Abstract
Introduction
Obesity and its co-morbidities, including type 2 diabetes (T2DM) and dyslipidemia, are accompanied by excess cardiovascular morbi-mortality. Aside from excess low density lipoprotein-cholesterol (LDL-C), atherogenic dyslipidemia (AD), mainly characterized by elevated triglycerides and decreased high density lipoprotein-cholesterol (HDL-C) levels, is often present in T2DM obese patients. Bariatric surgery, such as Roux-en-Y gastric bypass (RYGB) and sleeve gastrectomy (SG), has become a reference treatment in that population. However, the respective effects of RYGB vs SG on lipid metabolism in T2DM patients have been rarely studied.
Methods
A meta-analysis of randomized controlled trials, comparing the effects of RGYBG vs SG on lipid metabolism 12 months after surgery in T2DM patients, was performed.
Results
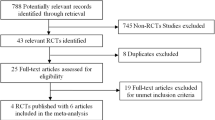
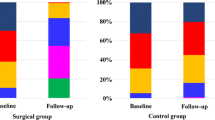
Four studies including a total of 298 patients (151 patients in the RYGB and 147 patients in the SG group) were examined. Despite a greater decrease in body mass index and greater improvement in glycemic control in RYGB compared to SG. RYGB vs SG was more effective in reducing total cholesterol, LDL-C, and non-HDL-C levels (mean difference [MD] −26.10 mg/dL, 95 % CI −38.88 to −13.50, p<0.00001; [MD] −20.10 mg/dL, 95 % CI −27.90 to −12.20, p<0.00001 and MD 31.90 mg/dl, 95 % CI −46.90 to −16.80, p<0.00001, respectively).
Conclusions
The superiority of RYGB vs SG in reducing LDL-C, with an effect comparable to a moderate-intensity statin, suggests RYBG should be favored in hypercholesterolemic T2DM patients in order to further reduce cardiovascular risk.




Similar content being viewed by others
References
Boles A, Kandimalla R, Reddy PH. Dynamics of diabetes and obesity: Epidemiological perspective. Biochim Biophys Acta Mol Basis Dis. 2017;1863(5):1026-1036. doi:https://doi.org/10.1016/j.bbadis.2017.01.016
Henning RJ. Type-2 diabetes mellitus and cardiovascular disease. Future Cardiol. 2018;14(6):491-509. doi:https://doi.org/10.2217/fca-2018-0045
Baigent C, Keech A, Kearney PM, et al. Efficacy and safety of cholesterol-lowering treatment: prospective meta-analysis of data from 90,056 participants in 14 randomised trials of statins. Lancet Lond Engl. 2005;366(9493):1267-1278. doi:https://doi.org/10.1016/S0140-6736(05)67394-1
Stahel P, Xiao C, Nahmias A, Lewis GF. Role of the Gut in Diabetic Dyslipidemia. Front Endocrinol. 2020;11. doi:https://doi.org/10.3389/fendo.2020.00116
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724-1737. doi:https://doi.org/10.1001/jama.292.14.1724
Schauer PR, Kashyap SR, Wolski K, et al. Bariatric surgery versus intensive medical therapy in obese patients with diabetes. N Engl J Med. 2012;366(17):1567-1576. doi:https://doi.org/10.1056/NEJMoa1200225
Cummings DE, Cohen RV. Beyond BMI: the need for new guidelines governing the use of bariatric and metabolic surgery. Lancet Diabetes Endocrinol. 2014;2(2):175-181. doi:https://doi.org/10.1016/S2213-8587(13)70198-0
Borén J, Chapman MJ, Krauss RM, et al. Low-density lipoproteins cause atherosclerotic cardiovascular disease: pathophysiological, genetic, and therapeutic insights: a consensus statement from the European Atherosclerosis Society Consensus Panel. Eur Heart J. 2020;41(24):2313-2330. doi:https://doi.org/10.1093/eurheartj/ehz962
Ceperuelo-Mallafré V, Llauradó G, Keiran N, et al. Preoperative Circulating Succinate Levels as a Biomarker for Diabetes Remission After Bariatric Surgery. Diabetes Care. 2019;42(10):1956-1965. doi:https://doi.org/10.2337/dc19-0114
Lee WJ, Chong K, Ser KH, et al. Gastric bypass vs sleeve gastrectomy for type 2 diabetes mellitus: a randomized controlled trial. Arch Surg Chic Ill 1960. 2011;146(2):143-148. doi:https://doi.org/10.1001/archsurg.2010.326
Murphy R, Clarke MG, Evennett NJ, et al. Laparoscopic Sleeve Gastrectomy Versus Banded Roux-en-Y Gastric Bypass for Diabetes and Obesity: a Prospective Randomised Double-Blind Trial. Obes Surg. 2018;28(2):293-302. doi:https://doi.org/10.1007/s11695-017-2872-6
Hayoz C, Hermann T, Raptis DA, Brönnimann A, Peterli R, Zuber M. Comparison of metabolic outcomes in patients undergoing laparoscopic roux-en-Y gastric bypass versus sleeve gastrectomy - a systematic review and meta-analysis of randomised controlled trials. Swiss Med Wkly. 2018;148:w14633. doi:https://doi.org/10.4414/smw.2018.14633
Liberati A, Altman DG, Tetzlaff J, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700. doi:https://doi.org/10.1136/bmj.b2700
Lally S, Tan CY, Owens D, Tomkin GH. Messenger RNA levels of genes involved in dysregulation of postprandial lipoproteins in type 2 diabetes: the role of Niemann-Pick C1-like 1, ATP-binding cassette, transporters G5 and G8, and of microsomal triglyceride transfer protein. Diabetologia. 2006;49(5):1008-1016. doi:https://doi.org/10.1007/s00125-006-0177-8
Bukoh MX, Siah CJR. A systematic review on the structured handover interventions between nurses in improving patient safety outcomes. J Nurs Manag. 2020;28(3):744-755. doi:https://doi.org/10.1111/jonm.12936
Higgins JPT, Altman DG, Gøtzsche PC, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928. doi:https://doi.org/10.1136/bmj.d5928
Viechtbauer W. Hypothesis tests for population heterogeneity in meta-analysis. Br J Math Stat Psychol. 2007;60(Pt 1):29-60. doi:https://doi.org/10.1348/000711005X64042
Duval S, Tweedie R. Trim and fill: A simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics. 2000;56(2):455-463. doi:https://doi.org/10.1111/j.0006-341x.2000.00455.x
Christou NV, Sampalis JS, Liberman M, et al. Surgery decreases long-term mortality, morbidity, and health care use in morbidly obese patients. Ann Surg. 2004;240(3):416-423; discussion 423-424. doi:https://doi.org/10.1097/01.sla.0000137343.63376.19
Bays HE, Jones PH, Jacobson TA, et al. Lipids and bariatric procedures part 1 of 2: Scientific statement from the National Lipid Association, American Society for Metabolic and Bariatric Surgery, and Obesity Medicine Association: EXECUTIVE SUMMARY. J Clin Lipidol. 2016;10(1):15-32. doi:https://doi.org/10.1016/j.jacl.2015.12.003
Vergès B. Pathophysiology of diabetic dyslipidaemia: where are we? Diabetologia. 2015;58(5):886-899. doi:https://doi.org/10.1007/s00125-015-3525-8
de Carvalho CP, Marin DM, de Souza AL, et al. GLP-1 and adiponectin: effect of weight loss after dietary restriction and gastric bypass in morbidly obese patients with normal and abnormal glucose metabolism. Obes Surg. 2009;19(3):313-320. doi:https://doi.org/10.1007/s11695-008-9678-5
Bays H, Kothari SN, Azagury DE, et al. Lipids and bariatric procedures Part 2 of 2: scientific statement from the American Society for Metabolic and Bariatric Surgery (ASMBS), the National Lipid Association (NLA), and Obesity Medicine Association (OMA). Surg Obes Relat Dis Off J Am Soc Bariatr Surg. 2016;12(3):468-495. doi:https://doi.org/10.1016/j.soard.2016.01.007
Padilla N, Maraninchi M, Béliard S, et al. Effects of bariatric surgery on hepatic and intestinal lipoprotein particle metabolism in obese, nondiabetic humans. Arterioscler Thromb Vasc Biol. 2014;34(10):2330-2337. doi:https://doi.org/10.1161/ATVBAHA.114.303849
Pontiroli AE, Laneri M, Veronelli A, et al. Biliary pancreatic diversion and laparoscopic adjustable gastric banding in morbid obesity: their long-term effects on metabolic syndrome and on cardiovascular parameters. Cardiovasc Diabetol. 2009;8:37. doi:https://doi.org/10.1186/1475-2840-8-37
Benaiges D, Flores-Le-Roux JA, Pedro-Botet J, et al. Impact of restrictive (sleeve gastrectomy) vs hybrid bariatric surgery (Roux-en-Y gastric bypass) on lipid profile. Obes Surg. 2012;22(8):1268-1275. doi:https://doi.org/10.1007/s11695-012-0662-8
Buchwald H, Stoller DK, Campos CT, Matts JP, Varco RL. Partial ileal bypass for hypercholesterolemia. 20- to 26-year follow-up of the first 57 consecutive cases. Ann Surg. 1990;212(3):318-329; discussion 329-331. doi:https://doi.org/10.1097/00000658-199009000-00010
Benetti A, Del Puppo M, Crosignani A, et al. Cholesterol metabolism after bariatric surgery in grade 3 obesity: differences between malabsorptive and restrictive procedures. Diabetes Care. 2013;36(6):1443-1447. doi:https://doi.org/10.2337/dc12-1737
Boyer M, Piché ME, Auclair A, et al. Acute and Chronic Impact of Bariatric Surgery on Plasma LDL Cholesterol and PCSK9 Levels in Patients With Severe Obesity. J Clin Endocrinol Metab. 2017;102(11):4023-4030. doi:https://doi.org/10.1210/jc.2017-00699
Cossu ML, Noya G, Tonolo GC, et al. Duodenal switch without gastric resection: results and observations after 6 years. Obes Surg. 2004;14(10):1354-1359. doi:https://doi.org/10.1381/0960892042583851
Noya G, Cossu ML, Iannuccelli M, Coppola M. Biliopancreatic diversion with pylorus-preserving technique: a new method for the surgical control of hypercholesterolaemia and diabetes II? Panminerva Med. 1997;39(1):35-40.
Gero D, Favre L, Allemann P, Fournier P, Demartines N, Suter M. Laparoscopic Roux-En-Y Gastric Bypass Improves Lipid Profile and Decreases Cardiovascular Risk: a 5-Year Longitudinal Cohort Study of 1048 Patients. Obes Surg. 2018;28(3):805-811. doi:https://doi.org/10.1007/s11695-017-2938-5
Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129(25 Suppl 2):S1-45. doi:https://doi.org/10.1161/01.cir.0000437738.63853.7a
Cannon CP, Blazing MA, Giugliano RP, et al. Ezetimibe Added to Statin Therapy after Acute Coronary Syndromes. N Engl J Med. 2015;372(25):2387-2397. doi:https://doi.org/10.1056/NEJMoa1410489
Silverman MG, Ference BA, Im K, et al. Association Between Lowering LDL-C and Cardiovascular Risk Reduction Among Different Therapeutic Interventions: A Systematic Review and Meta-analysis. JAMA. 2016;316(12):1289-1297. doi:https://doi.org/10.1001/jama.2016.13985
Magno FCCM, Sousa PAM de, Rodrigues MP, et al. Long term maintenance of glucose and lipid concentrations after Roux-en-Y gastric bypass. Arch Endocrinol Metab. 2018;62(3):346-351. doi:https://doi.org/10.20945/2359-3997000000047
Acknowledgments
We are grateful to Lagranja Elena at the Researcher at the CIENM center being part of the faculty of health sciences for performing the systematic search, and we thank for proofreading the manuscript.
Author information
Authors and Affiliations
Contributions
Nogueira Juan Patricio was the main coordinator of the project and was responsible for the study design. Closs Cecilia, Ackerman Marianela, and René Valéro drafted the manuscript of the present paper. Sophie Beliard, Mourre Florian, and Molinero Graciela were involved in the supervising of data collection and stratification. Lobo Martin and Nogueira Juan Patricio contributed to data assembly and analysis. Lavalle-Covos Augusto contributed with manuscript revision. All authors contributed intellectually to this manuscript and have approved this final version.
Corresponding author
Ethics declarations
Ethical Approval
Does not apply.
Informed Consent
Does not apply.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Closs, C., Ackerman, M., Masson, W. et al. Effectiveness of Roux-en-Y Gastric Bypass vs Sleeve Gastrectomy on Lipid Levels in Type 2 Diabetes: a Meta-analysis. J Gastrointest Surg 26, 1575–1584 (2022). https://doi.org/10.1007/s11605-022-05338-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-022-05338-5