Abstract
Objective
There is currently no objective quantification of the temporal changes in performance associated with a novice surgeon learning single-incision laparoscopic surgery (SILS) operative tasks. Analysing learning curves allows us to objectively quantify performance. The aim was to evaluate if the rate of learning and ultimate proficiency level reached in SILS when using straight or articulating instruments is different to conventional laparoscopy and if training in laparoscopy influences learning or proficiency for SILS.
Design and Setting
Thirty-six surgically naive medical students were randomised to complete the validated peg transfer task over 50 repetitions using a conventional laparoscopic set-up, SILS set-up with straight instruments or articulated instruments or SILS set-up after having reached proficiency using a conventional laparoscopy.
Results
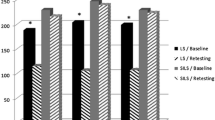
There was a significant increased overall proficiency between the group trained in conventional laparoscopy and all other groups (p < 0.01), with no difference between the other groups. There was no difference in the rate of learning between the groups. There was no difference in the ultimate proficiency level (p = 0.671) or rate of learning (p = 0.63) when using straight or articulating instruments. There was no difference in ultimate proficiency level (p = 0.59) or learning rate (p = 0.219) seen in the SILS group that had prior training on the task with a conventional laparoscopic set-up.
Conclusions
The results of this study indicate that the proficiency reached using a conventional laparoscopic set-up cannot be matched using a SILS configuration for the novice surgeon and that the choice of straight or articulated instruments as well as previous laparoscopic training does not confer an advantage in this basic task.



Similar content being viewed by others
References
Chow A, Purkayastha S, Aziz O, Pefanis D, Paraskeva P. Single-incision laparoscopic surgery for cholecystectomy: a retrospective comparison with 4-port laparoscopic cholecystectomy. Arch Surg 2010;145:1187–1191
Chow AG, Purkayastha S, Zacharakis E, Paraskeva P. Single-incision laparoscopic surgery for right hemicolectomy. Arch Surg 2011;146:183–186
Scott DJ, Bergen PC, Rege RV, et al. Laparoscopic training on bench models: better and more cost effective than operating room experience? J Am Coll Surg 2000;191:272–283
Peters JH, Fried GM, Swanstrom LL, et al. Development and validation of a comprehensive program of education and assessment of the basic fundamentals of laparoscopic surgery. Surgery 2004;135:21–27
Islam A, Castellvi AO, Tesfay ST, et al. Early surgeon impressions and technical difficulty associated with laparoendoscopic single-site surgery: a Society of American Gastrointestinal and Endoscopic Surgeons learning center study. Surg Endosc 2011;25(8):2597–603
Rieder E, Martinec DV, Cassera MA, et al. A triangulating operating platform enhances bimanual performance and reduces surgical workload in single-incision laparoscopy. J Am Coll Surg 2011;212:378–384
Montero PN, Acker CE, Heniford BT, Stefanidis D. Single Incision Laparoscopic Surgery (SILS) Is Associated with Poorer Performance and Increased Surgeon Workload Compared with Standard Laparoscopy. Am Surg 2011;77:73–77
Santos BF, Enter D, Soper NJ, Hungness ES. Single-incision laparoscopic surgery (SILS) versus standard laparoscopic surgery: a comparison of performance using a surgical simulator. Surg Endosc 2011;25:483–490
Froghi F, Sodergren MH, Darzi A, Paraskeva P. Single-incision Laparoscopic Surgery (SILS) in general surgery: a review of current practice. Surg Laparosc Endosc Percutan Tech 2010;20:191–204
Marks J, Tacchino R, Roberts K, et al. Prospective randomized controlled trial of traditional laparoscopic cholecystectomy versus single-incision laparoscopic cholecystectomy: Report of preliminary data. Am J Surg 2011;201:369–373
Kravetz AJ, Iddings D, Basson MD, Kia MA. The learning curve with single-port cholecystectomy. JSLS 2009;13:332–336
Feldman LS, Cao J, Andalib A, Fraser S, Fried GM. A method to characterize the learning curve for performance of a fundamental laparoscopic simulator task: defining “learning plateau” and “learning rate”. Surgery 2009;146:381–386
Fraser SA, Feldman LS, Stanbridge D, Fried GM. Characterizing the learning curve for a basic laparoscopic drill. Surg Endosc 2005;19:1572–1578
Madan AK, Harper JL, Frantzides CT, Tichansky DS. Nonsurgical skills do not predict baseline scores in inanimate box or virtual-reality trainers. Surg Endosc 2008;22:1686–1689
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sodergren, M., McGregor, C., Farne, H.A. et al. A Randomised Comparative Study Evaluating Learning Curves of Novices in a Basic Single-Incision Laparoscopic Surgery Task. J Gastrointest Surg 17, 569–575 (2013). https://doi.org/10.1007/s11605-012-2113-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-012-2113-1