Abstract
Purpose
To examine the general health status and health-related quality of life (HRQOL) along the diabetes continuum of middle-aged and older Finns, and to determine the glucose metabolism stage by which the HRQOL has decreased noticeably.
Methods
The cross-sectional sample consisted of 920 persons aged 51–75 from the general population in a single municipality in a rural area of Eastern Finland. Data were adjusted for age, sex, smoking history, current alcohol consumption, employment and marital status. The HRQOL and health status were evaluated using two preference-based HRQOL instruments, 15D and SF-6D, and one health profile instrument, 36-Item Short Form Health Survey (SF-36).
Results
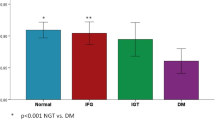
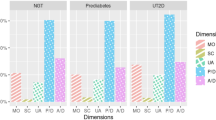
Individuals with impaired glucose tolerance (IGT) and type 2 diabetes had noticeably low mean SF-6D, 15D and general health status. The decrease in overall HRQOL was mainly due to a decline in the physical dimensions of HRQOL. The adjusted odds ratios (95 % CI) for having noticeably low HRQOL on SF-6D, 15D and general health dimension of SF-36 associated with IGT were 1.95 (1.18–3.25), 1.35 (0.84–2.18) and 2.00 (1.21–3.29), respectively.
Conclusions
The progression along the diabetes continuum was significantly associated with a decrease in HRQOL and health status. Furthermore, the data indicate that when a person is detected to have IGT, the HRQOL and general health status have already diminished noticeably. The prevailing evidence suggests that detection and intervention before a patient develops IGT is essential in order to minimize the loss of quality of life and quality-adjusted life years.


Similar content being viewed by others
Abbreviations
- BDI:
-
Becks Depression Inventory-scale
- HRQOL:
-
Health-related quality of life
- ICD-10:
-
International classification of diseases, 10th revision
- IFG:
-
Increased fasting glucose
- IGM:
-
Impaired glucose metabolism
- IGT:
-
Impaired glucose tolerance
- MID:
-
Minimally important difference
- NDM:
-
Newly diagnosed type 2 diabetes
- OGTT:
-
Oral glucose tolerance test
- QALY:
-
Quality-adjusted life year
References
Sikdar, K. C., Wang, P. P., MacDonald, D., & Gadag, V. G. (2010). Diabetes and its impact on health-related quality of life: A life table analysis. Quality of Life Research, 19, 781–787.
Williams, E. D., Rawal, L., Oldenburg, B. F., Renwick, C., Shaw, J. E., & Tapp, R. J. (2012). Risk of cardiovascular and all-cause mortality: Impact of impaired health-related functioning and diabetes—The Australian diabetes, obesity and lifestyle (AusDiab) study. Diabetes Care, 35, 1067–1073.
Chittleborough, C. R., Baldock, K. L., Taylor, A. W., & Phillips, P. J. (2006). Health status assessed by the SF-36 along the diabetes continuum in an Australian population. Quality of Life Research, 15, 687–694.
Tapp, R. J., Dunstan, D. W., Phillips, P., Tonkin, A., Zimmet, P. Z., & Shaw, J. E. (2006). Association between impaired glucose metabolism and quality of life: Results from the Australian diabetes obesity and lifestyle study. Diabetes Research and Clinical Practice, 74, 154–161.
Tapp, R. J., O’Neil, A., Shaw, J. E., Zimmet, P. Z., & Oldenburg, B. F. (2010). Is there a link between components of health-related functioning and incident impaired glucose metabolism and type 2 diabetes? The Australian diabetes obesity and lifestyle (AusDiab) study. Diabetes Care, 33, 757–762.
Seppälä, T., Saxen, U., Kautiainen, H., Järvenpää, S., & Korhonen, P. E. (2013). Impaired glucose metabolism and health related quality of life. Primary Care Diabetes, 7(3), 223–227.
Hiltunen, L., Keinänen-Kiukaanniemi, S., Läärä, E., & Kivelä, S. (1996). Self-perceived health and symptoms of elderly persons with diabetes and impaired glucose tolerance. Age and Ageing, 25, 59–66.
Hiltunen, L., & Keinänen-Kiukaanniemi, S. (1999). Does glucose tolerance affect quality of life in an elderly population? Diabetes Research and Clinical Practice, 46, 161–167.
Saramies, J. (2005). Risk factors of type 2 diabetes and screening of abnormal glucose metabolism in primary health care. Dissertation. Oulu: Faculty of Medicine, Department of Public Health Science and General Practice, University of Oulu.
Sintonen, H. (1994). The 15-D measure of health related quality of life I: Reliability, validity and sensitivity of its health state descriptive system. Melbourne: National Centre for Health Program Evaluation, Working Paper 41.
Sintonen, H. (1995). The 15-D measure of health related quality of life. II Feasibility, reliability and validity of its valuation system. Melbourne: National Centre for Health Program Evaluation, Working Paper 42.
Sintonen, H. (2001). The 15D instrument of health-related quality of life: Properties and applications. Annals of Medicine, 33(5), 328–336.
Aalto, A.-M., Aro, A. R., Teperi, J. (1999). RAND-36 as a measure of health-related quality of life. Reliability, construct validity and reference values in the Finnish general population. Helsinki: Stakes, Research Reports 101.
Hays, R. D., Sherbourne, C. D., & Mazel, R. M. (1993). The RAND 36-item health survey 1.0. Health Economics, 2, 217–227.
Jayadevappa, R., Malkowicz, S. B., Wittink, M., Wein, A. J., & Chhatre, S. (2012). Comparison of distribution- and anchor-based approaches to infer changes in health-related quality of life of prostate cancer survivors. Health Services Research, 47, 1902–1925.
Brazier, J., Usherwood, T., Harper, R., & Thomas, K. (1998). Deriving a preference-based single index from the UK SF-36 health survey. Journal of Clinical Epidemiology, 51, 1115–1128.
Brazier, J., Roberts, J., & Deverill, M. (2002). The estimation of a preference-based measure of health from the SF-36. Journal of health economics, 21, 271–292.
Brazier, J. E., & Roberts, J. (2004). The estimation of a preference-based measure of health from the SF-12. Medical Care, 42, 851–859.
Walters, S. J., & Brazier, J. E. (2005). Comparison of the minimally important difference for two health state utility measures: EQ-5D and SF-6D. Quality of Life Research, 14, 1523–1532.
Luo, N., Johnson, J. A., & Coons, S. J. (2010). Using instrument-defined health state transitions to estimate minimally important differences for four preference-based health-related quality of life instruments. Medical Care, 48, 365–371.
Ara, R., & Brazier, J. (2009). Predicting the short form-6D preference-based index using the eight mean short form-36 health dimension scores: Estimating preference-based health-related utilities when patient level data are not available. Value in Health, 12, 346–353.
Hanmer, J. (2009). Predicting an SF-6D preference-based score using MCS and PCS scores from the SF-12 or SF-36. Value in Health, 12, 958–966.
Hays, R. D., Sherbourne, C. D., Spirtzer, K. L., Dixon, W. (1996). A microcomputer program (sf36.exe) that generates SAS code for scoring the SF-36 health survey. In Proceedings of the 22nd Annual SAS Users Group International Conference 1996 (pp. 1128–1132).
World Health Organization. (2006). Definition and diagnosis of diabetes mellitus and intermediate hyperglycemia. Geneva: World Health Organization.
Elixhauser, A., Steiner, C., Harris, D. R., & Coffey, R. M. (1998). Comorbidity measures for use with administrative data. Medical Care, 36, 8–27.
Beck, A. T., Ward, C. H., Mendelson, M., et al. (1969). An inventory for measuring depression. Archives General Psychiatry, 4, 561–571.
Raitasalo, R. (2007). Mood questionnaire. Finnish modification of the short form of the Beck Depression Inventory measuring depression symptoms and self-esteem. Helsinki: The Social Insurance Institution, Finland. Studies in social security and health 86.
Beck, A. T., Steer, R. A., & Garbin, M. G. (1988). Psychometric properties of the Beck Depression Inventory: 25 years of evaluation. Clinical Psychology Review, 8, 77–100.
Väätäinen, S., Tuomilehto, H., Saramies, J., Tuomilehto, J., Uusitalo, H., Hussi, E., et al. (2013). The health-related quality-of-life impact of nocturnal awakenings in the middle-aged and older Finnish population. Quality of Life Research, 23(10), 2737–2748.
Hong, G. (2012). Marginal mean weighting through stratification: A generalized method for evaluating multivalued and multiple treatments with nonexperimental data. Psychological Methods, 17, 44–60.
O’Reilly, D. J., Xie, F., Pullenayegum, E., Gerstein, H. C., Greb, J., Blackhouse, G. K., et al. (2011). Estimation of the impact of diabetes-related complications on health utilities for patients with type 2 diabetes in Ontario, Canada. Quality of Life Research, 20, 939–943.
Tuomilehto, J., Lindström, J., Eriksson, J. G., Valle, T. T., Hamäläinen, H., Ianne-Parikka, P., et al. (2001). Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. New England Journal of Medicine, 344, 1343–1350.
Lindström, J., Peltonen, M., Eriksson, J. G., Ilanne-Parikka, P., Aunola, S., Keinänen-Kiukaanniemi, S., et al. (2012). Improved lifestyle and decreased diabetes risk over 13 years: Long-term follow-up of the randomised Finnish diabetes prevention study (DPS). Diabetologia, 56(2), 284–293.
Quan, H., Sundararajan, V., Halfon, P., Fong, A., Burnandm, B., Luthi, J-C., et al. (2005). Coding algorithms for defining comorbidities in ICD-9-CM and ICD-10 administrative data. Medical Care, 43(11), 1130–1139.
Acknowledgments
The authors wish to thank the study nurses for their valuable work in organizing and performing the examinations of the study subjects and the study subjects for their time and effort. This study was partly supported by grant from the South Karelia District of Social and Health Services.
Conflict of interest
Mr. Väätäinen declares no conflict of interest. Dr. H. Tuomilehto is a clinical specialist and founding partner of Oivauni Sleep Clinic, which provides clinical services for people with sleep disorders. Dr. Saramies, Dr. Hussi, Dr. Uusitalo and Dr. Keinänen-Kiukaanniemi declare no conflict of interest. Dr. J. Tuomilehto has received speaker’s fee from AstraZeneca, Bayer Healthcare and Novo Nordisk. Dr. Martikainen is a senior partner of ESiOR Oy, which performs studies and health economic evaluations for several pharmaceutical companies, food industry companies, medical device companies, hospitals, and academic institutions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Väätäinen, S., Keinänen-Kiukaanniemi, S., Saramies, J. et al. Quality of life along the diabetes continuum: a cross-sectional view of health-related quality of life and general health status in middle-aged and older Finns. Qual Life Res 23, 1935–1944 (2014). https://doi.org/10.1007/s11136-014-0638-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-014-0638-3