Abstract
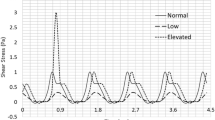
A heightened flow shear stress magnitude or increased exposure duration at any shear stress magnitude enhances platelet activation. It has been suggested that increased circulating activated platelets are an indication of enhanced cardiovascular risk and that activated platelets can perpetuate cardiovascular diseases. However, the combined effects that shear stress and shear exposure duration have on platelet activation and aggregation are not clear. Our objective was to identify a new parameter (“shear stress-exposure time”) to predict platelet functional changes better than the absolute magnitude of shear stress. Platelets were exposed to shear stress waveforms, with different combinations of shear stress magnitude and exposure duration, in a circulation flow loop. Timed samples were removed from the flow loop to quantify thrombogenicity (modified prothrombinase assay), aggregation potential (optical platelet aggregometry), and cell surface marker expression (flow cytometry). Flow induced platelet activation and aggregation was enhanced with increased shear stress-exposure time. Platelets that were exposed to waveforms with the same shear stress-exposure time had the same thrombogenicity and aggregation potential. This was true even for waveforms that exposed platelets to shear stress magnitudes varying from 4 to 40 dynes/cm2. These results indicate that shear stress-exposure time is a good predictor of platelet activation and aggregation levels and it may be able to predict the likelihood of cardiovascular disease onset.






Similar content being viewed by others
References
Cicha I, Yilmaz A, Suzuki Y, Maeda N, Daniel WG, Goppelt-Struebe M, Garlichs CD (2006) Connective tissue growth factor is released from platelets under high shear stress and is differentially expressed in endothelium along atherosclerotic plaques. Clin Hemorheol Microcirc 35:203–206
Nomura S, Tandon NN, Nakamura T, Cone J, Fukuhara S, Kambayashi J (2001) High-shear-stress-induced activation of platelets and microparticles enhances expression of cell adhesion molecules in THP-1 and endothelial cells. Atherosclerosis 158:277–287
Britten MB, Zeiher AM, Schachinger V (2003) Effects of cardiovascular risk factors on coronary artery remodeling in patients with mild atherosclerosis. Coron Artery Dis 14:415–422
Lindemann S, Kramer B, Seizer P, Gawaz M (2007) Platelets, inflammation and atherosclerosis. J Thromb Haemost 5(Suppl 1):203–211
Marquardt L, Ruf A, Mansmann U, Winter R, Schuler M, Buggle F, Mayer H, Grau AJ (2002) Course of platelet activation markers after ischemic stroke. Stroke 33:2570–2574
Hellums JD (1994) 1993 Whitaker Lecture: biorheology in thrombosis research. Ann Biomed Eng 22:445–455
Holme PA, Orvim U, Hamers MJ, Solum NO, Brosstad FR, Barstad RM, Sakariassen KS (1997) Shear-induced platelet activation and platelet microparticle formation at blood flow conditions as in arteries with a severe stenosis. Arterioscler Thromb Vasc Biol 17:646–653
Nomura S, Imamura A, Okuno M, Kamiyama Y, Fujimura Y, Ikeda Y, Fukuhara S (2000) Platelet-derived microparticles in patients with arteriosclerosis obliterans: enhancement of high shear-induced microparticle generation by cytokines. Thromb Res 98:257–268
Konstantopoulos K, Grotta JC, Sills C, Wu KK, Hellums JD (1995) Shear-induced platelet aggregation in normal subjects and stroke patients. Thromb Haemost 74:1329–1334
Rubenstein D, Jesty J, Bluestein D (2004) Differences between mainstream and sidestream cigarette smoke extracts and nicotine in the activation of platelets under static and flow conditions. Circulation 109:78–83
Jesty J, Yin W, Perrotta P, Bluestein D (2003) Platelet activation in a circulating flow loop: combined effects of shear stress and exposure time. Platelets 14:143–149
Pantos I, Patatoukas G, Efstathopoulos EP, Katritsis D (2007) In vivo wall shear stress measurements using phase-contrast MRI. Expert Rev Cardiovasc Ther 5:927–938
Soulis JV, Farmakis TM, Giannoglou GD, Louridas GE (2006) Wall shear stress in normal left coronary artery tree. J Biomech 39:742–749
Sui B, Gao P, Lin Y, Gao B, Liu L, An J (2008) Assessment of wall shear stress in the common carotid artery of healthy subjects using 3.0-tesla magnetic resonance. Acta Radiol 49:442–449
Jesty J, Bluestein D (1999) Acetylated prothrombin as a substrate in the measurement of the procoagulant activity of platelets: elimination of the feedback activation of platelets by thrombin. Anal Biochem 272:64–70
Rubenstein DA, Yin W (2009) Glycated albumin modulates platelet susceptibility to flow induced activation and aggregation. Platelets 20:206–215
Szarvas M, Oparaugo P, Udvardy ML, Toth J, Szanto T, Daroczi L, Vereb G, Harsfalvi J (2006) Differential platelet deposition onto collagen in cone-and-plate and parallel plate flow chambers. Platelets 17:185–190
Eto K, Isshiki T, Yamamoto H, Takeshita S, Ochiai M, Yokoyama N, Yoshimoto R, Ikeda Y, Sato T (1999) AJvW-2, an anti-vWF monoclonal antibody, inhibits enhanced platelet aggregation induced by high shear stress in platelet-rich plasma from patients with acute coronary syndromes. Arterioscler Thromb Vasc Biol 19:877–882
Sadiq A, Tamura N, Yoshida M, Hoshiba Y, Kumagai A, Tanabe T, Handa S, Ikeda Y, Goto S (2003) Possible contribution of acetylamrinone and its enhancing effects on platelet aggregation under shear stress conditions in the onset of thrombocytopenia in patients treated with amrinone. Thromb Res 111:357–361
Hu H, Varon D, Hjemdahl P, Savion N, Schulman S, Li N (2003) Platelet-leukocyte aggregation under shear stress: differential involvement of selectins and integrins. Thromb Haemost 90:679–687
Neeves KB, Maloney SF, Fong KP, Schmaier AA, Kahn ML, Brass LF, Diamond SL (2008) Microfluidic focal thrombosis model for measuring murine platelet deposition and stability: PAR4 signaling enhances shear-resistance of platelet aggregates. J Thromb Haemost 6:2193–2201
Yin W, Alemu Y, Affeld K, Jesty J, Bluestein D (2004) Flow-induced platelet activation in bileaflet and monoleaflet mechanical heart valves. Ann Biomed Eng 32:1058–1066
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rubenstein, D.A., Yin, W. Quantifying the effects of shear stress and shear exposure duration regulation on flow induced platelet activation and aggregation. J Thromb Thrombolysis 30, 36–45 (2010). https://doi.org/10.1007/s11239-009-0397-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-009-0397-0