Abstract
Introduction
Based on a mail-out questionnaire, this study analyzed compliance and side effects of one commonly used (TheraSnore) boil and bite oral appliance (OA) in patients with obstructive sleep apnea.
Methods
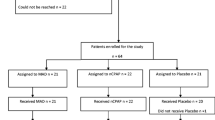
The questionnaire was sent to 84 patients 6 months after the delivery of the OA.
Results
Fifty-eight percent (n = 47) of the patients returned the questionnaire. There was no significant difference in baseline data [age, body mass index (BMI), apnea–hypopnea index or the Epworth Sleepiness Scale (ESS)] between the returned and nonreturned questionnaires. Of the responding patients, 74.5% (n = 35) continued to use the appliance. Nonusers had a higher BMI and higher baseline ESS when compared with users. The majority (74.3%) of the users and 50.0% of the nonusers previously used a nasal continuous positive airway pressure machine. Some 82.9% of the users wore their OA more than 3 days a week. Of the nonusers, 77.8% stopped using the OA in the first 3 months, and the most frequent reason given was “uncomfortable.” Many users complained about a dry mouth and/or excessive salivation and nonusers significantly complained more about ill-fitting appliances. Over 80% of the users experienced improvement in their snoring, daytime sleepiness, and apnea. More than 60% of the users were satisfied with OA therapy.
Conclusion
While this study demonstrated similar self-reported compliance as previous reports, there were different side effects from those reported for custom-made appliances. Difficulty in optimal fit is considered to be the main cause of the subsequent stopping of the use of the boil and bite appliance.




Similar content being viewed by others
References
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Weaver TE, Grunstein RR (2008) Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc 5:173–178
Rosenthal L, Gerhardstein R, Lumley A, Guido P, Day R, Syron ML, Roth T (2000) CPAP therapy in patients with mild OSA: implementation and treatment outcome. Sleep Med 1:215–220
Kushida CA, Morgenthaler TI, Littner MR, Alessi CA, Bailey D, Coleman J Jr, Friedman L, Hirshkowitz M, Kapen S, Kramer M, Lee-Chiong T, Owens J, Pancer JP (2006) Practice parameters for the treatment of snoring and obstructive sleep apnea with oral appliances: an update for 2005. Sleep 29:240–243
Marklund M, Franklin KA, Persson M (2001) Orthodontic side-effects of mandibular advancement devices during treatment of snoring and sleep apnoea. Eur J Orthod 23:135–144
Ringqvist M, Walker-Engstrom ML, Tegelberg A, Ringqvist I (2003) Dental and skeletal changes after 4 years of obstructive sleep apnea treatment with a mandibular advancement device: a prospective, randomized study. Am J Orthod Dentofacial Orthop 124:53–60
Pantin CC, Hillman DR, Tennant M (1999) Dental side effects of an oral device to treat snoring and obstructive sleep apnea. Sleep 22:237–240
McGown AD, Makker HK, Battagel JM, L'Estrange PR, Grant HR, Spiro SG (2001) Long-term use of mandibular advancement splints for snoring and obstructive sleep apnoea: a questionnaire survey. Eur Respir J 17:462–466
Clark GT, Sohn JW, Hong CN (2000) Treating obstructive sleep apnea and snoring: assessment of an anterior mandibular positioning device. J Am Dent Assoc 131:765–771
Fransson AM, Tegelberg A, Leissner L, Wenneberg B, Isacsson G (2003) Effects of a mandibular protruding device on the sleep of patients with obstructive sleep apnea and snoring problems: a 2-year follow-up. Sleep Breath 7:131–141
Vanderveken OM, Devolder A, Marklund M, Boudewyns AN, Braem MJ, Okkerse W, Verbraecken JA, Franklin KA, De Backer WA, Van de Heyning PH (2008) Comparison of a custom-made and a thermoplastic oral appliance for the treatment of mild sleep apnea. Am J Respir Crit Care Med 178:197–202
Ferguson KA, Cartwright R, Rogers R, Schmidt-Nowara W (2006) Oral appliances for snoring and obstructive sleep apnea: a review. Sleep 29:244–262
Izci B, McDonald JP, Coleman EL, Mackay TW, Douglas NJ, Engleman HM (2005) Clinical audit of subjects with snoring & sleep apnoea/hypopnoea syndrome fitted with mandibular repositioning splint. Respir Med 99:337–346
Mehta A, Qian J, Petocz P, Darendeliler MA, Cistulli PA (2001) A randomized, controlled study of a mandibular advancement splint for obstructive sleep apnea. Am J Respir Crit Care Med 163:1457–1461
Barnes M, McEvoy RD, Banks S, Tarquinio N, Murray CG, Vowles N, Pierce RJ (2004) Efficacy of positive airway pressure and oral appliance in mild to moderate obstructive sleep apnea. Am J Respir Crit Care Med 170:656–664
Pancer J, Al-Faifi S, Al-Faifi M, Hoffstein V (1999) Evaluation of variable mandibular advancement appliance for treatment of snoring and sleep apnea. Chest 116:1511–1518
Tegelberg A, Walker-Engstrom ML, Vestling O, Wilhelmsson B (2003) Two different degrees of mandibular advancement with a dental appliance in treatment of patients with mild to moderate obstructive sleep apnea. Acta Odontol Scand 61:356–362
Gotsopoulos H, Kelly JJ, Cistulli PA (2004) Oral appliance therapy reduces blood pressure in obstructive sleep apnea: a randomized, controlled trial. Sleep 27:934–941
Otsuka R, Ribeiro de Almeida F, Lowe AA, Linden W, Ryan F (2006) The effect of oral appliance therapy on blood pressure in patients with obstructive sleep apnea. Sleep Breath 10:29–36
Yoshida K, Sakamoto K, Takagi A, Iizuka T (2003) Three-piece oral appliance with herbst attachments for persistent vegetative state patient with sleep-disordered breathing. Int J Prosthodont 16:350–354
de Almeida FR, Lowe AA, Tsuiki S, Otsuka R, Wong M, Fastlicht S, Ryan F (2005) Long-term compliance and side effects of oral appliances used for the treatment of snoring and obstructive sleep apnea syndrome. J Clin Sleep Med 1:143–152
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tsuda, H., Almeida, F.R., Masumi, Si. et al. Side effects of boil and bite type oral appliance therapy in sleep apnea patients. Sleep Breath 14, 227–232 (2010). https://doi.org/10.1007/s11325-009-0304-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-009-0304-0