Abstract
Purpose
Sympathetic activation induced by sleep-disordered breathing may contribute to cardiovascular morbidity. However, the apnea–hypopnea index (AHI) excludes respiratory effort-related arousals (RERAs) associated with inspiratory flow limitation without oxygen desaturation. We sought to determine whether RERAs are associated with sympathetic activation.
Methods
Twenty-five adults (12 males, 13 females) with AHI < 10/h and RERA index >5/h were included in this study. Power spectral density analysis was performed on two non-contiguous 10-min segments containing inspiratory flow limitation and arrhythmia-free electrocardiogram during N2 sleep. One segment contained RERA; the other did not, NO-RERA. Spectral power was described in a low-frequency domain (LF; 0.04–0.15 Hz), primarily sympathetic modulation, and a high frequency domain (HF; 0.15–0.4 Hz), parasympathetic modulation.
Results
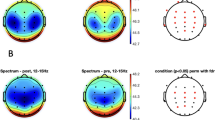
Analyses of LF and HF powers were made using normalized and absolute values. LF power was greater during RERA compared to NO-RERA (50.3 vs. 30.1 %, p < 0.001) whereas HF power was greater during NO-RERA compared to RERA (69.9 vs. 49.7 %, p < 0.001). The LF/HF ratio was greater during RERA than NO-RERA (1.01 vs. 0.43, p < 0.001). Gender differences emerged using absolute values of power: The percentage increase in LF power during RERA relative to NO-RERA was significantly greater for females than males, 247.6 vs. 31.9 %, respectively (p < 0.02).
Conclusions
RERAs are associated with a marked increase in cardiac sympathetic modulation, especially in females. Patients with a high RERA index, even in the setting of a low or normal AHI, may be exposed to elevated sympathetic tone during sleep.


Similar content being viewed by others
References
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. New Engl J Med 342:1378–1384
Nieto FJ, Young TB, Lind BK, Shahar E, Samet JM, Redline S, D’Agostino RB, Newman AB, Lebowitz MD, Pickering TG (2000) Association of sleep-disordered breathing, sleep apnea, and hypertension in a large community-based study. JAMA 283:1829–1836
Lattimore JD, Celermajer DS, Wilcox I (2003) Obstructive sleep apnea and cardiovascular disease. J Am Coll Cardiol 41:1429–1437
Leung RST, Bradley DT (2001) Sleep apnea and cardiovascular disease. Am J Respir Crit Care Med 64:2147–2165
Newman AB, Nieto FJ, Guidry U, Lind BK, Redline S, Pickering TG, Quan SF (2001) Relation of sleep-disordered breathing to cardiovascular disease risk factors. Am J Epidemiol 154:50–59
Manser RL, Rochford P, Naughton MT, Pierce RJ, Sasse A, Teichtahl H, Ho M, Campbell DA (2002) Measurement variability in sleep disorders medicine: the Victorian experience. Intern Med J 32:386–393
Moser NJ, Phillips BA, Berry DT, Harbison L (1994) What is hypopnea, anyway? Chest 105:426–428
Iber C, Ancoli-Israel S, Chesson Jr AL, Quan SF (2007) The AASM manual for the scoring of sleep and associated events rules, terminology and technical specifications. American Academy of Sleep Medicine, Darien
Bonnet M, Arand D (1997) Heart rate variability: sleep stage, time of night, and arousal influences. Electroencephalogr Clin Neurophysiol 102:390–396
Tarvainen MP, Ranta-Aho PO, Karjalainen PA (2002) An advanced detrending method with application to HRV analysis. IEEE Trans Biomed Eng 49:172–175
Vanoli E, Adamson PB, Ba-Lin PGD, Lazzara R, Orr WC (1995) Heart rate variability during specific sleep stages: a comparison of healthy subjects with patients after myocardial infarction. Circulation 91:1918–1922
Hornyak M, Cejnar M, Elam M, Matousek M, Wallin BG (1991) Sympathetic muscle nerve activity during sleep in man. Brain 114:1281–1295
Burgess HJ, Trinder J, Kim Y, Luke D (1997) Sleep and circadian influences on cardiac autonomic nervous system activity. Am J Physiol 273:H1761–H1768
Parish JM, Somers VK (2004) Obstructive sleep apnea and cardiovascular disease. Mayo Clin Proc 79:1036–1046
Reynolds EB, Seda G, Ware JC, Vinik AI, Risk MR, Fishback NF (2007) Autonomic function in sleep apnea patients: increased heart rate variability except during REM sleep in obese patients. Sleep Breath 11:53–60
The Report of an American Academy of Sleep Medicine Task Force (1999) Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. Sleep 22:667–689
Bonnet M, Carskadon M, Easton P, Guilleminault C, Harper R, Hayes B, Hirshkowitz M, Ktonas P, Keenan S, Pressman M, Roehrs T, Smith J, Walsh J, Weber S, Westbrook P (1992) EEG arousals: scoring rules and examples: a preliminary report from the sleep disorders atlas task force of the American Sleep Disorders Association, ASDA atlas task force. Sleep 15:173–184
Bloch KE, Russi EW, Kaplan V (2004) Variability of inspiratory conductance quantifies flow limitation. Clin Sci 106:589–598
Teschler H, Berthon-Jones M, Thompson AB, Henkel A, Henry J, Konietzko N (1996) Automated continuous positive airway pressure titration for obstructive sleep apnea syndrome. Am J Respir Crit Care Med 154:734–740
Huikuri H, Niemela M, Ojala S, Rantala A, Ikaheimo M, Airaksinen K (1994) Circadian rhythms of frequency domain measures of heart rate variability in healthy subjects and patients with coronary artery disease. Effects of arousal and upright posture. Circulation 90:121–126
Malliani A (1999) The pattern of sympathovagal balance explored in the frequency domain. News Physiol Sci 14:111–117
Niskanen JP, Tarvainen MP, Ranta-aho PO, Karjalainen PA (2004) Software for advanced HRV analysis. Comput Methods Programs Biomed 76(1):73–81
Burr RL (2007) Interpretation of normalized spectral heart rate variability indices in sleep research. Sleep 30:913–919
Dart AM, Du XJ, Kingwell BA (2002) Gender, sex hormones and autonomic nervous control of the cardiovascular system. Cardiovasc Res 53:678–687
Nugent AC, Bain EE, Thayer JF, Sollers JJ, Drevets WC (2011) Sex differences in the neural correlates of autonomic arousal: a pilot PET study. Int J Psychophysiol 80:182–191
Matsukawa T, Sugiyama Y, Watanabe T, Kobayashi F, Mano T (1998) Gender differences in age-related changes in muscle sympathetic nerve activity in healthy subjects. Am J Physiol 275:R1600–R1604
Narkiewicz K, Phillips BG, Kato M, Hering D, Bieniaszewski L, Somers VK (2005) Gender-selective interaction between aging, blood pressure, and sympathetic nerve activity. Hypertension 45:522–525
Ng A, Callister R, Johnson D, Seals D (1993) Age and gender influence muscles sympathetic nerve activity at rest in healthy humans. Hypertension 21:498–503
Guilleminault C, Poyares D, Rosa A, Huang YS (2005) Heart rate variability, sympathetic and vagal balance and EEG arousals in upper airway resistance and mild obstructive sleep apnea syndromes. Sleep Med 6:451–457
da Silva SP, Hulce VD, Backs RW (2009) Effects of obstructive sleep apnea on autonomic cardiac control during sleep. Sleep Breath 13:147–156
Narkiewicz K, Montano N, Cogliati C, van de Borne PJH, Dyken ME, Somers VK (1998) Altered cardiovascular variability in obstructive sleep apnea. Circulation 98:1071–1077
Conflicts of interest
None of the authors report any conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Work was performed at North Shore LIJ Sleep Disorders Center, Division of Pulmonary, Critical Care and Sleep Medicine, Hofstra North Shore-LIJ School of Medicine, New Hyde Park, NY.
Rights and permissions
About this article
Cite this article
Chandra, S., Sica, A.L., Wang, J. et al. Respiratory effort-related arousals contribute to sympathetic modulation of heart rate variability. Sleep Breath 17, 1193–1200 (2013). https://doi.org/10.1007/s11325-013-0823-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-013-0823-6