Abstract
Purpose
The purpose of this study was to investigate apnea–hypopnea index (AHI) across two polysomnographies (PSGs) to examine AHI variability and impact on clinical diagnosis.
Materials and methods
Two-night PSGs of 193 sleep clinic patients were reviewed, and the AHI variability was analyzed. Anonymized records from five patients with significant night-to-night AHI variability were used in this study: the two-night PSGs from two patients were represented as four individual PSGs; the two-night PSG for two others were represented as being obtained from two different sleep clinics; the last patient’s PSG was shown as a two-night study. Twenty-two sleep experts attending the Associated Professional Sleep Societies meeting were recruited to make diagnoses based on the PSGs. They were told that the PSGs were from seven patients: four with single-night PSG; two with two PSGs, each one from a different clinic; and one patient with a two-night PSG.
Results
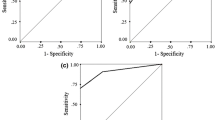
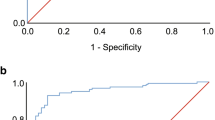
Twenty-one percent of the 193 sleep clinic patients had a nightly PSG AHI variability of greater than 5. Forty-eight percent of all patients had a significantly higher AHI on the first night, and 41% had a significantly higher AHI on the second night. Using an AHI > 15 diagnostic criteria, sleep apnea would have been undetected in 20% (n = 39) of patients due to low AHI on one night. Furthermore, 13% of all patients had a more severe sleep apnea classification based on the second night of PSG. For the seven cases, 27–36% of sleep experts failed to identify sleep apnea especially when presented with the PSG containing the lower AHI. Incidences of missed sleep apnea diagnoses were reduced to 15–18% when information from two PSGs was presented to the sleep experts.
Conclusions
Utilizing a large patient population, this study supports the significant night-to-night variability in PSG respiratory variables. Identification of sleep apnea in some patients is reduced when sleep experts are provided with only one PSG recording. The clinical implication is that about 13% of sleep clinic patients might benefit from a second night of PSG.


Similar content being viewed by others
References
Young T, Evans L, Finn L et al (1997) Estimation of the clinically diagnosed proportion of sleep apnea syndrome in middle-aged men and women. Sleep 20:705–706
Schafer H, Koehler U, Ewig S et al (1999) Obstructive sleep apnea as a risk marker in coronary artery disease. Cardiology 92:79–84. doi:10.1159/000006952
Hung J, Whitford EG, Parsons RW et al (1990) Association of sleep apnoea with myocardial infarction in men. Lancet 336:261–264. doi:10.1016/0140-6736(90)91799-G
Bixler EO, Vgontzas AN, Lin HM et al (2000) Association of hypertension and sleep-disordered breathing. Arch Intern Med 160:2289–2295. doi:10.1001/archinte.160.15.2289
Dyken ME, Somers VK, Yamada T et al (1996) Investigating the relationship between stroke and obstructive sleep apnea. Stroke 27:401–407
Nieto FJ, Young TB, Lind BK et al (2000) Association of sleep-disordered breathing, sleep apnea, and hypertension in a large community-based study. Sleep Heart Health Study. JAMA 283:1829–1836. doi:10.1001/jama.283.14.1829
Teran-Santos J, Jimenez-Gomez A, Cordero-Guevara J (1999) The association between sleep apnea and the risk of traffic accidents. Cooperative Group Burgos-Santander. N Engl J Med 340:847–851. doi:10.1056/NEJM199903183401104
Polysomnography Task Force, American Sleep Disorders Association Standards of Practice Committee (1997) Practice parameters for the indications for polysomnography and related procedures. Sleep 20:406–422
Riley RW, Powell NB, Guilleminault C et al (1995) Obstructive sleep apnea. Trends in therapy. West J Med 162:143–148
Le Bon O, Hoffmann G, Tecco J et al (2000) Mild to moderate sleep respiratory events: one negative night may not be enough. Chest 118:353–359. doi:10.1378/chest.118.2.353
Lord S, Sawyer B, O’Connell D et al (1991) Night-to-night variability of disturbed breathing during sleep in an elderly community sample. Sleep 14:252–258
Meyer TJ, Eveloff SE, Kline LR et al (1993) One negative polysomnogram does not exclude obstructive sleep apnea. Chest 103:756–760. doi:10.1378/chest.103.3.756
Mosko SS, Dickel MJ, Ashurst J (1988) Night-to-night variability in sleep apnea and sleep-related periodic leg movements in the elderly. Sleep 11:340–348
Stepnowsky CJ Jr, Orr WC, Davidson TM (2004) Nightly variability of sleep-disordered breathing measured over 3 nights. Otolaryngol Head Neck Surg 131:837–843. doi:10.1016/j.otohns.2004.07.011
Chediak AD, cevedo-Crespo JC, Seiden DJ et al (1996) Nightly variability in the indices of sleep-disordered breathing in men being evaluated for impotence with consecutive night polysomnograms. Sleep 19:589–592
Fietze I, Dingli K, Diefenbach K et al (2004) Night-to-night variation of the oxygen desaturation index in sleep apnoea syndrome. Eur Respir J 24:987–993. doi:10.1183/09031936.04.00100203
Rechtschaffen A, Kales A (1968) A manual of standardized terminology, techniques and scoring system for sleep stages of human subjects. UCLA, Los Angeles: BIS/BRI
Sleep-related breathing disorders in adults: recommendations for syndrome definition and measurement techniques in clinical research. The Report of an American Academy of Sleep Medicine Task Force. Sleep 22:667–689
Riedel BW, Winfield CF, Lichstein KL (2001) First night effect and reverse first night effect in older adults with primary insomnia: does anxiety play a role. Sleep Med 2:125–133. doi:10.1016/S1389-9457(00)00054-X
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure statement: This study did not receive external funding.
Rights and permissions
About this article
Cite this article
Ahmadi, N., Shapiro, G.K., Chung, S.A. et al. Clinical diagnosis of sleep apnea based on single night of polysomnography vs. two nights of polysomnography. Sleep Breath 13, 221–226 (2009). https://doi.org/10.1007/s11325-008-0234-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-008-0234-2