Background
Little evidence exists to support the value of reflection in the clinical setting.
Objective
To determine whether reflecting and revisiting the “patient” during a standardized patient (SP) examination improves junior medical students’ performance and to analyze students’ perceptions of its value.
Design
Students completed a six-encounter clinical skills examination, writing a guided assessment after each encounter to trigger reflection. SPs evaluated the students with Medical Skills and Patient Satisfaction checklists. During the last three encounters, students could opt to revisit the SP and be reevaluated with identical checklists.
Participants
One hundred and forty-nine third year medical students.
Measurements
Changes in scores in the Medical Skills and Patient Satisfaction checklists between first visit and revisit were tested separately per case as well as across cases.
Results
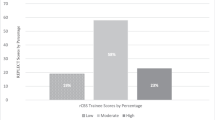
On the medical skills and patient satisfaction checklists, mean revisit scores across cases were significantly higher than mean first visit scores [12.6 vs 12.2 (pooled SD = 2.4), P = .0001; 31.2 vs 31.0 (pooled SD = 3.5), P = .0001)]. Sixty-five percent of the time, students rated “reflect–revisit” positively, 34% neutrally, and 0.4% negatively. Five themes were identified in the positive comments: enhancement of (1) medical decision making, (2) patient education/counseling, (3) student satisfaction/confidence, (4) patient satisfaction/confidence, and (5) clinical realism.
Conclusions
Offering third year medical students the option to reflect and revisit an SP during a clinical skills examination produced a small but nontrivial increase in clinical performance. Students perceived the reflect–revisit experience as enhancing patient-centered practices (counseling, education) as well as their own medical decision making and clinical confidence.
Similar content being viewed by others
References
Branch WT, Paranjape A. Feedback and reflection: teaching methods for clinical settings. Acad Med. 2002;77(12):1185–8.
Branch WT, Kern D, Haidet P, et al. Teaching the human dimensions of care in clinical settings. JAMA. 2001; 286(9):1067–74.
Pee B, Woodman T, Fry H, Davenport E. Appraising and assessing reflection in students’ writing on a structure worksheet. Med Educ. 2002;36:575–85.
Brookfield SD.Developing Critical Thinkers: Challenging Adults to Explore Alternative Ways of Thinking and Acting. San Francisco: Jossey-Bass, Inc; 1987.
Jarvis P, Holford J, Griffin C.The Theory and Practice of Learning. London: Kogan Page; 1998.
Mezirow JA.Fostering Critical Reflection in Adulthood: A Guide to Transformative and Emancipatory Learning. San Francisco: Jossey-Bass Publishers; 1990.
Schön DA.Educating the Reflective Practitioner. San Francisco: Jossey-Bass Publishers; 1987.
Killion J, Todnem G. A process for personal theory building. Educ Leadersh. 1991;48(6):14–6.
Kolb D.Experiential Learning: Experience as the Source of Learning and Development. Englewood Cliffs, NJ: Prentice-Hall, Inc; 1984.
Johns C.Becoming a Reflective Practitioner. 2nd ed. Oxford, UK: Blackwell Publishing Ltd; 2004.
American Board of internal Medicine. Using Patient Satisfaction Questionnaires (PSQs) for Recertification. Available at: http://www.uthscsa.edu/gme/nsgeval.pdf. Accessed 31 Aug 2005.
Lipner RS, Blank LL, Leas BF, Fortna GS. The value of patient and peer ratings in recertification. Acad Med. 2002;77(10 suppl):S64–6.
Strauss A, Corbin J.Basics of Qualitative Research. Thousand Oaks, CA: Sage Publications, Inc; 1998.
Merriam SB, Associates.Qualitative Research in Practice: Examples for Discussion and Analysis. San Francisco: Jossey-Bass, Inc; 2002.
Portney LG, Watkins MP.Foundations of Clinical Research: Applications to Practice. Upper Saddle River, NJ: Prentice Hall; 2000.
Kruger J, Dunning D. Unskilled and unaware of it: how difficulties in recognizing one’s own incompetence lead to inflated self-assessments. J Pers Soc Psychol. 1999;77(6):1121–1134.
Hasnain M, Bordage G, Connell KJ, Sinacore JM. History-taking behaviors associated with diagnostic competence of clerks: an exploratory study. Acad Med. 2001;76(10 suppl):S14–7.
Kaplan S, Greenfield S, Ware J. Assessing the effects of physician–patient interactions on the outcomes of chronic disease. Med Care. 1989;275:5110–27.
Kaplan S, Gandek B, Greenfield S, Rogers W, Ware J. Patient and visit characteristics related to physician’s participatory decision-making style. Results from the medical outcomes study. Med Care. 1995;33(12):1176–87.
Levinson W, Mullooly J, Dull V, Frankel R. Physician–patient communication; the relationship with malpractice claims among primary care physicians and surgeons. JAMA. 1997;272:1619–20.
Stewart M. Effective physician–patient communication and health outcomes: a review. Can Med Assoc J. 1995;152(9):1423–33.
ACGME. Outcome Project: ACGME General Competencies. Accreditation Counsel on Graduate Medical Education. Available at: http://www.acgme.org/outcome/comp/compFull.asp. Accessed 23 Jul 2005.
Acknowledgments
The authors gratefully acknowledge Karen Richardson-Nassif, PhD, and Richard Riegelman, MD, PhD for reviewing this manuscript and making valuable suggestions. They also wish to thank Afifa Kouj, PhD for her biostatistical contribution and Laura Abate, MA for her library research. Finally, the authors wish to acknowledge the generous support of The George Washington University Clinical Learning and Simulation Skills (CLASS) Center.
Potential Financial Conflicts of Interest
None disclosed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Blatt, B., Plack, M., Maring, J. et al. Acting on Reflection: the Effect of Reflection on Students’ Clinical Performance on a Standardized Patient Examination. J GEN INTERN MED 22, 49–54 (2007). https://doi.org/10.1007/s11606-007-0110-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11606-007-0110-y