Abstract
Purpose
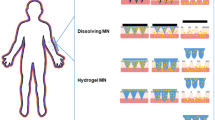
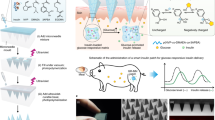
Good glycaemic control is essential to minimize the risk for diabetes-induced complications. Also, compliance is likely to be higher if the procedure is simple and painless. This study was designed to validate painless intradermal delivery via a patch-like microneedle array.
Materials and Methods
Diabetes was induced by an intravenous injection of streptozotocin (50 mg/kg bw) in adult male Sprague Dawley rats. Plasma insulin and blood glucose were measured before, during and after subcutaneous or intradermal (microneedles) infusion of insulin (0.2 IU/h) under Inactin-anaesthesia.
Results
Before insulin administration, all animals displayed a pronounced hyperglycaemia (19 ± 1 mM; 359 mg/dl). Administration of insulin resulted in a reduced plasma glucose independently of administration route (subcutaneous 7.5 ± 4.2, n = 9, and intradermal 11 ± 1.8, n = 9 after 240 min), but with less errors of the mean in the intradermal group. In the intradermal group, plasma insulin was increased in all latter measurements (72 ± 22, 81 ± 34, and 87 ± 20 μIU/ml), as compared to the first measurement (26 ± 13). In the subcutaneous group, plasma insulin was elevated during the last measurement (to 154 ± 3.5 μIU/ml from 21 ± 18).
Conclusion
This study presents a novel possibility of insulin delivery that is controllable and requires minimal training. This treatment strategy could improve compliance, and thus be beneficial for patients’ glycaemic control.









Similar content being viewed by others
References
The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. The Diabetes Control and Complications Trial Research Group. N. Engl. J. Med. 329: 977–986 (1993).
N. Sulliand and B. Shashaj. Long-term benefits of continuous subcutaneous insulin infusion in children with Type 1 diabetes: a 4-year follow-up. Diabet. Med. 23:900–906 (2006).
M. Korytkowski, L. Niskanen, and T. Asakura. FlexPen: Addressing issues of confidence and convenience in insulin delivery. Clin. Ther. 27(Suppl B):S89–S100 (2005).
D. R. Owens, B. Zinman, and G. Bolli. Alternative routes of insulin delivery. Diabet. Med. 20:886–898 (2003).
M. Davies. The reality of glycaemic control in insulin treated diabetes: defining the clinical challenges. Int. J. Obes. Relat. Metab. Disord. 28(Suppl 2):S14–S22 (2004).
N. H. Birkebaek, A. Johansen, and J. Solvig. Cutis/subcutis thickness at insulin injection sites and localization of simulated insulin boluses in children with type 1 diabetes mellitus: need for individualization of injection technique? Diabet. Med. 15:965–971 (1998).
M. Korytkowski, D. Bell, C. Jacobsen, and R. Suwannasari. A multicenter, randomized, open-label, comparative, two-period crossover trial of preference, efficacy, and safety profiles of a prefilled, disposable pen and conventional vial/syringe for insulin injection in patients with type 1 or 2 diabetes mellitus. Clin. Ther. 25:2836–2848 (2003).
A. H. Barnett. Exubera inhaled insulin: a review. Int. J. Clin. Pract. 58:394–401 (2004).
T. C. Woods, B. Zhang, F. Mercogliano, and S. M. Dinh. Response of the lung to pulmonary insulin dosing in the rat model and effects of changes in formulation. Diabetes Technol. Ther. 7:516–524 (2005).
T. K. Mandal. Inhaled insulin for diabetes mellitus. Am. J. Health Syst. Pharm. 62:1359–1364 (2005).
M. R. Prausnitz. Overcoming skin’s barrier: The search for effective and user-friendly drug delivery. Diabetes Technol. Ther. 3:233–236 (2001).
M. A. Teo, C. Shearwood, K. C. Ng, J. Lu, and S. Moochhala. In vitro and in vivo characterization of MEMS microneedles. Biomed Microdevices 7:47–52 (2005).
S. Kaushik, A. H. Hord, D. D. Denson, D. V. McAllister, S. Smitra, M. G. Allen, and M. R. Prausnitz. Lack of pain associated with microfabricated microneedles. Anesth. Analg. 92:502–504 (2001).
A. Junod, A. E. Lambert, W. Stauffacher, and A. E. Renold. Diabetogenic action of streptozotocin: relationship of dose to metabolic response. J. Clin. Invest. 48:2129–2139 (1969).
M. Madou. Fundamentals of Microfabrication, CRC, (1997).
N. Roxhed, P. Griss, and G. Stemme. Reliable in-vivo penetration and transdermal injection using ultra-sharp hollow microneedles. In Proceedings IEEE International Conference on Solid State Sensors, Actuators, and Microsystems (Transducers), vol. 1, IEEE, Seoul, Korea, 2005, pp. 213–216.
N. Roxhed, B. Samel, L. Nordquist, P. Griss, and G. Stemme. Compact, Seamless Integration of Active Dosing and Actuation with Microneedles for Transdermal Drug Delivery. In IEEE International Conference on Micro Electro Mechanical Systems (MEMS), 2006, pp. 414–417.
D. C. Howey, R. R. Bowsher, R. L. Brunelle, H. M. Rowe, P. F. Santa, J. Downing-Shelton, and J. R. Woodworth. [Lys(B28), Pro(B29)]-human insulin: effect of injection time on postprandial glycemia. Clin. Pharmacol. Ther. 58:459–469 (1995).
W. Martanto, S. P. Davis, N. R. Holiday, J. Wang, H. S. Gill, and M. R. Prausnitz. Transdermal delivery of insulin using microneedles in vivo. Pharm. Res. 21:947–952 (2004).
D. V. McAllister, P. M. Wang, S. P. Davis, J. H. Park, P. J. Canatella, M. G. Allen, and M. R. Prausnitz. Microfabricated needles for transdermal delivery of macromolecules and nanoparticles: fabrication methods and transport studies. Proc. Natl. Acad. Sci. U. S. A. 100:13755–13760 (2003).
S. P. Davis, B. J. Landis, Z. H. Adams, M. G. Allen, and M. R. Prausnitz. Insertion of microneedles into skin: measurement and prediction of insertion force and needle fracture force. J. Biomech. 37:1155–1163 (2004).
P. Griss, and G. Stemme. Side-opened out-of-plane microneedles for microfluidic transdermal liquid transfer. IEEE ASME J. Microelectromech. Syst. 12:296–301 (2003).
H. J. G. E. Gardeniers, R. Luttge, E. J. W. Berenschot, M. J. de Boer, S. Y. Yeshurun, M. Hefetz, R. van’t Oever, and A. van den Berg. Silicon micromachined hollow microneedles for transdermal liquid transport. IEEE ASME J. Microelectromech. Syst. 12:855–862 (2003).
P. M. Wang, M. Cornwell, J. Hill, and M. R. Prausnitz. Precise microinjection into skin using hollow microneedles. J. Invest. Dermatol. 126:1080–1087 (2006).
W. Martanto, J. S. Moore, O. Kashlan, R. Kamath, P. M. Wang, J. M. O’Neal, and M. R. Prausnitz. Microinfusion using hollow microneedles. Pharm. Res. 23: 104–113 (2006).
R. K. Sivamani, B. Stoeber, G. C. Wu, H. Zhai, D. Liepmann, and H. Maibach. Clinical microneedle injection of methyl nicotinate: stratum corneum penetration. Skin Res. Technol. 11:152–156 (2005).
M. Meurer, M. Stumvoll, and R. M. Szeimies. [Skin changes in diabetes mellitus]. Hautarzt 55:428–435 (2004).
S. P. Davis, W. Martanto, M. G. Allen, and M. R. Prausnitz. Hollow metal microneedles for insulin delivery to diabetic rats. IEEE Trans. Biomed. Eng. 52:909–915 (2005).
W. Waldhausland, and P. Bratusch-Marrain. [Causes of insulin resistance in type 1 diabetes]. Wien. Klin. Wochenschr. 97:359–363 (1985).
H. Wiig, O. Tenstad, and J. L. Bert. Effect of hydration on interstitial distribution of charged albumin in rat dermis in vitro. J. Physiol. 569:631–641 (2005).
R. K. Reed, S. Lepsoe, and H. Wiig. Interstitial exclusion of albumin in rat dermis and subcutis in over- and dehydration. Am. J. Physiol. 257:H1819–H1827 (1989).
J. Berger, C. Biswas, P. P. Vicario, H. V. Strout, R. Saperstein, and P. F. Pilch. Decreased expression of the insulin-responsive glucose transporter in diabetes and fasting. Nature 340:70–72 (1989).
E. Karnieli, P. J. Hissin, I. A. Simpson, L. B. Salans, and S. W. Cushman. A possible mechanism of insulin resistance in the rat adipose cell in streptozotocin-induced diabetes mellitus. Depletion of intracellular glucose transport systems. J. Clin. Invest. 68:811–814 (1981).
G. Lisato, I. Cusin, A. Tiengo, S. Del Prato, and B. Jeanrenaud. The contribution of hyperglycaemia and hypoinsulinaemia to the insulin resistance of streptozotocin-diabetic rats. Diabetologia 35:310–315 (1992).
W. Martanto, J. S. Moore, T. Couse, and M. R. Prausnitz. Mechanism of fluid infusion during microneedle insertion and retraction. J. Control. Release (2006).
R. J. Heine. Unlocking the opportunity of tight glycaemic control. Promise ahead: the role of inhaled insulin in clinical practice. Diabetes Obes. Metab. 7(Suppl 1):S19–S23 (2005).
E. V. Mukerjee, S. D. Collins, R. R. Isseroff, and R. L. Smith. Microneedle array for transdermal biological fluid extraction and in situ analysis. Sens. Actuators A, Phys. A114:267–275 (2004).
J. A. Matriano, M. Cormier, J. Johnson, W. A. Young, M. Buttery, K. Nyam, and P. E. Daddona. Macroflux microprojection array patch technology: a new and efficient approach for intracutaneous immunization. Pharm. Res. 19:63–70 (2002).
W. Lin, M. Cormier, A. Samiee, A. Griffin, B. Johnson, C. L. Teng, G. E. Hardee, and P. E. Daddona. Transdermal delivery of antisense oligonucleotides with microprojection patch (Macroflux) technology. Pharm. Res. 18:1789–1793 (2001).
S. A. Coulman, D. Barrow, A. Anstey, C. Gateley, A. Morrissey, N. Wilke, C. Allender, K. Brain, and J. C. Birchall. Minimally invasive cutaneous delivery of macromolecules and plasmid DNA via microneedles. Curr. Drug. Deliv. 3:65–75 (2006).
J. A. Mikszta, J. B. Alarcon, J. M. Brittingham, D. E. Sutter, R. J. Pettis, and N. G. Harvey. Improved genetic immunization via micromechanical disruption of skin-barrier function and targeted epidermal delivery. Nat. Med. 8:415–419 (2002).
M. Cormier, B. Johnson, M. Ameri, K. Nyam, L. Libiran, D. D. Zhang, and P. Daddona. Transdermal delivery of desmopressin using a coated microneedle array patch system. J. Control. Release 97:503–511 (2004).
Acknowledgements
The sharp-minded and kind-hearted help and support from Professor Leif Jansson is gratefully acknowledged. This work was funded by the Swedish Foundation for Strategic Research (SFF), the Swedish Association of Nephrology, the Petersenska Hemmet Foundation, and the Scandinavian Physiological Society.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nordquist, L., Roxhed, N., Griss, P. et al. Novel Microneedle Patches for Active Insulin Delivery are Efficient in Maintaining Glycaemic Control: An Initial Comparison with Subcutaneous Administration. Pharm Res 24, 1381–1388 (2007). https://doi.org/10.1007/s11095-007-9256-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-007-9256-x