Abstract
Background
Respiratory syncytial virus (RSV) infection in infants causes significant morbidity and is the strongest risk factor associated with asthma. Metabolites, which reflect the interactions between host cell and virus, provide an opportunity to identify the pathways that underlie severe infections and asthma development.
Objective
To study metabolic profile differences between infants with RSV infection, and human rhinovirus (HRV) infection, and healthy infants. To compare infant metabolic differences between children who do and do not wheeze.
Methods
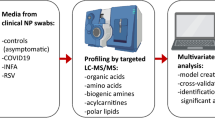
In a term birth cohort, urine was collected while healthy and during acute viral respiratory infection with RSV and HRV. We used 1H-NMR to identify urinary metabolites. Multivariate and univariate statistics were used to discriminate metabolic profiles of infants with either RSV ARI, or HRV ARI, and healthy infants. Multivariable logistic regression was used to assess the association of urine metabolites with 1st-, 2nd-, and 3rd-year recurrent wheezing.
Results
Several metabolites in nicotinate and nicotinamide metabolism pathways were down-regulated in infants with RSV infection compared to healthy controls. There were no significant differences in metabolite profiles between infants with RSV infection and infants with HRV Infection. Alanine was strongly associated with reduced risk of 1st-year wheezing (OR 0.18[0.0, 0.46]) and 2nd-year wheezing (OR 0.31[0.13, 0.73]), while 2-hydroxyisobutyric acid was associated with increased 3rd-year wheezing (OR 5.02[1.49, 16.93]) only among the RSV infected subset.
Conclusion
The metabolites associated with infant RSV infection and recurrent-wheezing are indicative of viral takeover of the cellular machinery and resources to enhance virulence, replication, and subversion of the host immune-response, highlighting metabolic pathways important in the pathogenesis of RSV infection and wheeze development.




Similar content being viewed by others
References
Adamko, D. J., Saude, E., Bear, M., Regush, S., & Robinson, J. L. (2016). Urine metabolomic profiling of children with respiratory tract infections in the emergency department: A pilot study. BMC Infectious Diseases, 16, 439. https://doi.org/10.1186/s12879-016-1709-6.
Bacharier, L. B., et al. (2012). Determinants of asthma after severe respiratory syncytial virus bronchiolitis. The Journal of Allergy and Clinical Immunology, 130, 91–100. https://doi.org/10.1016/j.jaci.2012.02.010.
Barker, M., & Rayens, W. (2003). Partial least squares for discrimination. Journal of Chemometrics, 17, 166–173. https://doi.org/10.1002/cem.785.
Beigelman, A., & Bacharier, L. B. (2013). The role of early life viral bronchiolitis in the inception of asthma. Current Opinion in Allergy and Clinical Immunology, 13, 211–216. https://doi.org/10.1097/ACI.0b013e32835eb6ef.
Benson, J. M., Barr, E. B., & Krone, J. R. (2001). MTBE inhaled alone and in combination with gasoline vapor: Uptake, distribution, metabolism, and excretion in rats. Research Report Health Effects Institute, 102, 73–94; (discussion 95–109).
Bernini, P., Bertini, I., Luchinat, C., Nincheri, P., Staderini, S., & Turano, P. (2011). Standard operating procedures for pre-analytical handling of blood and urine for metabolomic studies and biobanks. Journal of Biomolecular NMR, 49, 231–243. https://doi.org/10.1007/s10858-011-9489-1.
Bijlsma, S., et al. (2006). Large-scale human metabolomics studies: A strategy for data (pre-) processing and validation. Analytical Chemistry, 78, 567–574. https://doi.org/10.1021/ac051495j.
Boeke, C. E., et al. (2012). Gestational intake of methyl donors and global LINE-1 DNA methylation in maternal and cord blood Prospective results from a folate-replete population. Epigenetics, 7, 253–260. https://doi.org/10.4161/epi.7.3.19082.
Bylesjo, M., Rantalainen, M., Cloarec, O., Nicholson, J. K., Holmes, E., & Trygg, J. (2006). OPLS discriminant analysis: Combining the strengths of PLS-DA and SIMCA classification. Journal of Chemometrics, 20, 341–351. https://doi.org/10.1002/cem.1006.
Delgado, T., Sanchez, E. L., Camarda, R., & Lagunoff, M. (2012). Global metabolic profiling of infection by an oncogenic virus: KSHV induces and requires lipogenesis for survival of latent infection. PLOS Pathogens, 8, e1002866. https://doi.org/10.1371/journal.ppat.1002866.
Denkert, C., Warskulat, U., Hensel, F., & Haussinger, D. (1998). Osmolyte strategy in human monocytes and macrophages: Involvement of p38(MAPK) in hyperosmotic induction of betaine and myoinositol transporters. Archives of Biochemistry and Biophysics, 354, 172–180. https://doi.org/10.1006/abbi.1998.0661.
Dominguez-Salas, P., et al. (2014). Maternal nutrition at conception modulates DNA methylation of human metastable epialleles. Nature Communications. https://doi.org/10.1038/ncomms4746.
Gebicki, J., Sysa-Jedrzejowska, A., Adamus, J., Wozniacka, A., Rybak, M., & Zielonka, J. (2003). 1-methylnicotinamide: A potent anti-inflammatory agent of vitamin origin. Polish Journal of Pharmacology, 55, 109–112.
Golland, P., Grimson, W. E., Shenton, M. E., & Kikinis, R. (2005). Detection and analysis of statistical differences in anatomical shape. Medical Image Analysis, 9, 69–86. https://doi.org/10.1016/j.media.2004.07.003.
Gong, H. J. (1990). Wheezing and Asthma. In: H. K. Walker, W. D. Hall, J. W. Hurst (eds) Clinical methods: The history, physical, and laboratory examinations. Boston: Butterworths.
Haggarty, P., Hoad, G., Campbell, D. M., Horgan, G. W., Piyathilake, C., & McNeill, G. (2013). Folate in pregnancy and imprinted gene and repeat element methylation in the offspring. American Journal of Clinical Nutrition, 97, 94–99. https://doi.org/10.3945/ajcn.112.042572.
Hastie, T., Tibshirani, R., Sherlock, G., Eisen, M., Brown, P., & Botstein, D. (1999). Imputing missing data for gene expression arrays. Stanford: Stanford University Statistics Department Technical Report.
Hurwitz, J. L. (2011). Respiratory syncytial virus vaccine development. Expert Review of Vaccines, 10, 1415–1433. https://doi.org/10.1586/erv.11.120.
Infantino, V., Iacobazzi, V., Menga, A., Avantaggiati, M. L., & Palmieri, F. (2014). A key role of the mitochondrial citrate carrier (SLC25A1) in TNF alpha- and IFN gamma-triggered inflammation. Biochimica Et Biophysica Acta-Gene Regulatory Mechanisms, 1839, 1217–1225. https://doi.org/10.1016/j.bbagrm.2014.07.013.
Infantino, V., Iacobazzi, V., Palmieri, F., & Menga, A. (2013). ATP-citrate lyase is essential for macrophage inflammatory response. Biochemical and Biophysical Research Communications, 440, 105–111. https://doi.org/10.1016/j.bbrc.2013.09.037.
Jartti, T., et al. (2009). Systemic T-helper and T-regulatory cell type cytokine responses in rhinovirus vs. respiratory syncytial virus induced early wheezing: An observational study. Respiratory Research, 10, 85. https://doi.org/10.1186/1465-9921-10-85.
Kalapos, M. P. (1999). Possible physiological roles of acetone metabolism in humans. Medical Hypotheses, 53, 236–242. https://doi.org/10.1054/mehy.1998.0752.
Karnovsky, A., et al. (2012). Metscape 2 bioinformatics tool for the analysis and visualization of metabolomics and gene expression data. Bioinformatics, 28, 373–380. https://doi.org/10.1093/bioinformatics/btr661.
Kassel, D. B., Martin, M., Schall, W., & Sweeley, C. C. (1986). Urinary metabolites of l-threonine in type 1 diabetes determined by combined gas chromatography/chemical ionization mass spectrometry. Biomedical & Environmental Mass Spectrometry, 13, 535–540.
Lampropoulou, V., et al. (2016). Itaconate links inhibition of succinate dehydrogenase with macrophage metabolic remodeling and regulation of inflammation. Cell Metabolism, 24, 158–166. https://doi.org/10.1016/j.cmet.2016.06.004.
Larkin, E. K., et al. (2015). Objectives, design and enrollment results from the infant susceptibility to pulmonary infections and asthma following RSV Exposure Study (INSPIRE). BMC Pulmonary Medicine, 15, 45. https://doi.org/10.1186/s12890-015-0040-0.
Larkin, E. K., & Hartert, T. V. (2015). Genes associated with RSV lower respiratory tract infection and asthma: The application of genetic epidemiological methods to understand causality. Future Virology, 10, 883–897. https://doi.org/10.2217/fvl.15.55.
Mestas, J., & Hughes, C. C. (2004). Of mice and not men: Differences between mouse and human immunology. Journal of Immunology, 172, 2731–2738.
Milner, J. J., Wang, J., Sheridan, P. A., Ebbels, T., Beck, M. A., & Saric, J. (2014). 1H NMR-based profiling reveals differential immune-metabolic networks during influenza virus infection in obese mice. PLoS ONE, 9, e97238. https://doi.org/10.1371/journal.pone.0097238.
Munger, J., Bajad, S. U., Coller, H. A., Shenk, T., & Rabinowitz, J. D. (2006). Dynamics of the cellular metabolome during human cytomegalovirus infection. PLoS Pathogens, 2, e132. https://doi.org/10.1371/journal.ppat.0020132.
Musfeld, C., Biollaz, J., Belaz, N., Kesselring, U. W., & Decosterd, L. A. (2001). Validation of an HPLC method for the determination of urinary and plasma levels of N-1-methylnicotinamide, an endogenous marker of renal cationic transport and plasma flow. Journal of Pharmaceutical and Biomedical Analysis, 24, 391–404. https://doi.org/10.1016/S0731-7085(00)00425-8.
Nair, H., et al. (2010). Global burden of acute lower respiratory infections due to respiratory syncytial virus in young children: A systematic review and meta-analysis. The Lancet, 375, 1545–1555. https://doi.org/10.1016/S0140-6736(10)60206-1.
Openshaw, P. J. (2013). A gene expression signature for RSV: Clinical implications and limitations. PLoS Medicine, 10, e1001550. https://doi.org/10.1371/journal.pmed.1001550.
Papin, J. F., et al. (2013). Infant baboons infected with respiratory syncytial virus develop clinical and pathological changes that parallel those of human infants. American Journal of Physiology-Lung Cellular and Molecular Physiology, 304, L530–L539. https://doi.org/10.1152/ajplung.00173.2012.
Pearce, E. L., & Pearce, E. J. (2013). Metabolic pathways in immune cell activation and quiescence. Immunity, 38, 633–643. https://doi.org/10.1016/j.immuni.2013.04.005.
Peeples, M., & Levine, S. (1980). Metabolic requirements for the maturation of respiratory syncytial virus. Journal of General Virology, 50, 81–88. https://doi.org/10.1099/0022-1317-50-1-81.
Ritter, J. B., Wahl, A. S., Freund, S., Genzel, Y., & Reichl, U. (2010). Metabolic effects of influenza virus infection in cultured animal cells: Intra- and extracellular metabolite profiling. BMC Systems Biology, 4, 61. https://doi.org/10.1186/1752-0509-4-61.
Rosas-Salazar, C., et al. (2015). Urine club cell 16-kDa secretory protein and childhood wheezing illnesses after lower respiratory tract infections in infancy. Pediatric Allergy, Immunology, and Pulmonology, 28, 158–164. https://doi.org/10.1089/ped.2015.0528.
Sanchez, E. L., & Lagunoff, M. (2015). Viral activation of cellular metabolism. Virology, 479–480, 609–618. https://doi.org/10.1016/j.virol.2015.02.038.
Shi, T., et al. (2017). Global, regional, and national disease burden estimates of acute lower respiratory infections due to respiratory syncytial virus in young children in 2015: A systematic review and modelling study. The Lancet, 390, 946–958. https://doi.org/10.1016/S0140-6736(17)30938-8.
Sigurs, N., et al. (2010). Asthma and allergy patterns over 18 years after severe RSV bronchiolitis in the first year of life. Thorax, 65, 1045–1052. https://doi.org/10.1136/thx.2009.121582.
Simoes, E. A., et al. (2015). Challenges and opportunities in developing respiratory syncytial virus therapeutics. The Journal of Infectious Diseases, 211(Suppl 1), S1–S20. https://doi.org/10.1093/infdis/jiu828.
Stacklies, W., Redestig, H., Scholz, M., Walther, D., & Selbig, J. (2007). pcaMethods–a bioconductor package providing PCA methods for incomplete data. Bioinformatics, 23, 1164–1167. https://doi.org/10.1093/bioinformatics/btm069.
Stein, R. T., et al. (1999). Respiratory syncytial virus in early life and risk of wheeze and allergy by age 13 years. The Lancet, 354, 541–545. https://doi.org/10.1016/S0140-6736(98)10321-5.
Trygg, J., & Wold, S. (2002). Orthogonal projections to latent structures (O-PLS). Journal of Chemometrics, 16, 119–128. https://doi.org/10.1002/cem.695.
Ulrich, E. L., et al. (2008). BioMagResBank. Nucleic Acids Research, 36, D402–D408. https://doi.org/10.1093/nar/gkm957.
van den Berg, R. A., Hoefsloot, H. C. J., Westerhuis, J. A., Smilde, A. K., & van der Werf, M. J. (2006). Centering, scaling, and transformations: Improving the biological information content of metabolomics data. Bmc Genomics. https://doi.org/10.1186/1471-2164-7-142.
Vasudevamurthy, M. K., Lever, M., George, P. M., & Morison, K. R. (2009). Betaine structure and the presence of hydroxyl groups alters the effects on DNA melting temperatures. Biopolymers, 91, 85–94. https://doi.org/10.1002/bip.21085.
Veeranki, S. P., et al. (2014). Association of folic acid supplementation during pregnancy and infant bronchiolitis. American Journal of Epidemiology, 179, 938–946. https://doi.org/10.1093/aje/kwu019.
Wang, L., et al. (2013). Metabonomic profiling of serum and urine by (1)H NMR-based spectroscopy discriminates patients with chronic obstructive pulmonary disease and healthy individuals. PLoS ONE, 8, e65675. https://doi.org/10.1371/journal.pone.0065675.
Westerhuis, J. A., et al. (2008). Assessment of PLSDA cross validation. Metabolomics, 4, 81–89. https://doi.org/10.1007/s11306-007-0099-6.
Wettstein, M., Weik, C., Holneicher, C., & Haussinger, D. (1998). Betaine as an osmolyte in rat liver: Metabolism and cell-to-cell interactions. Hepatology, 27, 787–793. https://doi.org/10.1002/hep.510270321.
Wiklund, S., et al. (2008). Visualization of GC/TOF-MS-based metabolomics data for identification of biochemically interesting compounds using OPLS class models. Analytical Chemistry, 80, 115–122. https://doi.org/10.1021/ac0713510.
Wishart, D. S., et al. (2017). HMDB 4.0: The human metabolome database for 2018. Nucleic Acids Research. https://doi.org/10.1093/nar/gkx1089.
Wright, M., & Piedimonte, G. (2011). Respiratory syncytial virus prevention and therapy: Past, present, and future. Pediatric Pulmonology, 46, 324–347. https://doi.org/10.1002/ppul.21377.
Wu, P., et al. (2008). Evidence of a causal role of winter virus infection during infancy in early childhood asthma. American Journal of Respiratory and Critical Care Medicine, 178, 1123–1129. https://doi.org/10.1164/rccm.200804-579OC.
Xia, J., Sinelnikov, I. V., Han, B., & Wishart, D. S. (2015). MetaboAnalyst 3.0–making metabolomics more meaningful. Nucleic Acids Research, 43, W251–W257. https://doi.org/10.1093/nar/gkv380.
Xia, J., & Wishart, D. S. (2016). Using MetaboAnalyst 3.0 for comprehensive metabolomics data analysis. Current Protocols in Bioinformatics, 55, 14. https://doi.org/10.1002/cpbi.11.
Yu, Y., Clippinger, A. J., & Alwine, J. C. (2011). Viral effects on metabolism: Changes in glucose and glutamine utilization during human cytomegalovirus infection. Trends in Microbiology, 19, 360–367. https://doi.org/10.1016/j.tim.2011.04.002.
Zhang, B., et al. (2015). Both the folate cycle and betaine-homocysteine methyltransferase contribute methyl groups for DNA methylation in mouse blastocysts. The FASEB Journal, 29, 1069–1079. https://doi.org/10.1096/fj.14-261131.
Zhao, N. N., Yang, S., Hu, Y., Dong, H. B., & Zhao, R. Q. (2017). Maternal betaine supplementation in rats induces intergenerational changes in hepatic IGF-1 expression and DNA methylation. Molecular Nutrition & Food Research. https://doi.org/10.1002/mnfr.201600940.
Acknowledgements
We thank the NMR-Based Metabolomics Core at Cincinnati Children’s Hospital Medical Center for advising on study design and processing our samples.
Funding
This work was supported by the National Institute of Health U19AI95227, K24 AI 77930, R21HD087864, and T32HL087738. The funding agencies did not have any role in the study design, collection, analysis and interpretation of data, the writing of this report, or the decision to submit for publication. The funding was provided by National Institute of Allergy and Infectious Diseases.
Author information
Authors and Affiliations
Contributions
KNT, TVH, LA, and RSP designed the work; TVH collected the urine specimens; LR and MW performed the experiments; KNT, TG, SB and LR analyzed the NMR data; and KNT drafted the manuscript. KNT, TVH, LA, RSP TG, SB, EKL and LR edited the manuscript. All of the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Hartert has previously served as a consultant to Novavax and Regeneron. Dr. Kedir N Turi, Dr. Lindsey Romick-Rosendale, Tebeb Gebretsadik, Dr. Miki Watanabe, Dr. Steven Brunwasser, Dr. Larry J Anderson, Dr. Martin L Moore, Dr. Emma K Larkin, Dr. Ray Stokes Peebles and Dr. Tina V. Hartert have no conflicts of interest.
Ethical approval
This study was approved by the ethical committee of Vanderbilt University Medical Center, Nashville TN.
Informed consent
Informed written consent was obtained from the parent of each infant for study participation.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Turi, K.N., Romick-Rosendale, L., Gebretsadik, T. et al. Using urine metabolomics to understand the pathogenesis of infant respiratory syncytial virus (RSV) infection and its role in childhood wheezing. Metabolomics 14, 135 (2018). https://doi.org/10.1007/s11306-018-1431-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11306-018-1431-z