Abstract
Purpose
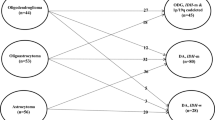
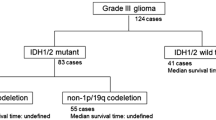
According to the 2016 WHO classification lower-grade gliomas consist of three groups: IDH-mutated and 1p/19q co-deleted, IDH-mutated and IDH-wildtype tumors. The aim of this study was to evaluate the impact of surgical therapy for lower-grade gliomas with a particular focus on the molecular subgroups.
Methods
This is a bi-centric retrospective analysis including 299 patients, who underwent treatment for lower-grade glioma between 1990 and 2016. All tumors were re-classified according to the 2016 WHO classification. Data concerning baseline and tumor characteristics, overall survival, different treatment modalities and functional outcome were analyzed.
Results
A total of 112 (37.5%) patients with IDH-mutation and 1p/19q co-deletetion, 86 (28.8%) patients with IDH-mutation and 101 (33.8%) patients with IDH-wildtype tumors were identified. The median overall survival (mOS) differed significantly between the groups (p < 0.001). Surgical resection was performed in 226 patients and showed significantly improved mOS compared to the biopsy group (p = 0.001). Gross total resection (GTR) was associated with better survival (p = 0.007) in the whole cohort as well as in the IDH-mutated and IDH-wildtype groups compared to partial resection or biopsy. IDH-wildtype patients presented a significant survival benefit after combined radio-chemotherapy compared to radio- or chemotherapy alone (p = 0.02). Good clinical status (NANO) was associated with longer OS (p = 0.001).
Conclusion
The impact of surgical treatment on the outcome of lower-grade gliomas depends to a great extent on the molecular subtype of the tumors. Patients with more aggressive tumors (IDH-wildtype) seem to profit from more intensive treatment like GTR, multiple resections and combined radio-/chemotherapy.




Similar content being viewed by others
References
Louis DN, Perry A, Reifenberger G et al (2016) The 2016 World Health Organization classification of tumors of the central nervous system: a summary. Acta Neuropathol 131:803–820. https://doi.org/10.1007/s00401-016-1545-1
The Cancer Genome Atlas Research Network (2015) Comprehensive, integrative genomic analysis of diffuse lower-grade gliomas. N Engl J Med 372:2481–2498. https://doi.org/10.1056/NEJMoa1402121
Leeper HE, Caron AA, Decker PA et al (2015) IDH mutation, 1p19q codeletion and ATRX loss in WHO grade II gliomas. Oncotarget 6:30295–30305. https://doi.org/10.18632/oncotarget.4497
Weller M, Weber RG, Willscher E et al (2015) Molecular classification of diffuse cerebral WHO grade II/III gliomas using genome- and transcriptome-wide profiling improves stratification of prognostically distinct patient groups. Acta Neuropathol 129:679–693. https://doi.org/10.1007/s00401-015-1409-0
Weller M, Felsberg J, Hartmann C et al (2009) Molecular predictors of progression-free and overall survival in patients with newly diagnosed glioblastoma: a prospective translational study of the German Glioma Network. J Clin Oncol 27:5743–5750. https://doi.org/10.1200/JCO.2009.23.0805
Buckner J, Giannini C, Eckel-Passow J et al (2017) Management of diffuse low-grade gliomas in adults—use of molecular diagnostics. Nat Publ Group 1–12. https://doi.org/10.1038/nrneurol.2017.54
Cahill DP, Sloan AE, Nahed BV et al (2015) The role of neuropathology in the management of patients with diffuse low grade glioma. J Neurooncol 125:531–549. https://doi.org/10.1007/s11060-015-1909-8
Olar A, Wani KM, Alfaro-Munoz KD et al (2015) IDH mutation status and role of WHO grade and mitotic index in overall survival in grade II–III diffuse gliomas. Acta Neuropathol 129:585–596. https://doi.org/10.1093/neuonc/nos263
Sanai N, Chang S, Berger MS (2011) Low-grade gliomas in adults. J Neurosurg 115:948–965. https://doi.org/10.3171/2011.7.JNS101238
Potts MB, Smith JS, Molinaro AM, Berger MS (2012) Natural history and surgical management of incidentally discovered low-grade gliomas. J Neurosurg 116:365–372. https://doi.org/10.3171/2011.9.JNS111068
Capelle L, Fontaine D, Mandonnet E et al (2013) Spontaneous and therapeutic prognostic factors in adult hemispheric World Health Organization Grade II gliomas: a series of 1097 cases: clinical article. J Neurosurg 118:1157–1168. https://doi.org/10.3171/2013.1.JNS121
Englot DJ, Chang EF, Vecht CJ (2016) Epilepsy and brain tumors. Handb Clin Neurol 134:267–285. https://doi.org/10.1016/B978-0-12-802997-8.00016-5
Englot DJ, Berger MS, Barbaro NM, Chang EF (2011) Predictors of seizure freedom after resection of supratentorial low-grade gliomas. J Neurosurg 115:240–244. https://doi.org/10.3171/2011.3.JNS1153
Duffau H (2014) Diffuse low-grade gliomas andneuroplasticity. Diagn Interv Imaging 95:945–955. https://doi.org/10.1016/j.diii.2014.08.001
Weller M, van den Bent M, Tonn JC et al (2017) European Association for Neuro-Oncology (EANO) guideline on the diagnosis and treatment of adult astrocytic and oligodendroglial gliomas. Lancet Oncol 18:e315–e329. https://doi.org/10.1016/S1470-2045(17)30194-8
Roelz R, Strohmaier D, Jabbarli R et al (2016) Residual tumor volume as best outcome predictor in low grade glioma—a nine-years near- randomized survey of surgery vs. biopsy. Nat Publ Group https://doi.org/10.1038/srep32286
Duffau H (2017) The role of surgery in low-grade gliomas: do timing and extent of resection matter? CNS Oncol 6:179–183. https://doi.org/10.2217/cns-2017-0009
Michaud K, Duffau H (2016) Surgery of insular and paralimbic diffuse low-grade gliomas: technical considerations. J Neurooncol 130:289–298. https://doi.org/10.1007/s11060-016-2120-2
Eseonu CI, ReFaey K, Garcia O et al (2017) Original article. World Neurosurg 103:265–274. https://doi.org/10.1016/j.wneu.2017.04.002
Gousias K, Schramm J, Simon M (2013) Extent of resection and survival in supratentorial infiltrative low-grade gliomas: analysis of and adjustment for treatment bias. Acta Neurochir (Wien) 156:327–337. https://doi.org/10.1158/1078-0432.CCR-07-0573
Englot DJ, Han SJ, Berger MS et al (2012) Extent of surgical resection predicts seizure freedom in low-grade temporal lobe brain tumors. Neurosurgery 70:921–928. https://doi.org/10.1227/NEU.0b013e31823c3a30
Sanai N, Berger MS (2008) Glioma extent of resection and its impact on patient outcome. Neurosurgery 62:753–764. https://doi.org/10.1227/01.neu.0000318159.21731.cf (discussion 264–6).
Smith JS, Chang EF, Lamborn KR et al (2008) Role of extent of resection in the long-term outcome of low-grade hemispheric gliomas. J Clin Oncol 26:1338–1345. https://doi.org/10.1200/JCO.2007.13.9337
Jakola AS, Myrmel KS, Kloster R et al (2012) Comparison of a strategy favoring early surgical resection vs a strategy favoring watchful waiting in low-grade gliomas. JAMA 308:1881. https://doi.org/10.1001/jama.2012.12807
Jakola AS, Skjulsvik AJ, Myrmel KS et al (2017) Surgical resection versus watchful waiting in low-grade gliomas. Ann Oncol. https://doi.org/10.1093/annonc/mdx230
Eseonu CI (2017) Comparative volumetric analysis of the extent of resection of molecularly and histologically distinct low grade gliomas and its role on survival. J Neurooncol 134:65–74. https://doi.org/10.1007/s11060-017-2486-9
van den Bent MJ, Wefel JS, Schiff D et al (2011) Response assessment in neuro-oncology (a report of the RANO group): assessment of outcome in trials of diffuse low-grade gliomas. Lancet Oncol 12:583–593. https://doi.org/10.1016/S1470-2045(11)70057-2
Weller M, van den Bent M, Hopkins K et al (2014) EANO guideline for the diagnosis and treatment of anaplastic gliomas and glioblastoma. Lancet Oncol 15:e395–e403. https://doi.org/10.1016/S1470-2045(14)70011-7
Nayak L, DeAngelis LM, Brandes AA et al (2017) The Neurologic Assessment in Neuro-Oncology (NANO) scale: a tool to assess neurologic function for integration into the Response Assessment in Neuro-Oncology (RANO) criteria. Neurooncology 19:625–635. https://doi.org/10.1093/neuonc/nox029
Wick W, Roth P, Hartmann C et al (2016) Long-term analysis of the NOA-04 randomized phase III trial of sequential radiochemotherapy of anaplastic glioma with PCV or temozolomide. Neuro-Oncology. https://doi.org/10.1093/neuonc/now133
van den Bent MDPMJ, MD BB, MD SCE et al (2017) Interim results from the CATNON trial (EORTC study 26053–22054) of treatment with concurrent and adjuvant temozolomide for 1p/19q non-co-deleted anaplastic glioma: a phase 3, randomised, open-label intergroup study. Lancet. https://doi.org/10.1016/S0140-6736(17)31442-3
Baumert BG, Hegi ME, van den Bent MJ et al (2016) Temozolomide chemotherapy versus radiotherapy in high-risk low-grade glioma (EORTC 22033–26033): a randomised, open-label, phase 3 intergroup study. Lancet Oncol 17:1521–1532. https://doi.org/10.1016/S1470-2045(16)30313-8
Wijnenga MMJ, French PJ, Dubbink HJ et al (2017) The impact of surgery in molecularly defined low-grade glioma: an integrated clinical, radiological, and molecular analysis. Neurooncology 20:103–112. https://doi.org/10.1093/neuonc/nou297
Kawaguchi T, Sonoda Y, Shibahara I et al (2016) Impact of gross total resection in patients with WHO grade III glioma harboring the IDH 1/2 mutation without the 1p/19q co-deletion. J Neurooncol 129:505–514. https://doi.org/10.1007/s11060-016-2201-2
Rahman M, Abbatematteo J, De Leo EK et al (2017) The effects of new or worsened postoperative neurological deficits on survival of patients with glioblastoma. J Neurosurg 127:123–131. https://doi.org/10.3171/2016.7.JNS16396
Duffau H, Taillandier L (2014) New concepts in the management of diffuse low-grade glioma: proposal of a multistage and individualized therapeutic approach. Neurooncology. https://doi.org/10.1093/neuonc/nou153
Aibaidula A, Chan AK-Y, Shi Z et al (2017) Adult IDH wild-type lower-grade gliomas should be further stratified. Neurooncology 19:1327–1337. https://doi.org/10.1093/neuonc/nox078
Appin CL, Brat DJ (2014) Molecular genetics of gliomas. Cancer J 20:66–72. https://doi.org/10.1097/PPO.0000000000000020
van den Bent MJ, Smits M, Kros JM, Chang SM (2017) Diffuse infiltrating oligodendroglioma and astrocytoma. J Clin Oncol 35:2394–2401. https://doi.org/10.1200/JCO.2017.72.6737
van den Bent MJ, Weller M, Wen PY et al (2017) A clinical perspective on the 2016 WHO brain tumor classification and routine molecular diagnostics. Neurooncology 19:614–624. https://doi.org/10.1093/neuonc/now277
Funding
This research did not receive any financial or material support from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Electronic supplementary material
Below is the link to the electronic supplementary material.
11060_2018_3030_MOESM1_ESM.png
Supplementary figure 1 Kaplan Meier Curves showing the overall survival according to extent of resection, comparing patients with at least one gross total resection (GTR) to those with biopsy or partial resection after molecular subgroup stratification (PNG 487 KB)
11060_2018_3030_MOESM2_ESM.png
Supplementary figure 2 Kaplan Meier Curves showing the overall survival according to WHO grade after molecular subgroup stratification (PNG 480 KB)
Rights and permissions
About this article
Cite this article
Delev, D., Heiland, D.H., Franco, P. et al. Surgical management of lower-grade glioma in the spotlight of the 2016 WHO classification system. J Neurooncol 141, 223–233 (2019). https://doi.org/10.1007/s11060-018-03030-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-018-03030-w