no significant complications, and a median hospital stay of 1 day. The median weight loss following revisional surgery was not significantly different from the background cohort.
Conclusion
SPD is the most common reason for revision of LAGB in this series. We postulate that SPD is caused by excessive pressure in the proximal gastric pouch. This may be generated either by eating too quickly or too large a volume or excessive tightening of the band. The radial forces in the pouch may ultimately cause pressure on the phrenoesophageal ligament and a secondary hiatal hernia.



Similar content being viewed by others
References
O’Brien PE, McPhail T, Chaston TB, Dixon JB. Systematic review of medium-term weight loss after bariatric operations. Obes Surg. 2006;16(8):1032–40.
Chapman AE, Kiroff G, Game P, et al. Laparoscopic adjustable gastric banding in the treatment of obesity: a systematic literature review. Surgery. 2004;135(3):326–51.
Allen JW. Laparoscopic gastric band complications. Med Clin North Am. 2007;91(3):485–97, xii.
Gagner M, Gentileschi P, de Csepel J, et al. Laparoscopic reoperative bariatric surgery: experience from 27 consecutive patients. Obes Surg. 2002;12(2):254–60.
Suter M, Bettschart V, Giusti V, et al. A 3-year experience with laparoscopic gastric banding for obesity. Surg Endosc. 2000;14(6):532–6.
O’Brien PE, Brown WA, Smith A, et al. Prospective study of a laparoscopically placed, adjustable gastric band in the treatment of morbid obesity. Br J Surg. 1999;86(1):113–8.
Fielding GA, Allen JW. A step-by-step guide to placement of the LAP-BAND adjustable gastric banding system. Am J Surg. 2002;184(6B):26S–30S.
O’Brien PE, Dixon JB, Laurie C, Anderson M. A prospective randomized trial of placement of the laparoscopic adjustable gastric band: comparison of the perigastric and pars flaccida pathways. Obes Surg. 2005;15(6):820–6.
Sherwinter DA, Powers CJ, Geiss A, et al. Posterior prolapse: an important entity even in the modern age of the pars flaccida approach to lap-band placement. Obes Surg. 2006;16(10):1312–7.
Elias BB, Staudt JP, Van Vyne EE. The technical approach in banding to avoid pouch dilatation. Obes Surg. 2001;11(3):311–4.
Ren CJ, Horgan S, Ponce J. US experience with the LAP-BAND system. Am J Surg. 2002;184(6B):46S–50S.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brown, W.A., Burton, P.R., Anderson, M. et al. Symmetrical Pouch Dilatation After Laparoscopic Adjustable Gastric Banding: Incidence and Management. OBES SURG 18, 1104–1108 (2008). https://doi.org/10.1007/s11695-008-9485-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-008-9485-z