Abstract
Background
High rates of persistent symptoms are found following cholecystectomy in patients with gallstones. The aim of this population based cohort study was to determine which symptoms were associated with the development of clinical gallstone events in a population unaware of their gallstones.
Material and Methods
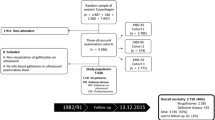
Three random population samples from Copenhagen (N = 6037) were examined with ultrasound during 1982–1994. Participants were not informed about gallstone status. Abdominal symptoms were assessed at baseline through a questionnaire. Follow-up for clinical events was performed through central registers until 2011. Multivariable Cox regression analyses were performed.
Results
Participants unaware of their gallstones (N = 595) were followed for median 17.5 years. A total of 16.6% participants developed clinical events. Both uncomplicated and complicated events were associated with high pain intensity at baseline. Complicated events were also associated with pain at night. Uncomplicated events were associated with pain localized in the epigastrium, of longer duration, and in need of pain medication. No associations were identified for dyspepsia or irritable bowel syndrome.
Conclusions
In a population of unaware gallstone carriers, it was possible to identify abdominal symptoms associated with later clinical detection of the gallstones. These finding may contribute to a better selection of patients for surgery.

Similar content being viewed by others
References
Shabanzadeh DM, Sorensen LT, Jorgensen T. A Prediction Rule for Risk Stratification of Incidentally Discovered Gallstones: Results From a Large Cohort Study. Gastroenterology. 2016;150(1):156-67 e1. doi:10.1053/j.gastro.2015.09.002.
Borly L, Anderson IB, Bardram L, Christensen E, Sehested A, Kehlet H et al. Preoperative prediction model of outcome after cholecystectomy for symptomatic gallstones. Scandinavian journal of gastroenterology. 1999;34(11):1144-52.
Weinert CR, Arnett D, Jacobs D, Jr., Kane RL. Relationship between persistence of abdominal symptoms and successful outcome after cholecystectomy. Archives of internal medicine. 2000;160(7):989-95.
Berger MY, Olde Hartman TC, Bohnen AM. Abdominal symptoms: do they disappear after cholecystectomy? Surgical endoscopy. 2003;17(11):1723-8. doi:10.1007/s00464-002-9154-6.
Lublin M, Crawford DL, Hiatt JR, Phillips EH. Symptoms before and after laparoscopic cholecystectomy for gallstones. Am Surg. 2004;70(10):863-6.
Vetrhus M, Berhane T, Soreide O, Sondenaa K. Pain persists in many patients five years after removal of the gallbladder: observations from two randomized controlled trials of symptomatic, noncomplicated gallstone disease and acute cholecystitis. J Gastrointest Surg. 2005;9(6):826-31. doi:10.1016/j.gassur.2005.01.291.
Halldestam I, Kullman E, Borch K. Defined indications for elective cholecystectomy for gallstone disease. Br J Surg. 2008;95(5):620-6. doi:10.1002/bjs.6020.
Thistle JL, Longstreth GF, Romero Y, Arora AS, Simonson JA, Diehl NN et al. Factors that predict relief from upper abdominal pain after cholecystectomy. Clin Gastroenterol Hepatol. 2011;9(10):891-6. doi:10.1016/j.cgh.2011.05.014.
Osler W. The principles and practice of medicine, designed for the use of practitioners and students of medicine. vol xvii, 1143 p. New York, Appleton: 1909.
Kraag N, Thijs C, Knipschild P. Dyspepsia--how noisy are gallstones? A meta-analysis of epidemiologic studies of biliary pain, dyspeptic symptoms, and food intolerance. Scandinavian journal of gastroenterology. 1995;30(5):411-21.
Berger MY, van der Velden JJ, Lijmer JG, de Kort H, Prins A, Bohnen AM. Abdominal symptoms: do they predict gallstones? A systematic review. Scandinavian journal of gastroenterology. 2000;35(1):70-6.
Jorgensen T. Abdominal symptoms and gallstone disease: an epidemiological investigation. Hepatology (Baltimore, Md ). 1989;9(6):856-60.
Shabanzadeh D, Sørensen L, Jørgensen T. Abdominal Symptoms and Incident Gallstones in a Population Unaware of Gallstone Status. Canadian Journal of Gastroenterology and Hepatology. 2016;2016.
McSherry CK, Ferstenberg H, Calhoun WF, Lahman E, Virshup M. The natural history of diagnosed gallstone disease in symptomatic and asymptomatic patients. Annals of surgery. 1985;202(1):59-63.
Friedman GD, Raviola CA, Fireman B. Prognosis of gallstones with mild or no symptoms: 25 years of follow-up in a health maintenance organization. Journal of clinical epidemiology. 1989;42(2):127-36.
Attili AF, De Santis A, Capri R, Repice AM, Maselli S. The natural history of gallstones: the GREPCO experience. The GREPCO Group. Hepatology. 1995;21(3):655-60.
Festi D, Reggiani ML, Attili AF, Loria P, Pazzi P, Scaioli E et al. Natural history of gallstone disease: Expectant management or active treatment? Results from a population-based cohort study. Journal of gastroenterology and hepatology. 2010;25(4):719-24. doi:10.1111/j.1440-1746.2009.06146.x.
Halldestam I, Enell EL, Kullman E, Borch K. Development of symptoms and complications in individuals with asymptomatic gallstones. The British journal of surgery. 2004;91(6):734-8. doi:10.1002/bjs.4547.
Shabanzadeh DM, Sørensen L, Jørgensen T. Determinants for Clinical Events in Gallstone Carriers Unaware of their Gallstones. Journal of gastroenterology and hepatology. 2016. doi:10.1111/jgh.13531.
Jorgensen T. Prevalence of gallstones in a Danish population. American journal of epidemiology. 1987;126(5):912-21.
Jensen KH, Jorgensen T. Incidence of gallstones in a Danish population. Gastroenterology. 1991;100(3):790-4.
Shabanzadeh DM, Sorensen LT, Jorgensen T. Determinants for gallstone formation - a new data cohort study and a systematic review with meta-analysis. Scandinavian journal of gastroenterology. 2016;51(10):1239-48. doi:10.1080/00365521.2016.1182583.
Shabanzadeh DM, Sorensen LT, Jorgensen T. Gallstone disease and mortality: a cohort study. Int J Public Health. 2016. doi:10.1007/s00038-016-0916-7.
Shabanzadeh DM, Jorgensen T, Linneberg A, Sorensen LT, Skaaby T. Vitamin D and gallstone disease-A population-based study. Endocrine. 2016;54(3):818-25. doi:10.1007/s12020-016-1113-4.
Kay L, Jorgensen T. Redefining abdominal syndromes. Results of a population-based study. Scandinavian journal of gastroenterology. 1996;31(5):469-75.
Fox J. Cox Proportional-Hazards Regression for Survival Data. 2002.
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP et al. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet. 2007;370(9596):1453-7. doi:10.1016/S0140-6736(07)61602-X.
Schmidt M, Sondenaa K, Dumot JA, Rosenblatt S, Hausken T, Ramnefjell M et al. Post-cholecystectomy symptoms were caused by persistence of a functional gastrointestinal disorder. World journal of gastroenterology : WJG. 2012;18(12):1365-72. doi:10.3748/wjg.v18.i12.1365.
Schein CJ, Rosenblatt MA. Biliary calculus size as a factor in prognosis of silent stones. Geriatrics. 1957;12(4):257-60.
Portincasa P, Moschetta A, Palasciano G. Cholesterol gallstone disease. Lancet. 2006;368(9531):230-9. doi:10.1016/S0140-6736(06)69044-2.
Wegstapel H, Bird NC, Chess-Williams R, Johnson AG. The relationship between in vivo emptying of the gallbladder, biliary pain, and in vitro contractility of the gallbladder in patients with gallstones: Is biliary colic muscular in origin? Scandinavian journal of gastroenterology. 1999;34(4):421-5.
Festi D, Sottili S, Colecchia A, Attili A, Mazzella G, Roda E et al. Clinical manifestations of gallstone disease: evidence from the multicenter Italian study on cholelithiasis (MICOL). Hepatology. 1999;30(4):839-46. doi:10.1002/hep.510300401.
Portincasa P, Di Ciaula A, Palmieri V, Velardi A, VanBerge-Henegouwen GP, Palasciano G. Impaired gallbladder and gastric motility and pathological gastro-oesophageal reflux in gallstone patients. Eur J Clin Invest. 1997;27(8):653-61.
Buxbaum KL. Bile Gastritis Occurring after Cholecystectomy. American Journal of Gastroenterology. 1982;77(5):305-11.
Svensson JO, Gelin J, Svanvik J. Gallstones, cholecystectomy, and duodenogastric reflux of bile acid. Scandinavian journal of gastroenterology. 1986;21(2):181-7.
Eyrebrook IA, Smythe A, Bird NC, Mangnall Y, Johnson AG. Relative Contribution of Bile and Pancreatic-Juice Duodenogastric Reflux in Gastric-Ulcer Disease and Cholelithiasis. Brit J Surg. 1987;74(8):721-5. doi:DOI 10.1002/bjs.1800740823.
Chen MF, Wang CS. A prospective study of the effect of cholecystectomy on duodenogastric reflux in humans using 24 hour gastric hydrogen monitoring. Surgery, gynecology & obstetrics. 1992;175(1):52-6.
Wilson P, Jamieson JR, Hinder RA, Anselmino M, Perdikis G, Ueda RK et al. Pathologic duodenogastric reflux associated with persistence of symptoms after cholecystectomy. Surgery. 1995;117(4):421-8.
Kuran S, Parlak E, Aydog G, Kacar S, Sasmaz N, Ozden A et al. Bile reflux index after therapeutic biliary procedures. BMC gastroenterology. 2008;8:4. doi:10.1186/1471-230X-8-4.
Brough WA, Taylor TV, Torrance HB. The Surgical Factors Influencing Duodenogastric Reflux. Brit J Surg. 1984;71(10):770-3. doi:DOI 10.1002/bjs.1800711011.
Lorusso D, Pezzolla F, Cavallini A, Messa C, Giorgio P, Caruso ML et al. A Prospective-Study on Duodenogastric Reflux and on Histological-Changes in Gastric-Mucosa after Cholecystectomy. Gastroenterologie clinique et biologique. 1992;16(4):328-33.
Aprea G, Canfora A, Ferronetti A, Giugliano A, Guida F, Braun A et al. Morpho-functional gastric pre-and post-operative changes in elderly patients undergoing laparoscopic cholecystectomy for gallstone related disease. BMC surgery. 2012;12 Suppl 1:S5. doi:10.1186/1471-2482-12-S1-S5.
Konsten J, Gouma DJ, von Meyenfeldt MF, Menheere P. Long-term follow-up after open cholecystectomy. The British journal of surgery. 1993;80(1):100-2.
Lorusso D, Porcelli P, Pezzolla F, Lantone G, Zivoli G, Guerra V et al. Persistent dyspepsia after laparoscopic cholecystectomy. The influence of psychological factors. Scandinavian journal of gastroenterology. 2003;38(6):653-8. doi:10.1080/00365520310002995.
Mertens MC, Roukema JA, Scholtes VP, De Vries J. Risk assessment in cholelithiasis: is cholecystectomy always to be preferred? Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2010;14(8):1271-9. doi:10.1007/s11605-010-1219-6.
Corazziari E, Attili AF, Angeletti C, De Santis A. Gallstones, cholecystectomy and irritable bowel syndrome (IBS) MICOL population-based study. Digestive and liver disease : official journal of the Italian Society of Gastroenterology and the Italian Association for the Study of the Liver. 2008;40(12):944-50. doi:10.1016/j.dld.2008.02.013.
McNally MA, Locke GR, Zinsmeister AR, Schleck CD, Peterson J, Talley NJ. Biliary events and an increased risk of new onset irritable bowel syndrome: a population-based cohort study. Alimentary pharmacology & therapeutics. 2008;28(3):334-43.
Kirk G, Kennedy R, McKie L, Diamond T, Clements B. Preoperative symptoms of irritable bowel syndrome predict poor outcome after laparoscopic cholecystectomy. Surgical endoscopy. 2011;25(10):3379-84. doi:10.1007/s00464-011-1729-7.
Acknowledgements
We would like to thank Anja Lykke Madsen for data management.
Grant Support
This study was financially supported by the Faculty of Health and Medical Sciences at the University of Copenhagen
Author Contributions
Daniel Mønsted Shabanzadeh: design, data analysis, interpretation of data, drafting of manuscript, and approval of final manuscript. Lars Tue Sørensen: design, interpretation of data, critical revision of manuscript, and approval of final manuscript. Torben Jørgensen: design, acquisition of data, interpretation of data, critical revision of manuscript, and approval of final manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Informed consent was obtained from all participants before enrollment into the study.
Rights and permissions
About this article
Cite this article
Shabanzadeh, D.M., Sørensen, L.T. & Jørgensen, T. Which Abdominal Symptoms are Associated with Clinical Events in a Population Unaware of Their Gallstones? a Cohort Study. J Gastrointest Surg 21, 831–839 (2017). https://doi.org/10.1007/s11605-016-3349-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-016-3349-y