Abstract
Objectives
To compare the outcome for DBT-detected and DM-detected suspicious AD, to evaluate the risk of malignancy and if is affected by the US or MRI imaging correlation.
Methods
All cases with suspicious AD (ultimately assigned BI-RADS 4 or 5 categories) were retrospectively included. Two radiologists independently reviewed DM and DBT images in two sessions for detection (DM vs. DBT). US and MRI imaging correlation findings were recorded. Pathologic results were compared between DBT-detected and DM-detected AD.
Results
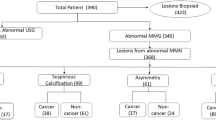
Among 137 detected ADs, 103 (75.2%) were DM-detected, and 34 (24.8%) were only DBT-detected (p = 0.01).
The malignancy rate was lower for DBT-detected than DM-detected AD (14.7% vs. 45.6%) (p = 0.01). Malignancy rate was higher with US-positive than US-negative correlation at DM-detected AD (49.4% vs. 27.8%) (p = 0.01). Malignancy rate was not different for DBT-detected AD with (16.7%) or without (12.5%) sonographic correlation. NPV based on radiologists’ level of suspicion was high (86.2%–97.2%) but not sufficient enough to forgo biopsy.
Of 34 sonographically occult ADs, a positive-MRI correlation was identified in 19 (55.9%) ADs (7 were malignant, 12 were benign). A negative-MRI correlation was identified in 15 (44.1%) ADs; all had a benign outcome (p = 0.01).
Conclusions
DBT-detected AD is less likely to represent malignancy than does DM-detected; however, the risk of malignancy is not low enough to forgo biopsy. MRI-negative correlation in sonographically occult AD was significantly associated with benign outcomes and can avoid unnecessary interventions.




Similar content being viewed by others
Abbreviations
- DBT:
-
Digital breast tomosynthesis
- DM:
-
Digital mammography
- AD:
-
Architectural distortion
- BI-RADS:
-
The Breast Imaging Reporting and Data System Lexicon
- DCIS:
-
Ductal carcinoma in situ
- US:
-
Ultrasound
- MRI:
-
Magnetic resonance imaging
- PPV:
-
Positive predictive value
- NPV:
-
Negative predictive value
References
D’Orsi CJ, Sickles EA, Mendelson EB, Morris EA (2013) ACR BI-RADS atlas, breast imaging reporting and data system, 5th edn, vol 114. American College of Radiology, Reston, pp 79–80
Dibble EH, Lourenco AP, Baird GL, Ward RC, Maynard AS, Mainiero MB (2018) Comparison of digital mammography and digital breast tomosynthesis in the detection of architectural distortion. Eur Radiol 28:3–10
Bahl M, Baker JA, Kinsey EN, Ghate SV (2015) Architectural distortion on mammography: correlation with pathologic outcomes and predictors of malignancy. AJR Am J Roentgenol 205(6):1339–1345
Andersson I, Ikeda DM, Zackrisson S et al (2008) Breast tomosynthesis and digital mammography: a comparison of breast cancer visibility and BIRADS classification in a population of cancers with subtle mammographic findings. Eur Radiol 18(12):2817–2825
Ray KM, Turner E, Sickles EA, Joe BN (2015) Suspicious findings at digital breast tomosynthesis occult to conventional digital mammography: imaging features and pathology findings. Breast J 21(5):538–542
Viala J, Gignier P, Perret B et al (2013) Stereotactic vacuum-assisted biopsies on a digital breast 3d-tomosynthesis system. Breast J 19:4–9
Partyka L, Lourenco AP, Mainiero MB (2014) Detection of mammographically occult architectural distortion on digital breast tomosynthesis screening: initial clinical experience. Am J Roentgenol 203(1):216–222
Bahl M, Lamb LR, Lehman CD (2017) Pathologic outcomes of architectural distortion on digital 2D versus tomosynthesis mammography. Am J Roentgenol 209(5):1162–1167
Alshafeiy TI, Nguyen JV, Rochman CM, Nicholson BT, Patrie JT, Harvey JA (2018) Outcome of architectural distortion detected only at breast tomosynthesis versus 2D mammography. Radiology 288(1):38–46
Giess CS, Chikarmane SA, Sippo DA, Birdwell RL (2016) Breast MR imaging for equivocal mammographic findings: help or hindrance? Radiographics 36(4):943–956
Si L, Zhai R, Liu X, Yang K, Wang Li, Jiang T (2016) MRI in the differential diagnosis of primary architectural distortion detected by mammography. Diagn Interv Radiol 22(2):141–150
Amitai Y, Scaranelo A, Menes TS, Fleming R, Kulkarni S, Ghai S, Freitas V (2020) Can breast MRI accurately exclude malignancy in mammographic architectural distortion? Eur Radiol
Durand MA, Wang S, Hooley RJ, Raghu M, Philpotts LE (2016) Tomosynthesisdetected architectural distortion: management algorithm with radiologicpathologic correlation. Radiographics 36(2):311–321
Lo G, Scaranelo AM, Aboras H et al (2017) Evaluation of the utility of screening mammography for high-risk women undergoing screening breast MR imaging. Radiology 285(1):36–43
Pujara AC, Hui J, Wang LC (2019) Architectural distortion in the era of digital breast tomosynthesis: outcomes and implications for management. Clin Imaging 54:133–137
Freer PE, Niell B, Rafferty EA (2015) Preoperative tomosynthesis-guided needle localization of mammographically and sonographically occult breast lesions. Radiology 275(2):377–383
Kim JY, Kang HJ, Shin JK et al (2017) Biologic profiles of invasive breast cacners detected only with digital breast tomosynthesis. Am J Rev 209:1411–1418
Walcott-Sapp S, Garreau J, Johnson N, Thomas KA (2019) Pathology results of architectural distortion on detected with digital breast tomosynthesis without definite sonographic correlate. Am J Surg 217(5):857–861
Vijapura C, Yang L, Xiong J, Fajardo LL (2018) Imaging features of nonmalignant and malignant architectural distortion detected by tomosynthesis. Am J Roentgenol 211(6):1397–1404
Taskin F, Durum Y, Soyder A, Unsal A (2017) Review and management of breast lesions detected with breast tomosynthesis but not visible on mammography and ultrasonography. Acta Radiol 58(12):1442–1447
Lang K, Nergarden M, Andersson I, Rosso A, Zackrisson S (2016) False positives in breast cancer screening with one-view breast tomosynthesis: an analysis of findings leading to recall, work-up and biopsy rates in the Malmö Breast Tomosynthesis Screening Trial. Eur Radiol 26(11):3899–390720
Bohan S, Ramli Hamid MT, Chan WY et al (2021) Diagnostic accuracy of tomosynthesis-guided vacuum assisted breast biopsy of ultrasound occult lesions. Sci Rep 11:129
Tsai H, Fu MC, Hsu OJKJ, Chiu MHH (2019) Accuracy and outcomes of stereotactic vacuum-assisted breast biopsy for diagnosis and management of nonpalpable breast lesions. 1–6
Rageth CJ et al (2019) Second international consensus conference on lesions of uncertain malignant potential in the breast (B3 lesions). Breast Cancer Res Treat 174:279–296
Mumin NA, Rahmat K, Fadzli F, Ramli MT, Westerhout CJ, Ramli N et al (2019) Diagnostic efficacy of synthesized 2D digital breast tomosynthesis in multi-ethnic Malaysian population. Sci Rep 9(1):1459
Murphy MC, Coffey L, O’Neill AC et al (2018) Can the synthetic C view images be used in isolation for diagnosing breast malignancy without reviewing the entire digital breast tomosynthesis data set? Ir J Med Sci 187:1077–1081
Goh Y, Chan CW, Pillay P et al (2020) Architecture distortion score (ADS) in malignancy risk stratification of architecture distortion on contrast-enhanced digital mammography. Eur Radiol
Du G, Dong M, Sun Y, Li S, Mu X, Wei H et al (2019) A new method for detecting architectural distortion in mammograms by non subsampled contourlet transform and improved PCNN. Appl Sci 9(22):4916
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The scientific guarantor of this publication is DR. Shimaa Abdalla Ahmed. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Ethical approval
Institutional Review Board approval was obtained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ahmed, S.A., Samy, M., Ali, A.M. et al. Architectural distortion outcome: digital breast tomosynthesis-detected versus digital mammography-detected. Radiol med 127, 30–38 (2022). https://doi.org/10.1007/s11547-021-01419-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-021-01419-8