Abstract
Purpose
Postmenopausal osteoporosis has become a global trend, which seriously affects women’s quality of life. However, the differences remain unclear in health-related quality of life (HRQoL) among postmenopausal women with normal bone mineral density, osteoporosis, and osteoporotic fractures. The aim of this study was to assess health-related quality of life in women with three different bone states.
Methods
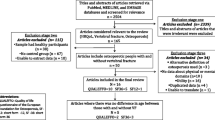
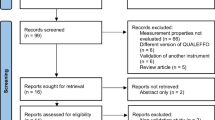
Databases of PubMed, Embase, Cochrane, and Web of Science were based on the search terms, and the search time was set from the inception of each database to January 2022. A study was included if the researchers used a validated quality of life questionnaire to investigate the quality of life of postmenopausal women with osteoporosis or osteoporotic fractures. The random-effect model was used for meta-analysis, and the mean difference with a 95% confidence interval (95%CI) was calculated.
Results
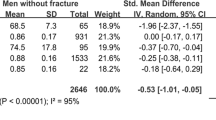
Thirteen studies that met the inclusion criteria were systematically reviewed, involving 2897 postmenopausal women, and 12 of them were included in the meta-analysis. Postmenopausal women with osteoporosis had worse overall HRQoL and different HRQoL dimensions compared with postmenopausal women with normal bone density. Compared with postmenopausal women with osteoporosis, postmenopausal women with osteoporotic fractures had worse overall HRQoL and individual dimensions of HRQoL, especially physical component summary (SMD = − 0.61, 95% CI, − 0.98 to − 0.24). Bone mineral density was positively associated with HRQoL, while fragility fracture severity was negatively associated with HRQoL.
Conclusions
Postmenopausal osteoporosis and fragility fractures reduce HRQoL to varying degrees in women. More research should be done to reduce the incidence of the disease.







Similar content being viewed by others
Data availability
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
References
Man, W., Wang, S., & Yang, H. (2021). Exploring the spatial-temporal distribution and evolution of population aging and social-economic indicators in China. BMC Public Health, 21(1), 966. https://doi.org/10.1186/s12889-021-11032-z
Li, L., & Wang, Z. (2018). Ovarian aging and osteoporosis. In Z. Wang (Ed.), Aging and aging-related diseases: mechanisms and interventions. Springer. https://doi.org/10.1007/978-981-13-1117-8_13
Gold, D. T. (1996). The clinical impact of vertebral fractures: Quality of life in women with osteoporosis. Bone, 18(3 Suppl), 185s–189s. https://doi.org/10.1016/8756-3282(95)00500-5
Cummings, S. R., & Melton, L. J. (2002). Epidemiology and outcomes of osteoporotic fractures. Lancet, 359(9319), 1761–1767. https://doi.org/10.1016/s0140-6736(02)08657-9
Masaryková, L., Fulmeková, M., Lehocká, Ľ, & Ďurdík, T. (2015). The quality of life of patients suffering from the osteoporosis. Ceska A Slovenska Farmacie, 64(3), 72–78.
Wilson, S., Sharp, C. A., & Davie, M. W. (2012). Health-related quality of life in patients with osteoporosis in the absence of vertebral fracture: A systematic review. Osteoporosis International, 23(12), 2749–2768. https://doi.org/10.1007/s00198-012-2050-6
Gokosmanoglu, F., Varim, C., Atmaca, A., Atmaca, M. H., & Colak, R. (2016). The effects of zoledronic acid treatment on depression and quality of life in women with postmenopausal osteoporosis: A clinical trial study. Journal of Research in Medical Sciences, 21(1), 112. https://doi.org/10.4103/1735-1995.193503
Huedo-Medina, T. B., Sánchez-Meca, J., Marín-Martínez, F., & Botella, J. (2006). Assessing heterogeneity in meta-analysis: Q statistic or I2 index? Psychological Methods, 11(2), 193–206. https://doi.org/10.1037/1082-989x.11.2.193
Cumpston, M., Li, T., Page, M. J., Chandler, J., Welch, V. A., Higgins, J. P., et al. (2019). Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database of Systematic Reviews. https://doi.org/10.1002/14651858.Ed000142
Ferreira, N., & d. O., Arthuso, M., da Silva, R., Pedro, A. O., Pinto Neto, A. M., & Costa-Paiva, L. (2009). Quality of life in women with postmenopausal osteoporosis: Correlation between QUALEFFO 41 and SF-36. Maturitas, 62(1), 85–90. https://doi.org/10.1016/j.maturitas.2008.10.012
Ciubean, A. D., Ungur, R. A., Irsay, L., Ciortea, V. M., Borda, I. M., Onac, L., et al. (2018). Health-related quality of life in Romanian postmenopausal women with osteoporosis and fragility fractures. Clinical Interventions in Aging, 13, 2465–2472. https://doi.org/10.2147/cia.S190440
Korkmaz, N., Tutoʇlu, A., Korkmaz, I., & Boyaci, A. (2013). The relationships between vitamin d level, balance, muscle strenght and quality of life in postmenopausal patients with osteoporosis. Turkiye Fiziksel Tip ve Rehabilitasyon Dergisi, 59(1), 381. https://doi.org/10.4274/tftr.24.59.1
Ferreira, N., & d. O., Arthuso, M., da Silva, R. B., Pinto-Neto, A. M., & Costa-Paiva, L. (2013). Validation of the Portuguese version of the quality of life questionnaire of the European foundation for osteoporosis (QUALEFFO-41) in Brazilian women with postmenopausal osteoporosis with vertebral fracture. Clinical Rheumatology, 32(11), 1585–1592. https://doi.org/10.1007/s10067-013-2265-8
Paker, N., Buǧdayci, D., Dere, D., Tekdöş, D., Erbil, E., & Dere, Ç. (2012). Relationship between bone density and quality of life in postmenopausal osteoporosis. Turk Geriatri Dergisi, 15(1), 19–23.
Sanfelix-Genoves, J., Hurtado, I., Sanfelix-Gimeno, G., Reig-Molla, B., & Peiro, S. (2011). Impact of osteoporosis and vertebral fractures on quality-of-life a population-based study in Valencia, Spain (The FRAVO Study). Health and Quality of Life Outcomes, 9(1), 1–20. https://doi.org/10.1186/1477-7525-9-20
Baczyk, G., Opala, T., & Kleka, P. (2011). Quality of life in postmenopausal women with reduced bone mineral density: Psychometric evaluation of the polish version of QUALEFFO-41. Archives of Medical Science, 7(3), 476–485. https://doi.org/10.5114/aoms.2011.23415
Lasaite, L., & Krasauskiene, A. (2009). Psychological state, quality of life, and body composition in postmenopausal women with osteoporosis in Lithuania. Archives of Osteoporosis, 4(1–2), 85–90. https://doi.org/10.1007/s11657-009-0034-8
Salaffi, F., Cimmino, M. A., Malavolta, N., Carotti, M., Di Matteo, L., Scendoni, P., et al. (2007). The burden of prevalent fractures on health-related quality of life in postmenopausal women with osteoporosis: The IMOF study. Journal of Rheumatology, 34(7), 1551–1560.
Bianchi, M. L., Orsini, M. R., Saraifoger, S., Ortolani, S., Radaelli, G., & Betti, S. (2005). Quality of life in post-menopausal osteoporosis. Health and Quality of Life Outcomes, 3(1), 78. https://doi.org/10.1186/1477-7525-3-78
Cvijetic, S., Mestrovic, T., Crkvenac, A., Davila, S., & Korsic, M. (2002). Quality of life in osteoporotic patients with hip fracture and without fracture. Arhiv za higijenu rada i toksikologiju, 53(4), 257–262.
Miyakoshi, N., Kudo, D., Hongo, M., Kasukawa, Y., Ishikawa, Y., & Shimada, Y. (2017). Comparison of spinal alignment, muscular strength, and quality of life between women with postmenopausal osteoporosis and healthy volunteers. Osteoporosis International, 28(11), 3153–3160. https://doi.org/10.1007/s00198-017-4184-z
Albayrak, I., Aydogmus, M., Ozerbil, O. M., & Levendoglu, F. (2016). The association between bone mineral density, quality of life, quality of sleep and fatigue. Acta Clinica Belgica, 71(2), 92–98. https://doi.org/10.1179/2295333715y.0000000061
Ensrud, K. E. (2013). Epidemiology of fracture risk with advancing age. Journals of Gerontology. Series A, Biological Sciences and Medical Sciences, 68(10), 1236–1242. https://doi.org/10.1093/gerona/glt092
Laurent, M. R., Dedeyne, L., Dupont, J., Mellaerts, B., Dejaeger, M., & Gielen, E. (2019). Age-related bone loss and sarcopenia in men. Maturitas, 122, 51–56. https://doi.org/10.1016/j.maturitas.2019.01.006
Elmadfa, I., & Meyer, A. L. (2008). Body composition, changing physiological functions and nutrient requirements of the elderly. Annals of Nutrition and Metabolism, 52(1), 2–5. https://doi.org/10.1159/000115339
Li, L., Bennett-Brown, K., Morgan, C., & Dattani, R. (2020). Hip fractures. British Journal of Hospital Medicine, 81(8), 1–10. https://doi.org/10.12968/hmed.2020.0215
Brunner, L. C., Eshilian-Oates, L., & Kuo, T. Y. (2003). Hip fractures in adults. American Family Physician, 67(3), 537–542.
Magaziner, J., Chiles, N., & Orwig, D. (2015). Recovery after Hip Fracture: Interventions and Their Timing to Address Deficits and Desired Outcomes Evidence from the Baltimore Hip Studies. In R. A. Fielding, C. Sieber, & B. Vellas (Eds.), Frailty Pathophysiology, Phenotype and Patient Care. Karger. https://doi.org/10.1159/000382064
Xu, B., Han, L., Liu, H., Wang, J., Bao, X. Y., Xi, H. X., et al. (2013). Cardiovascular disease and hip fracture among older inpatients in Beijing, China. BioMed Research International, 2013, 1–6. https://doi.org/10.1155/2013/493696
Forni, C., D’Alessandro, F., Gallerani, P., Genco, R., Bolzon, A., Bombino, C., et al. (2018). Effectiveness of using a new polyurethane foam multi-layer dressing in the sacral area to prevent the onset of pressure ulcer in the elderly with hip fractures: A pragmatic randomised controlled trial. International Wound Journal, 15(3), 383–390. https://doi.org/10.1111/iwj.12875
Ma, Y., Wu, X., Xiao, X., Ma, Y., Feng, L., Yan, W., et al. (2020). Effects of teriparatide versus percutaneous vertebroplasty on pain relief, quality of life and cost-effectiveness in postmenopausal females with acute osteoporotic vertebral compression fracture: A prospective cohort study. Bone, 131, 115154. https://doi.org/10.1016/j.bone.2019.115154
Mathews, N. E., Sengupta, P., & Benjamin, A. I. (2021). Effect of vitamin-D supplementation on self-perceived health-related quality of life in postmenopausal women in Ludhiana. Punjab. Indian Journal Public Health, 65(3), 294–297. https://doi.org/10.4103/ijph.IJPH_226_21
Simunovic, N., Devereaux, P. J., Sprague, S., Guyatt, G. H., Schemitsch, E., Debeer, J., et al. (2010). Effect of early surgery after hip fracture on mortality and complications: Systematic review and meta-analysis. CMAJ, 182(15), 1609–1616. https://doi.org/10.1503/cmaj.092220
Frimpong, E., Dafkin, C., Donaldson, J., Millen, A. M. E., & Meiring, R. M. (2019). The effect of home-based low-volume, high-intensity interval training on cardiorespiratory fitness, body composition and cardiometabolic health in women of normal body mass and those with overweight or obesity: protocol for a randomized controlled trial. BMC Sports Science Medicine and Rehabilitation, 11, 39. https://doi.org/10.1186/s13102-019-0152-6
Pfortmueller, C. A., Lindner, G., & Exadaktylos, A. K. (2014). Reducing fall risk in the elderly: Risk factors and fall prevention, a systematic review. Minerva Medica, 105(4), 275–281.
Acknowledgements
The authors are grateful to Hailing Guo for her help with the preparation of materials and data collection in this paper.
Funding
The authors have not disclosed any funding.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. SG and YZ contributed to materials preparation, data collection, and analysis. SG wrote the first draft of the manuscript and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gao, S., Zhao, Y. Quality of life in postmenopausal women with osteoporosis: a systematic review and meta-analysis. Qual Life Res 32, 1551–1565 (2023). https://doi.org/10.1007/s11136-022-03281-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-022-03281-1