Abstract
Background
In China, great efforts are dedicated to reducing discomfort and minimizing undesirable complications for patients undergoing upper gastrointestinal (UGI) endoscopy.
Methods
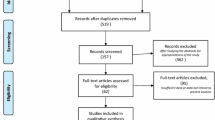
This study was conducted to compare the diagnostic accuracy, safety, complications, and patient and examiner satisfaction for different sedation approaches. We carried out a prospective and randomized study on 450 patients undergoing diagnostic UGI endoscopy. During the procedure, patients received N2O by inhalation; an intravenous mixture of midazolam, remifentanil, and propofol; or no sedative. The cardiorespiratory functions, procedure duration, recovery time, length of hospital stay, complications, and ratings of patient and examiner satisfaction were recorded.
Results
Compared to those deeply sedated, patients inhaling N2O had comparable diagnostic accuracy, significantly shorter procedure and recovery times, a lower risk of cardiorespiratory distress, but a higher number of minor complications and post-procedure mental issues. The procedural satisfaction ratings were highest for those receiving deep sedation; fewer patients reported willingness to reconsider N2O for a future upper GI endoscopy. The lowest satisfaction rating was given by those who received no sedation.
Conclusions
Multiple factors should be considered before selecting N2O as the sedative for diagnostic UGI endoscopy, including the patient’s economic status, potential risk of cardiorespiratory distress, and sensitivity to potential adverse effects of N2O administration.
Similar content being viewed by others
References
Evans LT, Saberi S, Kim HM, et al. Pharyngeal anesthesia during sedated EGDs: is "the spray" beneficial? A meta-analysis and systematic review. Gastrointest Endosc 2006;63:761–6.
Gross BJ, Bailey LP, Connis TR, et al. Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology 2002;96:1004–17.
Jung M, Hofmann C, Kiesslich R, et al. Improved sedation in diagnostic and therapeutic ERCP: propofol is an alternative to midazolam. Endoscopy 2000;32:233–8.
Wehrmann T, Kokabpick S, Lembcke B, et al. Efficacy and safety of intravenous propofol sedation during routine ERCP: a prospective, controlled study. Gastrointest Endosc 1999;49:677–83.
Lazzaroni M, Bianchi Porro G. Preparation, premedication, and surveillance. Endoscopy 2005;37:101–9.
Forbes GM, Collins BJ. Nitrous oxide for colonoscopy: a randomized controlled study. Gastrointest Endosc 2000;51:271–7.
Notini-Gudmarsson AK, Dolk A, Jakobsson J, et al. Nitrous oxide: a valuable alternative for pain relief and sedation during routine colonoscopy. Endoscopy 1996;28:283–7.
Welchman S, Cochrane S, Minto G, et al. Systematic review: the use of nitrous oxide gas for lower gastrointestinal endoscopy. Aliment Pharmacol Ther 2010;32:324–33.
Ramsay MA, Savege TM, Simpson BR, et al. Controlled sedation with alphaxalone-alphadolone. Br Med J 1974;2:656–9.
Bell GD. Preparation, premedication, and surveillance. Endoscopy 2004;36:23–31.
Fanti L, Testoni PA. Sedation and analgesia in gastrointestinal endoscopy: what's new? World J Gastroenterol 2010;16:2451–7.
Michaud L, Gottrand F, Ganga-Zandzou PS, et al. Nitrous oxide sedation in pediatric patients undergoing gastrointestinal endoscopy. J Pediatr Gastroenterol Nutr 1999;28(3):310–4.
Rao AS, Baron TH. Endoscopy: Nitrous oxide sedation for colonoscopy-no laughing matter. Nat Rev Gastroenterol Hepatol 2010;7:539–41.
Lichtenstein DR, Jagannath S, Baron TH, et al. Sedation and anesthesia in GI endoscopy. Gastrointest Endosc 2008;68:815–26.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lan, C., Shen, X., Cui, H. et al. Comparison of Nitrous Oxide to No Sedation and Deep Sedation for Diagnostic Upper Gastrointestinal Endoscopy. J Gastrointest Surg 17, 1066–1072 (2013). https://doi.org/10.1007/s11605-013-2160-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-013-2160-2