Abstract
Objectives
To report our experience with eosinophilic cystitis (EC) presented as invasive bladder cancer.
Materials and methods
We recently treated three patients with bladder masses mimicking neoplasms and biopsy proved the diagnosis of EC. Data from our three patients were presented.
Results
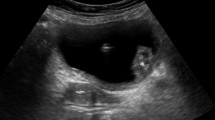
There were two females and one male with ages of 14, 43 and 38 years. All the three patients had irritative bladder symptoms, suprapubic pain and hematuria. Bladder mass was detected by pelvic examination in the three patients and confirmed by radiologic tests and cystoscopy. In one patient, the mass caused bilateral hydroureteronephrosis while the upper tract was normal in the other two. Elevated serum leukocytes was evident in the three cases while peripheral eosinophilia was observed in one. Biopsy showed EC in all the three patients who were treated by transurethral resection of the lesions followed by a combination of corticosteroids, antibiotics and antihistaminics. All patients experienced marked improvement during a follow-up duration up to 30 months.
Conclusion
EC is a rare disease. In addition to symptoms of frequency, dysuria, hematuria and suprapubic pain, the disease may present with a bladder mass mimicking invasive bladder cancer. Resection of the lesion is mandatory with systemic treatment of corticosteroids, antihistaminics and antibiotics. Early detection and prompt treatment usually result in a good prognosis.
Similar content being viewed by others
References
Brown EW (1960) Eosinophilic granuloma of the bladder. J Urol 83:665–668
Palubinskas AJ (1960) Eosinphilic cystitis: case report of eosinophilic infiltration of the urinary bladder. Radiology 75:589–591
Nancy IMB, Reza MS (2001) Eosinophilic cystitis in adults. J Urol 165:805–807
Thijssen A, Gerridzen RG (1990) Eosinophilic cystitis presenting as invasive bladder cancer: comments on pathogenesis and management. J Urol 144:97–99
Hansen MV, Kristensen PB (1993) Eosinophilic cystitis simulating invasive bladder carcinoma. Scand J Urol Nephrol 27:275–277
Constantinides C, Gavras P, Stinios J, Apostolaki C, Dimopoulos C (1994) Eosinophilic cystitis: a rare case which presented as an invasive bladder tumor. Acta Urol Belg 62:71–73
Barry KA, Jafri SZ (1994) Eosinophilic cystitis: CT findings. Abdom Imaging 19:272–273
van der Ouden D (2000) Diagnosis and management of eosinophilic cystitis. Eur Urol 37:386–394
Goldstein M (1971) Eosinophilic cystitis. J Urol 106:854–857
Littleton RH, Farah RN, Cerny JC (1982) Eosinophilic cystitis: an uncommon form of cystitis. J Urol 127:132–133
Mitas JA II, Thompson T (1985) Ureteral involvement complicating eosinophilic cystitis. Urology 26:67–70
Frensilli FJ, Sacher EC, Keegan GT (1972) Eosinopholic cystitis: observations on etiology. J Urol 10:595–596
Marshal FF, Middleton AW Jr (1974) Eosinophilic cystitis. J Urol 112:335–357
Hellstrom HR, Davis BK, Shonnard JW (1979) Eosinophilic cystitis. A study of 16 cases. Am J Clin Pathol 72:777–784
Sidh SM, Smith SP, Silber SB, Young JD (1980) Eosinophilic cystitis: advanced disease requiring surgical intervention. Urology 15:23–26
Castillo J Jr, Cartagena R, Montes M (1988) Eosinophilic cystitis: a therapeutic challenge. Urology 32:535–537
Motzkin D (1990) Nonsteroidal anti-inflammatory drugs in the treatment of eosinophilic cystitis. J Urol 144:1464–1466
Watson HS, Singh EO, Hermans MR, Coffield KS, Keegan GT (1992) Recurrent eosinophilic cystitis: a case responsive to steroids. J Urol 147:689–691
Oh SJ, Chi JG, Lee SE (1993) Eosinophilic cystitis caused by vesical sparganosis: a case report. J Urol 149:581–583
Flamm J (1992) Tumor associated tissue inflammatory reation and eosinophilia in primary superficial bladder cancer. Urology 40:180–182
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Salman, M., Al-Ansari, A.A., Talib, R.A. et al. Eosinophilic cystitis simulating invasive bladder cancer: a real diagnostic challenge. Int Urol Nephrol 38, 545–548 (2006). https://doi.org/10.1007/s11255-006-0103-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-006-0103-5