Abstract
Background
Hospitalized patients frequently have urinary catheters inserted for inappropriate reasons. This can lead to urinary tract infections and other complications.
Objective
To assess whether stop orders for indwelling urinary catheters reduces the duration of inappropriate urinary catheterization and the incidence of urinary tract infections.
Design
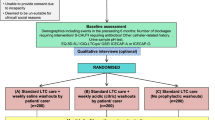
A randomized controlled trial was conducted in three tertiary-care hospitals in Ontario, Canada. Patients with indwelling urinary catheters were randomized to prewritten orders for the removal of urinary catheters if specified criteria were not present or to usual care.
Participants
Six hundred ninety-two hospitalized patients admitted to hospital with indwelling urinary catheters inserted for ≤48 h.
Measurements
The main outcomes included days of inappropriate indwelling catheter use, total days of catheter use, frequency of urinary tract infection, and catheter reinsertions.
Results
There were fewer days of inappropriate and total urinary catheter use in the stop-order group than in the usual care group (difference −1.69 [95% CI −1.23 to −2.15], P < 0.001 and −1.34 days, [95% CI, −0.64 to −2.05 days], P < 0.001, respectively). Urinary tract infections occurred in 19.0% of the stop-order group and 20.2% of the usual care group, relative risk 0.94 (95% CI, 0.66 to 1.33), P = 0.71. Catheter reinsertion occurred in 8.6% of the stop-order group and 7.0% in the usual care group, relative risk 1.23 (95% CI, 0.72 to 2.11), P = 0.45.
Conclusions
Stop orders for urinary catheterization safely reduced duration of inappropriate urinary catheterization in hospitalized patients but did not reduce urinary tract infections.

Similar content being viewed by others
References
Topal J , Conklin S , Camp K , Morris V , Balcezak T , Herbert P. Prevention of nosocomial catheter-associated urinary tract infections through computerized feedback to physicians and a nurse-directed protocol. Am J Med Qual. 2005;20:121–6.
Gokula RR , Hickner JA , Smith MA. Inappropriate use of urinary catheters in elderly patients at a midwestern community teaching hospital. Am J Infect Control. 2004;32:196–9.
Hazelett SE , Tsai M , Gareri M , Allen K. The association between indwelling urinary catheter use in the elderly and urinary tract infection in acute care. BMC Geriatr. 2006;6:15. http://www.biomedcentral.com/1471–2318/6/15 (accessed March 21, 2008).
Jain P , Parada J , Annette D , Smith L. Overuse of the indwelling urinary tract catheter in hospitalized medical patients. Arch Intern Med. 1995;155131425–9.
Munasinghe RL , Yazdani H , Siddique M , Hafeez W. Appropriateness of use of indwelling urinary catheters in patients admitted to the medical service. Infect Control Hosp Epidemiol. 2001;22:647–9.
Gardam MA , Amihod B , Orenstein P , Consolacion N , Miller MA. Overutilization of indwelling urinary catheters and the development of nosocomial urinary tract infections. Clin Perform Qual Health Care. 1998;6:99–102.
Saint S , Wiese J , Amory JK , et al.. Are physicians aware of which of their patients have indwelling urinary catheters? Am J Med. 2000;109:476–80.
Sedor J , Mulholland SG. Hospital-acquired urinary tract infections associated with the indwelling catheter. Urol Clin North Am. 1999;26:821–8.
Saint S , Lipsky BA. Preventing catheter-related bacteriuria: Should we? Can we? How? Arch Intern Med. 1999;159:800–8.
Stamm WE. Catheter-associated urinary tract infections: epidemiology, pathogenesis, and prevention. Am J Med. 1991;91suppl 3B65S–71S.
Warren JW. Catheter-associated urinary tract infections. Infect Dis Clin North Am. 1997;11:609–22.
Balows LE , eds. Manual of Clinical Microbiology. 5th ed. Washington DC: American Society for Microbiology; 1991.
Garner JS , Jarvis WR , Emori TG , Horan TC , Hughes JM. CDC definitions for nosocomial infections, 1988. Am J Infect Control. 1988;16:128–40.
National Committee for Clinical Laboratory Standards. Performance standards for antimicrobial susceptibility tests: sixth informational supplement M100-S6. Wayne: NCCLS; 1995.
Haley RW , Hooton TM , Culver DH , et al. Nosocomial infections in US hospitals, 1975–1976: estimated frequency by selected characteristics of patients. Am J Med. 1981;70:947–59.
Garibaldi RA , Burke JP , Dickman ML , Smith CB. Factors predisposing to bacteriuria during indwelling urethral catheterization. N Engl J Med. 1974;291:215–9.
Cornia PB , Amory JK , Fraser S , Saint S , Lipsky BA. Computer-based order entry decreases duration of indwelling urinary catheterization in hospitalized patients. Am J Med. 2003;114:404–7.
Saint S , Kaufman SR , Thompson M , Rogers MA , Chenoweth CE. A reminder reduces urinary catheterization in hospitalized patients. Jt Comm J Qual Patient Saf. 2005;31:455–62.
Huang WC , Wann SR , Lin SL , et al. Catheter-associated urinary tract infections in intensive care units can be reduced by prompting physicians to remove unnecessary catheters. Infect Control Hosp Epidemiol. 2004;25:974–8.
Saint S , Lipsky BA , Goold SD. Indwelling urinary catheters: a one-point restraint? Ann Intern Med. 2002;137:125–7.
Tambyah PA , Maki DG. Catheter-associated urinary tract infection is rarely symptomatic: a prospective study of 1,497 catheterized patients. Arch Intern Med. 2000;160:678–82.
Acknowledgements
This study was funded by the Physician’s Services Incorporated Foundation of Ontario.
Potential Financial Conflicts of interest:
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Loeb, M., Hunt, D., O’Halloran, K. et al. Stop Orders to Reduce Inappropriate Urinary Catheterization in Hospitalized Patients: A Randomized Controlled Trial. J GEN INTERN MED 23, 816–820 (2008). https://doi.org/10.1007/s11606-008-0620-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-008-0620-2