Abstract
Purpose
Although sleep bruxism (SB) is one of the most important clinical problems in dental practice, there is no definitive method for controlling it. This pilot study evaluated the effects of contingent vibratory feedback stimuli using an occlusal splint for inhibition of sleep bruxism.
Methods
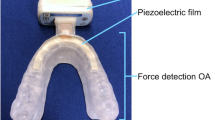
Thirteen subjects with clinically diagnosed SB participated after providing an informed consent. Portable polysomnographic recordings were conducted in the subjects’ home environment to make a definitive SB diagnosis and to evaluate the effects of the vibratory stimuli on SB. A force-based bruxism detection system, which used a pressure-sensitive piezoelectric film embedded in the occlusal splint, was utilized to trigger vibration feedback stimuli, which was scheduled to be applied intermittently for 30 min, at 30-min intervals.
Results
The number of SB episodes (times/hour), the total SB duration (seconds/hour), the mean duration of SB episodes (seconds/episode), and the micro-arousal index (times/hour) were scored for each time period (with and without vibration). The effects of the vibration on these scores were tested (paired t test; p < 0.05). The number of SB episodes tended to decrease with the vibration stimuli, and the decrease in the total SB duration was statistically significant (14.3 ± 9.5 vs. 26.0 ± 20.0, p = 0.03). No substantial change was found in terms of the micro-arousal index.
Conclusions
These study results suggested that the SB inhibitory system employing a vibratory stimulus might be able to suppress the total SB duration without disturbing sleep.







Similar content being viewed by others
References
Sateia MJ, Buysse DJ, Krystal AD, Neubauer DN, Heald JL (2017) Clinical practice guideline for the pharmacologic treatment of chronic insomnia in adults: an American Academy of Sleep Medicine clinical practice guideline. J Clin Sleep Med 13:307–349
Abe S, Yamaguchi T, Rompre PH, De Grandmont P, Chen YJ, Lavigne GJ (2009) Tooth wear in young subjects: a discriminator between sleep bruxers and controls? Int J Prosthodont 22:342–350
Yoshida Y, Suganuma T, Takaba M, Ono Y, Abe Y, Yoshizawa S, Sakai T, Yoshizawa A, Nakamura H, Kawana F, Baba K (2017) Association between patterns of jaw motor activity during sleep and clinical signs and symptoms of sleep bruxism. J Sleep Res 26:415–421
Yoshizawa S, Suganuma T, Takaba M, Ono Y, Sakai T, Yoshizawa A, Kawana F, Kato T, Baba K (2014) Phasic jaw motor episodes in healthy subjects with or without clinical signs and symptoms of sleep bruxism: a pilot study. Sleep Breath 18:187–193
Lin WS, Ercoli C, Lowenguth R, Yerke LM, Morton D (2012) Oral rehabilitation of a patient with bruxism and cluster implant failures in the edentulous maxilla: a clinical report. J Prosthet Dent 108:1–8
Baba K, Haketa T, Sasaki Y, Ohyama T, Clark GT (2005) Association between masseter muscle activity levels recorded during sleep and signs and symptoms of temporomandibular disorders in healthy young adults. J Orofac Pain 19:226–231
Jokubauskas L, Baltrusaityte A, Pileicikiene G (2018) Oral appliances for managing sleep bruxism in adults: a systematic review from 2007 to 2017. J Oral Rehabil 45:81–95
Sakai T, Kato T, Yoshizawa S, Suganuma T, Takaba M, Ono Y, Yoshizawa A, Yoshida Y, Kurihara T, Ishii M, Kawana F, Kiuchi Y, Baba K (2017) Effect of clonazepam and clonidine on primary sleep bruxism: a double-blind, crossover, placebo-controlled trial. J Sleep Res 26:73–83
Manfredini D, Ahlberg J, Winocur E, Lobbezoo F (2015) Management of sleep bruxism in adults: a qualitative systematic literature review. J Oral Rehabil 42:862–874
Jadidi F, Castrillon EE, Nielsen P, Baad-Hansen L, Svensson P (2013) Effect of contingent electrical stimulation on jaw muscle activity during sleep: a pilot study with a randomized controlled trial design. Acta Odontol Scand 71:1050–1062
Nishigawa K, Kondo K, Takeuchi H, Clark GT (2003) Contingent electrical lip stimulation for sleep bruxism: a pilot study. J Prosthet Dent 89:412–417
Watanabe T, Baba K, Yamagata K, Ohyama T, Clark GT (2001) A vibratory stimulation-based inhibition system for nocturnal bruxism: a clinical report. J Prosthet Dent 85:233–235
Harada T, Ichiki R, Tsukiyama Y, Koyano K (2006) The effect of oral splint devices on sleep bruxism: a 6-week observation with an ambulatory electromyographic recording device. J Oral Rehabil 33:482–488
Huynh N, Lavigne GJ, Lanfranchi PA, Montplaisir JY, de Champlain J (2006) The effect of 2 sympatholytic medications-propranolol and clonidine-on sleep bruxism: experimental randomized controlled studies. Sleep 29:307–316
Lobbezoo F, van der Zaag J, van Selms MK, Hamburger HL, Naeije M (2008) Principles for the management of bruxism. J Oral Rehabil 35:509–523
Valiente Lopez M, van Selms MK, van der Zaag J, Hamburger HL, Lobbezoo F (2015) Do sleep hygiene measures and progressive muscle relaxation influence sleep bruxism? Report of a randomised controlled trial. J Oral Rehabil 42:259–265
Cassisi JE, McGlynn FD, Belles DR (1987) EMG-activated feedback alarms for the treatment of nocturnal bruxism: current status and future directions. Biofeedback Self Regul 12:13–30
Kardachi BJ, Clarke NG (1977) The use of biofeedback to control bruxism. J Periodontol 48:639–642
Dube C, Rompre PH, Manzini C, Guitard F, de Grandmont P, Lavigne GJ (2004) Quantitative polygraphic controlled study on efficacy and safety of oral splint devices in tooth-grinding subjects. J Dent Res 83:398–403
Rompre PH, Daigle-Landry D, Guitard F, Montplaisir JY, Lavigne GJ (2007) Identification of a sleep bruxism subgroup with a higher risk of pain. J Dent Res 86:837–842
Baba K, Clark GT, Watanabe T, Ohyama T (2003) Bruxism force detection by a piezoelectric film-based recording device in sleeping humans. J Orofac Pain 17:58–64
Takeuchi H, Ikeda T, Clark GT (2001) A piezoelectric film-based intrasplint detection method for bruxism. J Prosthet Dent 86:195–202
Levendowski DJ, Ferini-Strambi L, Gamaldo C, Cetel M, Rosenberg R, Westbrook PR (2017) The accuracy, night-to-night variability, and stability of frontopolar sleep electroencephalography biomarkers. J Clin Sleep Med 13:791–803
Lavigne GJ, Rompre PH, Montplaisir JY (1996) Sleep bruxism: validity of clinical research diagnostic criteria in a controlled polysomnographic study. J Dent Res 75:546–552
Lavigne GJ, Guitard F, Rompre PH, Montplaisir JY (2001) Variability in sleep bruxism activity over time. J Sleep Res 10:237–244
Dutra KM, Pereira FJ Jr, Rompre PH, Huynh N, Fleming N, Lavigne GJ (2009) Oro-facial activities in sleep bruxism patients and in normal subjects: a controlled polygraphic and audio-video study. J Oral Rehabil 36:86–92
Jadidi F, Norregaard O, Baad-Hansen L, Arendt-Nielsen L, Svensson P (2011) Assessment of sleep parameters during contingent electrical stimulation in subjects with jaw muscle activity during sleep: a polysomnographic study. Eur J Oral Sci 119:211–218
Rugh JD, Johnson RW (1981) Temporal analysis of nocturnal bruxism during EMG feedback. J Periodontol 52:263–265
Pierce CJ, Gale EN (1988) A comparison of different treatments for nocturnal bruxism. J Dent Res 67:597–601
Kato T, Rompre P, Montplaisir JY, Sessle BJ, Lavigne GJ (2001) Sleep bruxism: an oromortor activity secondary to micro-arousal. J Dent Res 80:40–44
Funding
This study was supported by Japan Society for the Promotion of Science KAKENHI Grant No. 16K20514, Grant-in-Aid for Young Scientists (B).
Author information
Authors and Affiliations
Contributions
K Baba and H Nakamura designed the study. H Nakamura, M Takaba, Y Abe, and S Yoshizawa wrote the initial draft of the manuscript. Y Nakazato and Y Yoshida contributed to analysis and interpretation of data, and assisted in the preparation of the manuscript. All other authors have contributed to data collection and interpretation, and critically reviewed the manuscript. All authors approved the final version of the manuscript and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee (Ethics Committee of Showa University School of Dentistry, No.2014-034) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Statement of informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nakamura, H., Takaba, M., Abe, Y. et al. Effects of a contingent vibratory stimulus delivered by an intra-oral device on sleep bruxism: a pilot study. Sleep Breath 23, 363–372 (2019). https://doi.org/10.1007/s11325-019-01782-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-019-01782-x