Abstract
Purpose
To evaluate the factor structure of the revised Partners in Health (PIH) scale for measuring chronic condition self-management in a representative sample from the Australian community.
Methods
A series of consultations between clinical groups underpinned the revision of the PIH. The factors in the revised instrument were proposed to be: knowledge of illness and treatment, patient–health professional partnership, recognition and management of symptoms and coping with chronic illness. Participants (N = 904) reporting having a chronic illness completed the revised 12-item scale. Two a priori models, the 4-factor and bi-factor models were then evaluated using Bayesian confirmatory factor analysis (BCFA). Final model selection was established on model complexity, posterior predictive p values and deviance information criterion.
Results
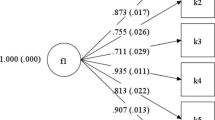
Both 4-factor and bi-factor BCFA models with small informative priors for cross-loadings provided an acceptable fit with the data. The 4-factor model was shown to provide a better and more parsimonious fit with the observed data in terms of substantive theory. McDonald’s omega coefficients indicated that the reliability of subscale raw scores was mostly in the acceptable range.
Conclusion
The findings showed that the PIH scale is a relevant and structurally valid instrument for measuring chronic condition self-management in an Australian community. The PIH scale may help health professionals to introduce the concept of self-management to their patients and provide assessment of areas of self-management. A limitation is the narrow range of validated PIH measurement properties to date. Further research is needed to evaluate other important properties such as test–retest reliability, responsiveness over time and content validity.
Similar content being viewed by others
References
Goldman, M. L., Spaeth-Rublee, B., & Pincus, H. (2015). Quality indicators for physical and behavioral health care integration. JAMA, 314(8), 769–770. doi:10.1001/jama.2015.6447.
Bauer, U. E., Briss, P. A., Goodman, R. A., & Bowman, B. A. (2014). Prevention of chronic disease in the 21st century: Elimination of the leading preventable causes of premature death and disability in the USA. The Lancet, 384(9937), 45–52.
AIHW (Australian Institute of Health and Welfare). (2012). Australia’s health 2012. Canberra: AIHW.
AIHW. (2011). Key indicators of progress for chronic disease and associated determinants: Data report. Canberra: AIHW.
Battersby, M. W., Beattie, J., Pols, R. G., Smith, D. P., Condon, J., & Blunden, S. (2013). A randomised controlled trial of the Flinders Program™ of chronic condition management in Vietnam veterans with co-morbid alcohol misuse, and psychiatric and medical conditions. Australian and New Zealand Journal of Psychiatry, 47(5), 451–462. doi:10.1177/0004867412471977.
Battersby, M., Harris, M., Smith, D., Reed, R., & Woodman, R. (2015). A pragmatic randomized controlled trial of the Flinders Program of chronic condition management in community health care services. Patient Education and Counseling, 98(11), 1367–1375.
Battersby, M. W., Kit, J. A., Prideaux, C., Harvey, P. W., Collins, J. P., & Mills, P. D. (2008). Research implementing the Flinders Model of Self-management Support with Aboriginal people who have diabetes: Findings from a pilot study. Australian Journal of Primary Health, 14(1), 66–74.
Lorig, K. R., Sobel, D. S., Ritter, P. L., Laurent, D., & Hobbs, M. (2000). Effect of a self-management program on patients with chronic disease. Effective Clinical Practice: ECP, 4(6), 256–262.
Battersby, M. W., Ask, A., Reece, M. M., Markwick, M. J., & Collins, J. P. (2003). The Partners in Health scale: The development and psychometric properties of a generic assessment scale for chronic condition self-management. Australian Journal of Primary Health, 9(3), 41–52.
Petkov, J., Harvey, P., & Battersby, M. (2010). The internal consistency and construct validity of the partners in health scale: Validation of a patient rated chronic condition self-management measure. Quality of Life Research, 19, 1079–1085.
Bodenheimer, T., Lorig, K., Holman, H., & Grumbach, K. (2002). Patient self-management of chronic disease in primary care. JAMA, 288(19), 2469–2475.
Pulvirenti, M., McMillan, J., & Lawn, S. (2014). Empowerment, patient centred care and self-management. Health Expectations, 17(3), 303–310. doi:10.1111/j.1369-7625.2011.00757.x.
Huber, M., Knottnerus, J. A., Green, L., van der Horst, H., Jadad, A. R., Kromhout, D., et al. (2011). How should we define health? BMJ (Clinical Research Edition),. doi:10.1136/bmj.d4163.
Sattoe, J. N., Bal, M. I., Roelofs, P. D., Bal, R., Miedema, H. S., & van Staa, A. (2015). Self-management interventions for young people with chronic conditions: A systematic overview. Patient Education and Counseling, 98(6), 704–715.
Laverack, G. (2009). Public health: Power, empowerment and professional practice. Basingstoke: Palgrave Macmillan.
Baum, F. (2003). The new public health (Vol. 2). Oxford: Oxford University Press.
Camerini, L., Schulz, P. J., & Nakamoto, K. (2012). Differential effects of health knowledge and health empowerment over patients’ self-management and health outcomes: A cross-sectional evaluation. Patient Education and Counseling, 89(2), 337–344.
Lawn, S., Battersby, M., & Pols, R. (2005). National chronic disease strategy—Self-management. Report to the Australian Government Department of Health and Ageing. Adelaide: Flinders Human Behaviour & Health Research Unit, Flinders University.
Barr, P. J., Scholl, I., Bravo, P., Faber, M. J., Elwyn, G., & McAllister, M. (2015). Assessment of patient empowerment—A systematic review of measures. PLoS One, 10(5), e0126553.
Bravo, P., Edwards, A., Barr, P. J., Scholl, I., Elwyn, G., & McAllister, M. (2015). Conceptualising patient empowerment: A mixed methods study. BMC Health Services Research, 15(1), 1.
McCorkle, R., Ercolano, E., Lazenby, M., Schulman-Green, D., Schilling, L. S., Lorig, K., et al. (2011). Self-management: Enabling and empowering patients living with cancer as a chronic illness. CA: A Cancer Journal for Clinicians, 61(1), 50–62. doi:10.3322/caac.20093.
Funnell, M. M., & Anderson, R. M. (2004). Empowerment and self-management of diabetes. Clinical Diabetes, 22(3), 123.
Funnell, M. M., Anderson, R. M., Arnold, M. S., Barr, P. A., Donnelly, M., Johnson, P. D., et al. (1991). Empowerment: An idea whose time has come in diabetes education. The Diabetes Educator, 17(1), 37–41.
Anderson, R. M., & Funnell, M. M. (2010). Patient empowerment: Myths and misconceptions. Patient Education and Counseling, 79(3), 277–282.
Barlow, J., Wright, C., Sheasby, J., Turner, A., & Hainsworth, J. (2002). Self-management approaches for people with chronic conditions: A review. Patient Education and Counseling, 48(2), 177–187.
Corbin, J. M., & Strauss, A. (1988). Unending work and care: Managing chronic illness at home. Los Angeles: Jossey-Bass.
Lorig, K. R., & Holman, H. R. (2003). Self-management education: History, definition, outcomes, and mechanisms. Annals of Behavioral Medicine, 26(1), 1–7.
Schulman-Green, D., Jaser, S., Martin, F., Alonzo, A., Grey, M., McCorkle, R., et al. (2012). Processes of self-management in chronic illness. Journal of Nursing Scholarship, 44(2), 136–144.
Maxine, A. (2006). Spirituality and quality of life in chronic illness. Journal of Theory Construction & Testing, 10(2), 42.
Rowe, M. M., & Allen, R. G. (2003). Spirituality as a means of coping with chronic illness. American Journal of Health Studies, 19(1), 62–66.
Zinnbauer, B. J., Pargament, K. I., & Scott, A. B. (1999). The emerging meanings of religiousness and spirituality: Problems and prospects. Journal of Personality, 67(6), 889–919.
Peterman, A. H., Fitchett, G., Brady, M. J., Hernandez, L., & Cella, D. (2002). Measuring spiritual well-being in people with cancer: The functional assessment of chronic illness therapy—Spiritual Well-being Scale (FACIT-Sp). Annals of Behavioral Medicine, 24(1), 49–58.
Elwyn, G., Lloyd, A., May, C., van der Weijden, T., Stiggelbout, A., Edwards, A., et al. (2014). Collaborative deliberation: A model for patient care. Patient Education and Counseling, 97(2), 158–164.
Kon, A. A. (2010). The shared decision-making continuum. JAMA, 304(8), 903–904.
Scholl, I., Koelewijn-van Loon, M., Sepucha, K., Elwyn, G., Légaré, F., Härter, M., et al. (2011). Measurement of shared decision making—A review of instruments. Zeitschrift für Evidenz, Fortbildung und Qualität im Gesundheitswesen, 105(4), 313–324.
Barry, M. J., & Edgman-Levitan, S. (2012). Shared decision making—the pinnacle of patient-centered care. New England Journal of Medicine, 366(9), 780–781.
Makoul, G., & Clayman, M. L. (2006). An integrative model of shared decision making in medical encounters. Patient Education and Counseling, 60(3), 301–312.
Singh, S., Butow, P., Charles, M., & Tattersall, M. H. (2010). Shared decision making in oncology: Assessing oncologist behaviour in consultations in which adjuvant therapy is considered after primary surgical treatment. Health Expectations, 13(3), 244–257.
Lawn, S., Delany, T., Sweet, L., Battersby, M., & C Skinner, T. (2014). Control in chronic condition self-care management: How it occurs in the health worker–client relationship and implications for client empowerment. Journal of Advanced Nursing, 70(2), 383–394.
Wilson, D., Wakefield, M., & Taylor, A. (1992). The South Australian health omnibus survey. Health Promotion Journal of Australia, 2(3), 47–49.
Australian Bureau of Statisitcs (2015). ASGS fact sheets: Statistical area level 1—Fact sheet. http://www.abs.gov.au/geography. Accessed 26 July 2015.
Lawn, S., & Battersby, M. (2009). Skills for person-centered care—health professionals supporting chronic condition prevention and self-management. In H. M. D’Cruz, S. W. Jacobs, & A. Schoo (Eds.), Knowledge-in-practice in the caring professions: Multi-disciplinary perspectives (pp. 161–192). Surrey: Ashgate.
Chen, F. F., West, S. G., & Sousa, K. H. (2006). A comparison of bifactor and second-order models of quality of life. Multivariate Behavioral Research, 41(2), 189–225.
Muthen, B., & Satorra, A. (1995). Complex sample data in structural equation modeling. Sociological Methodology, 25, 267–316.
Wu, J.-Y., & Kwok, O.-M. (2012). Using SEM to analyze complex survey data: A comparison between design-based single-level and model-based multilevel approaches. Structural Equation Modeling: A Multidisciplinary Journal, 19(1), 16–35.
Muthén, B., & Asparouhov, T. (2012). Bayesian structural equation modeling: A more flexible representation of substantive theory. Psychological Methods, 17(3), 313.
Muthén, L. K., & Muthén, B. O. (1998–2015). Mplus User’s guide. Los Angeles, CA: Muthén & Muthén.
Asparouhov, T., Muthén, B., & Morin, A. J. (2015). Bayesian structural equation modeling with cross-loadings and residual covariances: Comments on Stromeyer et al. Journal of Management, 41(6), 1561–1577.
Geldhof, G. J., Preacher, K. J., & Zyphur, M. J. (2014). Reliability estimation in a multilevel confirmatory factor analysis framework. Psychological Methods, 19(1), 72.
Terwee, C. B., Bot, S. D. M., de Boer, M. R., van der Windt, D. A., Knol, D. L., Dekker, J., et al. (2007). Quality criteria were proposed for measurement properties of health status questionnaires. Journal of Clinical Epidemiology, 60(1), 34–42.
Cohen, J. (1992). A power primer. Psychological Bulletin, 112(1), 155.
Warwick, M., Gallagher, R., Chenoweth, L., & Stein-Parbury, J. (2010). Self-management and symptom monitoring among older adults with chronic obstructive pulmonary disease. Journal of Advanced Nursing, 66(4), 784–793.
Kit, J. A. (2003). Chronic disease self-management in Aboriginal communities: Towards a sustainable program of care in rural communities. Australian Journal of Primary Health, 9(3), 168–176.
Gallagher, R., Donoghue, J., Chenoweth, L., & Stein-Parbury, J. (2008). Self-management in older patients with chronic illness. International Journal of Nursing Practice, 14(5), 373–382.
Walters, J., Cameron-Tucker, H., Wills, K., Schüz, N., Scott, J., Robinson, A., et al. (2013). Effects of telephone health mentoring in community-recruited chronic obstructive pulmonary disease on self-management capacity, quality of life and psychological morbidity: A randomised controlled trial. BMJ Open, 3(9), e003097.
Heijmans, M., Waverijn, G., Rademakers, J., van der Vaart, R., & Rijken, M. (2015). Functional, communicative and critical health literacy of chronic disease patients and their importance for self-management. Patient Education and Counseling, 98(1), 41–48.
Kline, R. B. (2011). Principles and practice of structural equation modeling (3rd ed.). New York: The Guilford Press.
Kenny, D. A., & McCoach, D. B. (2003). Effect of the number of variables on measures of fit in structural equation modeling. Structural Equation Modeling, 10(3), 333–351.
Bruyneel, L., Li, B., Squires, A., Spotbeen, S., Meuleman, B., Lesaffre, E., et al. (2014). Bayesian multilevel MIMIC Modeling for studying measurement invariance in cross-group comparisons. Medical Care. doi:10.1097/MLR.0000000000000164.
Mokkink, L. B., Terwee, C. B., Patrick, D. L., Alonso, J., Stratford, P. W., Knol, D. L., et al. (2010). The COSMIN checklist for assessing the methodological quality of studies on measurement properties of health status measurement instruments: An international Delphi study. Quality of Life Research, 19(4), 539–549.
Haynes, S. N., Richard, D., & Kubany, E. S. (1995). Content validity in psychological assessment: A functional approach to concepts and methods. Psychological Assessment, 7(3), 238.
Lawshe, C. H. (1975). A quantitative approach to content validity. Personnel Psychology, 28(4), 563–575.
Wilson, F. R., Pan, W., & Schumsky, D. A. (2012). Recalculation of the critical values for Lawshe’s content validity ratio. Measurement and Evaluation in Counseling and Development, 45(3), 197–210.
Vandenberg, R. J., & Lance, C. E. (2000). A review and synthesis of the measurement invariance literature: Suggestions, practices, and recommendations for organizational research. Organizational Research Methods, 3(1), 4–70.
Marsh, H. W., Morin, A. J., Parker, P. D., & Kaur, G. (2014). Exploratory structural equation modeling: An integration of the best features of exploratory and confirmatory factor analysis. Annual Review of Clinical Psychology, 10, 85–110.
Acknowledgments
The authors would like to thank the reviewers for their detailed and helpful comments to the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
As the developer of the Partners in Health (PIH) scale, Author MB has a potential conflict of interest. He has no commercial interests in the PIH.
Ethical approval
The study was approved by the University of Adelaide Human Research Ethics and was performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed consent
The study used a cross-sectional population-based survey methodology and did not require formal written consent. All data were de-identified.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Smith, D., Harvey, P., Lawn, S. et al. Measuring chronic condition self-management in an Australian community: factor structure of the revised Partners in Health (PIH) scale. Qual Life Res 26, 149–159 (2017). https://doi.org/10.1007/s11136-016-1368-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-016-1368-5