Abstract
Objective
This study was conducted to evaluate the association between weight gain and variability of sleep duration.
Methods
A retrospective cohort study was conducted involving apparently healthy individuals aged 20 years or older who underwent annual health checkup at the Center for Preventive Medicine, St. Luke’s International Hospital, between 2007 and 2010. The body mass index (BMI) of each participant was measured, and the change in BMI during the study period was calculated. The sleep duration was obtained using a questionnaire that was filled out by participants each year, and the variability in the sleep duration was calculated by dividing the standard deviation (SD) of the sleep duration for 3 years by the square root of the number of data points. Multivariate linear regression analysis was used to explore the association between the change in BMI and the variability of the sleep duration, adjusting for age, sex, alcohol consumption, current smoking, baseline sleep duration, past medical history, and level of physical activity.
Results
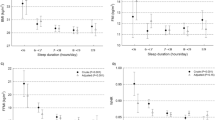
A total of 21,148 participants were included in this study. The mean age (SD) was 51 (12) years, and 10,993 (49.6%) participants were male. The mean baseline BMI was 22.4 (SD 3.2). According to the self-reported data, the mean sleep duration (SD) was 6.2 (1.0) h, and the mean of the SD of sleep duration for each participant was 0.32 (min–max, 0–7). The result of the linear regression analysis showed that greater variability in the sleep duration was independently related to an increase in BMI (β coefficient = 0.31; 95% CI = 0.01–0.61).
Conclusion
The variability of sleep duration is related to body weight gain. Maintaining a constant sleep duration may be recommended for controlling body weight.

Similar content being viewed by others
References
Organization for Economic Co-operation and Development. Obesity and the economics of prevention: fit not fat. http://www.oecd.org/document/31/0,3343,en_2649_33929_45999775_1_1_1_1,00.html. Accessed 9 Sep 2011
The Ministry of Health, Labour and Welfare in Japan. National health and nutrition surveillance (2004) http://www.mhlw.go.jp/houdou/2006/05/h0508-1a.html. Accessed 9 Sep 2011
The Ministry of Health, Labour and Welfare in Japan. National nutrition surveillance (1999) (2000) http://www.mhlw.go.jp/houdou/0103/h0309-7.html. Accessed 20 Dec 2011
The Ministry of Health, Labour and Welfare in Japan. National health and nutrition surveillance (2009) 2010; http://www.mhlw.go.jp/stf/houdou/2r9852000000xtwq-att/2r9852000000xu2x.pdf. Accessed 20 Dec 2011
Stevens J, Cai J, Pamuk ER, Williamson DF, Thun MJ, Wood JL (1998) The effect of age on the association between body-mass index and mortality. N Engl J Med 338(1):1–7
Hubert HB, Feinleib M, McNamara PM, Castelli WP (1983) Obesity as an independent risk factor for cardiovascular disease: a 26-year follow-up of participants in the Framingham Heart Study. Circulation 67(5):968–977
Jousilahti P, Tuomilehto J, Vartiainen E, Pekkanen J, Puska P (1996) Body weight, cardiovascular risk factors, and coronary mortality. 15-year follow-up of middle-aged men and women in eastern Finland. Circulation 93(7):1372–1379
Kobayashi D, Takahashi O, Deshpande GA, Shimbo T, Fukui T (2011) Relation between metabolic syndrome and sleep duration in Japan: a large scale cross-sectional study. Intern Med 50(2):103–107
Kobayashi D, Takahashi O, Deshpande GA, Shimbo T, Fukui T (2012) Association between osteoporosis and sleep duration in healthy middle-aged and elderly adults: a large-scale, cross-sectional study in Japan. Sleep Breath. doi:10.1007/s11325-011-0545-6
Kotchen TA (2010) Obesity-related hypertension: epidemiology, pathophysiology, and clinical management. Am J Hypertens 23(11):1170–1178
Whitmore C (2010) Type 2 diabetes and obesity in adults. Br J Nurs 19(14):880, 882–886
Sayeed MA, Mahtab H, Latif ZA, Khanam PA, Ahsan KA, Banu A, Azad Khan AK (2003) Waist-to-height ratio is a better obesity index than body mass index and waist-to-hip ratio for predicting diabetes, hypertension and lipidemia. Bangladesh Med Res Counc Bull 29(1):1–10
American Gastroenterological Association (2002) American Gastroenterological Association medical position statement on obesity. Gastroenterology 123(3):879–881
Seicean A, Redline S, Seicean S, Kirchner HL, Gao Y, Sekine M, Zhu X, Storfer-Isser A (2007) Association between short sleeping hours and overweight in adolescents: results from a US suburban high school survey. Sleep Breath 11(4):285–293
Watanabe M, Kikuchi H, Tanaka K, Takahashi M (2010) Association of short sleep duration with weight gain and obesity at 1-year follow-up: a large-scale prospective study. Sleep 33(2):161–167
Nishiura C, Hashimoto H (2010) A 4-year study of the association between short sleep duration and change in body mass index in Japanese male workers. J Epidemiol 20(5):385–390
Kobayashi D, Takahashi O, Deshpande GA, Shimbo T, Fukui T (2011) Association between weight gain, obesity, and sleep duration: a large-scale 3-year cohort study. Sleep Breath. doi:10.1007/s11325-011-0583-0
Kilpatrick ES, Rigby AS, Atkin SL (2010) The role of blood pressure variability in the development of nephropathy in type 1 diabetes. Diabetes Care 33(11):2442–2447
Alvarez-Castro P, Sangiao-Alvarellos S, Brandon-Sanda I, Cordido F (2011) Endocrine function in obesity. Endocrinol Nutr 58(8):422–432
Beccuti G, Pannain S (2011) Sleep and obesity. Curr Opin Clin Nutr Metab Care 14(4):402–412
Hasler G, Buysse DJ, Klaghofer R, Gamma A, Ajdacic V, Eich D, Rössler W, Angst J (2004) The association between short sleep duration and obesity in young adults: a 13-year prospective study. Sleep 27(4):661–666
Spruyt K, Molfese DL, Gozal D (2011) Sleep duration, sleep regularity, body weight, and metabolic homeostasis in school-aged children. Pediatrics 127(2):e345–e352
Minors DS, Waterhouse JM, Akerstedt T (1994) The effect of the timing, quality and quantity of sleep upon the depression (masking) of body temperature on an irregular sleep/wake schedule. J Sleep Res 3(1):45–51
Akerstedt T, Hume K, Minors D, Waterhouse J (1994) The meaning of good sleep: a longitudinal study of polysomnography and subjective sleep quality. J Sleep Res 3(3):152–158
Bidulescu A, Din-Dzietham R, Coverson DL, Chen Z, Meng YX, Buxbaum SG, Gibbons GH, Welch VL (2010) Interaction of sleep quality and psychosocial stress on obesity in African Americans: the Cardiovascular Health Epidemiology Study (CHES). BMC Publ Health 10:581
Esser KA, Young ME (2009) The role of clock genes in cardiometabolic disease. J Appl Physiol 107(4):1316–1317
Spiegel K, Tasali E, Penev P, Van Cauter E (2004) Brief communication: sleep curtailment in healthy young men is associated with decreased leptin levels, elevated ghrelin levels, and increased hunger and appetite. Ann Intern Med 141(11):846–850
Considine RV, Sinha MK, Heiman ML, Kriauciunas A, Stephens TW, Nyce MR, Ohannesian JP, Marco CC, McKee LJ, Bauer TL, Caro JF (1996) Serum immunoreactive-leptin concentrations in normal-weight and obese humans. N Engl J Med 334(5):292–295
Inui A, Asakawa A, Bowers CY, Mantovani G, Laviano A, Meguid MM, Fujimiya M (2004) Ghrelin, appetite, and gastric motility: the emerging role of the stomach as an endocrine organ. FASEB J 18(3):439–456
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235
Acknowledgment
We gratefully acknowledge Dr. Toshiko Kawakita for contributing data from the Center for Preventive Medicine at St. Luke’s International Hospital.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kobayashi, D., Takahashi, O., Shimbo, T. et al. High sleep duration variability is an independent risk factor for weight gain. Sleep Breath 17, 167–172 (2013). https://doi.org/10.1007/s11325-012-0665-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-012-0665-7