Abstract
Background
There is increasing need to expand availability of donor liver grafts, including steatotic livers. Steatotic liver is associated with poor outcome post-transplantation but with conflicting results in the literature. The aim of this systematic review was to evaluate the impact of steatotic livers on liver transplantation outcomes.
Methods
An electronic search of OVID Medline and Embase databases was performed to identify clinical studies that reported outcomes of steatotic livers in liver transplantation. Data were extracted, and basic descriptive statistics were used to summarise data pooled from individual clinical studies.
Results
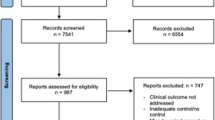
Ninety-two articles were identified, of which 34 met the inclusion criteria, and stratified analysis were performed. There was a lack of standardised definition of primary non-function or impaired primary function amongst the studies and description of type of steatosis. Severely (>60 %) steatotic grafts are associated with increased risk of poor graft function, whilst moderate–severe (>30 %) steatotic grafts are associated with decreased graft survival.
Conclusions
Available evidence showed increased risk of poor graft outcome in moderate–severe steatotic livers. A large prospective multi-centred trial will be required to identify the true risks of steatotic livers. Consistent definition of primary non-function/impaired primary function and description of type of steatosis is also required.

Similar content being viewed by others
Abbreviations
- ALT:
-
Alanine aminotransferase
- AST:
-
Aspartate aminotransferase
- CaCo:
-
Case–control study
- CaR:
-
Case report
- Co:
-
Cohort study
- DCD:
-
Donation after circulatory death
- DNF:
-
Delayed non-function
- EAD:
-
Early allograft dysfunction
- ECD:
-
Extended criteria donor
- EGD:
-
Early graft dysfunction
- INR:
-
International normalised ratio
- IPF:
-
Impaired primary function
- MELD:
-
Model for End-Stage Liver Disease
- ns:
-
Not stated
- OLT:
-
Orthotopic liver transplantation
- P:
-
Prospective
- PDF:
-
Primary dysfunction of graft
- PNF:
-
Primary non-function
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-analyses
- PT:
-
Prothrombin time
- PTA:
-
Prothrombin time activity
- PTT:
-
Partial thromboplastin time
- Re:
-
Retrospective
- RR:
-
Relative risk
- SGOT:
-
Serum glutamic oxaloacetic transaminases
References
Fishbein TM, Fiel MI, Emre S, Cubukcu O, Guy SR, Schwartz ME, Miller CM, Sheiner PA. Use of livers with microvesicular fat safely expands the donor pool. Transplantation. 1997;64(2):248–51.
Durand F, Renz JF, Alkofer B, Burra P, Clavien P-A, Porte RJ, Freeman RB, Belghiti J. Report of the Paris consensus meeting on expanded criteria donors in liver transplantation. Liver Transpl. 2008;14(12):1694–707.
Tector AJ, Mangus RS, Chestovich P, Vianna R, Fridell JA, Milgrom ML, Sanders C, Kwo PY. Use of extended criteria livers decreases wait time for liver transplantation without adversely impacting posttransplant survival. Ann Surg. 2006;244(3):439–50.
Renz JF, Kin C, Kinkhabwala M, Jan D, Varadarajan R, Goldstein M, Brown R, Jr., Emond JC. Utilization of extended donor criteria liver allografts maximizes donor use and patient access to liver transplantation. Ann Surg. 2005;242(4):556–63; discussion 63–5.
Todo S, Demetris AJ, Makowka L, Teperman L, Podesta L, Shaver T, Tzakis A, Starzl TE. Primary nonfunction of hepatic allografts with preexisting fatty infiltration. Transplantation. 1989;47(5):903–5.
D’Alessandro AM, Kalayoglu M, Sollinger HW, Hoffmann RM, Reed A, Knechtle SJ, Pirsch JD, Hafez GR, Lorentzen D, Belzer FO. The predictive value of donor liver biopsies for the development of primary nonfunction after orthotopic liver transplantation. Transplantation. 1991;51(1):157–63.
Ploeg RJ, D’Alessandro AM, Knechtle SJ, Stegall MD, Pirsch JD, Hoffmann RM, Sasaki T, Sollinger HW, Belzer FO, Kalayoglu M. Risk factors for primary dysfunction after liver transplantation—a multivariate analysis. Transplantation. 1993;55(4):807–13.
Yoong KF, Gunson BK, Neil DAH, Mirza DF, Mayer AD, Buckels JAC, McMaster P. Impact of donor liver microvesicular steatosis on the outcome of liver retransplantation. Transplant Proc. 1999;31(1–2):550–1.
Dare AJ, Phillips ARJ, Chu M, Hickey AJR, Bartlet ASJR. Appraisal of donor steatosis in liver transplantation: a survey of current practice in Australia and New Zealand. Transplant Research and Risk Management. 2012;4:31–7.
Imber CJ, St. Peter SD, Lopez I, Guiver L, Friend PJ. Current practice regarding the use of fatty livers: atrans-Atlantic survey. Liver Transpl. 2002;8(6):545–9.
Rey JW, Wirges U, Dienes HP, Fries JWU. Hepatic steatosis in organ donors: disparity between surgery and histology? Transplant Proc. 2009;41(6):2557–60.
Stahl JE, Kreke JE, Malek FAA, Schaefer AJ, Vacanti J. Consequences of cold-ischemia time on primary nonfunction and patient and graft survival in liver transplantation: a meta-analysis. PLoS ONE. 2008;3(6):e2468.
Todo S, Nery J, Yanaga K, Podesta L, Gordon RD, Starzl TE. Extended preservation of human liver grafts with UW solution. Jama. 1989;261(5):711–4.
Strasberg SM, Howard TK, Molmenti EP, Hertl M. Selecting the donor liver: risk factors for poor function after orthotopic liver transplantation. Hepatology. 1994;20(4 Pt 1):829–38.
Chavin KD, Taber DJ, Norcross M, Pilch NA, Crego H, McGillicuddy JW, Bratton CF, Lin A, Baliga PK. Safe use of highly steatotic livers by utilizing a donor/recipient clinical algorithm. Clin Transplant. 2013;27(5):732–41.
Gabrielli M, Moisan F, Vidal M, Duarte I, Jimenez M, Izquierdo G, Dominguez P, Mendez J, Soza A, Benitez C, Perez R, Arrese M, Guerra J, Jarufe N, Martinez J. Steatotic livers. Can we use them in OLTX? Outcome data from a prospective baseline liver biopsy study. Ann Hepatol. 2012;11(6):891–8.
Teng DH, Zhu ZJ, Zheng H, Deng YL, Sun LY, Pan C, Liu YH, Song HL, Shen ZY. Effect of steatosis donor liver transplantation on hepatocellular carcinoma recurrence: experience at a single institution. Hepatogastroenterology. 2012;59(115):858–62.
de Graaf EL, Kench J, Dilworth P, Shackel NA, Strasser SI, Joseph D, Pleass H, Crawford M, McCaughan GW, Verran DJ. Grade of deceased donor liver macrovesicular steatosis impacts graft and recipient outcomes more than the Donor Risk Index. J Gastroenterol Hepatol. 2012;27(3):540–6.
Sharkey FE, Lytvak I, Prihoda TJ, Speeg KV, Washburn WK, Halff GA. High-grade microsteatosis and delay in hepatic function after orthotopic liver transplantation. Hum Pathol. 2011;42(9):1337–42.
Deroose JP, Kazemier G, Zondervan P, Ijzermans JNM, Metselaar HJ, Alwayn IPJ. Hepatic steatosis is not always a contraindication for cadaveric liver transplantation. Hpb. 2011;13(6):417–25.
Spitzer AL, Lao OB, Dick AAS, Bakthavatsalam R, Halldorson JB, Yeh MM, Upton MP, Reyes JD, Perkins JD. The biopsied donor liver: incorporating macrosteatosis into high-risk donor assessment. Liver Transpl. 2010;16(7):874–84.
Doyle MBM, Vachharajani N, Wellen JR, Anderson CD, Lowell JA, Shenoy S, Brunt EM, Chapman WC. Short- and long-term outcomes after steatotic liver transplantation. Archives of Surgery. 2010;145(7):653–60.
Noujaim HM, de Ville de Goyet J, Montero EFS, Ribeiro CMF, Capellozzi VL, Crescentini F, Casagrande M, Santos RG, Curvello L, de Miranda MP, Genzini T. Expanding postmortem donor pool using steatotic liver grafts: a new look. Transplantation. 2009;87(6):919–25.
Li J, Liu B, Yan LN, Zuo YX, Li B, Zeng Y, Zhang SF, Li FG. Reversal of graft steatosis after liver transplantation: prospective study. Transplant Proc. 2009;41(9):3560–3.
Gao F, Xu X, Ling Q, Wu J, Zhou L, Xie H-Y, Wang H-P, Zheng S-S. Efficacy and safety of moderately steatotic donor liver in transplantation. Hepatobiliary Pancreat Dis Int. 2009;8(1):29–33.
Frongillo F, Avolio AW, Nure E, Mule A, Pepe G, Magalini SC, Agnes S. Quantification of degree of steatosis in extended criteria donor grafts with standardized histologic techniques: implications for graft survival. Transplant Proc. 2009;41(4):1268–72.
Fiorentino M, Vasuri F, Ravaioli M, Ridolfi L, Grigioni WF, Pinna AD, D’Errico-Grigioni A. Predictive value of frozen-section analysis in the histological assessment of steatosis before liver transplantation. Liver Transpl. 2009;15(12):1821–5.
Burra P, Loreno M, Russo FP, Germani G, Galligioni A, Senzolo M, Cillo U, Zanus G, Fagiuoli S, Rugge M. Donor livers with steatosis are safe to use in hepatitis C virus-positive recipients. Liver Transpl. 2009;15(6):619–28.
Reddy MS, Bhati C, Neil D, Mirza DF, Manas DM. National Organ Retrieval Imaging System: results of the pilot study. Transpl Int. 2008;21(11):1036–44.
Muscari F, Guinard JP, Foppa B, Trocard P, Danjoux M, Kamel MS, Duffas JP, Rostaing L, Fourtanier G, Suc B. Biological changes after liver transplantation according to the presence or not of graft steatosis. Transplant Proc. 2008;40(10):3562–5.
Angele MK, Rentsch M, Hartl WH, Wittmann B, Graeb C, Jauch KW, Loehe F. Effect of graft steatosis on liver function and organ survival after liver transplantation. American Journal of Surgery. 2008;195(2):214–20.
Nikeghbalian S, Nejatollahi SMR, Salahi H, Bahador A, Sabet B, Jalaeian H, Geramizadeh B, Dehghani SM, Malek-Hosseini SA. Does donor’s fatty liver change impact on early mortality and outcome of liver transplantation. Transplant Proc. 2007;39(4):1181–3.
McCormack L, Petrowsky H, Jochum W, Mullhaupt B, Weber M, Clavien PA. Use of severely steatotic grafts in liver transplantation: a matched case–control study. Ann Surg. 2007;246 (6):940–6.
Perez-Daga JA, Santoyo J, Suarez MA, Fernandez-Aguilar JA, Ramirez C, Rodriguez-Canete A, Aranda JM, Sanchez-Perez B, Montiel C, Palomo D, Ruiz M, Mate A. Influence of degree of hepatic steatosis on graft function and postoperative complications of liver transplantation. Transplant Proc. 2006;38 (8):2468–70.
Briceno J, Padillo J, Rufian S, Solorzano G, Pera C. Assignment of steatotic livers by the Mayo model for end-stage liver disease. Transpl Int. 2005;18(5):577–83.
Marsman H, Matsushita T, Dierkhising R, Kremers W, Rosen C, Burgart L, Nyberg SL. Assessment of donor liver steatosis: pathologist or automated software? Hum Pathol. 2004;35(4):430–5.
Afonso RC, Saad WA, Parra OM, Leitao R, Ferraz-Neto BH. Impact of steatotic grafts on initial function and prognosis after liver transplantation. Transplant Proc. 2004;36(4):909–11.
Verran D, Kusyk T, Painter D, Fisher J, Koorey D, Strasser S, Stewart G, McCaughan G, Verran D, Kusyk T, Painter D, Fisher J, Koorey D, Strasser S, Stewart G, McCaughan G. Clinical experience gained from the use of 120 steatotic donor livers for orthotopic liver transplantation. Liver Transpl. 2003;9(5):500–5.
Salizzoni M, Franchello A, Zamboni F, Ricchiuti A, Cocchis D, Fop F, Brunati A, Cerutti E. Marginal grafts: finding the correct treatment for fatty livers. Transpl Int. 2003;16(7):486–93.
Rull R, Vidal O, Momblan D, Xavier Gonzalez F, Lopez-Boado MA, Fuster J, Grande L, Bruguera M, Cabrer K, Garcia-Valdecasas JC. Evaluation of potential liver donors: limits imposed by donor variables in liver transplantation. Liver Transpl. 2003;9 (4):389–93.
Busquets J, Figueras J, Serrano T, Torras J, Ramos E, Rafecas A, Fabregat J, Lama C, Xiol X, Baliellas C, Jaurrieta E. Postreperfusion biopsies are useful in predicting complications after liver transplantation. Liver Transpl. 2001;7(5):432–5.
De Carlis L, Colella G, Sansalone CV, Aseni P, Rondinara GF, Slim AO, Di Benedetto F, Giacomoni A, Fesce R, Forti D. Marginal donors in liver transplantation: the role of donor age. Transplant Proc. 1999;31(1–2):397–400.
Canelo R, Braun F, Sattler B, Klinge B, Lorf T, Ramadori G, Ringe B. Is a fatty liver dangerous for transplantation? Transplant Proc. 1999;31(1–2):414–5.
Urena MA, Ruiz-Delgado FC, Gonzalez EM, Segurola CL, Romero CJ, Garcia IG, Gonzalez-Pinto I, Gomez Sanz R. Assessing risk of the use of livers with macro and microsteatosis in a liver transplant program. Transplant Proc. 1998;30(7):3288–91.
Marsman WA, Wiesner RH, Rodriguez L, Batts KP, Porayko MK, Hay JE, Gores GJ, Krom RAF. Use of fatty donor liver is associated with diminished early patient and graft survival. Transplantation. 1996;62(9):1246–51.
Markin RS, Wisecarver JL, Radio SJ, Stratta RJ, Langnas AN, Hirst K, Shaw BW, Jr. Frozen section evaluation of donor livers before transplantation. Transplantation. 1993;56(6):1403–9.
Adam R, Reynes M, Johann M, Morino M, Astarcioglu I, Kafetzis I, Castaing D, Bismuth H. The outcome of steatotic grafts in liver transplantation. Transplant Proc. 1991;23(1 Pt 2):1538–40.
Makowka L, Gordon RD, Todo S, Ohkohchi N, Marsh JW, Tzakis AG, Yokoi H, Ligush J, Esquivel CO, Satake M, et al. Analysis of donor criteria for the prediction of outcome in clinical liver transplantation. Transplant Proc. 1987;19(1 Pt 3):2378–82.
Busuttil RW, Tanaka K. The utility of marginal donors in liver transplantation. Liver Transpl. 2003;9(7):651–63.
McCormack L, Dutkowski P, El-Badry AM, Clavien P-A. Liver transplantation using fatty livers: always feasible? Journal of Hepatology. 2011;54(5):1055–62.
Kocbiyik A, Demirhan B, Sevmis S, Budakoglu I, Karakayali H, Haberal M. Role of postreperfusion subcapsular wedge biopsies in predicting initially poor graft function after liver transplantation. Transplant Proc. 2009;41(7):2747–8.
Ferraz-Neto BH, Zurstrassen MP, Hidalgo R, Fonseca LE, Motta TD, Pandullo FL, Rezende MB, Meira-Filho SP, Sa JR, Afonso RC, Zurstrassen MPVC, Fonseca LEP, Motta TDB. Donor liver dysfunction: application of a new scoring system to identify the marginal donor. Transplant Proc. 2007;39(8):2516–8.
Portmann B, Wight D. Pathology of liver transplantation. In: Calne R (ed). Liver transplantation. New York: Grune & Stratton. 1987. p. 437–70.
Nocito A, El-Badry AM, Clavien PA. When is steatosis too much for transplantation? Journal of Hepatology. 2006;45(4):494–9.
Angulo P. Nonalcoholic fatty liver disease and liver transplantation. Liver Transpl. 2006;12(4):523–34.
Jarnagin WR, Gonen M, Fong Y, DeMatteo RP, Ben-Porat L, Little S, Corvera C, Weber S, Blumgart LH, Nagorney DM. Improvement in perioperative outcome after hepatic resection: analysis of 1,803 consecutive cases over the past decade. Ann Surg. 2002;236(4):397–407.
Vetelainen R, van Vliet A, Gouma DJ, van Gulik TM. Steatosis as a risk factor in liver surgery. Ann Surg. 2007;245(1):20–30.
El-Badry AM, Breitenstein S, Jochum W, Washington K, Paradis V, Rubbia-Brandt L, Puhan MA, Slankamenac K, Graf R, Clavien PA, El-Badry AM, Breitenstein S, Jochum W, Washington K, Paradis V, Rubbia-Brandt L, Puhan MA, Slankamenac K, Graf R, Clavien P-A. Assessment of hepatic steatosis by expert pathologists: the end of a gold standard. Ann Surg. 2009;250(5):691–7.
Chen H, Xie J, Shen B, Deng X, Tao R, Peng C, Li H. Initial poor graft dysfunction and primary graft non-function after orthotopic liver transplantation. In: Mizuguchi DY, editor. Liver biopsy in modern medicine 2011. Rijeka, Croatia: InTech.
Acknowledgements
This work was directly supported by the University of Auckland Faculty Research Development Fund, Maurice Wilkins Centre for Biodiscovery and the Maurice & Phyllis Paykel Trust.
Author information
Authors and Affiliations
Corresponding author
Additional information
Michael J. J. Chu and Anna J. Dare contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Table S1
(DOCX 625 kb)
Rights and permissions
About this article
Cite this article
Chu, M.J.J., Dare, A.J., Phillips, A.R.J. et al. Donor Hepatic Steatosis and Outcome After Liver Transplantation: a Systematic Review. J Gastrointest Surg 19, 1713–1724 (2015). https://doi.org/10.1007/s11605-015-2832-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-015-2832-1