Abstract
Objective
To observe the efficacy and the influence on quality of life (QOL) of syndrome differentiation treatment with Chinese medicine (CM) for opioid-induced constipation as well as the safety and influence on analgesic effect of opioids.
Methods
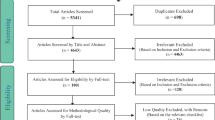
Totally 406 cases enrolled from 53 collaborating medical centers were randomly assigned to a CM group and a control group. The CM group were treated with CM decoction based on syndrome differentiation, and the control group were treated with Phenolphthalein Tablet. Both groups were treated for 14 days. Cleveland constipation score (CCS), numerical rating scale (NRS) of pain and Chinese version of European Organisation for Research and Treatment of Cancer, Quality of Life Questionnaire-C30 V3.0 (EORTC QLQ-C30 V3.0) were used to evaluate the efficacy, pain controlled and QOL status.
Results
The comparisons of CCS score reduction and QOL between the two groups after treatment suggested that the improvements of constipation and QOL in the CM group were better than that in the control group (P<0.05). The total efficiency of the CM group was better than the control group (93.5% vs. 86.4%, P<0.05). There was no significant difference in NRS scores between before and after treatment in both groups. There was no serious drug-related adverse event during the course of study.
Conclusion
CM decoction could effectively treat opioid-induced constipation and improve patients’ QOL at the same time. It is safe and doesn’t affect the analgesic effect of opioids when treating constipation.
Similar content being viewed by others
Refrences
Cohen MZ, Easley MK, Ellis C, Hughes B, Ownby K, Rashad BG, et al. Cancer pain management and the JCAHO’s pain standards:an institutional challenge. J Pain Symptomf Manage 2003;25:519–527.
Goudas LC, Bloch R, Gialeli-Goudas M, Lau J, Carr DB. The epidemiology of cancer pain. Cancer Investigat 2005;23:182–190.
Svendsen KB, Andersen S, Arnason S, Arnér S, Breivik H, Heiskanen T, et al. Breakthrough pain in malignant and nonmalignant diseases: a review of prevalence, characteristics and mechanisms. Eur J Pain 2005;9:195–206.
World Health Organization. Cancer pain relief. 2nd ed. Geneva, Switzerland: World Health Organization;1996.
Sun Y, Shi YK. Manual of clinical oncology. Beijing: People’s Medical Publishing House; 2007:277.
Cherny N, Ripamonti C, Pereira J, Davis C, Fallon M, McQuay H, et al. Strategies to manage the adverse effects of oral morphine: an evidence-based report. J Clin Oncol 2001;19:2542–2554.
Yu CP, An JX. How to prevent and control opioid-induced constipation. China Prescript Drug (Chin) 2008;8:74–76.
Liu M, Wittbrodt E. Low-dose oral naloxone reverses opioid-induced constipation and analgesia. J Pain Symptom Manage 2002;23:48–53.
Wang LN, Li J, Li DR, Lin HS. The status quo of the treatment of opioid-induced constipation with Chinese medicine. Chin J Integr Tradit West Med (Chin) 2010;16:116–119.
American College of Gastroenterology Chronic Constipation Task Force. An evidence-based approach to the management of chronic constipation in North America. Am J Gastroenterol 2005;100(Suppl 1):S1–S4.
Ministry of Health of the People’s Republic of China. Guideline for Clinical Study of New Chinese Medicines. Beijing, China: Ministry of Health of the People’s Republic of China; 1993:131–133.
EORTC Quality of Life Group. Guidelines for assessing quality of life in EORTC clinical trials. Brussels, Belgium: Quality Life Unit, EORTC Data Center 2002;22(15):21–24.
Wa CH, Chen MQ, Zhang CZ, Tang XL, Meng Q, Zhang XQ. The Chinese version of EORTC QLQ-C3 form in evaluation of QOL for patients with cancer. J Pract Oncol (Chin) 2005;10:353–355.
Swarm R, Abernethy AP, Anghelescu DL, Benedetti C, Blinderman CD, Boston B, et al. NCCN clinical practice guidelines in oncology on adult cancer pain. J Natl Compr Canc Netw 2010;8:1055.
Common Terminology Criteria for Adverse Events v3.0. Available at: http://ctep.cancer.gov/protocolDevelopment/electronic_applications/docs/ctcaev3.pdf. Accessed July 30, 2011.
Wood JD, Galligan JJ. Function of opioids in the enteric nervous system. Neurogastroenterol Motil 2004;16:17–28.
Galligan JJ, Vanner S. Basic and clinical pharmacology of new motility promoting agents. Neurogastroenterol Motil 2005;17:643–653.
De Schepper HU, Cremonini F, Park MI, Camilleri M. Opioids and the gut: pharmacology and current clinical experience. Neurogastroenterol Motil 2004;16:383–394.
Choi YS, Billings JA. Opioid antagonists: a review of their role in palliative care, focusing on use in opioid-related constipation. J Pain Symptom Manage 2002;24:71–90.
Gu Y J, Chen J, Sun YY, Zhang X. Clinical observation on Jiangni Kuanchang Decoction for opioid-related constipation. Liaoning J Tradit Chin Med (Chin) 2009;36:233–234.
Tian DL. Internal medicine of traditional Chinese medicine. Beijing: People’s Medical Publishing House; 2006:226–230.
Zhao YL, Zhang ZH, Wang ZR. Relationship between purgative effect of Rhubarb and 5-HT and it’s receptor in duodenum tissues. J Yunnan Univ Tradit Chin Med (Chin) 2002;25:1–3.
Yu M, Luo YL, Zheng JW, Ding YH, Li W, Zheng TZ, et al. Effects of Rhubarb on isolated gastric muscle strips of guinea pigs. World J Gastroenterol 2005;11:2670–2673.
Zhang QR, Li L, Chen DS, Peng JX, Wang XW. Effects of Cortex magnoliae officinalis, Fructus aurantii immaturus, Rhubarb and Pericarpium citri reticulatae on rabbits’ isolated fundal smooth muscle movement. Chin J Tradit Med Sci Technol (Chin) 2008;15:279–280.
Wang, CF, Yang DZ, Wei YQ, Xun QY. Study on the effect of Fructus aurantii immaturus on myoelectric of gastrointestinal tract in rats. J Southeast Univ (Med Sci Ed, Chin) 2001;20:153–154.
Zhang QR, Ding L, Zhao XM, Guo XD, Li L. The effect of Cortex magnoliae officinalis on the movement of rabbits’ dissociated smooth muscles of intestine and stomach. Shaanxi Med J (Chin) 2007;36:656–659.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Chen, Cm., Lin, Lz. & Zhang, Ex. Standardized treatment of chinese medicine decoction for cancer pain patients with opioid-induced constipation: A multi-center prospective randomized controlled study. Chin. J. Integr. Med. 20, 496–502 (2014). https://doi.org/10.1007/s11655-014-1864-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-014-1864-9