Abstract
Background
In 2011, a new European Staging System (ESS) for perihilar cholangiocarcinoma (PHC) was proposed with the expressed purpose of comparing treatment and outcomes data between institutions. The goal of this study was to evaluate the feasibility of ESS data capture.
Study Design
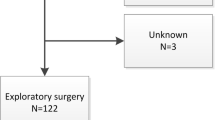
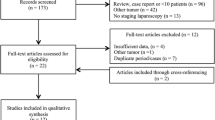
Forty-seven consecutive patients who underwent surgical resection for PHC between 1999 and 2013 were studied. Demographic variables, components of various staging systems (including the ESS), preoperative and perioperative details, pathology, and outcomes were recorded.
Results
The mean patient age was 63.2 and 62 % were male. Preoperative imaging included high-resolution CT in all patients, MRI in 34 %, and PET in 11 %. R0 resection was accomplished in 80 % of patients. Four patients (8.5 %) and 18 patients (38.3 %), respectively, received neoadjuvant or adjuvant therapy. During a mean follow-up of 36 months, recurrence rate was 51.3 % and 2- and 5-year survival rates were 69.4 and 33.3 %, respectively. Analysis of data capture found that tumor (T) classification was indeterminable in 7/47 patients (14.9 %). For two patients, the form (F) designation had insufficient data. The extent of vascular involvement (PV/HA) was different compared to preoperative imaging in nine patients (19.1 %). The liver remnant volume (V) was calculated in only 18 patients (38.3 %). The liver disease (D) variable did not account for four patients with inflammation/cirrhosis. In total, only 15 patients (31.9 %) had all required elements to complete the ESS.
Conclusions
Without templated radiology, surgery, and pathology reports, the ESS cannot be applied to current clinical/research practice. Although resection continues to provide significant survival benefit to patients with perihilar cholangiocarcinoma, lack of an accurate prognostic tool for resectability and outcomes continues to be a major impediment to progress in the field.
Similar content being viewed by others
References
Kamakamba A, DeOliveira ML. Perihilar Cholangiocarcinoma: Paradigms of surgical management. Am J Surg 2012; 208:563–570.
Nakeeb A, Pitt HA, Sohn TA, et al. Cholangiocarcinoma. A spectrum of intrahepatic, perihilar and distal tumors. Ann Surg 1996; 224:463–473.
Parikh AA, Abdalla EK, Vauthey JN. Operative considerations in resection of hilar cholangiocarcinoma. HPB, 2005; 7:254–258.
Nagino M, Ebata T, Yokoyama Y et al. Evolution of surgical treatment for perihilar cholangiocarcinoma: A single-center 34-year review of 574 consecutive resections. Ann Surg 2013; 258:129–140.
Bismuth H, Corlette MB. Intrahepatic cholangioenteric anastomosis in carcinoma of the hilus of the liver. Surg Gynecol Obstet 1975; 140:170–176.
Jarnagin WR, Fong Y, DeMatteo RP, et al. Staging, resectability, and outcome in 225 patients with hilar cholangiocarcinoma. Ann. Surg 2001; 234:507–519.
Edge SB. (2010) AJCC Cancer Staging Manual, 7th edn. New York: Springer.
DeOliveira ML, Schulick RD, Nimura Y, et al. New staging system and a registry for perihilar cholangiocarcinoma. Hepatology 2011; 53:1363–1371.
Masato Nagino. A much needed but imperfect new staging system. Nat Rev Gastroenterol Hepatol. 2011; 8(5):252–3.
Masato Nagino. Perihilar Cholangiocarcinoma: A surgeon’s viewpoint on current topics. J Gastroenterol 2012; 47:1165–1176.
Koerkamp BG, Wiggers JK, Allen PJ, et al. American Joint Committee on Cancer staging for resected perihilar cholangiocarcinoma: a comparison of the 6th and 7th editions. HPB 2014 Sept 29; Epub.
Sano T, Shimada, K Sakamoto Y et al. Prognosis of Perihilar Cholangiocarcinoma: Hilar bile duct cancer versus intrahepatic cholangiocarcinoma involving the hepatic hilus. Ann Surg Oncol 2007; 12(22):590–599.
Aloia TA, Charnsangavej C, Faria S et al. High-resolution computed tomography accurately predicts resectability in hilar cholangiocarcinoma.
Palavecino M, Abdalla EK, Madoff DC, et al. Portal vein embolization in hilar cholangiocarcinoma. Surg Oncol Clin N Am 18 2009; 257–267.
Vauthey JN, Chaoui A, Do KA, et al. Standardized measurement of the future liver remnant prior to extended liver resection: methodology and clinical associations. Surgery 2000;127(5):512–9.
Guglielmi A, Ruzzenente A, Campagnaro T, et al. Does intrahepatic cholangiocarcinoma have better prognosis compared to perihilar cholangiocarcinoma? J Surg Oncol 2010; 101:111–115.
Koerkamp BG, Fong Y. Outcomes in biliary malignancy. J Surg Oncol 2014; 110:585–591.
DeOliveira ML, Cunningham SC, Cameron JL et al. Cholangiocarcinoma: Thirty-one-year experience with 564 patients at a single institution. Ann Surg 2007; 245:755–762.
Ito F, Agni R, Rettamel R, et al. Resection of hilar cholangiocarcinoma: Concomitant liver resection decreases hepatic recurrence. Ann Surg 2008; 248(2):273–279.
Lu DS, Reber HA, Krasny RM, et al. Local staging of pancreatic cancer: criteria for unresectability of major vessels as revealed by pancreatic-phase, thin-section helical CT. Am J Roentgenol 1997;168:1439–1443.
Okumoto T, Sato A, Yamada T, et al. Correct diagnosis of vascular encasement and longitudinal extension of hilar cholangiocarcinoma by four-channel multidetector-row computed tomograpy. Tohoku J Exp Med 2009;217:1–8.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ismael, H.N., Loyer, E., Kaur, H. et al. Evaluating the Clinical Applicability of the European Staging System for Perihilar Cholangiocarcinoma. J Gastrointest Surg 20, 741–747 (2016). https://doi.org/10.1007/s11605-016-3075-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-016-3075-5