Abstract
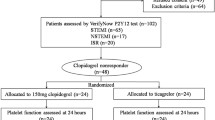
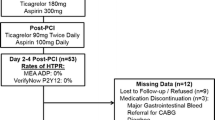
High on-treatment platelet reactivity (HTPR) despite use of P2Y12 antagonists is associated with adverse cardiac events. The long-term variability in response to prasugrel and ticagrelor is unclear. Our aim was to assess residual platelet reactivity (PR) and rates of HTPR during treatment with prasugrel versus ticagrelor in patients with myocardial infarction (MI). 114 patients with MI treated with percutaneous coronary intervention (PCI) were included. Sixty-two patients were treated with prasugrel (mean age 58 ± 8 years, 21 % women, 29 % diabetes), and 52 patients with ticagrelor (mean age 63 ± 9, 19 % women, 37 % diabetes). Patients were tested for PR at 2–4 days and 30 days post-PCI, using the VerifyNow P2Y12 assay and the multiple-electrode aggregometry. Our results show a higher residual PR in patients treated with prasugrel than those treated with ticagrelor (VerifyNow: 65.4 ± 60.6 vs. 26.0 ± 24.2 P2Y12 reaction units, p < 0.001 at 2–4 days, and 67.3 ± 62.5 vs. 21.1 ± 26.1, p < 0.001 at follow-up). HTPR rates were higher in the prasugrel group (8.1–11.3 % vs. none with ticagrelor in the early test, and 8.7–10.9 % vs. none with ticagrelor at follow-up). In conclusion, in patients with MI undergoing PCI, treatment with ticagrelor resulted in greater platelet inhibition and lower HTPR rates compared with prasugrel, up to 30 days after the event.


Similar content being viewed by others
References
Bonello L, Tantry US, Marcucci R, Blindt R, Angiolillo DJ, Becker R, Bhatt DL, Cattaneo M, Collet JP, Cuisset T, Gachet C, Montalescot G, Jennings LK, Kereiakes D, Sibbing D, Trenk D, Van Werkum JW, Paganelli F, Price MJ, Waksman R, Gurbel PA, Working Group on High On-Treatment Platelet Reactivity (2010) Consensus and future directions on the definition of high on-treatment platelet reactivity to adenosine diphosphate. J Am Coll Cardiol 56:919–933
Brar SS, ten Berg J, Marcucci R, Price MJ, Valgimigli M, Kim HS, Patti G, Breet NJ, DiSciascio G, Cuisset T, Dangas G (2011) Impact of platelet reactivity on clinical outcomes after percutaneous coronary intervention. A collaborative meta-analysis of individual participant data. J Am Coll Cardiol 58:1945–1954
Parodi G, Marcucci R, Valenti R, Gori AM, Migliorini A, Giusti B, Buonamici P, Gensini GF, Abbate R, Antoniucci D (2011) High residual platelet reactivity after clopidogrel loading and long-term cardiovascular events among patients with acute coronary syndromes undergoing PCI. JAMA 306:1215–1223
Sofi F, Marcucci R, Gori AM, Giusti B, Abbate R, Gensini GF (2010) Clopidogrel non-responsiveness and risk of cardiovascular morbidity.An updated meta-analysis. Thromb Haemost 103:841–848
Jernberg T, Payne CD, Winters KJ, Darstein C, Brandt JT, Jakubowski JA, Naganuma H, Siegbahn A, Wallentin L (2006) Prasugrel achieves greater inhibition of platelet aggregation and a lower rate of non-responders compared with clopidogrel in aspirin-treated patients with stable coronary artery disease. Eur Heart J 27:1166–1173
Wallentin L, Becker RC, Budaj A, Cannon CP, Emanuelsson H, Held C, Horrow J, Husted S, James S, Katus H, Mahaffey KW, Scirica BM, Skene A, Steg PG, Storey RF, Harrington RA, PLATO Investigators (2009) Ticagrelor versus clopidogrel in patients with acute coronary syndromes. N Engl J Med 361:1045–1057
Wiviott SD, Braunwald E, McCabe CH, Montalescot G, Ruzyllo W, Gottlieb S, Neumann FJ, Ardissino D, De Servi S, Murphy SA, Riesmeyer J, Weerakkody G, Gibson CM, Antman EM, TRITON-TIMI 38 Investigators (2007) Prasugrel versus clopidogrel in patients with acute coronary syndromes. N Engl J Med 357:2001–2015
Bonello L, Pansieri M, Mancini J, Bonello R, Maillard L, Barnay P, Rossi P, Ait-Mokhtar O, Jouve B, Collet F, Peyre JP, Wittenberg O, de Labriolle A, Camilleri E, Cheneau E, Cabassome E, Dignat-George F, Camoin-Jau L, Paganelli F (2011) High on-treatment platelet reactivity after prasugrel loading dose and cardiovascular events after percutaneous coronary intervention in acute coronary syndromes. J Am Coll Cardiol 58:467–473
Alexopoulos D, Xanthopoulou I, Gkizas V, Kassimis G, Theodoropoulos KC, Makris G, Koutsogiannis N, Damelou A, Tsigkas G, Davlouros P, Hahalis G (2012) Randomized assessment of ticagrelor versus prasugrel antiplatelet effects in patients with ST-segment-elevation myocardial infarction. Circ Cardiovasc Interv 5:797–804
Parodi G, Valenti R, Bellandi B, Migliorini A, Marcucci R, Comito V, Carrabba N, Santini A, Gensini GF, Abbate R, Antoniucci D (2013) Comparison of prasugrel and ticagrelor loading doses in ST-segment elevation myocardial infarction patients: RAPID (Rapid Activity of Platelet Inhibitor Drugs) primary PCI study. J Am Coll Cardiol 61:1601–1606
Perl L, Lerman-Shivek H, Rechavia E, Vaduganathan M, Leshem-Lev D, Zemer-Wassercug N, Dadush O, Codner P, Bental T, Battler A, Kornowski R, Lev EI (2014) Response to prasugrel and levels of circulating reticulated platelets in patients with st-segment elevation myocardial infarction. J Am Coll Cardiol 63(6):513–517
Alexopoulos D, Galati A, Xanthopoulou I, Mavronasiou E, Kassimis G, Theodoropoulos KC, Makris G, Damelou A, Tsigkas G, Hahalis G, Davlouros P (2012) Ticagrelor versus prasugrel in acute coronary syndrome patients with high on-clopidogrel platelet reactivity following percutaneous coronary intervention: a pharmacodynamic study. J Am Coll Cardiol 60:193–199
Laine M, Frère C, Toesca R, Berbis J, Barnay P, Pansieri M, Michelet P, Bessereau J, Camilleri E, Ronsin O, Helal O, Paganelli F, Dignat-George F, Bonello L (2013) Ticagrelor versus prasugrel in diabetic patients with an acute coronary syndrome.A pharmacodynamic randomised study. Thromb Haemost 111(2):273–278
Price MJ, Angiolillo DJ, Teirstein PS, Lillie E, Manoukian SV, Berger PB, Tanguay JF, Cannon CP, Topol EJ (2011) Platelet reactivity and cardiovascular outcomes after percutaneous coronary intervention: a time-dependent analysis of the gauging responsiveness with a Verifynow P2Y12 assay: impact on Thrombosis and Safety (GRAVITAS) trial. Circulation 124:1132–1137
Tantry US, Bonello L, Aradi D, Price MJ, Jeong YH, Angiolillo DJ, Stone GW, Curzen N, Geisler T, Ten Berg J, Kirtane A, Siller-Matula J, Mahla E, Becker RC, Bhatt DL, Waksman R, Rao SV, Alexopoulos D, Marcucci R, Reny JL, Trenk D, Sibbingc D, Gurbel PA, Working group on on-treatment platelet reactivity (2013) Consensus and update on the definition of on-treatment platelet reactivity to adenosine diphosphate associated with ischemia and bleeding. J Am Coll Cardiol 62(24):2261–2273
Jakubowski JA, Payne CD, Li YG, Brandt JT, Small DS, Farid NA, Salazar DE, Winters KJ (2008) The use of the VerifyNow P2Y12 point-of-care device to monitor platelet function across a range of P2Y12 inhibition levels following prasugrel and clopidogrel administration. Thromb Haemost 99:409–415
Park Y, Jeong YH, Kim IS, Yun SE, Kwon TJ, Hwang SJ, Kwak CH, Hwang JY (2012) The concordance and correlation of measurements by multiple electrode and light transmittance aggregometries based on the pre-defined cutoffs of high and low on-treatment platelet reactivity. Platelets 23:290–298
Ault KA, Rinder HM, Mitchell J, Carmody MB, Vary CP, Hillman RS (1992) The significance of platelets with increased RNA content (reticulated platelets). A measure of the rate of thrombopoiesis. Am J Clin Pathol 98:637–646
Parguiña AF, Grigorian-Shamagian L, Agra RM, López-Otero D, Rosa I, Alonso J, Teijeira-Fernández E, González-Juanatey JR, García Á (2011) Variations in platelet proteins associated with ST-elevation myocardial infarction: novel clues on pathways underlying platelet activation in acute coronary syndromes. Arterioscler Thromb Vasc Biol 31:2957–2964
Parguiña AF, Grigorian-Shamajian L, Agra RM, Teijeira-Fernández E, Rosa I, Alonso J, Viñuela-Roldán JE, Seoane A, González-Juanatey JR, García A (2010) Proteins involved in platelet signaling are differentially regulated in acute coronary syndrome: a proteomic study. PLoS One 5:e13404. doi:10.1371/journal.pone.0013404
Cuisset T, Loosveld M, Morange PE, Quilici J, Moro PJ, Saut N, Gaborit B, Castelli C, Beguin S, Grosdidier C, Fourcade L, Bonnet JL, Alessi MC (2012) CYP2C19*2 and *17 alleles have a significant impact on platelet response and bleeding risk in patients treated with prasugrel after acute coronary syndrome. J Am Coll Cardiol Intv 5:1280–1287
Franken CC, Kaiser AF, Kruger JC, Overbeck K, Mugge A, Neubauer H (2013) Cytochrome P450 2B6 and 2C9 genotype polymorphism–a possible cause of prasugrel low responsiveness. Thromb Haemost 110:131–140
Varenhorst C, James S, Erlinge D, Brandt JT, Braun OO, Man M, Siegbahn A, Walker J, Wallentin L, Winters KJ, Close SL (2009) Genetic variation of CYP2C19 affects both pharmacokinetic and pharmacodynamic responses to clopidogrel but not prasugrel in aspirin-treated patients with coronary artery disease. Eur Heart J 30:1744–1752
Brandt JT, Close SL, Iturria SJ, Payne CD, Farid NA, Ernest CS 2nd, Lachno DR, Salazar D, Winters KJ (2007) Common polymorphisms of CYP2C19 and CYP2C9 affect the pharmacokinetic and pharmacodynamic response to clopidogrel but not prasugrel. J Thromb Haemost 5(12):2429–2436
Tantry US, Bliden KP, Wei C, Storey RF, Armstrong M, Butler K, Gurbel PA (2010) First analysis of the relation between CYP2C19 genotype and pharmacodynamics in patients treated with ticagrelor versus clopidogrel: the ONSET/OFFSET and RESPOND genotype studies. Circ Cardiovasc Genet 3:556–566
Wallentin L, James S, Storey RF, Armstrong M, Barratt BJ, Horrow J, Husted S, Katus H, Steg PG, Shah SH, Becker RC, Investigators PLATO (2010) Effect of CYP2C19 and ABCB1 single nucleotide polymorphisms on outcomes of treatment with ticagrelor versus clopidogrel for acute coronary syndromes: a genetic substudy of the PLATO trial. Lancet 376:1320–1328
Sibbing D, Schulz S, Braun S, Morath T, Stegherr J, Mehilli J, Schömig A, von Beckerath N, Kastrati A (2010) Antiplatelet effects of clopidogrel and bleeding in patients undergoing coronary stent placement. J Thromb Haemost 8(2):250–256
Collet JP, Cuisset T, Rangé G, Cayla G, Elhadad S, Pouillot C, Henry P, Motreff P, Carrié D, Boueri Z, Belle L, Van Belle E, Rousseau H, Aubry P, Monségu J, Sabouret P, O’Connor SA, Abtan J, Kerneis M, Saint-Etienne C, Barthélémy O, Beygui F, Silvain J, Vicaut E, Montalescot G, ARCTIC Investigators (2012) Bedside monitoring to adjust antiplatelet therapy for coronary stenting. N Engl J Med 367(22):2100–2109
Cuisset T, Quilici J, Grosdidier C, Fourcade L, Gaborit B, Pankert M, Molines L, Morange PE, Bonnet JL, Alessi MC (2011) Comparison of platelet reactivity and clopidogrel response in patients ≤75 years versus >75 years undergoing percutaneous coronary intervention for non-ST-segment elevation acute coronary syndrome. Am J Cardiol 108(10):1411–1416
Silvain J, Cayla G, Hulot JS, Finzi J, Kerneis M, O’Connor SA, Bellemain-Appaix A, Barthélémy O, Beygui F, Collet JP, Montalescot G (2012) High on-thienopyridine platelet reactivity in elderly coronary patients: the SENIOR-PLATELET study. Eur Heart J 33(10):1241–1249
Vaturi M, Vaduganathan M, Bental T, Solodky A, Kornowski R, Lev EI (2013) Relation of aspirin response to age in patients with stable coronary artery disease. Am J Cardiol 112(2):212–216
Schulz S, Angiolillo DJ, Antoniucci D, Bernlochner I, Hamm C, Jaitner J, Laugwitz KL, Mayer K, von Merzljak B, Morath T, Neumann FJ, Richardt G, Ruf J, Schömig G, Schühlen H, Schunkert H, Kastrati A, Intracoronary Stenting and Antithrombotic Regimen: rapid Early Action for Coronary Treatment (ISAR-REACT) 5 Trial Investigators (2014) Randomized comparison of ticagrelor versus prasugrel in patients with acute coronary syndrome and planned invasive strategy–design and rationale of the Intracoronary Stenting and Antithrombotic Regimen: Rapid Early Action for Coronary Treatment (ISAR-REACT) 5 trial. J Cardiovasc Transl Res 7(1):91–100
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Perl, L., Zemer-Wassercug, N., Rechavia, E. et al. Comparison of platelet inhibition by prasugrel versus ticagrelor over time in patients with acute myocardial infarction. J Thromb Thrombolysis 39, 1–7 (2015). https://doi.org/10.1007/s11239-014-1119-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-014-1119-9