Abstract
Summary
Despite the significant improvements in the management of thalassemia, there are growing concerns regarding their long-term complications. We showed that low bone mass is one of the most prevalent complications among these patients. Insufficient physical activity and hypogonadism are the main possible associated factors followed by DM and insufficient sun exposure.
Purpose
Despite the significant improvements in the management of transfusion-dependent thalassemia (TDT), there are growing concerns regarding their long-term complications.
Methods
This cross-sectional study included 615 TDT patients who were registered and followed in a comprehensive thalassemia clinic in Southern Iran. We measured serum biochemical tests and bone mineral density in all patients. We recorded physical activity and sun exposure subjectively, and an endocrinologist visited and examined all the patients. A group of age- and gender-matched healthy volunteers participated in the study as the control group.
Results
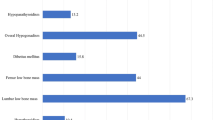
The mean age of the studied population was 28.4 ± 7.7 years, and 55.8% were female. The prevalence of vitamin D deficiency was 45.6% and 54.4% in TDT patients and the control group. A portion of TDT patients suffered from different endocrinopathies, which included hypogonadism (49.8%), diabetes mellitus (17.2%), hypoparathyroidism (14.6%), and hypothyroidism (6.3%). The prevalence of low bone mass in patients with TDT was 48.3 and 74.6% in the femoral and lumbar bones, respectively. Low physical activity, insufficient sun exposure, diabetes mellitus, and hypogonadism were associated with low bone mass.
Conclusion
Low bone mass is highly prevalent among TDT patients in Southern Iran. Insufficient physical activity and hypogonadism are the main possible associated factors, followed by DM and insufficient sun exposure.
Similar content being viewed by others
Data availability
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
References
Bordbar M, Haghpanah S, Zekavat OR, Saki F, Bazrafshan A, Bozorgi H (2019) Effect of different iron chelation regimens on bone mass in transfusion-dependent thalassemia patients. Expert Rev Hematol 12(11):997–1003
Gaudio A, Morabito N, Catalano A, Rapisarda R, Xourafa A, Lasco A (2019) Pathogenesis of thalassemia major-associated osteoporosis: a review with insights from clinical experience. J Clin Res Pediatr Endocrinol 11(2):110–117
Bordbar M, Bozorgi H, Saki F, Haghpanah S, Karimi M, Bazrafshan A, Zekavat OR (2019) Prevalence of endocrine disorders and their associated factors in transfusion-dependent thalassemia patients: a historical cohort study in Southern Iran. J Endocrinol Investig 42(12):1467–1476
De Sanctis V, Soliman AT, El-Hakim I, Christou S, Mariannis D, Karimi M et al (2019) Marital status and paternity in patients with transfusion-dependent thalassemia (TDT) and non transfusion-dependent thalassemia (NTDT): an ICET - a survey in different countries. Acta Biomed 90(3):225–237
Dede AD, Trovas G, Chronopoulos E, Triantafyllopoulos IK, Dontas I, Papaioannou N, Tournis S (2016) Thalassemia-associated osteoporosis: a systematic review on treatment and brief overview of the disease. Osteoporos Int 27(12):3409–3425
Voskaridou E, Terpos E (2004) New insights into the pathophysiology and management of osteoporosis in patients with beta thalassaemia. Br J Haematol 127(2):127–139
De Sanctis V, Soliman AT, Canatan D, Tzoulis P, Daar S, Di Maio S et al (2019) An ICET-a survey on occult and emerging endocrine complications in patients with beta-thalassemia major: conclusions and recommendations. Acta Biomed 89(4):481–489
Tzoulis P, Ang AL, Shah FT, Berovic M, Prescott E, Jones R, Barnard M (2014) Prevalence of low bone mass and vitamin D deficiency in beta-thalassemia major. Hemoglobin. 38(3):173–178
Anapliotou ML, Kastanias IT, Psara P, Evangelou EA, Liparaki M, Dimitriou P (1995) The contribution of hypogonadism to the development of osteoporosis in thalassaemia major: new therapeutic approaches. Clin Endocrinol 42(3):279–287
Chatterjee R, Katz M (2000) Reversible hypogonadotrophic hypogonadism in sexually infantile male thalassaemic patients with transfusional iron overload. Clin Endocrinol 53(1):33–42
Scacchi M, Danesi L, Cattaneo A, Valassi E, Pecori Giraldi F, Argento C et al (2008) Bone demineralization in adult thalassaemic patients: contribution of GH and IGF-I at different skeletal sites. Clin Endocrinol 69(2):202–207
Lasco A, Morabito N, Gaudio A, Crisafulli A, Meo A, Denuzzo G, Frisina N (2002) Osteoporosis and beta-thalassemia major: role of the IGF-I/IGFBP-III axis. J Endocrinol Investig 25(4):338–344
De Sanctis V, Soliman AT, Canatan D, Elsedfy H, Karimi M, Daar S et al (2018) An ICET- a survey on hypoparathyroidism in patients with thalassaemia major and intermedia: a preliminary report. Acta Biomed 88(4):435–444
Voskaridou E, Terpos E (2008) Pathogenesis and management of osteoporosis in thalassemia. Pediatr Endocrinol Rev 6(Suppl 1):86–93
Skordis N, Efstathiou E, Kyriakou A, Toumba M (2008) Hormonal dysregulation and bones in thalassaemia--an overview. Pediatr Endocrinol Rev 6(Suppl 1):107–115
De Sanctis V, Pinamonti A, Di Palma A, Sprocati M, Atti G, Gamberini MR et al (1996) Growth and development in thalassaemia major patients with severe bone lesions due to desferrioxamine. Eur J Pediatr 155(5):368–372
Terpos E, Voskaridou E (2010) Treatment options for thalassemia patients with osteoporosis. Ann N Y Acad Sci 1202:237–243
Johanson NA (1990) Musculoskeletal problems in hemoglobinopathy. Orthop Clin North Am 21(1):191–198
Origa R, Fiumana E, Gamberini MR, Armari S, Mottes M, Sangalli A et al (2005) Osteoporosis in beta-thalassemia: clinical and genetic aspects. Ann N Y Acad Sci 1054:451–456
Al-Agha AE, Bawahab NS, Nagadi SA, Alghamdi SA, Felemban DA, Milyani AA (2020) Endocrinopathies complicating transfusion-dependent hemoglobinopathy. Saudi Med J 41(2):138–143
Abbasi S, Asl JF, Zadeh LM, Mirdoraghi M (2018) Measurement bone mineral density (BMD) of patients with beta thalassemia. Data Brief 19:1021–1024
Larijani B, Moayyeri A, Keshtkar AA, Hossein-Nezhad A, Soltani A, Bahrami A, Omrani GH, Rajabian R, Nabipour I (2006) Peak bone mass of Iranian population: the Iranian Multicenter Osteoporosis Study. J Clin Densitom 9(3):367–374
Pellegrino F, Zatelli MC, Bondanelli M, Carnevale A, Cittanti C, Fortini M, Gamberini MR, Giganti M, Ambrosio MR (2019) Dual-energy X-ray absorptiometry pitfalls in thalassemia major. Endocrine. 12:1–4
Bozzola M, Bozzola E, Montalbano C, Stamati FA, Ferrara P, Villani A (2018) Delayed puberty versus hypogonadism: a challenge for the pediatrician. Ann Pediatr Endocrinol Metab 23(2):57–61
Kennel KA, Drake MT, Hurley DL (2010) Vitamin D deficiency in adults: when to test and how to treat. Mayo Clin Proc 85(8):752–757 quiz 7-8
Baldini M, Forti S, Orsatti A, Ulivieri FM, Airaghi L, Zanaboni L, Cappellini MD (2014) Bone disease in adult patients with beta-thalassaemia major: a case-control study. Intern Emerg Med 9(1):59–63
Karimi M, Ghiam AF, Hashemi A, Alinejad S, Soweid M, Kashef S (2007) Bone mineral density in beta-thalassemia major and intermedia. Indian Pediatr 44(1):29–32
Valizadeh N, Farrokhi F, Alinejad V, Said Mardani S, Valizadeh N, Hejazi S et al (2014) Bone density in transfusion dependent thalassemia patients in Urmia, Iran. Iran J Ped Hematol Oncol 4(2):68–71
Meena MC, Hemal A, Satija M, Arora SK, Bano S (2015) Comparison of bone mineral density in thalassemia major patients with healthy controls. Adv Hematol 2015:648349
Naithani R, Seth T, Tandon N, Chandra J, Pati H, Saxena R, Choudhry VP (2018) Fractures and low bone mineral density in patients with beta thalassemia major. Indian J Hematol Blood Transfus 34(1):163–165
Aslan I, Canatan D, Balta N, Kacar G, Dorak C, Ozsancak A et al (2012) Bone mineral density in thalassemia major patients from Antalya, Turkey. Int J Endocrinol 2012:573298
Benigno V, Bertelloni S, Baroncelli GI, Bertacca L, Di Peri S, Cuccia L et al (2003) Effects of thalassemia major on bone mineral density in late adolescence. J Pediatr Endocrinol Metab 16(Suppl 2):337–342
Vogiatzi MG, Macklin EA, Fung EB, Cheung AM, Vichinsky E, Olivieri N, Kirby M, Kwiatkowski JL, Cunningham M, Holm IA, Lane J, Schneider R, Fleisher M, Grady RW, Peterson CC, Giardina PJ, for the Thalassemia Clinical Research Network (2009) Bone disease in thalassemia: a frequent and still unresolved problem. J Bone Miner Res 24(3):543–557
Mohkam M, Shamsian BS, Gharib A, Nariman S, Arzanian MT (2008) Early markers of renal dysfunction in patients with beta-thalassemia major. Pediatr Nephrol 23(6):971–976
Chan YL, Pang LM, Chik KW, Cheng JC, Li CK (2002) Patterns of bone diseases in transfusion-dependent homozygous thalassaemia major: predominance of osteoporosis and desferrioxamine-induced bone dysplasia. Pediatr Radiol 32(7):492–497
Fung EB, Xu Y, Kwiatkowski JL, Vogiatzi MG, Neufeld E, Olivieri N et al (2010) Relationship between chronic transfusion therapy and body composition in subjects with thalassemia. J Pediatr 157(4):641–647 7 e1-2
Baldini M, Forti S, Marcon A, Ulivieri FM, Orsatti A, Tampieri B, Airaghi L, Zanaboni L, Cappellini MD (2010) Endocrine and bone disease in appropriately treated adult patients with beta-thalassemia major. Ann Hematol 89(12):1207–1213
Trachtenberg F, Foote D, Martin M, Carson S, Coates T, Beams O et al (2010) Pain as an emergent issue in thalassemia. Am J Hematol 85(5):367–370
Dede AD, Tournis S, Dontas I, Trovas G (2014) Type 2 diabetes mellitus and fracture risk. Metabolism. 63(12):1480–1490
Vogiatzi MG, Macklin EA, Fung EB, Vichinsky E, Olivieri N, Kwiatkowski J, Cohen A, Neufeld E, Giardina PJ (2006) prevalence of fractures among the thalassemia syndromes in North America. Bone. 38(4):571–575
Hamann C, Kirschner S, Gunther KP, Hofbauer LC (2012) Bone, sweet bone--osteoporotic fractures in diabetes mellitus. Nat Rev Endocrinol 8(5):297–305
Leidig-Bruckner G, Ziegler R (2001) Diabetes mellitus a risk for osteoporosis? Exp Clin Endocrinol Diabetes 109(Suppl 2):S493–S514
Hofbauer LC, Brueck CC, Singh SK, Dobnig H (2007) Osteoporosis in patients with diabetes mellitus. J Bone Miner Res 22(9):1317–1328
Polat HB, Beyazal MS (2018) The effect of cholecystectomy on 25-hydroxyvitamin D levels and bone mineral density in postmenopausal women. Arch Osteoporos 13(1):61
Baschant U, Rauner M, Balaian E, Weidner H, Roetto A, Platzbecker U, Hofbauer LC (2016) Wnt5a is a key target for the pro-osteogenic effects of iron chelation on osteoblast progenitors. Haematologica. 101(12):1499–1507
Momeni A, Rapp S, Donneys A, Buchman SR, Wan DC (2016) Clinical use of deferoxamine in distraction osteogenesis of irradiated bone. J Craniofac Surg 27(4):880–882
Wong P, Fuller PJ, Gillespie MT, Kartsogiannis V, Kerr PG, Doery JC et al (2014) Thalassemia bone disease: a 19-year longitudinal analysis. J Bone Miner Res 29(11):2468–2473
Fung EB, Harmatz PR, Milet M, Coates TD, Thompson AA, Ranalli M, Mignaca R, Scher C, Giardina P, Robertson S, Neumayr L, Vichinsky EP, Multi-Center Iron Overload Study Group (2008) Fracture prevalence and relationship to endocrinopathy in iron overloaded patients with sickle cell disease and thalassemia. Bone. 43(1):162–168
Acknowledgments
The authors wish to thank Mr. H. Argasi at the Research Consultation Center (RCC) of Shiraz University of Medical Sciences for his invaluable assistance in editing this manuscript.
Author information
Authors and Affiliations
Contributions
1. Mohammadreza Bordbar: concept, design, data gathering, and preparing the manuscript
2. Gholamhossein Ranjbar Omrani: design, data gathering of the control group, and preparing the manuscript
3. Forough Saki: design, data gathering, preparing the manuscript, and the correspondence
4. Sezaneh Haghpanah: design, data analysis, and preparing the manuscript
5. Mehran Karimi: concept, design, and data gathering
6. Omidreza Zekavat: concept, design, and data gathering
Corresponding author
Ethics declarations
Conflicts of interest
None.
Ethics approval
The local Ethics Committee of Shiraz University of Medical Sciences (SUMS) approved the study. Vice-chancellor of research at SUMS approved this study with ID: 98-01-32-21135. All participants signed an informed consent form.
Consent to participate
All patients signed a written informed consent form after explaining the aim, method, and goal of the study for participation.
Consent for publication
All patients signed a written informed consent form after explaining the aim, method, and goal of the study for publishing any data from their records.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bordbar, M., Omrani, G.R., Haghpanah, S. et al. Bone mineral density in transfusion-dependent thalassemia patients and its associated factors in Southern Iran. Arch Osteoporos 15, 148 (2020). https://doi.org/10.1007/s11657-020-00811-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-020-00811-7