Abstract
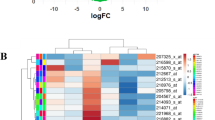
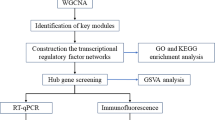
Neuroblastomas (NB) are childhood malignant tumors originating in the sympathetic nervous system. MicroRNAs (miRNAs) play an essential regulatory role in tumorigenesis and development. In this study, NB miRNA and mRNA expression profile data in the Gene Expression Omnibus database were used to screen for differentially expressed miRNAs (DEMs) and genes (DEGs). We used the miRTarBase and miRSystem databases to predict the target genes of the DEMs, and we selected target genes that overlapped with the DEGs as candidate genes for further study. Annotations, visualization, and the DAVID database were used to perform Gene Ontology (GO) and Kyoto Encyclopedia of Genes and Genomes (KEGG) enrichment analysis on the candidate genes. Additionally, the protein–protein interaction (PPI) network and miRNA–mRNA regulatory network were constructed and visualized using the STRING database and Cytoscape, and the hub modules were analyzed for function and pathway enrichment using the DAVID database and BiNGO plug-in. 107 DEMs and 1139 DEGs were identified from the miRNA and mRNA chips, respectively. 4390 overlapping target genes were identified using the two databases, and 405 candidate genes which intersected with the DEGs were selected. These candidate genes were enriched in 363 GO terms and 24 KEGG pathways. By constructing a PPI network and a miRNA–mRNA regulatory network, three hub miRNAs (hsa-miR-30e-5p, hsa-miR-15a, and hsa-miR-16) were identified. The target genes of the hub miRNAs were significantly enriched in the following pathways: microRNAs in cancer, the PI3K-Akt signaling pathway, pathways in cancer, the p53 signaling pathway, and the cell cycle. In summary, our results have identified candidate genes and pathways related to the underlying molecular mechanism of NB. These findings provide a new perspective for NB research and treatment.









Similar content being viewed by others
Data Availability
All data is available upon reasonable request.
Code Availability
Not applicable.
References
Gains JE, Sebire NJ, Moroz V, Wheatley K, Gaze MN (2018) Immunohistochemical evaluation of molecular radiotherapy target expression in neuroblastoma tissue. Eur J Nucl Med Mol Imaging 45(3):402–411. https://doi.org/10.1007/s00259-017-3856-4
Marshall GM, Carter DR, Cheung BB, Liu T, Mateos MK, Meyerowitz JG, Weiss WA (2014) The prenatal origins of cancer. Nat Rev Cancer 14(4):277–289. https://doi.org/10.1038/nrc3679
Park JR, Eggert A, Caron H (2010) Neuroblastoma: biology, prognosis, and treatment. Hematol Oncol Clin N Am 24(1):65–86. https://doi.org/10.1016/j.hoc.2009.11.011
Steliarova-Foucher E, Colombet M, Ries LAG, Moreno F, Dolya A, Bray F, Hesseling P, Shin HY, Stiller CA, contributors I (2017) International incidence of childhood cancer, 2001–10: a population-based registry study. Lancet Oncol 18(6):719–731. https://doi.org/10.1016/S1470-2045(17)30186-9
Sharp SE, Gelfand MJ, Shulkin BL (2011) Pediatrics: diagnosis of neuroblastoma. Semin Nucl Med 41(5):345–353. https://doi.org/10.1053/j.semnuclmed.2011.05.001
Southgate HED, Chen L, Curtin NJ, Tweddle DA (2020) Targeting the DNA damage response for the treatment of high risk neuroblastoma. Front Oncol 10:371. https://doi.org/10.3389/fonc.2020.00371
Casey DL, Pitter KL, Kushner BH, Cheung NV, Modak S, LaQuaglia MP, Wolden SL (2018) Radiation therapy to sites of metastatic disease as part of consolidation in high-risk neuroblastoma: can long-term control be achieved? Int J Radiat Oncol Biol Phys 100(5):1204–1209. https://doi.org/10.1016/j.ijrobp.2018.01.008
Kreissman SG, Seeger RC, Matthay KK, London WB, Sposto R, Grupp SA, Haas-Kogan DA, Laquaglia MP, Yu AL, Diller L, Buxton A, Park JR, Cohn SL, Maris JM, Reynolds CP, Villablanca JG (2013) Purged versus non-purged peripheral blood stem-cell transplantation for high-risk neuroblastoma (COG A3973): a randomised phase 3 trial. Lancet Oncol 14(10):999–1008. https://doi.org/10.1016/S1470-2045(13)70309-7
Smith MA, Seibel NL, Altekruse SF, Ries LA, Melbert DL, O’Leary M, Smith FO, Reaman GH (2010) Outcomes for children and adolescents with cancer: challenges for the twenty-first century. J Clin Oncol 28(15):2625–2634. https://doi.org/10.1200/JCO.2009.27.0421
Lewis EC, Kraveka JM, Ferguson W, Eslin D, Brown VI, Bergendahl G, Roberts W, Wada RK, Oesterheld J, Mitchell D, Foley J, Zage P, Rawwas J, Rich M, Lorenzi E, Broglio K, Berry D, Saulnier Sholler GL (2020) A subset analysis of a phase II trial evaluating the use of DFMO as maintenance therapy for high-risk neuroblastoma. Int J Cancer. https://doi.org/10.1002/ijc.33044
Irwin MS, Park JR (2015) Neuroblastoma: paradigm for precision medicine. Pediatr Clin N Am 62(1):225–256. https://doi.org/10.1016/j.pcl.2014.09.015
Olsson M, Beck S, Kogner P, Martinsson T, Caren H (2016) Genome-wide methylation profiling identifies novel methylated genes in neuroblastoma tumors. Epigenetics 11(1):74–84. https://doi.org/10.1080/15592294.2016.1138195
Parveen A, Mustafa SH, Yadav P, Kumar A (2019) Applications of machine learning in miRNA discovery and target prediction. Curr Genom 20(8):537–544. https://doi.org/10.2174/1389202921666200106111813
Chen W, Gao C, Liu Y, Wen Y, Hong X, Huang Z (2020) Bioinformatics analysis of prognostic miRNA signature and potential critical genes in colon cancer. Front Genet 11:478. https://doi.org/10.3389/fgene.2020.00478
Bartel DP (2018) Metazoan microRNAs. Cell 173(1):20–51. https://doi.org/10.1016/j.cell.2018.03.006
Huntzinger E, Izaurralde E (2011) Gene silencing by microRNAs: contributions of translational repression and mRNA decay. Nat Rev Genet 12(2):99–110. https://doi.org/10.1038/nrg2936
Pottoo FH, Barkat MA, Harshita AMA, Javed MN, Sajid Jamal QM, Kamal MA (2019) Nanotechnological based miRNA intervention in the therapeutic management of neuroblastoma. Semin Cancer Biol. https://doi.org/10.1016/j.semcancer.2019.09.017
Schmittgen TD (2019) Exosomal miRNA cargo as mediator of immune escape mechanisms in neuroblastoma. Cancer Res 79(7):1293–1294. https://doi.org/10.1158/0008-5472.CAN-19-0021
De Preter K, Mestdagh P, Vermeulen J, Zeka F, Naranjo A, Bray I, Castel V, Chen C, Drozynska E, Eggert A, Hogarty MD, Izycka-Swieszewska E, London WB, Noguera R, Piqueras M, Bryan K, Schowe B, van Sluis P, Molenaar JJ, Schramm A, Schulte JH, Stallings RL, Versteeg R, Laureys G, Van Roy N, Speleman F, Vandesompele J (2011) miRNA expression profiling enables risk stratification in archived and fresh neuroblastoma tumor samples. Clin Cancer Res 17(24):7684–7692. https://doi.org/10.1158/1078-0432.CCR-11-0610
Yang C, Dou R, Yin T, Ding J (2020) MiRNA-106b-5p in human cancers: diverse functions and promising biomarker. Biomed Pharmacother 127:110211. https://doi.org/10.1016/j.biopha.2020.110211
Ramassone A, Pagotto S, Veronese A, Visone R (2018) Epigenetics and microRNAs in cancer. Int J Mol Sci 19(2):285–294. https://doi.org/10.3390/ijms19020459
Qu H, Zheng L, Pu J, Mei H, Xiang X, Zhao X, Li D, Li S, Mao L, Huang K, Tong Q (2015) miRNA-558 promotes tumorigenesis and aggressiveness of neuroblastoma cells through activating the transcription of heparanase. Hum Mol Genet 24(9):2539–2551. https://doi.org/10.1093/hmg/ddv018
Cao XY, Sun ZY, Zhang LJ, Chen MK, Yuan B (2019) microRNA-144-3p suppresses human neuroblastoma cell proliferation by targeting HOXA7. Eur Rev Med Pharmacol Sci 23(2):716–723. https://doi.org/10.26355/eurrev_201901_16885
Cheng X, Xu Q, Zhang Y, Shen M, Zhang S, Mao F, Li B, Yan X, Shi Z, Wang L, Sheng G, Zhang Q (2019) miR-34a inhibits progression of neuroblastoma by targeting autophagy-related gene 5. Eur J Pharmacol 850:53–63. https://doi.org/10.1016/j.ejphar.2019.01.071
Li Z, Chen H (2019) miR-34a inhibits proliferation, migration and invasion of paediatric neuroblastoma cells via targeting HNF4alpha. Artif Cells Nanomed Biotechnol 47(1):3072–3078. https://doi.org/10.1080/21691401.2019.1637886
Wan MF, Yang N, Qu NY, Pan YY, Shan YQ, Li P (2020) MiR-424 suppressed viability and invasion by targeting to the DCLK1 in neuroblastoma. Eur Rev Med Pharmacol Sci 24(10):5526–5533. https://doi.org/10.26355/eurrev_202005_21338
Mao F, Zhang J, Cheng X, Xu Q (2019) miR-149 inhibits cell proliferation and enhances chemosensitivity by targeting CDC42 and BCL2 in neuroblastoma. Cancer Cell Int 19:357. https://doi.org/10.1186/s12935-019-1082-9
Megiorni F, Colaiacovo M, Cialfi S, McDowell HP, Guffanti A, Camero S, Felsani A, Losty PD, Pizer B, Shukla R, Cappelli C, Ferrara E, Pizzuti A, Moles A, Dominici C (2017) A sketch of known and novel MYCN-associated miRNA networks in neuroblastoma. Oncol Rep 38(1):3–20. https://doi.org/10.3892/or.2017.5701
Bray I, Bryan K, Prenter S, Buckley PG, Foley NH, Murphy DM, Alcock L, Mestdagh P, Vandesompele J, Speleman F, London WB, McGrady PW, Higgins DG, O’Meara A, O’Sullivan M, Stallings RL (2009) Widespread dysregulation of MiRNAs by MYCN amplification and chromosomal imbalances in neuroblastoma: association of miRNA expression with survival. PLoS One 4(11):e7850. https://doi.org/10.1371/journal.pone.0007850
Buhagiar A, Ayers D (2015) Chemoresistance, cancer stem cells, and miRNA influences: the case for neuroblastoma. Anal Cell Pathol (Amst) 2015:150634. https://doi.org/10.1155/2015/150634
Marengo B, Monti P, Miele M, Menichini P, Ottaggio L, Foggetti G, Pulliero A, Izzotti A, Speciale A, Garbarino O, Traverso N, Fronza G, Domenicotti C (2018) Etoposide-resistance in a neuroblastoma model cell line is associated with 13q14.3 mono-allelic deletion and miRNA-15a/16-1 down-regulation. Sci Rep 8(1):13762. https://doi.org/10.1038/s41598-018-32195-7
Toro-Dominguez D, Martorell-Marugan J, Lopez-Dominguez R, Garcia-Moreno A, Gonzalez-Rumayor V, Alarcon-Riquelme ME, Carmona-Saez P (2019) ImaGEO: integrative gene expression meta-analysis from GEO database. Bioinformatics 35(5):880–882. https://doi.org/10.1093/bioinformatics/bty721
Clough E, Barrett T (2016) The Gene Expression Omnibus database. Methods Mol Biol 1418:93–110. https://doi.org/10.1007/978-1-4939-3578-9_5
Barrett T, Wilhite SE, Ledoux P, Evangelista C, Kim IF, Tomashevsky M, Marshall KA, Phillippy KH, Sherman PM, Holko M, Yefanov A, Lee H, Zhang N, Robertson CL, Serova N, Davis S, Soboleva A (2013) NCBI GEO: archive for functional genomics data sets—update. Nucleic Acids Res 41(Database issue):D991–D995. https://doi.org/10.1093/nar/gks1193
Dumas J, Gargano MA, Dancik GM (2016) shinyGEO: a web-based application for analyzing gene expression omnibus datasets. Bioinformatics 32(23):3679–3681. https://doi.org/10.1093/bioinformatics/btw519
Edgar R, Domrachev M, Lash AE (2002) Gene Expression Omnibus: NCBI gene expression and hybridization array data repository. Nucleic Acids Res 30(1):207–210. https://doi.org/10.1093/nar/30.1.207
Gautier L, Cope L, Bolstad BM, Irizarry RA (2004) affy—analysis of Affymetrix GeneChip data at the probe level. Bioinformatics 20(3):307–315. https://doi.org/10.1093/bioinformatics/btg405
Diboun I, Wernisch L, Orengo CA, Koltzenburg M (2006) Microarray analysis after RNA amplification can detect pronounced differences in gene expression using limma. BMC Genom 7:252. https://doi.org/10.1186/1471-2164-7-252
Huang HY, Lin YC, Li J, Huang KY, Shrestha S, Hong HC, Tang Y, Chen YG, Jin CN, Yu Y, Xu JT, Li YM, Cai XX, Zhou ZY, Chen XH, Pei YY, Hu L, Su JJ, Cui SD, Wang F, Xie YY, Ding SY, Luo MF, Chou CH, Chang NW, Chen KW, Cheng YH, Wan XH, Hsu WL, Lee TY, Wei FX, Huang HD (2020) miRTarBase 2020: updates to the experimentally validated microRNA-target interaction database. Nucleic Acids Res 48(D1):D148–D154. https://doi.org/10.1093/nar/gkz896
Lu TP, Lee CY, Tsai MH, Chiu YC, Hsiao CK, Lai LC, Chuang EY (2012) miRSystem: an integrated system for characterizing enriched functions and pathways of microRNA targets. PLoS One 7(8):e42390. https://doi.org/10.1371/journal.pone.0042390
Dennis G Jr, Sherman BT, Hosack DA, Yang J, Gao W, Lane HC, Lempicki RA (2003) DAVID: database for annotation, visualization, and integrated discovery. Genome Biol 4(5):P3
Maere S, Heymans K, Kuiper M (2005) BiNGO: a Cytoscape plugin to assess overrepresentation of gene ontology categories in biological networks. Bioinformatics 21(16):3448–3449. https://doi.org/10.1093/bioinformatics/bti551
Szklarczyk D, Franceschini A, Kuhn M, Simonovic M, Roth A, Minguez P, Doerks T, Stark M, Muller J, Bork P, Jensen LJ, von Mering C (2011) The STRING database in 2011: functional interaction networks of proteins, globally integrated and scored. Nucleic Acids Res 39(Database issue):D561–D568. https://doi.org/10.1093/nar/gkq973
Szklarczyk D, Morris JH, Cook H, Kuhn M, Wyder S, Simonovic M, Santos A, Doncheva NT, Roth A, Bork P, Jensen LJ, von Mering C (2017) The STRING database in 2017: quality-controlled protein–protein association networks, made broadly accessible. Nucleic Acids Res 45(D1):D362–D368. https://doi.org/10.1093/nar/gkw937
Pan Q, Zhou R, Su M, Li R (2019) The effects of plumbagin on pancreatic cancer: a mechanistic network pharmacology approach. Med Sci Monit 25:4648–4654. https://doi.org/10.12659/MSM.917240
Gupta MK, Vadde R, Gouda G, Donde R, Kumar J, Behera L (2019) Computational approach to understand molecular mechanism involved in BPH resistance in Bt-rice plant. J Mol Graph Model 88:209–220. https://doi.org/10.1016/j.jmgm.2019.01.018
Chin CH, Chen SH, Wu HH, Ho CW, Ko MT, Lin CY (2014) cytoHubba: identifying hub objects and sub-networks from complex interactome. BMC Syst Biol 8(Suppl 4):S11. https://doi.org/10.1186/1752-0509-8-S4-S11
Pugh TJ, Morozova O, Attiyeh EF, Asgharzadeh S, Wei JS, Auclair D, Carter SL, Cibulskis K, Hanna M, Kiezun A, Kim J, Lawrence MS, Lichenstein L, McKenna A, Pedamallu CS, Ramos AH, Shefler E, Sivachenko A, Sougnez C, Stewart C, Ally A, Birol I, Chiu R, Corbett RD, Hirst M, Jackman SD, Kamoh B, Khodabakshi AH, Krzywinski M, Lo A, Moore RA, Mungall KL, Qian J, Tam A, Thiessen N, Zhao Y, Cole KA, Diamond M, Diskin SJ, Mosse YP, Wood AC, Ji L, Sposto R, Badgett T, London WB, Moyer Y, Gastier-Foster JM, Smith MA, Guidry Auvil JM, Gerhard DS, Hogarty MD, Jones SJ, Lander ES, Gabriel SB, Getz G, Seeger RC, Khan J, Marra MA, Meyerson M, Maris JM (2013) The genetic landscape of high-risk neuroblastoma. Nat Genet 45(3):279–284. https://doi.org/10.1038/ng.2529
Canete A (2020) High-risk neuroblastoma: where do we go? Ann Oncol 31(3):326–327. https://doi.org/10.1016/j.annonc.2019.12.003
Kraszewska I, Tomczyk M, Andrysiak K, Biniecka M, Geisler A, Fechner H, Zembala M, Stepniewski J, Dulak J, Jazwa-Kusior A (2020) Variability in cardiac miRNA-122 level determines therapeutic potential of miRNA-regulated AAV vectors. Mol Ther Methods Clin Dev 17:1190–1201. https://doi.org/10.1016/j.omtm.2020.05.006
Narayanan R, Schratt G (2020) miRNA regulation of social and anxiety-related behaviour. Cell Mol Life Sci. https://doi.org/10.1007/s00018-020-03542-7
Sun DG, Tian S, Zhang L, Hu Y, Guan CY, Ma X, Xia HF (2020) The miRNA-29b is downregulated in placenta during gestational diabetes mellitus and may alter placenta development by regulating trophoblast migration and invasion through a HIF3A-dependent mechanism. Front Endocrinol (Lausanne) 11:169. https://doi.org/10.3389/fendo.2020.00169
Slaby O, Laga R, Sedlacek O (2017) Therapeutic targeting of non-coding RNAs in cancer. Biochem J 474(24):4219–4251. https://doi.org/10.1042/BCJ20170079
Nowak I, Boratyn E, Durbas M, Horwacik I, Rokita H (2018) Exogenous expression of miRNA-3613-3p causes APAF1 downregulation and affects several proteins involved in apoptosis in BE(2)-C human neuroblastoma cells. Int J Oncol 53(4):1787–1799. https://doi.org/10.3892/ijo.2018.4509
D’Aiuto F, Callari M, Dugo M, Merlino G, Musella V, Miodini P, Paolini B, Cappelletti V, Daidone MG (2015) miR-30e* is an independent subtype-specific prognostic marker in breast cancer. Br J Cancer 113(2):290–298. https://doi.org/10.1038/bjc.2015.206
Cordeau M, Belounis A, Lelaidier M, Cordeiro P, Sartelet H, Herblot S, Duval M (2016) Efficient killing of high risk neuroblastoma using natural killer cells activated by plasmacytoid dendritic cells. PLoS One 11(10):e0164401. https://doi.org/10.1371/journal.pone.0164401
Wang P, Gu Y, Zhang Q, Han Y, Hou J, Lin L, Wu C, Bao Y, Su X, Jiang M, Wang Q, Li N, Cao X (2012) Identification of resting and type I IFN-activated human NK cell miRNomes reveals microRNA-378 and microRNA-30e as negative regulators of NK cell cytotoxicity. J Immunol 189(1):211–221. https://doi.org/10.4049/jimmunol.1200609
Klein U, Lia M, Crespo M, Siegel R, Shen Q, Mo T, Ambesi-Impiombato A, Califano A, Migliazza A, Bhagat G, Dalla-Favera R (2010) The DLEU2/miR-15a/16-1 cluster controls B cell proliferation and its deletion leads to chronic lymphocytic leukemia. Cancer Cell 17(1):28–40. https://doi.org/10.1016/j.ccr.2009.11.019
Chava S, Reynolds CP, Pathania AS, Gorantla S, Poluektova LY, Coulter DW, Gupta SC, Pandey MK, Challagundla KB (2020) miR-15a-5p, miR-15b-5p, and miR-16-5p inhibit tumor progression by directly targeting MYCN in neuroblastoma. Mol Oncol 14(1):180–196. https://doi.org/10.1002/1878-0261.12588
Klein S, Abraham M, Bulvik B, Dery E, Weiss ID, Barashi N, Abramovitch R, Wald H, Harel Y, Olam D, Weiss L, Beider K, Eizenberg O, Wald O, Galun E, Pereg Y, Peled A (2018) CXCR4 promotes neuroblastoma growth and therapeutic resistance through miR-15a/16-1-mediated ERK and BCL2/Cyclin D1 pathways. Cancer Res 78(6):1471–1483. https://doi.org/10.1158/0008-5472.CAN-17-0454
Matuzelski E, Harvey TJ, Harkins D, Nguyen T, Ruitenberg MJ, Piper M (2020) Expression of NFIA and NFIB within the murine spinal cord. Gene Expr Patterns 35:119098. https://doi.org/10.1016/j.gep.2020.119098
Liu Z, Chen J, Yuan W, Ruan H, Shu Y, Ji J, Wu L, Tang Q, Zhou Z, Zhang X, Cheng Y, He S, Shu X (2019) Nuclear factor I/B promotes colorectal cancer cell proliferation, epithelial-mesenchymal transition and 5-fluorouracil resistance. Cancer Sci 110(1):86–98. https://doi.org/10.1111/cas.13833
Xu L, Ni J, Wang Y, Dong Y, Wang S (2019) Genetic variant of NFIB is associated with the metastasis of osteosarcoma in Chinese population. Technol Cancer Res Treat 18:1533033819874802. https://doi.org/10.1177/1533033819874802
Becker-Santos DD, Thu KL, English JC, Pikor LA, Martinez VD, Zhang M, Vucic EA, Luk MT, Carraro A, Korbelik J, Piga D, Lhomme NM, Tsay MJ, Yee J, MacAulay CE, Lam S, Lockwood WW, Robinson WP, Jurisica I, Lam WL (2016) Developmental transcription factor NFIB is a putative target of oncofetal miRNAs and is associated with tumour aggressiveness in lung adenocarcinoma. J Pathol 240(2):161–172. https://doi.org/10.1002/path.4765
Liu RZ, Vo TM, Jain S, Choi WS, Garcia E, Monckton EA, Mackey JR, Godbout R (2019) NFIB promotes cell survival by directly suppressing p21 transcription in TP53-mutated triple-negative breast cancer. J Pathol 247(2):186–198. https://doi.org/10.1002/path.5182
Ortega S, Malumbres M, Barbacid M (2002) Cyclin D-dependent kinases, INK4 inhibitors and cancer. Biochim Biophys Acta 1602(1):73–87. https://doi.org/10.1016/s0304-419x(02)00037-9
Rader J, Russell MR, Hart LS, Nakazawa MS, Belcastro LT, Martinez D, Li Y, Carpenter EL, Attiyeh EF, Diskin SJ, Kim S, Parasuraman S, Caponigro G, Schnepp RW, Wood AC, Pawel B, Cole KA, Maris JM (2013) Dual CDK4/CDK6 inhibition induces cell-cycle arrest and senescence in neuroblastoma. Clin Cancer Res 19(22):6173–6182. https://doi.org/10.1158/1078-0432.CCR-13-1675
Rihani A, Vandesompele J, Speleman F, Van Maerken T (2015) Inhibition of CDK4/6 as a novel therapeutic option for neuroblastoma. Cancer Cell Int 15:76. https://doi.org/10.1186/s12935-015-0224-y
Kato K, Miya F, Hamada N, Negishi Y, Narumi-Kishimoto Y, Ozawa H, Ito H, Hori I, Hattori A, Okamoto N, Kato M, Tsunoda T, Kanemura Y, Kosaki K, Takahashi Y, Nagata KI, Saitoh S (2019) MYCN de novo gain-of-function mutation in a patient with a novel megalencephaly syndrome. J Med Genet 56(6):388–395. https://doi.org/10.1136/jmedgenet-2018-105487
Harmelink C, Peng Y, DeBenedittis P, Chen H, Shou W, Jiao K (2013) Myocardial Mycn is essential for mouse ventricular wall morphogenesis. Dev Biol 373(1):53–63. https://doi.org/10.1016/j.ydbio.2012.10.005
Cohn SL, Pearson AD, London WB, Monclair T, Ambros PF, Brodeur GM, Faldum A, Hero B, Iehara T, Machin D, Mosseri V, Simon T, Garaventa A, Castel V, Matthay KK, Force IT (2009) The International Neuroblastoma Risk Group (INRG) classification system: an INRG Task Force report. J Clin Oncol 27(2):289–297. https://doi.org/10.1200/JCO.2008.16.6785
Giangarra V, Igea A, Castellazzi CL, Bava FA, Mendez R (2015) Global analysis of CPEBs reveals sequential and non-redundant functions in mitotic cell cycle. PLoS One 10(9):e0138794. https://doi.org/10.1371/journal.pone.0138794
DeLigio JT, Lin G, Chalfant CE, Park MA (2017) Splice variants of cytosolic polyadenylation element-binding protein 2 (CPEB2) differentially regulate pathways linked to cancer metastasis. J Biol Chem 292(43):17909–17918. https://doi.org/10.1074/jbc.M117.810127
Tordjman J, Majumder M, Amiri M, Hasan A, Hess D, Lala PK (2019) Tumor suppressor role of cytoplasmic polyadenylation element binding protein 2 (CPEB2) in human mammary epithelial cells. BMC Cancer 19(1):561. https://doi.org/10.1186/s12885-019-5771-5
Johnson RM, Vu NT, Griffin BP, Gentry AE, Archer KJ, Chalfant CE, Park MA (2015) The alternative splicing of cytoplasmic polyadenylation element binding protein 2 drives anoikis resistance and the metastasis of triple negative breast cancer. J Biol Chem 290(42):25717–25727. https://doi.org/10.1074/jbc.M115.671206
Li C, Gao Y, Li Y, Ding D (2017) TUG1 mediates methotrexate resistance in colorectal cancer via miR-186/CPEB2 axis. Biochem Biophys Res Commun 491(2):552–557. https://doi.org/10.1016/j.bbrc.2017.03.042
Acknowledgements
We thank the staff from the Medical Research Center of Shengjing Hospital who supported us throughout the experiments.
Funding
The work was supported by the National Natural Science Foundation of China (Nos. 81972515, 81472359), Key Research and Development Foundation of Liaoning Province (2019JH8/10300024), 2013 Liaoning Climbing Scholar Foundation, and 345 Talent Project of Shengjing Hospital of China Medical University.
Author information
Authors and Affiliations
Contributions
BC contributed to the study design, collection and interpretation of data, and the writing of the manuscript; ZH and XQ contributed to collection of data; ZL contributed to the study design, interpretation of the data, the writing of the manuscript, and the submission of the manuscript for publication.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants or animals.
Informed Consent
For this type of study, formal consent is not required.
Consent to Participate
Not applicable.
Consent for Publication
All authors consent to the publication of this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, B., Hua, Z., Qin, X. et al. Integrated Microarray to Identify the Hub miRNAs and Constructed miRNA–mRNA Network in Neuroblastoma Via Bioinformatics Analysis. Neurochem Res 46, 197–212 (2021). https://doi.org/10.1007/s11064-020-03155-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-020-03155-3