Abstract
Purpose
To assess the efficacy of hyaluronic acid (HA) application after urethral trauma for preventing spongiofibrosis and inflammation in the early period.
Methods
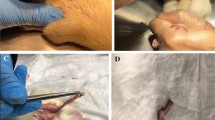
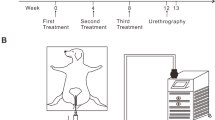
A total of twenty-four rats were divided into 3 groups, with 8 rats in each. The urethra was traumatized with a 24 G needle sheath in all rats. Group 1 of rats were applied 0.9% saline solution twice a day, Group 2 were applied 0.9% saline solution and sodium HA 1% once a day, Group 3 were applied 1.0% HA twice a day. After 21 days, penectomy was performed in all rats. Inflammation, spongiofibrosis, hyperemia and edema in the urethra were investigated for each group.
Results
Histopathologic analysis revealed less fibrosis in both group 2 and group 3 compared to Group 1 (p = 0.004). There were no statistically significant differences among the groups in terms of inflammation, hyperemia, edema and congestion (p = 0.563, p = 0.069, p = 0.069, p = 0.068, respectively).
Severe fibrosis was observed in 6 (75%) rats in Group 1, and in none of the rats of Group 2 or Group 3. With respect to spongiofibrosis compared to the control group, both Group 2 and Group 3 have statistically significant differences (p = 0.004).
Moderate spongiofibrosis was observed in 5 (62.5%) rats in Group 2 and in 3 (37.5%) rats in Group 3. Statistically, there were no significant differences in respect of severity between Group 2 and Group 3 (p = 0.014).
Conclusion
Intraurethral HA application after urethral trauma can decrease spongiofibrosis.


Similar content being viewed by others
References
Nathan MS, Krishnan V (2018) Endoscopic management of urethral stricture: review and practice algorithm for management of male urethral stricture disease. Curr Urol Rep 19(3):19. https://doi.org/10.1007/s11934-018-0771-6
Stein DM, Thum DJ, Barbagli G et al (2013) A geographic analysis of male urethral stricture aetiology and location. BJU Int 112(6):830–834. https://doi.org/10.1111/j.1464-410X.2012.11600.x
Chen C, Zeng M, Xue R et al (2018) Causes and management for male urethral stricture. Zhong Nan Da Xue Xue Bao Yi Xue Ban 43(5):520–527. https://doi.org/10.11817/j.issn.1672-7347.2018.05.010
Chaloupka M, Beck V, Kretschmer A, Tritschler S, Stief CG, Strittmatter F (2018) Diagnostic workup of urethral strictures. Urologe A 57(1):6–10. https://doi.org/10.1007/s00120-017-0547-5
Gozzi C, Tritschler S, Bastian PJ, Stief CG (2008) Management of urethral strictures. Urologe A 47(12):1615–1622. https://doi.org/10.1007/s00120-008-1903-2
Barbagli G, Lazzeri M (2006) Urethral reconstruction. Curr Opin Urol 16(6):391–395. https://doi.org/10.1097/01.mou.0000250277.44990.ab
Sahinkanat T, Ozkan KU, Ciralik H et al (2009) Botulinum toxin-A to improve urethral wound healing: an experimental study in a rat model. Urology 73(2):405–409. https://doi.org/10.1016/j.urology.2008.07.051
Natalia MS, Katarzyna AB, Dominika AZ, Dominika LW (2016) Physiochemical properties and application of hyaluronic acid: a systematic review. J Cosmet Dermatol 15(4):520–526. https://doi.org/10.1111/jocd.12237
Mineo JA, Suzuki R, Kuroyanagi Y, Biomater J (2013) Development of an artificial dermis composed of hyaluronic acid and collagen. Sci Polym Ed 24(6):726–740. https://doi.org/10.1080/09205063.2012.708190
Reitinger S, Lepperdinger G (2012) Hyaluronan, a ready choice to fuel regeneration: a mini-review. Gerontology 59(1):71–76. https://doi.org/10.1159/000342200
Prosdocimi M, Bevilacqua C (2012) Exogenous hyaluronic acid and wound healing: an updated vision. Panminerva Med 54(2):129–135
Paweł O, Komosińska-Vassev K, Winsz-Szczotka K, Kuźnik-Trocha K, Olczyk K (2008) Hyaluronan: structure, metabolism, functions, and role in wound healing. Postepy Hig Med Dosw (Online) 62:651–659
Palminteri E, Maruccia S, Berdondini E et al (2014) Male urethral strictures: a national survey among urologists in Italy. Urology 83:477–484. https://doi.org/10.1016/j.urology.2013.10.043
Hofer MD, Chneng EY, Burby MI, Park E, Xu V (2014) Analysis of primer urethral wound healing in the rat. Urology 84:246. https://doi.org/10.1016/j.urology.2014.04.012
Hebert PW (1972) The treatment of urethral stricture: transurethral injection of triamcinolone. J Urol 108:745–747. https://doi.org/10.1016/s0022-5347(17)60856-5
Shirazi M, Khezri A, Samani SM et al (2007) Effect of intraurethral captopril gel on the recurrence of urethralstricture after direct vision internal urethrotomy: phase II clinical trial. Int J Urol 14:203–208. https://doi.org/10.1111/j.1442-2042.2007.01693.x
Nagler A, Gofrit O, Ohana M et al (2000) The effect of halofuginone, an inhibitor of collagen type I synthesis, on urethral stricture formation: in vivo and in vitro study in a rat model. J Urol 164:1776–1780
Mazdak H, Meshki I, Ghassami F (2007) Effect of mitomycin C on anterior urethral stricture recurrence after internal urethrotomy. Eur Urol 51:1089–1092. https://doi.org/10.1016/j.eururo.2006.11.038
Yardimci I, Karakan T, Resorlu B et al (2015) The effect of intraurethral dexpanthenol on healing and fibrosis in rats with experimentally induced urethral trauma. Urology 85:274. https://doi.org/10.1016/j.urology.2014.09.038
Chung JH, Kang DH, Choi HY et al (2013) The effects of hyaluronic acid and carboxymethylcellulose in preventing recurrence of urethral stricture after endoscopic internal urethrotomy: a multicenter, randomized controlled, single-blinded study. J Endourol 27:756–762. https://doi.org/10.1089/end.2012.0613
Dundar M, Koçak I, Erkus M et al (2002) The effect of diltiazem on the healing of traumatic urethral inflamation. Urol Int 68:268–272. https://doi.org/10.1159/000058449
Ayyildiz A, Akgül KT, Cebeci O, Nuhoğlu B, Caydere M, Ustün H, Germiyanoğlu C (2007) Intraurethral honey application for urethral injury: an experimental study. Int Urol Nephrol 39(3):815–821. https://doi.org/10.1007/s11255-006-9152-z
Yıldızhan M, Dundar M, Demirci B, Çulhacı N (2020) The effects of hyaluronic acid on traumatic urethral inflammation. Urol İnt 104(3–4):283–286. https://doi.org/10.1159/000504766
Hortensius RA, Harley BA (2013) The use of bioinspired alterations in the glycosaminoglycan content of collagen-GAG scaffolds to regulate cell activity. Biomaterials 34(31):7645–7652. https://doi.org/10.1016/j.biomaterials.2013.06.056
Lv YS, Yao YS, Lin ME, Rong L, Deng BH, Huang J et al (2013) Interleukin-6 levels in female rats with protamine sulfate-induced chronic cystitis treated with hyaluronic acid. Int J Urol 20(10):1017–1022. https://doi.org/10.1111/iju.12090
Boucher WS, Letourneau R, Huang M, Kempuraj D, Green M, Sant GR et al (2002) Intravesical sodium hyaluronate inhibits the rat urinary mast cell mediator increase triggered by acute immobilization stress. J Urol 167(1):380–384
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Doğantekin, E., Akgül, T., Eser, E.P. et al. The effect of intraurethral hyaluronic acid on healing and fibrosis in rats with experimentally induced urethral trauma. Int Urol Nephrol 54, 757–761 (2022). https://doi.org/10.1007/s11255-022-03128-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-022-03128-1