Abstract
Purpose
Image texture analysis (TA) is a heterogeneity quantifying approach that cannot be appreciated by the naked eye, and early evidence suggests that TA has great potential in the field of oncology. The aim of this study is to evaluate parotid gland texture analysis (TA) combined with formal dosimetry as a factor for predicting severe late xerostomia in patients undergoing radiation therapy for head and neck cancers.
Methods
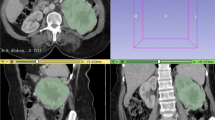
We performed a retrospective analysis of patients treated at our Radiation Oncology Unit between January 2010 and December 2015, and selected the patients whose normal dose constraints for the parotid gland (mean dose < 26 Gy for the bilateral gland) could not be satisfied due to the presence of positive nodes close to the parotid glands. The parotid gland that showed the higher V30 was contoured on CT simulation and analysed with LifeX Software©. TA parameters included features of grey-level co-occurrence matrix (GLCM), neighbourhood grey-level dependence matrix (NGLDM), grey-level run length matrix (GLRLM), grey-level zone length matrix (GLZLM), sphericity, and indices from the grey-level histogram. We performed a univariate and multivariate analysis between all the texture parameters, the volume of the gland, the normal dose parameters (V30 and Mean Dose), and the development of severe chronic xerostomia.
Results
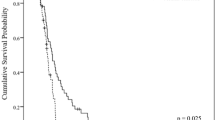
Seventy-eight patients were included and 25 (31%) developed chronic xerostomia. The TA parameters correlated with severe chronic xerostomia included V30 (OR 5.63), Dmean (OR 5.71), Kurtosis (OR 0.78), GLCM Correlation (OR 1.34), and RLNU (OR 2.12). The multivariate logistic regression showed a significant correlation between V30 (0.001), GLCM correlation (p: 0.026), RLNU (p: 0.011), and chronic xerostomia (p < 0.001, R2:0.664).
Conclusions
Xerostomia represents an important cause of morbidity for head and neck cancer survivors after radiation therapy, and in certain cases normal dose constraints cannot be satisfied. Our results seem promising as texture analysis could enhance the normal dose constraints for the prediction of xerostomia.

Similar content being viewed by others
References
Dirix P, Nuyts S (2010) Evidence-based organ-sparing radiotherapy in head and neck cancer. Lancet Oncol 11(1):85–91. https://doi.org/10.1016/S1470-2045(09)70231-1
Retel VP, van der Molen L, Hilgers FJ, Rasch CR, L’Ortye AA, Steuten LM, van Harten WH (2011) A cost-effectiveness analysis of a preventive exercise program for patients with advanced head and neck cancer treated with concomitant chemo-radiotherapy. BMC Cancer 11:475. https://doi.org/10.1186/1471-2407-11-475
Vissink A, Jansma J, Spijkervet FK, Burlage FR, Coppes RP (2003) Oral sequelae of head and neck radiotherapy. Crit Rev Oral Biol Med Off Publ Am Assoc of Oral Biol 14(3):199–212
Chao KS, Ozyigit G, Blanco AI, Thorstad WL, Deasy JO, Haughey BH, Spector GJ, Sessions DG (2004) Intensity-modulated radiation therapy for oropharyngeal carcinoma: impact of tumor volume. Int J Radiat Oncol Biol Phys 59(1):43–50. https://doi.org/10.1016/j.ijrobp.2003.08.004
Chao KS, Deasy JO, Markman J, Haynie J, Perez CA, Purdy JA, Low DA (2001) A prospective study of salivary function sparing in patients with head-and-neck cancers receiving intensity-modulated or three-dimensional radiation therapy: initial results. Int J Radiat Oncol Biol Phys 49(4):907–916
Eisbruch A, Ship JA, Dawson LA, Kim HM, Bradford CR, Terrell JE, Chepeha DB, Teknos TN, Hogikyan ND, Anzai Y, Marsh LH, Ten Haken RK, Wolf GT (2003) Salivary gland sparing and improved target irradiation by conformal and intensity modulated irradiation of head and neck cancer. World J Surg 27(7):832–837
Eisbruch A, Ten Haken RK, Kim HM, Marsh LH, Ship JA (1999) Dose, volume, and function relationships in parotid salivary glands following conformal and intensity-modulated irradiation of head and neck cancer. Int J Radiat Oncol Biol Phys 45(3):577–587
Vissink A, Burlage FR, Spijkervet FK, Jansma J, Coppes RP (2003) Prevention and treatment of the consequences of head and neck radiotherapy. Crit Rev Oral Biol Med Off Publ Am Assoc of Oral Biol 14(3):213–225
Epstein JB, Emerton S, Kolbinson DA, Le ND, Phillips N, Stevenson-Moore P, Osoba D (1999) Quality of life and oral function following radiotherapy for head and neck cancer. Head Neck 21(1):1–11
Blanco AI, Chao KS, El Naqa I, Franklin GE, Zakarian K, Vicic M, Deasy JO (2005) Dose-volume modeling of salivary function in patients with head-and-neck cancer receiving radiotherapy. Int J Radiat Oncol Biol Phys 62(4):1055–1069. https://doi.org/10.1016/j.ijrobp.2004.12.076
Pow EH, Kwong DL, McMillan AS, Wong MC, Sham JS, Leung LH, Leung WK (2006) Xerostomia and quality of life after intensity-modulated radiotherapy vs. conventional radiotherapy for early-stage nasopharyngeal carcinoma: initial report on a randomized controlled clinical trial. Int J Radiat Oncol Biol Phys 66(4):981–991. https://doi.org/10.1016/j.ijrobp.2006.06.013
McMillan AS, Pow EH, Kwong DL, Wong MC, Sham JS, Leung LH, Leung WK (2006) Preservation of quality of life after intensity-modulated radiotherapy for early-stage nasopharyngeal carcinoma: results of a prospective longitudinal study. Head Neck 28(8):712–722. https://doi.org/10.1002/hed.20378
Bhide SA, Gulliford S, Schick U, Miah A, Zaidi S, Newbold K, Nutting CM, Harrington KJ (2012) Dose-response analysis of acute oral mucositis and pharyngeal dysphagia in patients receiving induction chemotherapy followed by concomitant chemo-IMRT for head and neck cancer. Radiother Oncol J Eur Soc Ther Radiol Oncol 103(1):88–91. https://doi.org/10.1016/j.radonc.2011.12.027
Logemann JA, Pauloski BR, Rademaker AW, Colangelo LA (1997) Speech and swallowing rehabilitation for head and neck cancer patients. Oncology 11(5):651–656 (discussion 659, 663–654)
Marks LB, Yorke ED, Jackson A, Ten Haken RK, Constine LS, Eisbruch A, Bentzen SM, Nam J, Deasy JO (2010) Use of normal tissue complication probability models in the clinic. Int J Radiat Oncol Biol Phys 76(3 Suppl):S10–19. https://doi.org/10.1016/j.ijrobp.2009.07.1754
Davnall FYCSP, Ljungqvist G et al (2012) Assessment of tumor heterogeneity: an emerging imaging tool for clinical practice? Insights Imaging 3:573–589
Nardone V, Tini P, Carbone SF, Grassi A, Biondi M, Sebaste L, Carfagno T, Vanzi E, De Otto G, Battaglia G, Rubino G, Pastina P, Belmonte G, Mazzoni LN, Banci Buonamici F, Mazzei MA, Pirtoli L (2017) Bone texture analysis using CT-simulation scans to individuate risk parameters for radiation-induced insufficiency fractures. Osteoporos Int. https://doi.org/10.1007/s00198-017-3968-5
Nardone V, Tini P, Sebaste L, Biondi M, Banci Buonamici F, Pirtoli L (2016) Bone structure texture analysis as a potential tool to estimate radiation induced insufficiency fracture risk. Radiother Oncol. https://doi.org/10.1016/j.radonc.2016.06.001
Alobaidli S, McQuaid S, South C, Prakash V, Evans P, Nisbet A (2014) The role of texture analysis in imaging as an outcome predictor and potential tool in radiotherapy treatment planning. Br J Radiol 87(1042):20140369. https://doi.org/10.1259/bjr.20140369
Coroller TP, Agrawal V, Narayan V, Hou Y, Grossmann P, Lee SW, Mak RH, Aerts HJ (2016) Radiomic phenotype features predict pathological response in non-small cell lung cancer. Radiother Oncol. https://doi.org/10.1016/j.radonc.2016.04.004
Scalco E, Fiorino C, Cattaneo GM, Sanguineti G, Rizzo G (2013) Texture analysis for the assessment of structural changes in parotid glands induced by radiotherapy. Radioth Oncol J Eur Soc Ther Radiol Oncol 109(3):384–387. https://doi.org/10.1016/j.radonc.2013.09.019
Fruehwald-Pallamar J, Czerny C, Holzer-Fruehwald L, Nemec SF, Mueller-Mang C, Weber M, Mayerhoefer ME (2013) Texture-based and diffusion-weighted discrimination of parotid gland lesions on MR images at 3.0 Tesla. NMR Biomed 26(11):1372–1379. https://doi.org/10.1002/nbm.2962
Yang X, Tridandapani S, Beitler JJ, Yu DS, Yoshida EJ, Curran WJ, Liu T (2012) Ultrasound GLCM texture analysis of radiation-induced parotid-gland injury in head-and-neck cancer radiotherapy: an in vivo study of late toxicity. Med Phys 39(9):5732–5739. https://doi.org/10.1118/1.4747526
Eisbruch A, Kim HM, Terrell JE, Marsh LH, Dawson LA, Ship JA (2001) Xerostomia and its predictors following parotid-sparing irradiation of head-and-neck cancer. Int J Radiat Oncol Biol Phys 50(3):695–704
Meirovitz A, Murdoch-Kinch CA, Schipper M, Pan C, Eisbruch A (2006) Grading xerostomia by physicians or by patients after intensity-modulated radiotherapy of head-and-neck cancer. Int J Radiat Oncol Biol Phys 66(2):445–453. https://doi.org/10.1016/j.ijrobp.2006.05.002
van der Schaaf A, Xu CJ, van Luijk P, Van’t Veld AA, Langendijk JA, Schilstra C (2012) Multivariate modeling of complications with data driven variable selection: guarding against overfitting and effects of data set size. Radiother Oncol 105(1):115–121. https://doi.org/10.1016/j.radonc.2011.12.006
Hanley JA, McNeil BJ (1982) The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology 143(1):29–36. https://doi.org/10.1148/radiology.143.1.7063747
van Acker F, Flamen P, Lambin P, Maes A, Kutcher GJ, Weltens C, Hermans R, Baetens J, Dupont P, Rijnders A, Maes A, van den Bogaert W, Mortelmans L (2001) The utility of SPECT in determining the relationship between radiation dose and salivary gland dysfunction after radiotherapy. Nucl Med Commun 22(2):225–231
Buus S, Grau C, Munk OL, Rodell A, Jensen K, Mouridsen K, Keiding S (2006) Individual radiation response of parotid glands investigated by dynamic 11C-methionine PET. Radiother Oncol J Eur Soc Ther Radiol Oncol 78(3):262–269. https://doi.org/10.1016/j.radonc.2006.02.013
Braam PM, Roesink JM, Moerland MA, Raaijmakers CP, Schipper M, Terhaard CH (2005) Long-term parotid gland function after radiotherapy. Int J Radiat Oncol Biol Phys 62(3):659–664. https://doi.org/10.1016/j.ijrobp.2004.12.015
Pellegrino F, Groff E, Bastiani L, Fattori B, Sotti G (2015) Assessment of radiation-induced xerostomia: validation of the Italian version of the xerostomia questionnaire in head and neck cancer patients. Support Care Cancer Off J Multinatl Assoc Support Care Cancer 23(4):925–932. https://doi.org/10.1007/s00520-014-2438-2
Lee TF, Fang FM (2013) Quantitative analysis of normal tissue effects in the clinic (QUANTEC) guideline validation using quality of life questionnaire datasets for parotid gland constraints to avoid causing xerostomia during head-and-neck radiotherapy. Radiother Oncol J Eur Soc Ther Radiol Oncol 106(3):352–358. https://doi.org/10.1016/j.radonc.2012.11.013
Beetz I, Steenbakkers RJ, Chouvalova O, Leemans CR, Doornaert P, van der Laan BF, Christianen ME, Vissink A, Bijl HP, van Luijk P, Langendijk JA (2014) The QUANTEC criteria for parotid gland dose and their efficacy to prevent moderate to severe patient-rated xerostomia. Acta Oncol 53(5):597–604. https://doi.org/10.3109/0284186X.2013.831186
Miah AB, Gulliford SL, Clark CH, Bhide SA, Zaidi SH, Newbold KL, Harrington KJ, Nutting CM (2013) Dose-response analysis of parotid gland function: what is the best measure of xerostomia? Radiother Oncol 106(3):341–345. https://doi.org/10.1016/j.radonc.2013.03.009
Tribius S, Sommer J, Prosch C, Bajrovic A, Muenscher A, Blessmann M, Kruell A, Petersen C, Todorovic M, Tennstedt P (2013) Xerostomia after radiotherapy. What matters–mean total dose or dose to each parotid gland? Strahlentherapie und Onkologie : Organ der Deutschen Rontgengesellschaft [et al] 189(3):216–222. https://doi.org/10.1007/s00066-012-0257-2
Nutting CM, Morden JP, Harrington KJ, Urbano TG, Bhide SA, Clark C, Miles EA, Miah AB, Newbold K, Tanay M, Adab F, Jefferies SJ, Scrase C, Yap BK, A’Hern RP, Sydenham MA, Emson M, Hall E, group Ptm (2011) Parotid-sparing intensity modulated versus conventional radiotherapy in head and neck cancer (PARSPORT): a phase 3 multicentre randomised controlled trial. Lancet Oncol 12(2):127–136. https://doi.org/10.1016/S1470-2045(10)70290-4
Scalco E, Moriconi S, Rizzo G (2015) Texture analysis to assess structural modifications induced by radiotherapy. In: Conference proceedings : annual international conference of the IEEE Engineering in Medicine and Biology Society IEEE Engineering in Medicine and Biology Society Annual Conference 2015, pp 5219–5222. https://doi.org/10.1109/embc.2015.7319568
Teshima K, Murakami R, Yoshida R, Nakayama H, Hiraki A, Hirai T, Nakaguchi Y, Tsujita N, Tomitaka E, Furusawa M, Yamashita Y, Shinohara M (2012) Histopathological changes in parotid and submandibular glands of patients treated with preoperative chemoradiation therapy for oral cancer. J Radiat Res 53(3):492–496
van Dijk LV, Brouwer CL, van der Schaaf A, Burgerhof JG, Beukinga RJ, Langendijk JA, Sijtsema NM, Steenbakkers RJ (2016) CT image biomarkers to improve patient-specific prediction of radiation-induced xerostomia and sticky saliva. Radiother Oncol. https://doi.org/10.1016/j.radonc.2016.07.007
Nardone V, Tini P, Nioche C, Biondi M, Sebaste L, Mazzei MA, Banci Buonamici F, Pirtoli L (2016) Texture analysis of parotid gland as a predictive factor of radiation induced xerostomia: a subset analysis. Radiother Oncol. https://doi.org/10.1016/j.radonc.2016.09.004
van Dijk LV, Langendijk JA, Sijtsema NM, Steenbakkers RJHM (2017) Reply letter to “Texture analysis of parotid gland as a predictive factor of radiation induced xerostomia: a subset analysis”. Radiother Oncol 122(2):322. https://doi.org/10.1016/j.radonc.2016.11.002
Fiorino C, Rizzo G, Scalco E, Broggi S, Belli ML, Dell’Oca I, Dinapoli N, Ricchetti F, Rodriguez AM, Di Muzio N, Calandrino R, Sanguineti G, Valentini V, Cattaneo GM (2012) Density variation of parotid glands during IMRT for head-neck cancer: correlation with treatment and anatomical parameters. Radiother Oncol J Eur Soc Ther Radiol Oncol 104(2):224–229. https://doi.org/10.1016/j.radonc.2012.06.003
Beetz I, Schilstra C, Burlage FR, Koken PW, Doornaert P, Bijl HP, Chouvalova O, Leemans CR, de Bock GH, Christianen ME, van der Laan BF, Vissink A, Steenbakkers RJ, Langendijk JA (2012) Development of NTCP models for head and neck cancer patients treated with three-dimensional conformal radiotherapy for xerostomia and sticky saliva: the role of dosimetric and clinical factors. Radiother Oncol J Eur Soc Ther Radiol Oncol 105(1):86–93. https://doi.org/10.1016/j.radonc.2011.05.010
Funding
No funding has been provided for this Work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the Authors declare no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Nardone, V., Tini, P., Nioche, C. et al. Texture analysis as a predictor of radiation-induced xerostomia in head and neck patients undergoing IMRT. Radiol med 123, 415–423 (2018). https://doi.org/10.1007/s11547-017-0850-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-017-0850-7