Abstract
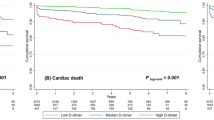
D-dimer is a final product of fibrin degradation and gives an indirect estimation of the thrombotic burden. We aimed to investigate the value of plasma D-dimer levels on admission in predicting no-reflow after primary percutaneous coronary intervention (p-PCI) and long-term prognosis in patients with ST segment elevation myocardial infarction (STEMI). We retrospectively involved 569 patients treated with p-PCI for acute STEMIs. We prospectively followed up the patients for a median duration of 38 months. Angiographic no-reflow was defined as postprocedural thrombolysis in myocardial infarction (TIMI) flow grade <3 or TIMI 3 with a myocardial blush grade <2. Electrocardiographic no-reflow was defined as ST-segment resolution <70 %. The primary clinical end points were mortality and major adverse cardiovascular events (MACE). The incidences of angiographic and electrocardiographic no-reflow were 31 and 39 % respectively. At multivariable analysis, D-dimer was found to be an independent predictor of both angiographic (p < 0.001), and electrocardiographic (p < 0.001) no-reflow. Both mortality (from Q1 to Q4, 5.7, 6.4, 11.3 and 34.1 %, respectively, p < 0.001) and MACE (from Q1 to Q4, 17.9, 29.3, 36.9 and 52.2 %, respectively, p < 0.001) rates at long-term follow-up were highest in patients with admission D-dimer levels in the highest quartile (Q4), compared to the rates in other quartiles. However, Cox proportional hazard model revealed that high D-dimer on admission (Q4) was not an independent predictor of mortality or MACE. In contrast, electrocardiographic no-reflow was independently predictive of both mortality [Hazard ratio (HR) 2.88, 95 % confidence interval (CI) 1.04–8.58, p = 0.041] and MACE [HR 1.90, 95 % CI 1.32–4.71, p = 0.042]. In conclusion, plasma D-dimer level on admission independently predicts no-reflow after p-PCI. However, D-dimer has no independent prognostic value in patients with STEMI.


Similar content being viewed by others
References
Keeley EC, Boura JA, Grines CL (2003) Primary angioplasty versus intravenous thrombolytic therapy for acute myocardial infarction: a quantitative review of 23 randomised trials. Lancet 361:13–20
Rezkalla SH, Kloner RA (2008) Coronary no-reflow phenomenon: from the experimental laboratory to the cardiac catheterization laboratory. Catheter Cardiovasc Interv 72:950–957
Niccoli G, Burzotta F, Galiuto L, Crea F (2009) Myocardial no-reflow in humans. J Am Coll Cardiol 54:281–292
Jaffe R, Dick A, Strauss BH (2010) Prevention and treatment of microvascular obstruction-related myocardial injury and coronary no-reflow following percutaneous coronary intervention: a systematic approach. JACC Cardiovasc Interv 3:695–704
Niccoli G, Kharbanda RK, Crea F, Banning AP (2010) No-reflow: again prevention is better than treatment. Eur Heart J 31:2449–2455
Hou H, Ge Z, Ying P, Dai J, Shi D, Xu Z, Chen D, Jiang Q (2012) Biomarkers of deep venous thrombosis. J Thromb Thrombolysis 34:335–346
Undas A, Szułdrzynski K, Stepien E, Zalewski J, Godlewski J, Tracz W, Pasowicz M, Zmudka K (2008) Reduced clot permeability and susceptibility to lysis in patients with acute coronary syndrome: effects of inflammation and oxidative stress. Atherosclerosis 196:551–557
Napodano M, Ramondo A, Tarantini G, Peluso D, Compagno S, Fraccaro C, Frigo AC, Razzolini R, Iliceto S (2009) Predictors and time-related impact of distal embolization during primary angioplasty. Eur Heart J 30:305–313
Izgi A, Kirma C, Tanalp AC, Dundar C, Oduncu V, Aung SM, Sonmez K, Mutlu B, Mansuroglu D (2007) Predictors and clinical significance of angiographically detected distal embolization after primary percutaneous coronary interventions. Coron Artery Dis 18:443–449
de Lemos JA, Braunwald E (2001) ST segment resolution as a tool for assessing the efficacy of reperfusion therapy. J Am Coll Cardiol 38:1283–1294
Gottdiener JS, Bednarz J, Devereux R, Gardin J, Klein A, Manning WJ, Morehead A, Kitzman D, Oh J, Quinones M, Schiller NB, Stein JH, Weissman NJ (2004) American Society of Echocardiography recommendations for use of echocardiography in clinical trials. J Am Soc Echocardiogr 17:1086–1119
Gibson CM, Murphy SA, Rizzo MJ, Ryan KA, Marble SJ, McCabe CH, Cannon CP, Van de Werf F, Braunwald E (1999) The relationship between the TIMI frame count and clinical outcomes after thrombolytic administration. Circulation 99:1945–1950
van’t Hof AWJ, Liem A, Suryapranata H, Hoorntje JC, de Boer MJ, Zijlstra F (1998) Angiographic assessment of myocardial reperfusion in patients treated with primary angioplasty for acute myocardial infarction: myocardial blush grade. Circulation 97:2302–2306
Gibson CM, de Lemos JA, Murphy SA, Marble SJ, McCabe CH, Cannon CP, Antman EM, Braunwald E (2001) Combination therapy with abciximab reduces angiographically evident thrombus in acute myocardial infarction: a TIMI 14 substudy. Circulation 103:2550–2554
Rentrop KP, Cohen M, Blanke H, Phillips RA (1985) Changes in collateral channel filling immediately after controlled coronary artery occlusion by an angioplasty balloon in human subjects. J Am Coll Cardiol 5:587–592
Yip HK, Chen MC, Chang HW, Hang CL, Hsieh YK, Fang CY, Wu CJ (2002) Angiographic morphologic features of infarct-related arteries and timely reperfusion in acute myocardial infarction: predictors of slow-flow and no-reflow phenomenon. Chest 122:1322–1332
Limbruno U, De Carlo M, Pistolesi S, Micheli A, Petronio AS, Camacci T, Fontanini G, Balbarini A, Mariani M, De Caterina R (2005) Distal embolization during primary angioplasty: histopathologic features and predictability. Am Heart J 150:102–108
Becattini C, Lignani A, Masotti L, Forte MB, Agnelli G (2012) D-dimer for risk stratification in patients with acute pulmonary embolism. J Thromb Thrombolysis 33:48–57
Hochuli M, Duewell S, Frauchiger B (2007) Quantitative d-dimer levels and the extent of venous thromboembolism in CT angiography and lower limb ultrasonography. Vasa 36:267–274
Fokkema ML, Vlaar PJ, Svilaas T, Vogelzang M, Amo D, Diercks GF, Suurmeijer AJ, Zijlstra F (2009) Incidence and clinical consequences of distal embolization on the coronary angiogram after percutaneous coronary intervention for ST-elevation myocardial infarction. Eur Heart J 30:908–915
Demircan S, Yazici M, Hamiseyev C, Demircan G, Sultansuyu S, Yasar E, Sahin M (2007) The role of fibrinolytic system in no-reflow after stenting with and without predilation in patients with acute coronary syndromes: fibrinolysis and no-reflow after coronary stenting. J Thromb Thrombolysis 24:109–114
Francis CW, Connaghan DG, Scott WL, Marder VJ (1987) Increased plasma concentration of cross-linked fibrin polymers in acute myocardial infarction. Circulation 75:1170–1177
McCann CJ, Glover BM, Menown IB, Moore MJ, McEneny J, Owens CG, Smith B, Sharpe PC, Young IS, Adgey JA (2009) Prognostic value of a multimarker approach for patients presenting to hospital with acute chest pain. Am J Cardiol 103:22–28
Brügger-Andersen T, Pönitz V, Staines H, Grundt H, Hetland Ø, Nilsen DW (2008) The prognostic utility of D-dimer and fibrin monomer at long-term follow-up after hospitalization with coronary chest pain. Blood Coagul Fibrinolysis 19:701–707
Fiotti N, Di Chiara A, Altamura N, Miccio M, Fioretti P, Guarnieri G, Giansante C (2002) Coagulation indicators in chronic stable effort angina and unstable angina: relationship with acute phase reactants and clinical outcome. Blood Coagul Fibrinolysis 13:247–255
Yang J, Li CS (2012) The predictive values of D-dimer for the early prognosis of the acute myocardial infarction (AMI): a review of 3134 AMI patients]. Zhongguo Wei Zhong Bing Ji Jiu Yi Xue 24:725–729
Kikkert WJ, Claessen BE, Stone GW, Mehran R, Witzenbichler B, Brodie BR, Wöhrle J, Witkowski A, Guagliumi G, Zmudka K, Henriques JP, Tijssen JG, Sanidas EA, Chantziara V, Xu K, Dangas GD (2013) D-dimer levels predict ischemic and hemorrhagic outcomes after acute myocardial infarction: a HORIZONS-AMI biomarker substudy. J Thromb Thrombolysis. doi:10.1007/s11239-013-0953-5
Akgul O, Uyarel H, Pusuroglu H, Gul M, Isiksacan N, Turen S, Erturk M, Surgit O, Cetin M, Bulut U, Baycan OF, Uslu N (2013) Predictive value of elevated D-dimer in patients undergoing primary angioplasty for ST elevation myocardial infarction. Blood Coagul Fibrinolysis 24:704–710
Ndrepepa G, Tiroch K, Fusaro M, Keta D, Seyfarth M, Byrne RA, Pache J, Alger P, Mehilli J, Schömig A, Kastrati A (2010) 5-year prognostic value of no-reflow phenomenon after percutaneous coronary intervention in patients with acute myocardial infarction. J Am Coll Cardiol 55:2383–2389
Goldin Y, Pasvolsky O, Rogowski O, Shapira I, Steinvil A, Halpern P, Serov J, Deutsch V, Aviram G, Berliner S (2011) The diagnostic yield of D-Dimer in relation to time from symptom onset in patients evaluated for venous thromboembolism in the emergency medicine department. J Thromb Thrombolysis 31:1–5
Acknowledgments
None.
Conflict of interest
The authors have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Erkol, A., Oduncu, V., Turan, B. et al. The value of plasma D-dimer level on admission in predicting no-reflow after primary percutaneous coronary intervention and long-term prognosis in patients with acute ST segment elevation myocardial infarction. J Thromb Thrombolysis 38, 339–347 (2014). https://doi.org/10.1007/s11239-013-1044-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-013-1044-3