Abstract
Introduction
Gestational hypertension (GH) is defined as the presence of systolic blood pressure (BP) ≥ 140 mm Hg and/or diastolic BP ≥ 90 mm Hg, measured at least 4 h apart after 20 weeks of gestation. Early identification of women at high-risk of developing GH could contribute significantly towards improved maternal and fetal outcomes.
Objectives
To determine early metabolic biomarkers in women with GH as compared with normotensive women.
Methods
Serum samples were collected from subjects during three stages of their pregnancy: 8–12 weeks, 18–20 weeks and after 28 weeks (< 36 weeks) of gestation and studied using nuclear magnetic resonance (NMR) metabolomics approach. Multivariate and univariate analyses were performed to determine the significantly altered metabolites in GH women.
Results
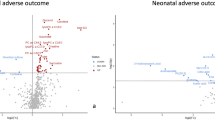
A total of 10 metabolites, including isoleucine, glutamine, lysine, proline, histidine, phenylalanine, alanine, carnitine, N-acetyl glycoprotein and lactic acid were observed to be significantly downregulated during all pregnancy stages in women with GH as compared with controls. Furthermore, expression of 5 metabolites in the first trimester i.e., phenylalanine [area under the curve (AUC) = 0.745], histidine [AUC = 0.729], proline [AUC = 0.722], lactic acid [AUC = 0.722], and carnitine [AUC = 0.714] exhibited highest potential in discriminating GH from normotensive women.
Conclusion
The present study is the first of its kind to identify significantly altered metabolites that have the potential to discriminate between women at risk of developing GH and normotensive women across three trimesters of pregnancy. This opens up the possibility of exploring these metabolites as potential early predictive markers of GH.





Similar content being viewed by others
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
- HDP:
-
Hypertensive disorders of pregnancy
- GH:
-
Gestational hypertension
- PIH:
-
Pregnancy-induced hypertension
- ACOG:
-
American College of Obstetricians and Gynecologists
- BP:
-
Blood pressure
- NMR:
-
Nuclear magnetic resonance
- MS:
-
Mass spectrometry
- BMI:
-
Body mass index
- PCA:
-
Principal component analysis
- PLS-DA:
-
Partial least squares discriminant analysis
- OPLS-DA:
-
Orthogonal partial least squares discriminant analysis
- HMDB:
-
Human metabolome database
- MetPA:
-
Metabolomics pathway analysis
- MSEA:
-
Metabolite set enrichment analysis
- VIP:
-
Variable-importance in projection
- ROC:
-
Receiver operating characteristic
- AUC:
-
Area under the curve
References
Ameta, K., Gupta, A., Kumar, S., Sethi, R., Kumar, D., & Mahdi, A. A. (2017). Essential hypertension: A filtered serum based metabolomics study. Scientific Reports, 7(1), 2153. https://doi.org/10.1038/s41598-017-02289-9
Austdal, M., Tangerås, L. H., Skråstad, R. B., Salvesen, K., Austgulen, R., Iversen, A. C., & Bathen, T. F. (2015). First trimester urine and serum metabolomics for prediction of preeclampsia and gestational hypertension: A prospective screening study. International Journal of Molecular Sciences, 16(9), 21520–21538. https://doi.org/10.3390/ijms160921520
Bahado-Singh, R. O., Syngelaki, A., Mandal, R., Graham, S. F., Akolekar, R., Han, B., Bjondahl, T. C., Dong, E., Bauer, S., Alpay-Savasan, Z., Turkoglu, O., Ogunyemi, D., Poon, L. C., Wishart, D. S., & Nicolaides, K. H. (2017). Metabolomic determination of pathogenesis of late-onset preeclampsia. The Journal of Maternal-Fetal & Neonatal Medicine, 30(6), 658–664. https://doi.org/10.1080/14767058.2016.1185411
Broekhuizen, M., Klein, T., Hitzerd, E., de Rijke, Y. B., Schoenmakers, S., Sedlmayr, P., Danser, A. H. J., Merkus, D., & Reiss, I. K. M. (2020). L-tryptophan–induced vasodilation is enhanced in preeclampsia: Studies on its uptake and metabolism in the human placenta. Hypertension, 76(1), 184–194.
Choudhury, P., Bhattacharya, A., Dasgupta, S., Ghosh, N., Senpupta, S., Joshi, M., Bhattacharyya, P., & Chaudhury, K. (2021). Identification of novel metabolic signatures potentially involved in the pathogenesis of COPD associated pulmonary hypertension. Metabolomics, 17(10), 94. https://doi.org/10.1007/s11306-021-01845-9
Cloarec, O., Dumas, M. E., Trygg, J., Craig, A., Barton, R. H., Lindon, J. C., Nicholson, J. K., & Holmes, E. (2005). Evaluation of the orthogonal projection on latent structure model limitations caused by chemical shift variability and improved visualization of biomarker changes in 1H NMR spectroscopic metabonomic studies. Analytical Chemistry, 77(2), 517–526. https://doi.org/10.1021/ac048803i
Dasgupta, S., Ghosh, N., Choudhury, P., Joshi, M., Chowdhury, S. R., Bhattacharyya, P., & Chaudhury, K. (2022). NMR metabolomic and microarray-based transcriptomic data integration identifies unique molecular signatures of hypersensitivity pneumonitis. Molecular Omics, 18(2), 101–111. https://doi.org/10.1039/d1mo00209k
Dasgupta, S., Das, S. S., Patidar, S., Kajaria, V., Chowdhury, S. R., & Chaudhury, K. (2023a). Identification of common dysregulated genes in COVID-19 and hypersensitivity pneumonitis: A systems biology and machine learning approach. Omics: A Journal of Integrative Biology. https://doi.org/10.1089/omi.2022.0171
Dasgupta, S., Ghosh, N., Bhattacharyya, P., Roy Chowdhury, S., & Chaudhury, K. (2023b). Metabolomics of asthma, COPD, and asthma-COPD overlap: An overview. Critical Reviews in Clinical Laboratory Sciences, 60(2), 153–170. https://doi.org/10.1080/10408363.2022.2140329
Durante, W. (2019). The emerging role of L-glutamine in cardiovascular health and disease. Nutrients, 11(9). https://doi.org/10.3390/nu11092092
Dutta, M., Singh, B., Joshi, M., Das, D., Subramani, E., Maan, M., Jana, S. K., Sharma, U., Das, S., Dasgupta, S., Ray, C. D., Chakravarty, B., & Chaudhury, K. (2018). Metabolomics reveals perturbations in endometrium and serum of minimal and mild endometriosis. Scientific Reports, 8(1), 6466. https://doi.org/10.1038/s41598-018-23954-7
Emwas, A.-H. M. (2015). The strengths and weaknesses of NMR spectroscopy and mass spectrometry with particular focus on metabolomics research. Methods in Molecular Biology (Clifton, N.J.), 1277, 161–193. https://doi.org/10.1007/978-1-4939-2377-9_13
Ennis, M. A., Rasmussen, B. F., Lim, K., Ball, R. O., Pencharz, P. B., Courtney-Martin, G., & Elango, R. (2020). Dietary phenylalanine requirements during early and late gestation in healthy pregnant women. The American Journal of Clinical Nutrition, 111(2), 351–359. https://doi.org/10.1093/ajcn/nqz288
Fardin, P., Manzari, M. B., Petretto, A., Ricciardi, A., & Varesio, L. (2007). Tryptophan metabolism and non-hypoxic induction of hypoxia-inducible factor (HIF). International Congress Series, 1304, 241–249.
Ferranti, E. P., Frediani, J. K., Mitchell, R., Fernandes, J., Li, S., Jones, D. P., Corwin, E., & Dunlop, A. L. (2020). Early pregnancy serum metabolite profiles associated with hypertensive disorders of pregnancy in African American women: A pilot study. Journal of Pregnancy, 2020, 1515321. https://doi.org/10.1155/2020/1515321
Gestational Hypertension and Preeclampsia: ACOG Practice Bulletin, Number 222. (2020). Obstetrics and Gynecology, 135(6), e237–e260. https://doi.org/10.1097/AOG.0000000000003891
Glew, R. H., Melah, G., El-Nafaty, A. I., Brandt, Y., Morris, D., & VanderJagt, D. J. (2004). Plasma and urinary free amino acid concentrations in preeclamptic women in northern Nigeria. Clinica Chimica Acta; International Journal of Clinical Chemistry, 342(1–2), 179–185. https://doi.org/10.1016/j.cccn.2003.12.028
Harville, E. W., Li, Y.-Y., Pan, K., McRitchie, S., Pathmasiri, W., & Sumner, S. (2021). Untargeted analysis of first trimester serum to reveal biomarkers of pregnancy complications: A case–control discovery phase study. Scientific Reports, 11(1), 3468. https://doi.org/10.1038/s41598-021-82804-1
Honda, M., Omori, Y., Minei, S., Oshiyama, T., Shimizu, M., Sanaka, M., Kohama, T., Nakabayashi, M., & Hirata, Y. (1990). Quantitative analysis of serum α1-acid glycoprotein levels in normal and diabetic pregnancy. Diabetes Research and Clinical Practice, 10(2), 147–152. https://doi.org/10.1016/0168-8227(90)90037-T
Hsu, C.-N., & Tain, Y.-L. (2020). Amino acids and developmental origins of hypertension. Nutrients, 12(6), 1763. https://doi.org/10.3390/nu12061763
Hypertension in pregnancy. Report of the American College of Obstetricians and Gynecologists’ Task Force on Hypertension in Pregnancy. (2013). Obstetrics and Gynecology, 122(5), 1122–1131. https://doi.org/10.1097/01.AOG.0000437382.03963.88
Karna, E., Szoka, L., Huynh, T. Y. L., & Palka, J. A. (2020). Proline-dependent regulation of collagen metabolism. Cellular and Molecular Life Sciences: CMLS, 77(10), 1911–1918. https://doi.org/10.1007/s00018-019-03363-3
Kenny, L. C., Broadhurst, D. I., Dunn, W., Brown, M., North, R. A., McCowan, L., Roberts, C., Cooper, G. J. S., Kell, D. B., & Baker, P. N. (2010). Robust early pregnancy prediction of later preeclampsia using metabolomic biomarkers. Hypertension (Dallas, Tex.: 1979), 56(4), 741–749. https://doi.org/10.1161/HYPERTENSIONAHA.110.157297
Koo, W. W., Krug Wispe, S. K., Succop, P., Champlin, A., Sherman, R., & Berry, H. (1990). Urinary hydroxyproline in infants with and without fractures/rickets. Clinical Chemistry, 36(4), 642–644.
Lee, S. M., Park, J. S., Han, Y. J., Kim, W., Bang, S. H., Kim, B. J., Park, C. W., & Kim, M. Y. (2020). Elevated alanine aminotransferase in early pregnancy and subsequent development of gestational diabetes and preeclampsia. Journal of Korean Medical Science, 35(26), e198. https://doi.org/10.3346/jkms.2020.35.e198
Lourenço, A. B., Roque, F. C., Teixeira, M. C., Ascenso, J. R., & Sá-Correia, I. (2013). Quantitative 1H-NMR-metabolomics reveals extensive metabolic reprogramming and the effect of the aquaglyceroporin FPS1 in ethanol-stressed yeast cells. PloS One, 8(2), e55439. https://doi.org/10.1371/journal.pone.0055439
Odibo, A. O., Goetzinger, K. R., Odibo, L., Cahill, A. G., Macones, G. A., Nelson, D. M., & Dietzen, D. J. (2011). First-trimester prediction of preeclampsia using metabolomic biomarkers: A discovery phase study. Prenatal Diagnosis, 31(10), 990–994. https://doi.org/10.1002/pd.2822
Pang, Z., Chong, J., Zhou, G., de Lima Morais, D. A., Chang, L., Barrette, M., Gauthier, C., Jacques, P.-É., Li, S., & Xia, J. (2021). MetaboAnalyst 5.0: Narrowing the gap between raw spectra and functional insights. Nucleic Acids Research, 49(W1), W388–W396. https://doi.org/10.1093/nar/gkab382
Payne, M., Stephens, T., Lim, K., Ball, R. O., Pencharz, P. B., & Elango, R. (2018). Lysine requirements of healthy pregnant women are higher during late stages of gestation compared to early gestation. The Journal of Nutrition, 148(1), 94–99. https://doi.org/10.1093/jn/nxx034
Pijnenborg, R., Dixon, G., Robertson, W. B., & Brosens, I. (1980). Trophoblastic invasion of human decidua from 8 to 18 weeks of pregnancy. Placenta, 1(1), 3–19. https://doi.org/10.1016/s0143-4004(80)80012-9
Raymond, R., & Millhorn, D. (1997). Regulation of tyrosine hydroxylase gene expression during hypoxia: Role of Ca2 + and PKC. Kidney International, 51(2), 536–541. https://doi.org/10.1038/ki.1997.74
Regitz-Zagrosek, V., Roos-Hesselink, J. W., Bauersachs, J., Blomström-Lundqvist, C., Cífková, R., De Bonis, M., Iung, B., Johnson, M. R., Kintscher, U., Kranke, P., Lang, I. M., Morais, J., Pieper, P. G., Presbitero, P., Price, S., Rosano, G. M. C., Seeland, U., Simoncini, T., Swan, L., & Warnes, C. A. (2018). 2018 ESC guidelines for the management of cardiovascular diseases during pregnancy. European Heart Journal, 39(34), 3165–3241. https://doi.org/10.1093/eurheartj/ehy340
Report of the National High Blood Pressure Education Program Working Group on High Blood Pressure in Pregnancy. (2000). American Journal of Obstetrics and Gynecology, 183(1), S1–S22.
Roberts JM, August PA, Bakris G, Barton JR, Bernstein IM, D. M. (2013). Hypertension in pregnancy. Obstetrics and Gynecology, 122(5), 1122–1131.
Subramani, E., Jothiramajayam, M., Dutta, M., Chakravorty, D., Joshi, M., Srivastava, S., Mukherjee, A., Datta Ray, C., Chakravarty, B. N., & Chaudhury, K. (2016). NMR-based metabonomics for understanding the influence of dormant female genital tuberculosis on metabolism of the human endometrium. Human Reproduction, 31(4), 854–865. https://doi.org/10.1093/humrep/dew003
Tan, R., Li, J., Liu, F., Liao, P., Ruiz, M., Dupuis, J., Zhu, L., & Hu, Q. (2020). Phenylalanine induces pulmonary hypertension through calcium-sensing receptor activation. American Journal of Physiology-Lung Cellular and Molecular Physiology, 319(6), L1010–L1020.
Thiele, I. G. I., Niezen-Koning, K. E., van Gennip, A. H., & Aarnoudse, J. G. (2004). Increased plasma carnitine concentrations in preeclampsia. Obstetrics and Gynecology, 103(5 Pt 1), 876–880. https://doi.org/10.1097/01.AOG.0000125699.60416.03
Trygg, J., & Wold, S. (2002). Orthogonal projections to latent structures (O-PLS). Journal of Chemometrics, 16, 119–128. https://doi.org/10.1002/cem.695
Veerbeek, J. H. W., Hermes, W., Breimer, A. Y., van Rijn, B. B., Koenen, S. V, Mol, B. W., Franx, A., de Groot, C. J. M., & Koster, M. P. H. (2015). Cardiovascular disease risk factors after early-onset preeclampsia, late-onset preeclampsia, and pregnancy-induced hypertension. Hypertension, 65(3), 600–606. https://doi.org/10.1161/HYPERTENSIONAHA.114.04850
Vuvor, F., Mohammed, H., Ndanu, T., & Harrison, O. (2017). Effect of lysine supplementation on hypertensive men and women in selected peri-urban community in Ghana. BMC Nutrition, 3(1), 67. https://doi.org/10.1186/s40795-017-0187-6
Wang, Z., Cheng, C., Yang, X., & Zhang, C. (2021). L-phenylalanine attenuates high salt-induced hypertension in Dahl SS rats through activation of GCH1-BH4. PloS One, 16(4), e0250126. https://doi.org/10.1371/journal.pone.0250126
Wishart, D. S., Feunang, Y. D., Marcu, A., Guo, A. C., Liang, K., Vázquez-Fresno, R., Sajed, T., Johnson, D., Li, C., Karu, N., Sayeeda, Z., Lo, E., Assempour, N., Berjanskii, M., Singhal, S., Arndt, D., Liang, Y., Badran, H., Grant, J., Serra-Cayuela, A., Liu, Y., Mandal, R., Neveu, V., Pon, A., Knox, C., Wilson, M., Manach, C., Scalbert, A. (2018). HMDB 4.0: The human metabolome database for 2018. Nucleic Acids Research, 46(D1), D608–D617. https://doi.org/10.1093/nar/gkx1089
Ying, W., Catov, J. M., & Ouyang, P. (2018). Hypertensive disorders of pregnancy and future maternal cardiovascular risk. Journal of the American Heart Association, 7(17), e009382. https://doi.org/10.1161/JAHA.118.009382
Zhang, A., Sun, H., Yan, G., Wang, P., & Wang, X. (2015). Metabolomics for biomarker discovery: Moving to the clinic. BioMed Research International, 2015, 354671. https://doi.org/10.1155/2015/354671
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
The study was designed by SD, ES, PC, CD and KC. Experimentation and data analysis were performed by SD, ES, IM, AB, DS and MJ. The draft of the manuscript was written by SD and AB and reviewed by PC, CD and KC. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed were in accordance with the ethical standards of the institutional research committee and with the principles of the 1964 Declaration of Helsinki and its later amendments. Informed consent was obtained from all individual participants included in the study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dasgupta, S., Subramani, E., Mitra, I. et al. Discovery of novel metabolic signatures for early identification of women at risk of developing gestational hypertension. Metabolomics 19, 50 (2023). https://doi.org/10.1007/s11306-023-02012-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11306-023-02012-y