Abstract
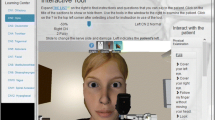
Systematic reviews and meta-analyses of randomized controlled studies conclude that virtual patient simulations are consistently associated with higher learning outcomes compared to other educational methods. However, we cannot assume that students will learn from simply exposing students to the simulations. The instructional features that are integrated before, during and after the simulations may affect learning and performance as much as or more than the simulation and how those features are used. Here, we examine the design and development of NERVE: A virtual patient simulation created to give medical students standardized experiences in interviewing, examining, and diagnosing virtual patients with cranial nerve disorders. We depict key design features of the simulation and discuss how two sets of design research studies were completed to improve the total learning experience, including the virtual patient simulations and the instructional features incorporated with the simulations.





Similar content being viewed by others
References
Agency for Healthcare Research and Quality (AHRQ) (2013). PAR-11-024 Advances in patient safety through simulation research. http://grants.nih.gov/grants/guide/pa-files/PAR-11-024.html. Accessed 20 Jan 20.
Baehr, M., & Frotscher, M. (2012). Duus’ topical diagnosis in neurology: anatomy, physiology, signs, symptoms (5th ed.). New York: Thieme.
Bateman, J., Allen, M., Samani, D., Kidd, J., & Davies, D. (2013). Virtual patient design: exploring what works and why. A grounded theory study. Medical Education, 47(6), 595–606.
Bearman, M. (2003). Is virtual the same as real? Medical students’ experiences of a virtual patient. Academic Medicine, 78(5), 538–545.
Bearman, M., Cesnik, B., & Liddell, M. (2001). Random comparison of ‘virtual patient’ models in the context of teaching clinical communication skills. Medical Education, 35, 824–832.
Benedict, N. (2010). Virtual patients and problem-based learning in advanced therapeutics. American Journal of Pharmaceutical Education, 74(8), 151.
Berman, N., Fall, L., Smith, S., Levine, D. A., Maloney, C. G., Potts, M., et al. (2009). Integration strategies for using virtual patients in clinical clerkships. Academic Medicine, 84(7), 943–949.
Brazis, P. W., Masdeu, J. C., & Biller, J. (2011). Localization in clinical neurology (6th ed.). Philadelphia: LWW.
Cannon-Bowers, J. A., & Bowers, C. A. (2009). Synthetic learning environments: On developing a science of simulation, games and virtual worlds for training. In S. W. J. Kozlowski & E. Salas (Eds.), Learning, training, and development in organizations (pp. 229–261). Mahwah, NJ: Erlbaum.
Cendan, J., & Lok, B. (2012). The use of virtual patients in medical school curricula. Advances in Physiology Education, 36(1), 48–53.
Churchill, D. (2007). Towards a useful classification of learning objects. Educational Technology Research and Development, 55(5), 479–497.
Cobb, P., Confrey, J., diSessa, A., Lehrer, R., & Schauble, L. (2003). Design experiments in educational research. Educational Researcher, 32(1), 9–13.
Collins, A. (1992). Toward a design science of education. In E. Scanlon & T. O’Shea (Eds.), New directions in educational technology (pp. 15–22). Berlin: Springer.
Cook, D., & Triola, M. (2009). Virtual patients: a critical literature review and proposed next steps. Medical Education, 43(4), 303–311.
Cook, D. A., Erwin, P. J., & Triola, M. M. (2010). Computerized virtual patients in health professions education: A systematic review and meta-analysis. Academic Medicine, 85, 1602–15890.
Department of Defense. (2011, October 1). Modeling and simulation (M&S) glossary. Alexandria, VA: Modeling and Simulation Coordination Office. Retrieved from http://www.msco.mil/documents/_4_DoD%20M&S%20Glossary%20Combined.pdf.
Duchastel, P. (1990–1991). Instructional strategies for simulation-based learning. Journal of Educational Technology Systems, 19(3), 265–275.
Edelbring, S., Broström, O., Henriksson, P., Vassiliou, D., Spaak, J., Dahlgren, L. O., & Zary, N. (2012). Integrating virtual patients into courses: follow-up seminars and perceived benefit. Medical Education, 46(4), 417–425.
Ellaway, R. H., Poulton, T., Smothers, V., & Greene, P. (2009). Virtual patients come of age. Medical Teacher, 31, 683–684.
Fiorella, L., Vogel-Walcutt, J. J., & Schatz, S. (2012). Applying the modality principle to real-time feedback and the acquisition of higher-order cognitive skills. Educational Technology Research and Development, 60(2), 223–238.
Fischer, M., Hege, I., Hörnlein, A., Puppe, F., Tönshoff, B., & Huwendiek, S. (2007). Virtual patients in medical education: a comparison of various strategies for curricular integration. Zeitschrift fur Evidenz, Fortbildung und Qualitat im Gesundheitswesen, 102(10), 648–653.
Fortin, A. H., Dwamena, F. C., Frankel, R. M., & Smith, R. C. (2012). Smith’s Patient-centered interviewing: an evidence-based method (3rd ed.). New York: McGraw-Hill.
Greenberg, D., Aminoff, M., & Simon, R. (2012). Clinical Neurology (8th ed.). China: McGraw-Hill Professional.
Halan, S., Sai, I., Crary, M., & Lok, B. (2014). Virtual Agent constructionism: experiences from health professions students creating virtual conversational agent representations of patients. Presented at the IEEE 14th International Conference on Advanced Learning Technologies (ICALT), July 7–10, Athens, Greece.
Hays, R. T. (2006). The science of learning: A systems theory approach. Boca Raton, FL: BrownWalker Press.
Hirumi, A. (2014). Advancing virtual patient simulations with interPLAY: examining the role of id principles and practices. Concurrent Session presented the annual Association for Educational Communication and Technology conference, Jacksonville, FL. Nov. 5–9.
Hirumi, A., Johnson, T. & Reyes, R. J. (2015). Field-testing strategies to improve the integration of virtual patient simulations into medical school curriculum. Concurrent session presented the annual Association for Educational Communication and Technology conference, Indianapolis, IN. Nov. 4–6.
Huang, G., Reynolds, R., & Candler, C. (2007). Virtual patient simulation at US and Canadian medical schools. Academic Medicine, 82(5), 446–451.
Issenberg, S. B., McGaghie, W. C., Petrusa, E., Gordon, D. L., & Scalese, R. J. (2005). Features and uses of high-fidelity medical simulations that lead to effective learning: A BEME systematic review. Medical Teacher, 27(1), 10–28.
Johnson, T. R., Lyons, R., Chuah, J. H., Kopper, R., Lok, B., & Cendan, J. C. (2013). Optimal learning in a virtual patient simulation of cranial nerve palsies: The interaction between social learning context and student aptitude. Medical Teacher, 35(1), 899–907.
Johnson, T. R., Lyons, R., Kopper, R., Johnsen, K. J., Lok, B., & Cendan, J. C. (2014). Virtual patient simulations and optimal social learning context: A replication of an aptitude-treatment interaction effect. Medical Teacher, 36(6), 486–494.
Klopfer, E., & Squire, K. (2008). Environmental detectives—The development of an augmented reality platform for environmental simulations. Educational Technology Research and Development, 56(2), 203–228.
Kotranza, A., Johnsen, K., Cendan, J., Miller, G., Lind, D. S., & Lok, B. (2009). Virtual multi-tools for hand and tool-based interactions with life-size virtual human agents. 2009 IEEE Symposium on 3D User Interfaces, 23. Doi: 10.1109/3DUI.2009.4811201.
Le, T., & Bhushan, V. (2015). First Aid for the USMLE Step 1 2015 (25th ed.). China: McGraw-Hill Education.
Liaison Committee on Medical Education (2011). Functions and Structures of a Medical School. Standards for Accreditation of Medical Education Programs Leading to the M.D. Degree. http://www.lcme.org/functions2010jun.pdf. Accessed on 19 Dec.
Lin, C., Laserna, C., Lind, D., Kalaria, C., Aryal, T., Lok, B., et al. (2012). User response to the simulation of a virtual patient with cranial nerve injury. Journal of Bio-Algorithms & Med-Systems, 8(1), 1–12.
Lindsey, L., & Berger, N. (2009). Experiential approach to instruction. In C. Reigeluth & A. Carr-Chellman (Eds.), Instructional-design theories and models (Vol. 3, pp. 117–142)., Building a common knowledge based New York, NY: Routledge.
Liu, G. T., Volpe, N. J., & Galetta, S. L. (2012). Neuro-ophthalmology: diagnosis and management (2nd ed.). Philadelphia: Saunders.
Lyons, R., Johnson, T. R., Khalil, M. K., & Cendan, J. C. (2014). The impact of social context on learning and cognitive demands for interactive virtual human simulations. PeerJ, 2, e372.
Maran, N. J., & Glavin, R. J. (2003). Low-to high-fidelity simulation – a continuum of medical education? Medical Education, 37(1), 22–28.
McGee, J. B., Neill, J., Goldman, L., & Casey, E. (1998). Using multimedia virtual patients to enhance the clinical curriculum for medical students. Student Health Technol Inform., 52, 732–735.
McKenney, S. E., & Reeves, T. (2012). Conducting educational design research: what, why and how. London: Taylor & Francis Ltd.
Moore, F., & Chalk, C. (2009). The essential neurologic examination: What should medical students be taught? Neurology, 72(23), 2020–2023.
Navy Modeling & Simulation Office. (2005). Essentials of modeling and simulation. Retrieved from https://nmso.navy.mil/ems.
O’Connell, T. X., Pedigo, R. A., & Blair, T. E. (2013). Crush step 1: the ultimate USMLE step 1 review (1st ed.). Philadelphia: Saunders.
Platt, F. W., Gaspar, D. L., Coulehan, J. L., Fox, L., Adler, A. J., Weston, W. W., et al. (2001). “Tell me about yourself”: the patient-centered interview. Annals of Internal Medicine, 134(11), 1079–1085.
Reigeluth, C., & Schwartz, E. (1989). An instructional theory for the design of computer-based simulations. Journal of Computer-Based Instruction, 16(1), 1–10.
Rieber, L. P. (1996). Animation as feedback in a computer-based simulation: Representation matters. Educational Technology Research and Development, 44(1), 5–22.
Rosen, M. A., Salas, E., Silvestri, S., Wu, T. S., & Lazzara, E. H. (2008). A measurement tool for simulation-based training in emergency medicine. The simulation module for assessment of resident targeted event responses (SMARTER) approach. Simulation in Healthcare, 3(3), 170–179.
Rossen, B., & Lok, B. (2012). A Crowdsourcing Method to Develop Virtual Human Conversational Agents. International Journal of Human-Computer Studies, 70(4), 301–319.
Salas, E., & Gregory, M. E. (2011). Simulation-based training: Beyond the bells and whistles! CyberTherapy Magazine, 4, 18–19.
Waxman, S. (2013). Clinical neuroanatomy (27th ed.). China: McGraw-Hill Education.
Ziv, A., Wolpe, P. R., Small, S. D., & Glick, S. (2003). Simulation-based medical education: An ethical imperative. Academic Medicine, 78, 783–788.
Acknowledgments
Research reported in this paper was supported by the National Institutes of Health (NIH) under award number 1R01LM010813-01. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Hirumi, A., Kleinsmith, A., Johnsen, K. et al. Advancing virtual patient simulations through design research and interPLAY: part I: design and development. Education Tech Research Dev 64, 763–785 (2016). https://doi.org/10.1007/s11423-016-9429-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11423-016-9429-6