Abstract
Purpose
Weight loss leads to improvement of obstructive sleep apnea (OSA), based on frequency of respiratory events (apnea-hypopnea index, AHI). However, AHI does not incorporate the severity of individual obstruction events. The American Academy of Sleep Medicine suggests two alternative oxygen desaturation thresholds (ODT) for scoring of hypopneas. We hypothesize that lowering the ODT level increases the determined impact of weight loss on OSA severity. We investigate this during weight change with AHI and adjusted AHI. Adjusted AHI is a novel parameter incorporating both severity and number of the events.
Methods
Ambulatory polygraphic data of 54 OSA patients (F 15/M 39, 51.7 ± 8.4 years), divided into weight loss (>5 %, n = 20), control (weight change 0–5 %, n = 26), and weight gain (>5 %, n = 8) groups, were evaluated at baseline and after 5-year follow-up. Effect of ODT (ODT2%–ODT6%) on AHI and adjusted AHI was investigated.
Results
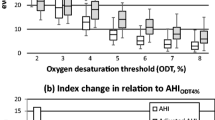
The greatest changes in AHI (decrease in weight loss group and increase in weight gain group) were observed with ODT2%. Changes in AHI diminished with increasing ODT. In weight loss group, adjusted AHI showed a similar but non-significant trend. In contrast, the higher ODT was used in weight gain group, the greater increase in adjusted AHI resulted. Using adjusted AHI instead of AHI, led to a smaller number of patients (20 vs. 55 %, ODT3%) whose OSA severity category improved along weight loss.
Conclusions
Weight loss significantly reduced AHI. This reduction was highly dependent on selected ODT. The change in adjusted AHI did not occur in the same extent. This was expected as the more severe events which tend to remain during the weight loss have greater importance in adjusted AHI, while the event severity is neglected in AHI.


Similar content being viewed by others
References
Peppard PE, Young T, Palta M, Dempsey J, Skatrud J (2000) Longitudinal study of moderate weight change and sleep-disordered breathing. JAMA 284:3015–3021
Wolk R, Shamsuzzaman AS, Somers VK (2003) Obesity, sleep apnea, and hypertension. Hypertension 42:1067–1074
Young T, Skatrud J, Peppard PE (2004) Risk factors for obstructive sleep apnea in adults. JAMA 291:2013–2016
Strobel RJ, Rosen RC (1996) Obesity and weight loss in obstructive sleep apnea: a critical review. Sleep 19:104–115
Vgontzas AN (2008) Does obesity play a major role in the pathogenesis of sleep apnoea and its associated manifestations via inflammation, visceral adiposity, and insulin resistance? Arch Physiol Biochem 114:211–223
Foster GD, Borradaile KE, Sanders MH, Sleep AHEAD Research Group of Look AHEAD Research Group et al (2009) A randomized study on the effect of weight loss on obstructive sleep apnea among obese patients with type 2 diabetes: the Sleep AHEAD study. Arch Intern Med 169:1619–1626
Tuomilehto H, Seppa J, Uusitupa M (2013) Obesity and obstructive sleep apnea—clinical significance of weight loss. Sleep Med Rev 17:321–329
Pillar G, Shehadeh N (2008) Abdominal fat and sleep apnea: the chicken or the egg? Diabetes Care 31(Suppl 2):S303–S309
American Academy of Sleep Medicine (1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The Report of an American Academy of Sleep Medicine Task Force. Sleep 22:667–689
Iber C, Ancoli-Israel S, Chesson AL Jr, Quan SF, for the American Academy of Sleep Medicine (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester
Berry RB, Budhiraja R, Gottlieb DJ, American Academy of Sleep Medicine et al (2012) Rules for scoring respiratory events in sleep: update of the 2007 AASM manual for the scoring of sleep and associated events. Deliberations of the Sleep Apnea Definitions Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 8:597–619
AASM suspends required use of 3 percent hypopnea desaturation scoring criterion. (August 27, 2013) American Academy of Sleep Medicine. http://www.aasmnet.org/articles.aspx?id=4132. Accessed 5 May 2014
Manser RL, Rochford P, Pierce RJ, Byrnes GB, Campbell DA (2001) Impact of different criteria for defining hypopneas in the apnea-hypopnea index. Chest 120:909–914
Mehra R, Benjamin EJ, Shahar E et al (2006) Association of nocturnal arrhythmias with sleep-disordered breathing: the sleep heart health study. Am J Respir Crit Care Med 173:910–916
Ruehland WR, Rochford PD, O'Donoghue FJ, Pierce RJ, Singh P, Thornton AT (2009) The new AASM criteria for scoring hypopneas: impact on the apnea hypopnea index. Sleep 32:150–157
Bahammam AS, Obeidat A, Barataman K, Bahammam SA, Olaish AH, Sharif MM (2014) A comparison between the AASM 2012 and 2007 definitions for detecting hypopnea. Sleep Breath 18:767–773
Myllymaa S, Myllymaa K, Kupari S et al (2015) Effect of different oxygen desaturation threshold levels on hypopnea scoring and classification of severity of sleep apnea. Sleep Breath. doi:10.1007/s11325-015-1118-x
Shahar E (2014) Apnea-hypopnea index: time to wake up. Nat Sci Sleep 6:51–56
Tam S, Woodson BT, Rotenberg B (2014) Outcome measurements in obstructive sleep apnea: beyond the apnea-hypopnea index. Laryngoscope 124:337–343
Muraja-Murro A, Kulkas A, Hiltunen M et al (2013) The severity of individual obstruction events is related to increased mortality rate in severe obstructive sleep apnea. J Sleep Res 22:663–669
Otero A, Felix P, Presedo J, Zamarron C (2012) An evaluation of indexes as support tools in the diagnosis of sleep apnea. Ann Biomed Eng 40:1825–1834
Kulkas A, Tiihonen P, Julkunen P, Mervaala E, Toyras J (2013) Novel parameters indicate significant differences in severity of obstructive sleep apnea with patients having similar apnea-hypopnea index. Med Biol Eng Comput 51:697–708
Berger G, Berger R, Oksenberg A (2009) Progression of snoring and obstructive sleep apnoea: the role of increasing weight and time. Eur Respir J 33:338–345
Johansson K, Neovius M, Lagerros YT et al (2009) Effect of a very low energy diet on moderate and severe obstructive sleep apnoea in obese men: a randomised controlled trial. BMJ 339:b4609
Tuomilehto HP, Seppa JM, Partinen MM, Kuopio Sleep Apnea Group et al (2009) Lifestyle intervention with weight reduction: first-line treatment in mild obstructive sleep apnea. Am J Respir Crit Care Med 179:320–327
Tuomilehto H, Gylling H, Peltonen M, Kuopio Sleep Apnea Group et al (2010) Sustained improvement in mild obstructive sleep apnea after a diet- and physical activity-based lifestyle intervention: postinterventional follow-up. Am J Clin Nutr 92:688–696
Kuna ST, Reboussin DM, Borradaile KE, Sleep AHEAD Research Group of the Look AHEAD Research Group et al (2013) Long-term effect of weight loss on obstructive sleep apnea severity in obese patients with type 2 diabetes. Sleep 36:641–649A
Kulkas A, Leppanen T, Sahlman J et al (2013) Novel parameters reflect changes in morphology of respiratory events during weight loss. Physiol Meas 34:1013–1026
Kulkas A, Leppänen T, Sahlman J et al (2014) Weight loss alters severity of individual nocturnal respiratory events depending on sleeping position. Physiol Meas 35:2037–2052
Muraja-Murro A, Kulkas A, Hiltunen M et al (2014) Adjustment of apnea-hypopnea index with severity of obstruction events enhances detection of sleep apnea patients with the highest risk of severe health consequences. Sleep Breath 18:641–647
Tuomilehto H, Seppä J, Uusitupa M, Tuomilehto J, Gylling H (2013) Weight reduction and increased physical activity to prevent the progression of obstructive sleep apnea: a 4-year observational postintervention follow-up of a randomized clinical trial. JAMA Intern Med 173:930–932
Tuomilehto H, Seppä J, Uusitupa M, Kuopio Sleep Apnea Group et al (2014) The impact of weight reduction in the prevention of the progression of obstructive sleep apnea: an explanatory analysis of a 5-year observational follow-up trial. Sleep Med 15:329–335
Punjabi NM, Caffo BS, Goodwin JL et al (2009) Sleep-disordered breathing and mortality: a prospective cohort study. PLoS Med 6:e1000132
Peppard PE, Ward NR, Morrell MJ (2009) The impact of obesity on oxygen desaturation during sleep-disordered breathing. Am J Respir Crit Care Med 180:788–793
Sato M, Suzuki M, Suzuki J et al (2008) Overweight patients with severe sleep apnea experience deeper oxygen desaturation at apneic events. J Med Dent Sci 55:43–47
Collop NA, Anderson WM, Boehlecke B, Portable Monitoring Task Force of the American Academy of Sleep Medicine et al (2007) Clinical guidelines for the use of unattended portable monitors in the diagnosis of obstructive sleep apnea in adult patients. Portable Monitoring Task Force of the American Academy of Sleep Medicine. J Clin Sleep Med 3:737–747
Acknowledgments
This study work was financially supported by grants from the Research Committee of the Kuopio University Hospital Catchment Area for the State Research Funding (Projects 5041732, 5041733, and 5041748) and Seinäjoki Central Hospital, the Competitive State Research Financing of the Expert Responsibility Area of Tampere University Hospital (Grant Numbers VTR3040 and VTR3114). One author (KM) is supported by the Finnish Cultural Foundation of Northern Savo and the Finnish Brain Foundation.
Author information
Authors and Affiliations
Corresponding author
Additional information
Katja Myllymaa and Sami Myllymaa contributed equally to this work.
Rights and permissions
About this article
Cite this article
Myllymaa, K., Myllymaa, S., Leppänen, T. et al. Effect of oxygen desaturation threshold on determination of OSA severity during weight loss. Sleep Breath 20, 33–42 (2016). https://doi.org/10.1007/s11325-015-1180-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-015-1180-4