Abstract
Background
Systematic reviews have the potential to inform clinical decisions, yet little is known about the impact of interventions on increasing the use of systematic reviews in clinical decision-making.
Purpose
To systematically review the evidence on the impact of interventions for seeking, appraising, and applying evidence from systematic reviews in decision-making by clinicians.
Data Sources
Medline, EMBASE, CINAHL, Cochrane Central Register of Controlled Trials, and LISA were searched from the earliest date available until July 2009.
Study Selection and Data Extraction
Two independent reviewers selected studies for inclusion if the intervention intended to increase seeking, appraising, or applying evidence from systematic reviews by a clinician. Information about the study population, features of each intervention, methods used to measure the use of systematic reviews and those used to measure professional performance or health care outcomes, existence and use of statistical tests, study outcomes, and comparative data were extracted.
Data Synthesis
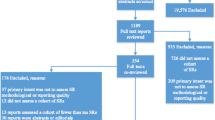
A total of 8,104 titles and abstracts were reviewed, leading to retrieval of 189 full-text articles for assessment; five of these studies met all inclusion criteria. All five studies reported on professional performance behavior; none reported on patient health outcomes. One study reported positive outcomes in improving preventive care. Three studies focused on obstetrical care, with two reporting no impact on professional practice change, and one study reporting increases in the use of prophylactic oxytocin and episiotomy. One study found no improvement in the sealant rate of newly erupted molars among dentists in Scotland.
Limitations
The small number of studies available for examination indicates the difficulty in summarizing and identifying key aspects in successful strategies that encourage clinicians to use systematic reviews in decision-making. Other concerns lay in selective reporting and lack of blinding during data collection.
Conclusions
The limited empirical data render the strength of evidence weak for the effectiveness and types of interventions that encourage clinicians to use systematic reviews in clinical decision making.

Similar content being viewed by others
References
Grol R, Grimshaw J. From best evidence to best practice: effective implementation of change in patients' care. Lancet. 2003;362(9391):1225–30.
Olson KL, Bungard TJ, Tsuyuki RT. Cholesterol risk management: a systematic examination of the gap from evidence to practice. Pharmacotherapy. 2001;21(7):807–17.
Arnold SR, Straus SE. Interventions to improve antibiotic prescribing practices in ambulatory care. Cochrane Database Syst Rev 2005; Issue 4. Art. No.: CD003539. doi: 10.1002/14651858.CD003539.pub2.
Buchan H. Gaps between best evidence and practice: causes for concern. Med J Aust. 2004;180(6 Suppl):S48–9.
Villar J, Carroli G, Gulmezoglu AM. The gap between evidence and practice in maternal healthcare. Int J Gynaecol Obstet. 2001;75(Suppl 1):S47–54.
Higgins JPT, Green S (editors). Cochrane Handbook for Systematic Reviews of Interventions Version 5.0.1 [updated September 2009]. The Cochrane Collaboration, 2008. Available from http://www.cochrane-handbook.org. Accessed August 21, 2010.
Laupacis A, Straus S. Systematic reviews: time to address clinical and policy relevance as well as methodological rigor. Ann Intern Med. 2007;147(4):273–4.
De Vito C, Nobile CG, Furnari G, Pavia M, De Giusti M, Angelillo IF, Villari P. Physicians' knowledge, attitudes and professional use of RCTs and meta-analyses: a cross-sectional survey. Eur J Public Health. 2009;19(3):297–302.
Dawes M, Sampson U. Knowledge management in clinical practice: a systematic review of information seeking behavior in physicians. Int J Med Inform. 2003;71(1):9–15.
Wilson PM, Watt IS, Hardman GF. Survey of medical directors’ views and use of the Cochrane Library. Br J Clin Governance. 2001;6(1):34–9.
Kerse N, Arroll B, Lloyd T, Young J, Ward J. Evidence databases, the Internet, and general practitioners: the New Zealand story. N Z Med J. 2001;114(1127):89–91.
Ram FSF, Wellington SR. General practitioners use of the Cochrane Library in London. Prim Care Respir J. 2002;11(4):123–5.
Estabrooks CA, Chong H, Brigidear K, Profetto-McGrath J. Profiling Canadian nurses' preferred knowledge sources for clinical practice. Can J Nurs Res. 2005;37(2):118–40.
Berlin JA. Does blinding of readers affect the results of meta-analyses? University of Pennsylvania Meta-analysis Blinding Study Group. Lancet. 1997;350(9072):185–6.
Kjaergard LL, Villumsen J, Gluud C. Reported methodologic quality and discrepancies between large and small randomized trials in meta-analyses. Ann Intern Med. 2001;135(11):982–9.
Lemelin J, Hogg W, Baskerville N. Evidence to action: a tailored multifaceted approach to changing family physician practice patterns and improving preventive care. CMAJ. 2001;164(6):757–63.
Gülmezoglu AM, Langer A, Piaggio G, Lumbiganon P, Villar J, Grimshaw J. Cluster randomised trial of an active, multifaceted educational intervention based on the WHO Reproductive Health Library to improve obstetric practices. BJOG. 2007;114(1):16–23.
Wyatt JC, Paterson-Brown S, Johanson R, Altman DG, Bradburn MJ, Fisk NM. Randomised trial of educational visits to enhance use of systematic reviews in 25 obstetric units. BMJ. 1998;317(7165):1041–6.
Althabe F, Buekens P, Bergel E, Belizán JM, Campbell MK, Moss N, Hartwell T, Wright LL, Guidelines Trial Group. A behavioral intervention to improve obstetrical care. N Engl J Med. 2008;358(18):1929–40.
Clarkson JE, Turner S, Grimshaw JM, Ramsay CR, Johnston M, Scott A, Bonetti D, Tilley CJ, Maclennan G, Ibbetson R, Macpherson LM, Pitts NB. Changing clinicians' behavior: a randomized controlled trial of fees and education. J Dent Res. 2008;87(7):640–4.
Krahn J, Sauerland S, Rixen D, Gregor S, Bouillon B, Neugebauer EA. Applying evidence-based surgery in daily clinical routine: a feasibility study. Arch Orthop Trauma Surg. 2006;126(2):88–92.
Langham J, Tucker H, Sloan D, Pettifer J, Thom S, Hemingway H. Secondary prevention of cardiovascular disease: a randomised trial of training in information management, evidence-based medicine, both or neither: the PIER trial. Br J Gen Pract. 2002;52(483):818–24.
Mukohara K, Schwartz MD. Electronic delivery of research summaries for academic generalist doctors: a randomised trial of an educational intervention. Med Educ. 2005;39(4):402–9.
Seers K, Crichton N, Carroll D, Richards S, Saunders T. Evidence-based postoperative pain management in nursing: is a randomized-controlled trial the most appropriate design? J Nurs Manag. 2004;12(3):183–93.
Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8(1):19–32.
Acknowledgements
We are grateful to David Newton for his technical assistance.
Funders
Canadian Institutes of Health Research, and each author’s institution. The funding source had no role in the study design, collection, analysis, and interpretation of results, in the writing of the report, or in the decision to submit the paper for publication.
Prior presentations
May 19, 2010, Cochrane Canada 8th Annual Symposium
Conflict of interest
None disclosed.
Ethical approval
Not required
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Perrier, L., Mrklas, K., Shepperd, S. et al. Interventions Encouraging the Use of Systematic Reviews in Clinical Decision-Making: A Systematic Review. J GEN INTERN MED 26, 419–426 (2011). https://doi.org/10.1007/s11606-010-1506-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-010-1506-7