ABSTRACT
Purpose
To evaluate precipitation in and supersaturation of intestinal contents after administration of pharmacologically relevant doses of dipyridamole and ketoconazole to 12 healthy adults.
Methods
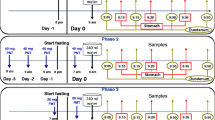
On two separate days each subject was administered in stomach 240 ml aqueous solutions of two dipyridamole doses (30/90 mg) and two ketoconazole doses (100/300 mg). Physicochemical characteristics, total drug content, and drug concentration were measured in individual intestinal contents (≤7 ml) aspirated at specific times post-dosing. Drug concentration after incubation (37°C/48 h) and equilibrium solubility were measured. Precipitate crystallinity was evaluated by x-ray powder diffraction.
Results
Precipitated fraction was minimal (dipyridamole, ≤7%) or limited (ketoconazole, ≤16%). Ketoconazole precipitates were mostly amorphous. Depending on dose, intestinal contents with pH > 3.6 were supersaturated with dipyridamole up to 10 and 30 min and with ketoconazole up to 30 and 50 min post-administration. Intestinal contents with pH > 5 and concentration of micellar components <5 mM were supersaturated with ketoconazole or dipyridamole, but precipitated fraction was significant only for ketoconazole. After incubation, crystalline precipitates were found in almost all samples. Slow precipitation of base and/or precipitation of other phases account for this observation.
Conclusions
Intralumenal precipitation of weakly alkaline, lipophilic, high permeability drugs may not be substantial. Estimating intestinal supersaturation in regard to free base is inadequate as other phases may precipitate.






Similar content being viewed by others
REFERENCES
Box KJ, Comer JE. Using measured pKa, LogP and solubility to investigate supersaturation and predict BCS class. Curr Drug Metab. 2008;9(9):869–78.
Bevernage J, Brouwers J, Clarysse S, Vertzoni M, Tack J, Annaert P, et al. Drug supersaturation in simulated and human intestinal fluids representing different nutritional states. J Pharm Sci. 2010;99(11):4525–34.
Brouwers J, Brewster ME, Augustijns P. Supersaturating drug delivery systems: the answer to solubility-limited oral bioavailability? J Pharm Sci. 2009;98(8):2549–72.
Paulekuhn GS, Dressman JB, Saal C. Trends in active pharmaceutical ingredient salt selection base on analysis of the orange book database. J Med Chem. 2007;50(26):6665–72.
Carlert S, Pålsson A, Hanisch G, von Corswant C, Nilsson C, Lindfors L, et al. Predicting intestinal precipitation-a case example for a basic BCS class II drug. Pharm Res. 2010;27(10):2119–30.
Vertzoni M, Pastelli E, Psachoulias D, Kalantzi L, Reppas C. Estimation of intragastric solubility of drugs: in what medium? Pharm Res. 2007;24(5):909–17.
National Formulary (Greek), Dipyridamole, page 138, Ketoconazole, page 330, ISBN 978-960-86876-8-4, Athens, Greece, National Drug Organization; 2007.
Kalantzi L, Persson E, Polentarutti B, Abrahamsson B, Goumas K, Dressman JB, et al. Canine intestinal contents vs. simulated media for the assessment of solubility of two weak bases in the human small intestinal contents. Pharm Res. 2006;23(6):1373–81.
Vertzoni M, Diakidou A, Chatzilias M, Söderlind E, Abrahamsson B, Dressman JB, et al. Biorelevant media to simulate fluids in the ascending colon of humans and their usefulness in predicting intracolonic drug solubility. Pharm Res. 2010;27(10):2187–96.
Vertzoni M, Archontaki H, Reppas C. Determination of intralumenal individual bile acids by HPLC with charged aerosol detection. J Lipid Res. 2008;49(12):2690–5.
Diakidou A, Vertzoni M, Goumas K, Söderlind E, Abrahamsson B, Dressman J, et al. Characterization of the contents of ascending colon to which drugs are exposed after oral administration to healthy adults. Pharm Res. 2009;26(9):2141–51.
Kalantzi L, Goumas K, Kalioras V, Abrahamsson B, Dressman JB, Reppas C. Characterization of the human upper gastrointestinal contents under conditions simulating bioavailability/bioequivalence studies. Pharm Res. 2006;23(1):165–76.
Persson EM, Gustafsson AS, Carlsson AS, Nilsson RG, Knutson L, Forsell P, et al. The effects of food on the dissolution of poorly soluble drugs in human and in model small intestinal fluids. Pharm Res. 2005;22(12):2141–51.
Mudie DM, Amidon GL, Amidon GE. Physiological parameters for oral delivery and in vitro testing. Mol Pharmaceutics. 2010;7(5):1388–405.
Brouwers J, Tack J, Lammert F, Augustijns P. Intraluminal drug and formulation behavior and integration in in vitro permeability estimation: A case study with Amprenavir. J Pharm Sci. 2006;95(2):372–83.
Clarysse S, Tack J, Lammert F, Duchateau G, Reppas C, Augustijns P. Postprandial evolution in composition and characteristics of human duodenal fluids in different nutritional states. J Pharm Sci. 2009;98(3):1177–92.
Armand M, Borel P, Pasquier B, Dubois C, Senft M, Andre M, et al. Physicochemical characteristics of emulsions during fat digestion in human stomach and duodenum. Am J Physiol. 1996;271(1 Pt 1):G172–83.
Lindahl A, Ungell AL, Knutson L, Lennernäs H. Characterization of fluids from the stomach and proximal jejunum in men and women. Pharm Res. 1997;14(4):497–502.
Clarysse S, Psachoulias D, Brouwers J, Tack J, Annaert P, Duchateau G, et al. Postprandial changes in solubilizing capacity of human intestinal fluids for BCS class II drugs. Pharm Res. 2009;26(6):1456–66.
Tian F, Zhang F, Sandler N, Gordon KC, McGoverin CM, Strachan CJ, et al. Influence of sample characteristics on quantification of carbamazepine hydrate formation by X-ray powder diffraction and Raman spectroscopy. Eur J Pharm Biopharm. 2007;66(3):466–74.
Shono Y, Jantratid E, Dressman JB. Precipitation in the small intestine may play a more important role in the in vivo performance of poorly soluble weak bases in the fasted state: case example nelfinavir. Eur J Pharm Biopharm. 2011. doi:10.1016/j.ejpb.2011.04.005.
Petrova RI, Peresypkin A, Mortko CJ, McKeown AE, Lee J, Williams JM. Rapid conversion of API hydrates to anhydrous forms in aqueous media. J Pharm Sci. 2009;98(11):4111–8.
Buchanan CM, Buchanan NL, Edgar KJ, Ramsey MG. Solubility and dissolution studies of antifungal drug: hydroxybutenyl-β-cyclodextrin complexes. Cellulose. 2007;14(1):35–47.
Kostewicz ES, Wunderlich M, Brauns U, Becker R, Bock T, Dressman JB. Predicting the precipitation of poorly soluble weak bases upon entry in the small intestine. J Pharm Pharmacol. 2004;56(1):43–51.
Gu CH, Rao D, Gandhi RB, Hilden J, Raghavan K. Using a novel multicompartment dissolution system to predict the effect of gastric pH on the oral absorption of weak bases with poor intrinsic solubility. J Pharm Sci. 2005;94(1):199–208.
ACKNOWLEDGMENTS & DISCLOSURES
Part of this work was presented at the AAPS Annual Meeting in New Orleans, 2010.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Psachoulias, D., Vertzoni, M., Goumas, K. et al. Precipitation in and Supersaturation of Contents of the Upper Small Intestine After Administration of Two Weak Bases to Fasted Adults. Pharm Res 28, 3145–3158 (2011). https://doi.org/10.1007/s11095-011-0506-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-011-0506-6