Abstract
Background
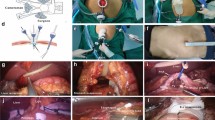
Tumor localization during totally laparoscopic gastrectomy is challenging owing to the invisibility of tumors on the serosal surface. We aimed to evaluate the clinical significance of intra-operative gastroscopy in totally laparoscopic partial gastrectomy.
Methods
We reviewed 1084 gastric cancer patients who underwent either intra- or extracorporeal partial gastrectomy between 2014 and 2018. The intracorporeal group with intra-operative gastroscopy (intra-operative gastroscopy group, n = 187), the intracorporeal group without intra-operative gastroscopy (non-intra-operative gastroscopy group, n = 267), and the extracorporeal group (n = 630) were evaluated for the adequacy of surgical resection margins. We assessed whether total gastrectomy could be avoided according to the performance of intra-operative gastroscopy if the tumor was located within 3–5 cm away from the gastroesophageal junction.
Results
The proximal margin positivity was lesser in the intra-operative gastroscopy group than in the non-intra-operative gastroscopy group (0% versus 2.2%; P = 0.045) but similar to that in the extracorporeal group (0% versus 0.6%; P = 0.579). The number of cases with proximal resection margins < 1 cm was lower in the intra-operative gastroscopy group than in the non-intra-operative gastroscopy group (3.7% versus 9.4%; P = 0.025) but comparable with that in the extracorporeal group (3.7% versus 4.1%; P = 0.815). Among 94 patients with lesions located within 3–5 cm apart from the gastroesophageal junction, the intra-operative gastroscopy group (n = 47) had fewer patients who underwent total gastrectomy than the non-intra-operative gastroscopy group (n = 47) (12.8% versus 44.7%; P = 0.001). Intra-operative gastroscopy was the only independent factor that prevented total gastrectomy (P = 0.001).
Conclusion
Intra-operative gastroscopy can provide margin safety during intracorporeal partial gastrectomy, avoiding unnecessary total gastrectomy.




Similar content being viewed by others
References
Takahashi T, Saikawa Y, Kitagawa Y. Gastric cancer: current status of diagnosis and treatment. Cancers (Basel) 2013;5:48-63.
Han G, Park JY, Kim YJ. Comparison of short-term postoperative outcomes in totally laparoscopic distal gastrectomy versus laparoscopy-assisted distal gastrectomy. J Gastric Cancer 2014;14:105-110.
Ikeda O, Sakaguchi Y, Aoki Y, Harimoto N, Taomoto J, Masuda T, Ohga T, Adachi E, Toh Y, Okamura T, Baba H. Advantages of totally laparoscopic distal gastrectomy over laparoscopically assisted distal gastrectomy for gastric cancer. Surg Endosc 2009;23:2374-2379.
Ikeda T, Kawano H, Hisamatsu Y, Ando K, Saeki H, Oki E, Ohga T, Kakeji Y, Tsujitani S, Kohnoe S, Maehara Y. Progression from laparoscopic-assisted to totally laparoscopic distal gastrectomy: comparison of circular stapler (i-DST) and linear stapler (BBT) for intracorporeal anastomosis. Surg Endosc 2013;27:325-332.
Kinoshita T, Shibasaki H, Oshiro T, Ooshiro M, Okazumi S, Katoh R. Comparison of laparoscopy-assisted and total laparoscopic Billroth-I gastrectomy for gastric cancer: a report of short-term outcomes. Surg Endosc 2011;25:1395-1401.
Lee HJ, Yang HK. Laparoscopic gastrectomy for gastric cancer. Dig Surg 2013;30:132-141.
Song KY, Park CH, Kang HC, Kim JJ, Park SM, Jun KH, Chin HM, Hur H. Is totally laparoscopic gastrectomy less invasive than laparoscopy-assisted gastrectomy?: prospective, multicenter study. J Gastrointest Surg 2008;12:1015-1021.
Hyung WJ, Lim JS, Cheong JH, Kim J, Choi SH, Song SY, Noh SH. Intraoperative tumor localization using laparoscopic ultrasonography in laparoscopic-assisted gastrectomy. Surg Endosc 2005;19:1353-1357.
Kim HI, Hyung WJ, Lee CR, Lim JS, An JY, Cheong JH, Choi SH, Noh SH. Intraoperative portable abdominal radiograph for tumor localization: a simple and accurate method for laparoscopic gastrectomy. Surg Endosc 2011;25:958-963.
Imamura Y, Oki E, Ohgaki K, Nakashima Y, Ando K, Tsutsumi S, Tsurumaru D, Saeki H, Baba H, Maehara Y. Real-time accurate identification of tumor site using a mobile X-ray image-intensifier system during laparoscopic gastrectomy. J Am Coll Surg 2016;222:e1-e7.
. Valenzuela-Salazar C, Rojano-Rodríguez ME, Romero-Loera S, Trejo-Ávila ME, Bañuelos-Mancilla J, Delano-Alonso R, Moreno-Portillo M. Intraoperative endoscopy prevents technical defect related leaks in laparoscopic Roux-en-Y gastric bypass: a randomized control trial. Int J Surg 2018;50:17-21.
Kalmar CL, Reed CM, Peery CL, Salzber AD. Intraluminal indocyanine green for intraoperative staple line leak testing in bariatric surgery. Surg Endosc 2020 May 8. doi: https://doi.org/10.1007/s00464-020-07606-4. Online ahead of print.
Hur H, Son SY, Cho YK, Han SU. Intraoperative gastroscopy for tumor localization in laparoscopic surgery for gastric adenocarcinoma. J Vis Exp 2016:e53170.
Kawakatsu S, Ohashi M, Hiki N, Nunobe S, Nagino M, Sano T. Use of GFS to determine the resection margin during laparoscopic gastrectomy for cancer. Br J Surg 2017;104:1829-1836.
Xuan Y, Hur H, Byun CS, Han SU, Cho YK. Efficacy of intraoperative gastroscopy for tumor localization in totally laparoscopic distal gastrectomy for cancer in the middle third of the stomach. Surg Endosc 2013;27:4364-4370.
Kosuga T, Hiki N, Nunobe S, Noma H, Honda M, Tanimura S, Sano T, Yamaguchi T. Feasibility and nutritional impact of laparoscopy-assisted subtotal gastrectomy for early gastric cancer in the upper stomach. Ann Surg Oncol 2014;21:2028-2035.
Shintani M, Ogawa Y, Ebihara K, Aizawa-Abe M, Miyanaga F, Takaya K, Hayashi T, Inoue G, Hosoda K, Kojima M, Kangawa K, Nakao K. Ghrelin, an endogenous growth hormone secretagogue, is a novel orexigenic peptide that antagonizes leptin action through the activation of hypothalamic neuropeptide Y/Y1 receptor pathway. Diabetes 2001;50:227-232.
Neary NM, Small CJ, Wren AM, Lee JL, Druce MR, Palmieri C, Frost GS, Ghatei MA, Coombes RC, Bloom SR. Ghrelin increases energy intake in cancer patients with impaired appetite: acute, randomized, placebo-controlled trial. J Clin Endocrinol Metab 2004;89:2832-2836.
Cascinu S, Giordani P, Catalano V, Agostinelli R, Catalano G. Resection-line involvement in gastric cancer patients undergoing curative resections: implications for clinical management. Jpn J Clin Oncol 1999;29:291-293.
Morgagni P, Garcea D, Marrelli D, De Manzoni G, Natalini G, Kurihara H, Marchet A, Saragoni L, Scarpi E, Pedrazzani C, Di Leo A, De Santis F, Panizzo V, Nitti D, Roviello F. Resection line involvement after gastric cancer surgery: clinical outcome in nonsurgically retreated patients. World J Surg 2008;32:2661-2667.
Choi JH, Suh YS, Park SH, Kong SH, Lee HJ, Kim WH, Yang HK. Risk factors of microscopic invasion in early gastric cancer. J Gastric Cancer 2017;17:331-341.
Fayers P, Bottomley A, EORTC Quality of Life Group; Quality of Life Unit. Quality of life research within the EORTC-the EORTC QLQ-C30. European Organisation for Research and Treatment of Cancer. Eur J Cancer 2002;38:S125-S133.
Japanese Gastric Cancer Association. Japanese gastric cancer treatment guidelines 2014 (ver. 4). Gastric Cancer 2017;20:1-19.
Park DJ, Lee HJ, Kim SG, Jung HC, Song IS, Lee KU, Choe KJ, Yang HK. Intraoperative gastroscopy for gastric surgery. Surg Endosc 2005;19:1358-1361.
Gunji H, Horibe D, Uesato M, Kano M, Hayano K, Hanari N, Kawahira H, Hayashi H, Matsubara H. Gastric resection under retroflexed endoscopic guidance: a reliable procedure for totally laparoscopic subtotal gastrectomy. Dig Surg 2017;34:12-17.
Park DH, Moon HS, Sul JY, Kwon IS, Yun GY, Lee SH, Kim SH, Sung JK, Lee BS, Jeong HY. Role of preoperative endoscopic clipping in laparoscopic distal gastrectomy for early gastric cancer. Medicine (Baltimore) 2018;97:e13165.
Funding
This study was supported by a grant from the Seoul National University Hospital research fund (grant number 04-2019-3120). The funder had no role in the study design, data analysis, or writing of this article.
Author information
Authors and Affiliations
Contributions
Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work: Shin-Hoo Park, Ji-Ho Park, Tae-Han Kim, Young-Gil Son, Yeon-Ju Huh, Ji-Hyun Park, Jong-Ho Choi, Sa-Hong Kim, Yun-Suhk Suh, Hyunsoo Chung, Seong-Ho Kong, Do Joong Park, Hyuk-Joon Lee, and Han-Kwang Yang
Drafting the work or revising it critically for important intellectual content: Shin-Hoo Park, Jong-Ho Choi, Tae-Han Kim, Ji-Ho Park, Young-Gil Son, Yeon-Ju Huh, Yun-Suhk Suh, Hyunsoo Chung, Seong-Ho Kong, Do Joong Park, and Han-Kwang Yang
Final approval of the version to be published: Shin-Hoo Park, Seong-Ho Kong, Do Joong Park, Hyuk-Joon Lee, and Han-Kwang Yang
Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved: Shin-Hoo Park, Ji-Ho Park, Tae-Han Kim, Yun-Suhk Suh, Hyunsoo Chung, Hyuk-Joon Lee, Seong-Ho Kong, Do Joong Park, and Han-Kwang Yang
Corresponding author
Ethics declarations
Human Rights Statement and Informed Consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later versions. The requirement for written consent was waived by the IRB because of the retrospective nature of this study.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Materials
ESM 1
(PDF 1009 kb)
Rights and permissions
About this article
Cite this article
Park, SH., Lee, HJ., Park, JH. et al. Clinical Significance of Intra-operative Gastroscopy for Tumor Localization in Totally Laparoscopic Partial Gastrectomy. J Gastrointest Surg 25, 1134–1146 (2021). https://doi.org/10.1007/s11605-020-04809-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-020-04809-x