Abstract
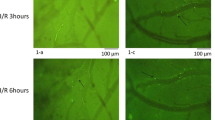
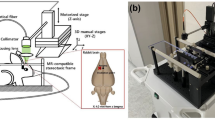
Antiplatelet drugs have been evaluated by measuring platelet aggregation ex vivo, but in vivo studies were scanty. The purpose of this study was to observe the effects of an antiplatelet agent (clopidogrel) on the process of laser-induced thrombus formation in mice using intravital fluorescence microscopy. C57 BL/6J mice (n = 19) were anesthetized using chloral hydrate. The head of each mouse was fixed with a head holder, and a cranial window was made in the parietal region. Platelets were labeled in vivo by intravenous administration of carboxyfluorescein diacetate succinimidyl ester. Clopidogrel (1 mg/kg, n = 6; 10 mg/kg, n = 6) was administered orally for 2 days before the experiment. Another seven mice were used as controls. Laser irradiation (1,000 mA, 9.8 mW, diode-pumped solid-state (DPSS) laser 532 nm) was directed for 4 s at pial arteries to induce thrombus formation. Labeled platelets and thrombus were observed continuously under fluorescence microscopy. We recorded the area of thrombus after 30 min and determined the complete occlusion rate. After laser irradiation to the pial artery, complete occlusion rate was significantly lower in the clopidogrel (10 mg/kg) group (16%, 4/25 vessels) than in the control group (60%, 12/20 vessels) or clopidogrel (1 mg/kg) group (55%, 11/20 vessels). Area of platelet thrombus at 30 min after laser irradiation was significantly smaller in the clopidogrel (10 mg/kg) group (209 ± 128 μm2) than in the control group (358 ± 256 μm2) or clopidogrel (1 mg/kg) group (355 ± 57 μm2). The apparatus which we developed is convenient for inducing thrombus formation by causing endothelial cell damage to the brain surface vasculature in small animals without damage of extravascular tissue. Clopidogrel significantly inhibited laser-induced thrombus formation in pial arteries of mice in a dose-dependent manner.





Similar content being viewed by others
References
Ruggeri ZM (2003) Von Willebrand factor, platelets and endothelial cell interactions. J Thromb Haemost 1(7):1335–1342
Ishikawa M, Sekizuka E, Oshio C, Sato S, Yamaguchi N, Terao S, Tsukada K, Minamitani H, Kawase T (2002) Platelet adhesion and arteriolar dilation in the photothrombosis: observation with the rat closed cranial and spinal windows. J Neurol Sci 194(1):59–69
Watson BD, Dietrich WD, Busto R, Wachtel MS, Ginsberg MD (1985) Induction of reproducible brain infarction by photochemically initiated thrombosis. Ann Neurol 17(5):497–504. doi:10.1002/ana.410170513
Dietrich WD, Watson BD, Busto R, Ginsberg MD, Bethea JR (1987) Photochemically induced cerebral infarction. I. Early microvascular alterations. Acta Neuropathol 72(4):315–325
Nakayama H, Dietrich WD, Watson BD, Busto R, Ginsberg MD (1988) Photothrombotic occlusion of rat middle cerebral artery: histopathological and hemodynamic sequelae of acute recanalization. J Cereb Blood Flow Metab 8(3):357–366
Umemura K, Ishihara H, Nakashima M (1995) Anti-platelet effects of clopidogrel in rat middle cerebral artery thrombosis model. Thromb Res 80(3):209–216
Umemura K (1997) A novel photochemical model of the middle cerebral artery for thrombosis research and evaluation of anti-thrombotic agents. Folia Pharmacologica Japonica 109(4):175–185 (in Japanese)
Nishimura H, Naritomi H, Iwamoto Y, Tachibana H, Sugita M (1996) In vivo evaluation of antiplatelet agents in gerbil model of carotid artery thrombosis. Stroke 27(6):1099–1103 (discussion 1104)
Hechler B, Gachet C (2011) Comparison of two murine models of thrombosis induced by atherosclerotic plaque injury. Thromb Haemost 105(Suppl 1):S3–S12. doi:10.1160/THS10-11-0730
Hechler B, Nonne C, Eckly A, Magnenat S, Rinckel JY, Denis CV, Freund M, Cazenave JP, Lanza F, Gachet C (2010) Arterial thrombosis: relevance of a model with two levels of severity assessed by histologic, ultrastructural and functional characterization. J Thromb Haemost 8(1):173–184. doi:10.1111/j.1538-7836.2009.03666.x
Falati S, Gross P, Merrill-Skoloff G, Furie BC, Furie B (2002) Real-time in vivo imaging of platelets, tissue factor and fibrin during arterial thrombus formation in the mouse. Nat Med 8(10):1175–1181. doi:10.1038/nm782
Celi A, Merrill-Skoloff G, Gross P, Falati S, Sim DS, Flaumenhaft R, Furie BC, Furie B (2003) Thrombus formation: direct real-time observation and digital analysis of thrombus assembly in a living mouse by confocal and widefield intravital microscopy. J Thromb Haemost 1(1):60–68
Rosen ED, Raymond S, Zollman A, Noria F, Sandoval-Cooper M, Shulman A, Merz JL, Castellino FJ (2001) Laser-induced noninvasive vascular injury models in mice generate platelet- and coagulation-dependent thrombi. Am J Pathol 158(5):1613–1622. doi:10.1016/S0002-9440(10)64117-X
Kovacs IB, Tigyi-Sebes A, Trombitas K, Gorog P (1975) Evans blue: an ideal energy-absorbing material to produce intravascular microinjury by HE-NE gas laser. Microvasc Res 10(1):107–124
Yamashita T, Oda E, Sano T, Ijiru Y, Giddings JC, Yamamoto J (2005) Varying the ratio of dietary n − 6/n − 3 polyunsaturated fatty acid alters the tendency to thrombosis and progress of atherosclerosis in apoE−/− LDLR−/− double knockout mouse. Thromb Res 116(5):393–401. doi:10.1016/j.thromres.2005.01.011
Nishimura N, Schaffer CB, Friedman B, Tsai PS, Lyden PD, Kleinfeld D (2006) Targeted insult to subsurface cortical blood vessels using ultrashort laser pulses: three models of stroke. Nat Methods 3(2):99–108. doi:10.1038/nmeth844
CAPRIE Steering Committee (1996) A randomised, blinded, trial of clopidogrel versus aspirin in patients at risk of ischaemic events (CAPRIE). Lancet 348(9038):1329–1339
Bhatt DL, Hirsch AT, Ringleb PA, Hacke W, Topol EJ (2000) Reduction in the need for hospitalization for recurrent ischemic events and bleeding with clopidogrel instead of aspirin. CAPRIE investigators. Am Heart J 140(1):67–73
Fukuoka T, Furuya D, Takeda H, Dembo T, Nagoya H, Kato Y, Deguchi I, Maruyama H, Horiuchi Y, Tanahashi N (2011) Evaluation of clopidogrel resistance in ischemic stroke patients. Intern Med 50(1):31–35
Maruyama H, Takeda H, Dembo T, Nagoya H, Kato Y, Fukuoka T, Deguchi I, Horiuchi Y, Tanahashi N (2011) Clopidogrel resistance and the effect of combination cilostazol in patients with ischemic stroke or carotid artery stenting using the VerifyNow P2Y12 Assay. Intern Med 50(7):695–698
Acknowledgments
The authors wish to thank Professor Masumi Akita and Kayoko Tanaka from the Division of Morphological Science, Biomedical Research Center, Saitama Medical University for their cooperation in preparing electron micrographs of mouse pial arteries.
Conflicts of interest
NT has received payment for development of educational presentations from Mitsubishi Tanabe Pharma, Pfizer Japan, Sanofi-Aventis, and Otsuka Pharmaceutical. TF, KH, HM and MH declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
This study was supported by Grant from Ochiai memorial award 2011.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary material 1 (WMV 8486 kb)
Supplementary material 2 (WMV 6453 kb)
Rights and permissions
About this article
Cite this article
Fukuoka, T., Hattori, K., Maruyama, H. et al. Laser-induced thrombus formation in mouse brain microvasculature: effect of clopidogrel. J Thromb Thrombolysis 34, 193–198 (2012). https://doi.org/10.1007/s11239-012-0703-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-012-0703-0