Abstract
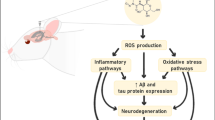
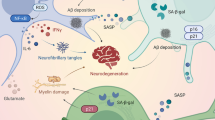
Curcumin has been reported to have a therapeutic effect on Alzheimer’s disease (AD), but the specific mechanism remains to be elucidated. In the present research, we aimed to investigate the effect and molecular mechanism of curcumin on AD. Mouse primary hippocampal neuron cells were treated with various concentrations of beta-amyloid 42 (Aβ42) and the results found that Aβ42 inhibited cell viability in a dose-dependent manner. Compared with 50 ng/mL Aβ42, 500 ng/mL Aβ42 could further promote cell apoptosis, reduce the ratio of Nicotinamide adenine dinucleotide (NAD(+))/Nicotinamide adenine diphosphate hydride (NADH) and Adenosine 5′-triphosphate (ATP) level, and inhibit Sirtuins 3 (SIRT3) deacetylation activity and protein expression of Thyroid hormone receptor beta (Thrb) and SIRT3. Hence, 500 ng/mL Aβ42 was used to establish a cell model of AD. Curcumin significantly reversed the inhibitory effects of Aβ42 on cell viability, SIRT3 deacetylation activity, the ratio of NAD+/NADH, ATP level and the protein expression of Thrb and SIRT3, and the promotive effect on apoptosis. ChIPBase was used to predict the binding region of Thrb and SIRT3. Dual luciferase reporter gene and Chromatin immune precipitation (ChIP) assays were employed to verify the relationship between Thrb and promoter of SIRT3 mRNA. Overexpression of Thrb recovered Aβ42 induced metabolic dysfunction, while Thrb silence aggravated Aβ42 induced metabolic dysfunction. Moreover, Thrb silence or 3-TYP (a selective inhibitor of SIRT3) treatment abolished the amelioration of curcumin on Aβ42 induced metabolic dysfunction. Additionally, curcumin attenuated memory deficits in Amyloid precursor protein transgenic (APPTG) mice. Collectively, curcumin alleviated Aβ42-induced neuronal metabolic dysfunction through increasing Thrb expression and SIRT3 activity and improved cognition in APPTG mice.






Similar content being viewed by others
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Bondi MW, Edmonds EC, Salmon DP (2017) Alzheimer’s disease: past, present, and future. J Int Neuropsychol Soc 23:818–831. https://doi.org/10.1017/s135561771700100x
Rabbito A, Dulewicz M, Kulczyńska-Przybik A, Mroczko B (2020) Biochemical markers in Alzheimer’s disease. Int J Mol Sci. https://doi.org/10.3390/ijms21061989
Soria Lopez JA, González HM, Léger GC (2019) Alzheimer’s disease. Handb Clin Neurol 167:231–255. https://doi.org/10.1016/b978-0-12-804766-8.00013-3
Oboudiyat C, Glazer H, Seifan A, Greer C, Isaacson RS (2013) Alzheimer’s disease. Semin Neurol 33:313–329. https://doi.org/10.1055/s-0033-1359319
Tiwari S, Atluri V, Kaushik A, Yndart A, Nair M (2019) Alzheimer’s disease: pathogenesis, diagnostics, and therapeutics. Int J Nanomed 14:5541–5554. https://doi.org/10.2147/ijn.s200490
Czech C, Tremp G, Pradier L (2000) Presenilins and Alzheimer’s disease: biological functions and pathogenic mechanisms. Prog Neurobiol 60:363–384. https://doi.org/10.1016/s0301-0082(99)00033-7
Teunissen CE, Chiu MJ, Yang CC, Yang SY, Scheltens P, Zetterberg H, Blennow K (2018) Plasma amyloid-β (Aβ42) correlates with cerebrospinal fluid Aβ42 in Alzheimer’s disease. J Alzheimer’s Dis 62:1857–1863. https://doi.org/10.3233/jad-170784
Li W, Wu Y, Min F, Li Z, Huang J, Huang R (2010) A nonhuman primate model of Alzheimer’s disease generated by intracranial injection of amyloid-β42 and thiorphan. Metab Brain Dis 25:277–284. https://doi.org/10.1007/s11011-010-9207-9
Yin P, Wang X, Wang S, Wei Y, Feng J, Zhu M (2019) Maresin 1 improves cognitive decline and ameliorates inflammation in a mouse model of Alzheimer’s disease. Front Cell Neurosci 13:466. https://doi.org/10.3389/fncel.2019.00466
Anyetei-Anum CS, Roggero VR, Allison LA (2018) Thyroid hormone receptor localization in target tissues. J Endocrinol 237:R19-r34. https://doi.org/10.1530/joe-17-0708
van Gucht ALM, Moran C, Meima ME, Visser WE, Chatterjee K, Visser TJ, Peeters RP (2017) Resistance to thyroid hormone due to heterozygous mutations in thyroid hormone receptor alpha. Curr Top Dev Biol 125:337–355. https://doi.org/10.1016/bs.ctdb.2017.02.001
Zhou Z, Yang C, Lv F, Liu W, Yan S, Zang H, Li M, Wang F, Zang Y, Liu S (2018) Novel THRB mutation analysis in congenital hypothyroidism with thyroid dysgenesis. J Cell Biochem 119:9474–9482. https://doi.org/10.1002/jcb.27264
Choi HJ, Byun MS, Yi D, Sohn BK, Lee JH, Lee JY, Kim YK, Lee DY (2017) Associations of thyroid hormone serum levels with in-vivo Alzheimer’s disease pathologies. Alzheimer’s Res Ther 9:64. https://doi.org/10.1186/s13195-017-0291-5
Tan ZS, Vasan RS (2009) Thyroid function and Alzheimer’s disease. J Alzheimer’s Dis 16:503–507. https://doi.org/10.3233/jad-2009-0991
Belakavadi M, Dell J, Grover GJ, Fondell JD (2011) Thyroid hormone suppression of β-amyloid precursor protein gene expression in the brain involves multiple epigenetic regulatory events. Mol Cell Endocrinol 339:72–80. https://doi.org/10.1016/j.mce.2011.03.016
Shi H, Deng HX, Gius D, Schumacker PT, Surmeier DJ, Ma YC (2017) Sirt3 protects dopaminergic neurons from mitochondrial oxidative stress. Hum Mol Genet 26:1915–1926. https://doi.org/10.1093/hmg/ddx100
Jing E, Emanuelli B, Hirschey MD, Boucher J, Lee KY, Lombard D, Verdin EM, Kahn CR (2011) Sirtuin-3 (Sirt3) regulates skeletal muscle metabolism and insulin signaling via altered mitochondrial oxidation and reactive oxygen species production. Proc Natl Acad Sci U S A 108:14608–14613. https://doi.org/10.1073/pnas.1111308108
Marfe G, Tafani M, Indelicato M, Sinibaldi-Salimei P, Reali V, Pucci B, Fini M, Russo MA (2009) Kaempferol induces apoptosis in two different cell lines via Akt inactivation, Bax and SIRT3 activation, and mitochondrial dysfunction. J Cell Biochem 106:643–650. https://doi.org/10.1002/jcb.22044
Yin J, Li S, Nielsen M, Carcione T, Liang WS, Shi J (2018) Sirtuin 3 attenuates amyloid-β induced neuronal hypometabolism. Aging (Albany NY) 10:2874–2883. https://doi.org/10.18632/aging.101592
Salvatori I, Valle C, Ferri A, Carrì MT (2017) SIRT3 and mitochondrial metabolism in neurodegenerative diseases. Neurochem Int 109:184–192. https://doi.org/10.1016/j.neuint.2017.04.012
Kunnumakkara AB, Bordoloi D, Padmavathi G, Monisha J, Roy NK, Prasad S, Aggarwal BB (2017) Curcumin, the golden nutraceutical: multitargeting for multiple chronic diseases. Br J Pharmacol 174:1325–1348. https://doi.org/10.1111/bph.13621
Li L, Zhang X, Pi C, Yang H, Zheng X, Zhao L, Wei Y (2020) Review of curcumin physicochemical targeting delivery system. Int J Nanomed 15:9799–9821. https://doi.org/10.2147/ijn.s276201
Narasingappa RB, Javagal MR, Pullabhatla S, Htoo HH, Rao JK, Hernandez JF, Govitrapong P, Vincent B (2012) Activation of α-secretase by curcumin-aminoacid conjugates. Biochem Biophys Res Commun 424:691–696. https://doi.org/10.1016/j.bbrc.2012.07.010
Tiwari SK, Agarwal S, Seth B, Yadav A, Nair S, Bhatnagar P, Karmakar M, Kumari M, Chauhan LK, Patel DK, Srivastava V, Singh D, Gupta SK, Tripathi A, Chaturvedi RK, Gupta KC (2014) Curcumin-loaded nanoparticles potently induce adult neurogenesis and reverse cognitive deficits in Alzheimer’s disease model via canonical Wnt/β-catenin pathway. ACS Nano 8:76–103. https://doi.org/10.1021/nn405077y
Martín-Moreno AM, Brera B, Spuch C, Carro E, García-García L, Delgado M, Pozo MA, Innamorato NG, Cuadrado A, de Ceballos ML (2012) Prolonged oral cannabinoid administration prevents neuroinflammation, lowers β-amyloid levels and improves cognitive performance in Tg APP 2576 mice. J Neuroinflammation 9:8. https://doi.org/10.1186/1742-2094-9-8
He Y, Jiang K, Zhao X (2020) Taraxasterol protects hippocampal neurons from oxygen-glucose deprivation-induced injury through activation of Nrf2 signalling pathway. Artif Cells Nanomed Biotechnol 48:252–258. https://doi.org/10.1080/21691401.2019.1699831
Rouble AN, Storey KB (2015) Characterization of the SIRT family of NAD+-dependent protein deacetylases in the context of a mammalian model of hibernation, the thirteen-lined ground squirrel. Cryobiology 71:334–343. https://doi.org/10.1016/j.cryobiol.2015.08.009
Belkacemi A, Doggui S, Dao L, Ramassamy C (2011) Challenges associated with curcumin therapy in Alzheimer disease. Expert Rev Mol Med 13:e34. https://doi.org/10.1017/s1462399411002055
Reddy PH, Manczak M, Yin X, Grady MC, Mitchell A, Tonk S, Kuruva CS, Bhatti JS, Kandimalla R, Vijayan M, Kumar S, Wang R, Pradeepkiran JA, Ogunmokun G, Thamarai K, Quesada K, Boles A, Reddy AP (2018) Protective effects of Indian spice curcumin against amyloid-β in Alzheimer’s disease. J Alzheimer’s Dis 61:843–866. https://doi.org/10.3233/jad-170512
Olesen MA, Torres AK, Jara C, Murphy MP, Tapia-Rojas C (2020) Premature synaptic mitochondrial dysfunction in the hippocampus during aging contributes to memory loss. Redox Biol 34:101558. https://doi.org/10.1016/j.redox.2020.101558
Wu J, Zeng Z, Zhang W, Deng Z, Wan Y, Zhang Y, An S, Huang Q, Chen Z (2019) Emerging role of SIRT3 in mitochondrial dysfunction and cardiovascular diseases. Free Radic Res 53:139–149. https://doi.org/10.1080/10715762.2018.1549732
Cheng A, Wang J, Ghena N, Zhao Q, Perone I, King TM, Veech RL, Gorospe M, Wan R, Mattson MP (2020) SIRT3 haploinsufficiency aggravates loss of GABAergic interneurons and neuronal network hyperexcitability in an Alzheimer’s disease model. J Neurosci 40:694–709. https://doi.org/10.1523/jneurosci.1446-19.2019
Kim SH, Lu HF, Alano CC (2011) Neuronal Sirt3 protects against excitotoxic injury in mouse cortical neuron culture. PLoS ONE 6:e14731. https://doi.org/10.1371/journal.pone.0014731
Lee J, Kim Y, Liu T, Hwang YJ, Hyeon SJ, Im H, Lee K, Alvarez VE, McKee AC, Um SJ, Hur M, Mook-Jung I, Kowall NW, Ryu H (2018) SIRT3 deregulation is linked to mitochondrial dysfunction in Alzheimer’s disease. Aging Cell. https://doi.org/10.1111/acel.12679
Li H, Jia J, Wang W, Hou T, Tian Y, Wu Q, Xu L, Wei Y, Wang X (2018) Honokiol alleviates cognitive deficits of Alzheimer’s disease (PS1V97L) transgenic mice by activating mitochondrial SIRT3. J Alzheimer’s Dis 64:291–302. https://doi.org/10.3233/jad-180126
Satterstrom FK, Swindell WR, Laurent G, Vyas S, Bulyk ML, Haigis MC (2015) Nuclear respiratory factor 2 induces SIRT3 expression. Aging Cell 14:818–825. https://doi.org/10.1111/acel.12360
Giralt A, Hondares E, Villena JA, Ribas F, Díaz-Delfín J, Giralt M, Iglesias R, Villarroya F (2011) Peroxisome proliferator-activated receptor-gamma coactivator-1alpha controls transcription of the Sirt3 gene, an essential component of the thermogenic brown adipocyte phenotype. J Biol Chem 286:16958–16966. https://doi.org/10.1074/jbc.M110.202390
Ortiga-Carvalho TM, Sidhaye AR, Wondisford FE (2014) Thyroid hormone receptors and resistance to thyroid hormone disorders. Nat Rev Endocrinol 10:582–591. https://doi.org/10.1038/nrendo.2014.143
Jones I, Srinivas M, Ng L, Forrest D (2003) The thyroid hormone receptor beta gene: structure and functions in the brain and sensory systems. Thyroid 13:1057–1068. https://doi.org/10.1089/105072503770867228
Ng L, Rüsch A, Amma LL, Nordström K, Erway LC, Vennström B, Forrest D (2001) Suppression of the deafness and thyroid dysfunction in Thrb-null mice by an independent mutation in the Thra thyroid hormone receptor alpha gene. Hum Mol Genet 10:2701–2708. https://doi.org/10.1093/hmg/10.23.2701
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, M., Zhang, X. & Wang, Y. Curcumin Alleviates Aβ42-Induced Neuronal Metabolic Dysfunction via the Thrb/SIRT3 Axis and Improves Cognition in APPTG Mice. Neurochem Res 46, 3166–3178 (2021). https://doi.org/10.1007/s11064-021-03414-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-021-03414-x