Abstract
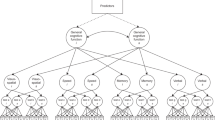
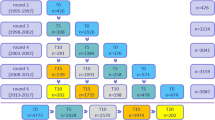
Maintaining good cognitive function at older age is important, but our knowledge of patterns and predictors of cognitive aging is still limited. We used Bayesian model-based clustering to group 5064 participants of the Long Life Family Study (ages 49–110 years) into clusters characterized by distinct trajectories of cognitive change in the domains of episodic memory, attention, processing speed, and verbal fluency. For each domain, we identified 4 or 5 large clusters with representative patterns of change ranging from rapid decline to exceptionally slow change. We annotated the clusters by their correlation with genetic and molecular biomarkers, non-genetic risk factors, medical history, and other markers of aging to discover correlates of cognitive changes and neuroprotection. The annotation analysis discovered both predictors of multi-domain cognitive change such as gait speed and predictors of domain-specific cognitive change such as IL6 and NTproBNP that correlate only with change of processing speed or APOE genotypes that correlate only with change of processing speed and logical memory. These patterns also suggest that cognitive decline starts at young age and that maintaining good physical function correlates with slower cognitive decline. To better understand the agreement of cognitive changes across multiple domains, we summarized the results of the cluster analysis into a score of cognitive function change. This score showed that extreme patterns of change affecting multiple cognitive domains simultaneously are rare in this study and that specific signatures of biomarkers of inflammation and metabolic disease predict severity of cognitive changes. The substantial heterogeneity of change patterns within and between cognitive domains and the net of correlations between patterns of cognitive aging and other aging traits emphasizes the importance of measuring a wide range of cognitive functions and the need for studying cognitive aging in concert with other aging traits.



Similar content being viewed by others
References
Andersen SL, Du M, Cosentino S, Schupf N, Rosso A, Perls TT, Sebastiani P (2019a) Slower decline in processing speed is associated with familial longevity in the long life family study J Gerontol, B in review.
Andersen SL, Sebastiani P, Dworkis DA, Feldman L, Perls TT. Health span approximates life span among many supercentenarians: compression of morbidity at the approximate limit of life span. J Gerontol A Biol Sci Med Sci. 2012;67:395–405. https://doi.org/10.1093/gerona/glr223.
Andersen SL, Sweigart B, Sebastiani P, Drury J, Sidlowski S, Perls TT. Reduced prevalence and incidence of cognitive impairment among centenarian offspring. J Gerontol A Biol Sci Med Sci. 2019b;74:108–13. https://doi.org/10.1093/gerona/gly141.
Anstey KJ, Hofer SM, Luszcz MA. A latent growth curve analysis of late-life sensory and cognitive function over 8 years: evidence for specific and common factors underlying change. Psychol Aging. 2003;18:714–26. https://doi.org/10.1037/0882-7974.18.4.714.
Bae HT, Sebastiani P, Sun JX, Andersen SL, Daw EW, Terracciano A, et al. Genome-wide association study of personality traits in the long life family study. Front Genet. 2013;4:65. https://doi.org/10.3389/fgene.2013.00065.
Barral S, et al. Common genetic variants on 6q24 associated with exceptional episodic memory performance in the elderly. JAMA Neurol. 2014;71:1514–9. https://doi.org/10.1001/jamaneurol.2014.1663.
Barral S, et al. Exceptional memory performance in the long life family study. Neurobiol Aging. 2013;34:2445–8. https://doi.org/10.1016/j.neurobiolaging.2013.05.002.
Benjamini Y, Hochberg Y. Controlling the false discovery rate - a practical and powerful approach to multiple testing. J Roy Stat Soc B Met. 1995;57:289–300.
Birks HJB. Recent methodological developments in quantitative descriptive biogeography. Ann Zool Fenn. 1987;24:165–78.
Blanken AE, Jang JY, Ho JK, Edmonds EC, Han SD, Bangen KJ, et al. Distilling heterogeneity of mild cognitive impairment in the National Alzheimer Coordinating Center database using latent profile analysis. JAMA Netw Open. 2020;3:e200413. https://doi.org/10.1001/jamanetworkopen.2020.0413.
Buracchio T, Dodge HH, Howieson D, Wasserman D, Kaye J. The trajectory of gait speed preceding mild cognitive impairment. Arch Neurol. 2010;67:980–6. https://doi.org/10.1001/archneurol.2010.159.
Clouston SA, et al. The dynamic relationship between physical function and cognition in longitudinal aging cohorts. Epidemiol Rev. 2013;35:33–50. https://doi.org/10.1093/epirev/mxs004.
Cloutier S, Chertkow H, Kergoat M-J, Gauthier S, Belleville S. Patterns of cognitive decline prior to dementia in persons with mild cognitive impairment. J Alzheimers Dis. 2015;47:901–13. https://doi.org/10.3233/JAD-142910.
Cosentino S, Schupf N, Christensen K, Andersen SL, Newman A, Mayeux R. Reduced prevalence of cognitive impairment in families with exceptional longevity. JAMA Neurol. 2013;70:867–74. https://doi.org/10.1001/jamaneurol.2013.1959.
Duncan TE, Duncan SC. The ABC’s of LGM: an introductory guide to latent variable growth curve modeling. Soc Personal Psychol Compass. 2009;3:979–91. https://doi.org/10.1111/j.1751-9004.2009.00224.x.
Elo IT, Mykyta L, Sebastiani P, Christensen K, Glynn NW, Perls T. Age validation in the long life family study through a linkage to early-life census records. J Gerontol B Psychol Sci Soc Sci. 2013;68:580–5. https://doi.org/10.1093/geronb/gbt033.
Folstein MF, Folstein SE, McHugh PR. Mini-mental state: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12:189–98.
Fraley C, Raftery AE. Model-based clustering, discriminant analysis, and density estimation. J Am Stat Assoc. 2002;97:611–31.
Goh JO, An Y, Resnick SM. Differential trajectories of age-related changes in components of executive and memory processes. Psychol Aging. 2012;27:707–19. https://doi.org/10.1037/a0026715.
Gu Z, Gu L, Eils R, Schlesner M, Brors B. Circlize implements and enhances circular visualization in R. Bioinformatics. 2014;30:2811–2. https://doi.org/10.1093/bioinformatics/btu393.
Harada CN, Natelson Love MC, Triebel KL. Normal cognitive aging. Clin Geriatr Med. 2013;29:737–52. https://doi.org/10.1016/j.cger.2013.07.002.
Kim YJ, et al. Protective effects of APOE e2 against disease progression in subcortical vascular mild cognitive impairment patients: a three-year longitudinal study. Sci Rep. 2017;7:1910. https://doi.org/10.1038/s41598-017-02046-y.
Lee JS, Cho SK, Kim HJ, Kim YJ, Park KC, Lockhart SN, et al. Prediction models of cognitive trajectories in patients with nonamnestic mild cognitive impairment. Sci Rep. 2018;8:10468. https://doi.org/10.1038/s41598-018-28881-1.
Lindenberger U, Ghisletta P. Cognitive and sensory declines in old age: gauging the evidence for a common cause. Psychol Aging. 2009;24:1–16. https://doi.org/10.1037/a0014986.
Lovden M, Bergman L, Adolfsson R, Lindenberger U, Nilsson LG. Studying individual aging in an interindividual context: typical paths of age-related, dementia-related, and mortality-related cognitive development in old age. Psychol Aging. 2005;20:303–16. https://doi.org/10.1037/0882-7974.20.2.303.
Lunn D (2013) The BUGS book: a practical introduction to Bayesian analysis. Texts Stat Sci Series.
Marron MM, et al. Heterogeneity of healthy aging: comparing long-lived families across five healthy aging phenotypes of blood pressure, memory, pulmonary function, grip strength, and metabolism. Geroscience. 2019. https://doi.org/10.1007/s11357-019-00086-y.
Matteini AM, et al. Heritability estimates of endophenotypes of long and health life: the long life family study. J Gerontol A Biol Sci Med Sci. 2010;65:1375–9. https://doi.org/10.1093/gerona/glq154.
Matyi JM, Rattinger GB, Schwartz S, Buhusi M, Tschanz JT. Lifetime estrogen exposure and cognition in late life: the Cache County Study. Menopause. 2019;26:1366–74. https://doi.org/10.1097/gme.0000000000001405.
Murman DL. The impact of age on cognition. Semin Hear. 2015;36:111–21. https://doi.org/10.1055/s-0035-1555115.
Newman AB, et al. Health and function of participants in the Long Life Family Study: a comparison with other. Cohorts Aging (Albany NY). 2011;3:63–76.
Núñez F, Maraver MJ, Colzato LS. Sex hormones as cognitive enhancers? J Cogn Enhancement. 2019;4(228):233. https://doi.org/10.1007/s41465-019-00156-1.
Rosano C, Newman AB, Katz R, Hirsch CH, Kuller LH. Association between lower digit symbol substitution test score and slower gait and greater risk of mortality and of developing incident disability in well-functioning older adults. J Am Geriatr Soc. 2008;56:1618–25. https://doi.org/10.1111/j.1532-5415.2008.01856.x.
Salmon DP, et al. Age and apolipoprotein E genotype influence rate of cognitive decline in nondemented elderly. Neuropsychology. 2013;27:391–401. https://doi.org/10.1037/a0032707.
Salthouse TA. Trajectories of normal cognitive aging. Psychol Aging. 2019;34:17–24. https://doi.org/10.1037/pag0000288.
Schneider AL, et al. Normative data for 8 neuropsychological tests in older blacks and whites from the atherosclerosis risk in communities (ARIC) study. Alzheimer Dis Assoc Disord. 2015;29:32–44. https://doi.org/10.1097/WAD.0000000000000042.
Schultz BG, Patten DK, Berlau DJ. The role of statins in both cognitive impairment and protection against dementia: a tale of two mechanisms. Transl Neurodegener. 2018;7:5. https://doi.org/10.1186/s40035-018-0110-3.
Sebastiani P, et al. APOE alleles and extreme human longevity. J Gerontol A Biol Sci Med Sci. 2018. https://doi.org/10.1093/gerona/gly174.
Sebastiani P, Hadley EC, Province M, Christensen K, Rossi W, Perls TT, et al. A family longevity selection score: ranking sibships by their longevity, size, and availability for study. Am J Epidemiol. 2009;170:1555–62. https://doi.org/10.1093/aje/kwp309.
Sebastiani P, Perls TT (2016) Detection of significant groups in hierarchical clustering by resampling. Front Genet 7 doi:https://doi.org/10.3389/fgene.2016.00144
Sebastiani P, Sun FX, Andersen SL, Lee JH, Wojczynski MK, Sanders JL, et al. Families enriched for exceptional longevity also have increased health-span: findings from the Long Life Family Study. Front Public Health. 2013;1:38. https://doi.org/10.3389/fpubh.2013.00038.
Sebastiani P, Thyagarajan B, Sun F, Honig LS, Schupf N, Cosentino S, et al. Age and sex distributions of age-related biomarker values in healthy older adults from the long life family study. J Am Geriatr Soc. 2016;64:e189–94. https://doi.org/10.1111/jgs.14522.
Sebastiani P, Thyagarajan B, Sun F, Schupf N, Newman AB, Montano M, et al. Biomarker signatures of aging. Aging Cell. 2017;16:329–38. https://doi.org/10.1111/acel.12557.
Singh-Manoux A, Dugravot A, Brunner E, Kumari M, Shipley M, Elbaz A, et al. Interleukin-6 and C-reactive protein as predictors of cognitive decline in late midlife. Neurology. 2014;83:486–93. https://doi.org/10.1212/WNL.0000000000000665.
Small BJ, Dixon RA, McArdle JJ. Tracking cognition-health changes from 55 to 95 years of age. J Gerontol B Psychol Sci Soc Sci. 2011;66(Suppl 1):i153–61. https://doi.org/10.1093/geronb/gbq093.
Wahlin A, MacDonald SW, deFrias CM, Nilsson LG, Dixon RA. How do health and biological age influence chronological age and sex differences in cognitive aging: moderating, mediating, or both? Psychol Aging. 2006;21:318–32. https://doi.org/10.1037/0882-7974.21.2.318.
Wechsel D (1981) Wechsler adult intelligence scale – revised. Harcourt brace Jovanovich [for] psychological Corp; revised edition.
Wechsel D. Wechsler adult intelligence scale—fourth edition administration and scoring manual. San Antonio: Pearson; 2008.
Wechsler D. WMS-R: Wechsler memory scale-revised manual. Harcourt Brace Jovanovich: Psychological Corp; 1987.
Weintraub S, et al. The Alzheimer’s disease centers’ uniform data set (UDS): the neuropsychologic test battery. Alzheimer Dis Assoc Disord. 2009;23:91–101. https://doi.org/10.1097/WAD.0b013e318191c7dd.
Wiecki TV, Poland G, Frank MJ. Model-based cognitive neuroscience approaches to computational psychiatry: clustering and classification. Clin Psychol Sci. 2015;3:378–99.
Wilson RS, Beckett LA, Barnes LL, Schneider JA, Bach J, Evans DA, et al. Individual differences in rates of change in cognitive abilities of older persons. Psychol Aging. 2002;17:179–93.
Acknowledgments
PS: designed the study, conducted the analyses, and drafted the manuscript; MD and BS: statistical analyses; SA: study design and interpretation of results; BT, SC, NS, KC, and TTP: interpretation of the results. All authors edited the manuscript.
Funding
This work was supported by the National Institute on Aging (NIA cooperative agreements U01-AG023712, U01-AG23744, U01-AG023746, U01-AG023749, U01-AG023755, U19AG023122, P30AG031679, R01AG061844, R21AG056630, and K01-AG057798), the National Institute of General Medical (NIGMS) Interdisciplinary Training Grant for Biostatisticians [T32 GM74905], and the Paulette and Marty Samowitz Family Foundation (TP).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Sebastiani, P., Andersen, S.L., Sweigart, B. et al. Patterns of multi-domain cognitive aging in participants of the Long Life Family Study. GeroScience 42, 1335–1350 (2020). https://doi.org/10.1007/s11357-020-00202-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11357-020-00202-3