Abstract
Summary
This study demonstrates a low anti-osteoporosis drug treatment rate (22.1% in women, 9.5% in men) after osteoporotic fracture in the real-world setting of Fujian, China. The primary medication was calcitonin. The suboptimal treatment was particularly critical among men, low-level hospitals, wrist/vertebral fracture, and the younger elderly patients.
Introduction
The objective of this study was to investigate the prescription patterns and related influencing factors of anti-osteoporosis drug prescribing after osteoporotic fracture in Fujian, China, between 2010 and 2016.
Methods
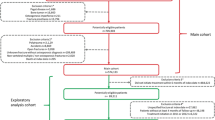
This is a retrospective cohort study based on an existing electronic health record database (National Healthcare Big Data in Fuzhou, China, 37 hospitals included). Patients over 50 years old with newly diagnosed osteoporotic fractures between 2010 and 2016 were included. Postfracture osteoporosis therapies were summarized by overall and fracture site. Multivariate logistic regression was performed to identify influencing factors of anti-osteoporosis medication (AOM) prescription.
Results
Overall, 22.1% of women and 9.5% of men over 50 years old received AOM treatment after osteoporotic fracture within 1 year during 2010–2016, with particular low use of bisphosphonates, 5.3% in women and 1.5% in men. The highest rate of AOM treatment was found in patients with hip fracture (24.5%), followed by vertebral fracture (14.2%) and wrist fracture (2.3%). Of the AOM-treated patients, 90.5% received calcitonin therapy. The treatment rate of AOM showed a slight decline during 2010–2016, but steady rise trends were observed in Ca/vitamin D (VD) prescription. Hospital level, age, sex, previous osteoporosis, previous AOM prescription, and previous oral glucocorticoid prescription were strong predicting factors of AOM prescription.
Conclusion
In a real-world setting, AOM treatment was suboptimal and the treatment rate even decreased over time among osteoporosis fracture patients in Fujian, China. The suboptimal treatment was particularly critical among men, low-level hospitals, wrist/vertebral fracture, and the younger elderly patients.



Similar content being viewed by others
References
Alejandro P, Constantinescu F (2018) A review of osteoporosis in the older adult: an update. Rheum Dis Clin N Am 44(3):437–451. https://doi.org/10.1016/j.rdc.2018.03.004
Hernlund E, Svedbom A, Ivergard M, Compston J, Cooper C, Stenmark J et al (2013) Osteoporosis in the European Union: medical management, epidemiology and economic burden. A report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Arch Osteoporos 8:136. https://doi.org/10.1007/s11657-013-0136-1
Strom O, Borgstrom F, Kanis JA, Compston J, Cooper C, McCloskey EV et al (2011) Osteoporosis: burden, health care provision and opportunities in the EU: a report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Arch Osteoporos 6:59–155. https://doi.org/10.1007/s11657-011-0060-1
Zeng Q, Li N, Wang Q, Feng J, Sun D, Zhang Q et al (2019) The prevalence of osteoporosis in China, a nationwide, multicenter DXA survey. J Bone Miner Res 34(10):1789–1797. https://doi.org/10.1002/jbmr.3757
Wang Y, Tao Y, Hyman ME, Li J, Chen Y (2009) Osteoporosis in China. Osteoporos Int 20(10):1651–1662. https://doi.org/10.1007/s00198-009-0925-y
Si L, Winzenberg TM, Jiang Q, Chen M, Palmer AJ (2015) Projection of osteoporosis-related fractures and costs in China: 2010-2050. Osteoporos Int 26(7):1929–1937. https://doi.org/10.1007/s00198-015-3093-2
Melton LR, Crowson CS, O'Fallon WM (1999) Fracture incidence in Olmsted County, Minnesota: comparison of urban with rural rates and changes in urban rates over time. Osteoporos Int 9(1):29–37
Brauer CA, Coca-Perraillon M, Cutler DM, Rosen AB (2009) Incidence and mortality of hip fractures in the United States. JAMA. 302(14):1573–1579. https://doi.org/10.1001/jama.2009.1462
Jean S, O'Donnell S, Lagace C, Walsh P, Bancej C, Brown JP et al (2013) Trends in hip fracture rates in Canada: an age-period-cohort analysis. J Bone Miner Res 28(6):1283–1289. https://doi.org/10.1002/jbmr.1863
Chen IJ, Chiang CY, Li YH, Chang CH, Hu CC, Chen DW et al (2015) Nationwide cohort study of hip fractures: time trends in the incidence rates and projections up to 2035. Osteoporos Int 26(2):681–688. https://doi.org/10.1007/s00198-014-2930-z
Nymark T, Lauritsen JM, Ovesen O, Rock ND, Jeune B (2006) Decreasing incidence of hip fracture in the Funen County. Denmark Acta Orthop 77(1):109–113. https://doi.org/10.1080/17453670610045777
Dimai HP, Svedbom A, Fahrleitner-Pammer A, Pieber T, Resch H, Zwettler E et al (2011) Epidemiology of hip fractures in Austria: evidence for a change in the secular trend. Osteoporos Int 22(2):685–692. https://doi.org/10.1007/s00198-010-1271-9
Hawley S, Leal J, Delmestri A, Prieto-Alhambra D, Arden NK, Cooper C et al (2016) Anti-osteoporosis medication prescriptions and incidence of subsequent fracture among primary hip fracture patients in England and Wales: an interrupted time-series analysis. J Bone Miner Res 31(11):2008–2015. https://doi.org/10.1002/jbmr.2882
Kim SC, Kim MS, Sanfelix-Gimeno G, Song HJ, Liu J, Hurtado I et al (2015) Use of osteoporosis medications after hospitalization for hip fracture: a cross-national study. Am J Med 128(5):519–526. https://doi.org/10.1016/j.amjmed.2015.01.014
Munson JC, Bynum JP, Bell JE, Cantu R, McDonough C, Wang Q et al (2016) Patterns of prescription drug use before and after fragility fracture. JAMA Intern Med 176(10):1531–1538. https://doi.org/10.1001/jamainternmed.2016.4814
Shah A, Prieto-Alhambra D, Hawley S, Delmestri A, Lippett J, Cooper C et al (2017) Geographic variation in secondary fracture prevention after a hip fracture during 1999-2013: a UK study. Osteoporos Int 28(1):169–178. https://doi.org/10.1007/s00198-016-3811-4
Gonnelli S, Caffarelli C, Iolascon G, Bertoldo F, Letizia MG, Patti A et al (2017) Prescription of anti-osteoporosis medications after hospitalization for hip fracture: a multicentre Italian survey. Aging Clin Exp Res 29(5):1031–1037. https://doi.org/10.1007/s40520-016-0681-8
Yu YM, Lee JY, Lee E (2017) Access to anti-osteoporosis medication after hip fracture in Korean elderly patients. Maturitas. 103:54–59. https://doi.org/10.1016/j.maturitas.2017.06.021
Sundararajan V, Henderson T, Perry C, Muggivan A, Quan H, Ghali WA (2004) New ICD-10 version of the Charlson comorbidity index predicted in-hospital mortality. J Clin Epidemiol 57(12):1288–1294. https://doi.org/10.1016/j.jclinepi.2004.03.012
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40(5):373–383. https://doi.org/10.1016/0021-9681(87)90171-8
Belhassen M, Confavreux CB, Cortet B, Lamezec L, Ginoux M, Van Ganse E (2017) Anti-osteoporotic treatments in France: initiation, persistence and switches over 6 years of follow-up. Osteoporos Int 28(3):853–862. https://doi.org/10.1007/s00198-016-3789-y
van der Velde RY, Wyers CE, Teesselink E, Geusens P, van den Bergh J, de Vries F et al (2017) Trends in oral anti-osteoporosis drug prescription in the United Kingdom between 1990 and 2012: variation by age, sex, geographic location and ethnicity. Bone. 94:50–55. https://doi.org/10.1016/j.bone.2016.10.013
Li JT (2013) Analysis on the trend and application of anti-osteoporosis drugs in our hospital. Hebei Med 17:2683–2684. https://doi.org/10.3969/j.issn.1002-7386.2013.17.071
Zhang XC, Wan B, Zhou WM, Pan LY. Investigation on the use of anti-osteoporosis drugs in outpatient department of a hospital. People’s military doctors 2019;62(2):142-7
Kanis JA, McCloskey EV, Johansson H, Cooper C, Rizzoli R, Reginster JY (2013) European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporos Int 24(1):23–57. https://doi.org/10.1007/s00198-012-2074-y
Forciea MA, McLean RM, Qaseem A (2017) Treatment of low bone density or osteoporosis to prevent fractures in men and women. Ann Intern Med 167(12):904. https://doi.org/10.7326/L17-0490
Ma YZ, Wang YP, Liu Q, Li CL, Ma X, Wang YJ et al (2019) Guidelines for diagnosis and treatment of osteoporosis in the elderly in China (2018). Chin J Gerontol 39(11):2561–2579. https://doi.org/10.3969/j.issn.1005-9202.2019.11.001
Wang PW, Li YZ, Zhuang HF, Yu HM, Cai SQ, Xu H et al (2019) Anti-osteoporosis medications associated with decreased mortality after hip fracture. Orthop Surg 11(5):777–783. https://doi.org/10.1111/os.12517
Klop C, Gibson-Smith D, Elders PJ, Welsing PM, Leufkens HG, Harvey NC et al (2015) Anti-osteoporosis drug prescribing after hip fracture in the UK: 2000-2010. Osteoporos Int 26(7):1919–1928. https://doi.org/10.1007/s00198-015-3098-x
Fraser LA, Ioannidis G, Adachi JD, Pickard L, Kaiser SM, Prior J et al (2011) Fragility fractures and the osteoporosis care gap in women: the Canadian Multicentre Osteoporosis Study. Osteoporos Int 22(3):789–796. https://doi.org/10.1007/s00198-010-1359-2
Cadarette SM, Katz JN, Brookhart MA, Levin R, Stedman MR, Choudhry NK, Solomon DH (2008) Trends in drug prescribing for osteoporosis after hip fracture, 1995-2004. J Rheumatol 35(2):319–326
Roerholt C, Eiken P, Abrahamsen B (2009) Initiation of anti-osteoporotic therapy in patients with recent fractures: a nationwide analysis of prescription rates and persistence. Osteoporos Int 20(2):299–307. https://doi.org/10.1007/s00198-008-0651-x
Alves SM, Economou T, Oliveira C, Ribeiro AI, Neves N, Gomez-Barrena E et al (2013) Osteoporotic hip fractures: bisphosphonates sales and observed turning point in trend. A population-based retrospective study. Bone. 53(2):430–436. https://doi.org/10.1016/j.bone.2012.12.014
Zhang J, Delzell E, Curtis JR, Hooven F, Gehlbach SH, Anderson FJ et al (2014) Use of pharmacologic agents for the primary prevention of osteoporosis among older women with low bone mass. Osteoporos Int 25(1):317–324. https://doi.org/10.1007/s00198-013-2444-0
Corsonello A, Pedone C, Incalzi RA (2010) Age-related pharmacokinetic and pharmacodynamic changes and related risk of adverse drug reactions. Curr Med Chem 17(6):571–584. https://doi.org/10.2174/092986710790416326
Tsoi CS, Chow JY, Choi KS, Li HW, Nie JX, Tracy CS et al (2014) Medical characteristics of the oldest old: retrospective chart review of patients aged 85+ in an academic primary care centre. BMC Res Notes 7:340. https://doi.org/10.1186/1756-0500-7-340
Bor A, Matuz M, Gyimesi N, Biczok Z, Soos G, Doro P (2015) Gender inequalities in the treatment of osteoporosis. Maturitas. 80(2):162–169. https://doi.org/10.1016/j.maturitas.2014.11.001
Yusuf AA, Matlon TJ, Grauer A, Barron R, Chandler D, Peng Y (2016) Utilization of osteoporosis medication after a fragility fracture among elderly Medicare beneficiaries. Arch Osteoporos 11(1):31. https://doi.org/10.1007/s11657-016-0285-0
De Vries F, Bracke M, Leufkens HG, Lammers JW, Cooper C, Van Staa TP (2007) Fracture risk with intermittent high-dose oral glucocorticoid therapy. Arthritis Rheum 56(1):208–214. https://doi.org/10.1002/art.22294
Acknowledgments
We thank China Electronics Corporation (CEC) Data for granting access to the National Health database.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
This study was approved by China Ethnic Committee of Registering Clinical Trials (ChiECRCT-20190178).
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, X., Li, C., He, Y. et al. Anti-osteoporosis medication treatment pattern after osteoporotic fracture during 2010–2016 in Fujian, China. Arch Osteoporos 15, 134 (2020). https://doi.org/10.1007/s11657-020-00798-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-020-00798-1