Abstract
Background
The aim of the study was to evaluate factors for predicting lymph node metastasis in patients who had T1 and T2 colorectal cancer.
Methods
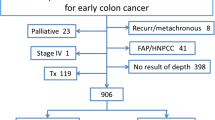
A total of 224 patients with T1 or T2 colorectal cancers who underwent radical surgery with regional lymphadenectomy from January 1999 to January 2008 were analyzed.
Results
Predictive factors for lymph node metastasis and prognostic factors were analyzed. Tumor stage was classified as T1 in 69 (30.8%) and T2 in 155 (69.2%) of patients. The overall incidence of lymph node metastasis was 21.0% (14.5% for T1 cancer and 23.9% for T2 cancer; P = 0.112). The node positive and negative groups were similar with regard to patient demographics, except that the former contained a significantly higher number of lymphovascular invasion and perineural invasion cases. During the median follow-up period of 49 months, the 5-year overall and disease-free survival rates for patients without lymph node metastasis were 97.1% and 94.6%, which were significantly higher than the rates for those with lymph node metastasis (85.5%, P = 0.008, and 82.0%, P = 0.007, respectively). A multivariate analysis revealed that lymph node status was the only significant independent prognostic factor for both overall survival (P = 0.025) and disease-free survival (P = 0.040). Moreover, the presence of lymphovascular invasion (P < 0.001) or perineural invasion (P = 0.004) was an independent predictor for lymph node metastasis.
Conclusion
Lymph node metastasis was the most powerful predictor for poorer survival in patients with T1 or T2 colorectal cancer. For patients with positive lymphovascular or perineural invasion, radical surgery should be recommended because of a greater chance for lymph node metastasis.

Similar content being viewed by others
References
Rasheed S, Bowley DM, Aziz O, Tekkis PP, Sadat AE, Guenther T, Boello ML, McDonald PJ, Talbot IC, Northover JM. Can depth of tumour invasion predict lymph node positivity in patients undergoing resection for early rectal cancer? A comparative study between T1 and T2 cancers. Colorectal Dis 2008;10:231-238.
Chok KS, Law WL. Prognostic factors affecting survival and recurrence of patients with pT1 and pT2 colorectal cancer. World J Surg 2007;31:1485-1490.
Fang WL, Chang SC, Lin JK, Wang HS, Yang SH, Jiang JK Chen WC, Lin TC. Metastatic potential in T1 and T2 colorectal cancer. Hepatogastroenterology 2005;52:1688-1691.
Bayar S, Saxena R, Emir B, Salem RR. Venous invasion may predict lymph node metastasis in early rectal cancer. Eur J Surg Oncol 2002;28:413-417.
Sitzler PJ, Seow-Choen F, Ho YH, Leong AP. Lymph node involvement and tumor depth in rectal cancers: an analysis of 805 patients. Dis Colon Rectum 1997;40:1472-1476.
Baxter NN, Morris AM, Rothenberger DA, Tepper JE. Impact of preoperative radiation for rectal cancer on subsequent lymph node evaluation: a population-based analysis. Int J Radiat Oncol Biol Phys 2005;61:426-431.
Huh JW, Kim HR, Kim YJ. Anastomotic leakage after laparoscopic resection of rectal cancer: the impact of fibrin glue. Am J Surg 2010;199:435-441.
Huh JW, Kim HR, Kim YJ. Proliferating cell nuclear antigen as a prognostic factor after total mesorectal excision of stage II-III rectal cancer. Ann Surg Oncol 2009;16:1494-1500.
Huh JW, Park YA, Lee KY, Kim SA, Sohn SK. Recurrences after local excision for early rectal adenocarcinoma. Yonsei Med J 2009;50:704-708.
Lee HS, Lee S, Seo JH, Kwack KK, Kim JS, Jung HC, Song IS. Follow-up results of endoscopic mucosal resection for early colorectal cancer. J Korean Soc Coloproctol 2006;22:103-112.
Huh JW, Jung EJ, Park YA, Lee KY, Sohn SK. Sphincter-preserving operations following preoperative chemoradiation: an alternative to abdominoperineal resection for lower rectal cancer? World J Surg 2008;32:1116-1123.
Norton SA, Thomas MG. Staging of rectosigmoid neoplasia with colonoscopic endoluminal ultrasonography. Br J Surg 1999;86:942-946.
Heneghan JP, Salem RR, Lange RC, Taylor KJ, Hammers LW. Transrectal sonography in staging rectal carcinoma: the role of gray-scale, color-flow, and Doppler imaging analysis. AJR Am J Roentgenol 1997;169:1247-1252.
Huh JW, Park YA, Jung EJ, Lee KY, Sohn SK. Accuracy of endorectal ultrasonography and computed tomography for restaging rectal cancer after preoperative chemoradiation. J Am Coll Surg 2008;207:7-12.
Nascimbeni R, Burgart LJ, Nivatvongs S, Larson DR. Risk of lymph node metastasis in T1 carcinoma of the colon and rectum. Dis Colon Rectum 2002;45:200-206.
Goldstein NS, Hart J. Histologic features associated with lymph node metastasis in stage T1 and superficial T2 rectal adenocarcinomas in abdominoperineal resection specimens. Identifying a subset of patients for whom treatment with adjuvant therapy or completion abdominoperineal resection should be considered after local excision. Am J Clin Pathol 1999;111:51-58.
Huh JW, Oh BR, Kim HR, Kim YJ. Preoperative carcinoembryonic antigen level as an independent prognostic factor in potentially curative colon cancer. J Surg Oncol 2010;101:396-400.
Liebig C, Ayala G, Wilks JA, Berger DH, Albo D. Perineural invasion in cancer: a review of the literature. Cancer 2009;115:3379-3391.
Quah HM, Chou JF, Gonen M, Shia J, Schrag D, Landmann RG, Guillem JG, Paty PB, Temple LK, Wong WD, Weiser MR. Identification of patients with high-risk stage II colon cancer for adjuvant therapy. Dis Colon Rectum 2008;51:503-507.
Huh JW, Kim YJ, Kim HR. Prognostic value of perineural invasion in patients with stage II colorectal cancer. Ann Surg Oncol 2010. doi:10.1245/S10434-010-0982-7
Acknowledgments
This study was supported by a grant from Chonnam National University Research Institute of Medical Sciences.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Huh, J.W., Kim, H.R. & Kim, Y.J. Lymphovascular or Perineural Invasion May Predict Lymph Node Metastasis in Patients With T1 and T2 Colorectal Cancer. J Gastrointest Surg 14, 1074–1080 (2010). https://doi.org/10.1007/s11605-010-1206-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-010-1206-y