Abstract
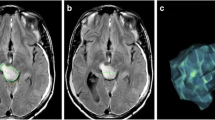
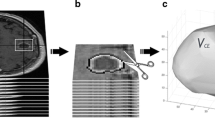
Diagnosis of progressive disease or (partial) response during tumor treatment is based on manual size estimates of enhancing tumor area: an expert measures two perpendicular diameters of the enhancing tumor region in a single MRI slice with the largest enhancing area. This paper analyzes the reliability of the area measure with respect to head placement in the MRI scanner and compares it with 3D volume measures in a dataset of eight subjects (5–7 follow-up scans each) with high-grade glioma. We show that the manual area measure is highly sensitive to head position changes, with a root mean squared error of 22 %, compared to volume estimates with less than 5 % error. In our simulated study using the 2D manual measurements, the majority of subjects would have been incorrectly diagnosed with progressive disease without any true anatomical changes. These results highlight the urgent need for revised and more reliable response assessment criteria, for example, based on increased slice resolution, 3D volume analysis and percent change computation with respect to an average of patient specific longitudinal measurements instead of a single measurement to define progression or response.




Similar content being viewed by others
References
Benner T, Wisco JJ, van der Kouwe AJW, Fischl B, Vangel MG, Hochberg FH, Sorensen AG (2006) Comparison of manual and automatic section positioning of brain MR images. Radiology 239(1):246–254. doi:10.1148/radiol.2391050221
Lin L (1989) A concordance correlation coefficient to evaluate reproducibility. Biometrics 45(1):255–268. http://www.jstor.org/stable/2532051
Macdonald DR, Cascino TL, Schold SC Jr, Cairncross JG (1990) Response criteria for phase II studies of supratentorial malignant glioma. J Clin Oncol 8(7):1277–1280. http://jco.ascopubs.org/content/8/7/1277.long
Reuter M, Rosas HD, Fischl B (2010) Highly accurate inverse consistent registration: a robust approach. Neuroimage 53(4):1181–1196. doi:10.1016/j.neuroimage.2010.07.020
Shah GD et al (2006) Comparison of linear and volumetric criteria in assessing tumor response in adult high-grade gliomas. Neuro Oncol 8(1):38–46
Schmitt P, Mandonnet E, Perdreau A, Angelini ED (2013) Effects of slice thickness and head rotation when measuring glioma sizes on MRI: in support of volume segmentation versus two largest diameters methods. J Neuro-Oncol 112(2):165–172. doi:10.1007/s11060-013-1051-4
Thevenaz P, Blu T, Unser M (2000) Interpolation revisited. IEEE Trans Med Imaging 19(7):739–758. doi:10.1109/42.875199
van den Bent MJ, Wefel JS, Schiff D, Taphoorn MJ, Jaeckle K, Junck L, Armstrong T, Choucair A, Waldman AD, Gorlia T, Chamberlain M, Baumert BG, Vogelbaum MA, Macdonald DR, Reardon DA, Wen PY, Chang SM, Jacobs AH (2011) Response assessment in neuro-oncology (a report of the RANO group): assessment of outcome in trials of diffuse low-grade gliomas. Lancet Oncol 12(6):583–593. doi:10.1016/S1470-2045(11)70057-2
van der Kouwe AJ, Benner T, Fischl B, Schmitt F, Salat DH, Harder M, Sorensen AG, Dale AM (2005) On-line automatic slice positioning for brain MR imaging. Neuroimage 27(1):222–230. doi:10.1016/j.neuroimage.2005.03.035
van der Kouwe AJ, Benner T, Salat DH, Fischl B (2008) Brain morphometry with multiecho MPRAGE. Neuroimage 40(2):559–569. doi:10.1016/j.neuroimage.2007.12.025
Wen PY, Macdonald DR, Reardon DA, Cloughesy TF, Sorensen AG, Galanis E, Degroot J, Wick W, Gilbert MR, Lassman AB, Tsien C, Mikkelsen T, Wong ET, Chamberlain MC, Stupp R, Lamborn KR, Vogelbaum MA, van den Bent MJ, Chang SM (2010) Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol 28(11):1963–1972. doi:10.1200/JCO.2009.26.3541
Wilcoxon F (1945) Individual comparisons by ranking methods. Biometr Bull 1(6):80–83. http://www.jstor.org/stable/3001968
Wolak ME, Fairbairn DJ, Paulsen YR (2012) Guidelines for estimating repeatability. Methods Ecol Evol 3(1):129–137. doi:10.1111/j.2041-210X.2011.00125.x
Acknowledgments
Support for this research was provided in part by the National Center for Research Resources (P41-RR14075, U24-RR021382, 1UL1-RR025758-01, 1S10-RR023401, 1S10-RR019307, 1S10-RR023043), the National Institute for Biomedical Imaging and Bioengineering (5P41-EB015896-15, R01-EB006758), the National Cancer Institute (5U01-CA154601-03, N01-CM-2008-00060C), the National Institute on Aging (AG022381, 5R01-AG008122-22), the National Center for Alternative Medicine (RC1-AT005728-01), the National Institute for Neurological Disorders and Stroke (R01-NS052585-01, 1R21-NS072652-01, 1R01-NS070963), Merck, the Ellison Medical Foundation (The Autism & Dyslexia Project) and by the National Institute of Health Blueprint for Neuroscience Research (5U01-MH093765 Human Connectome Project).
Conflict of interest
BF has a financial interest in CorticoMetrics, a company whose medical pursuits focus on brain imaging and measurement technologies. BF’s interests were reviewed and are managed by Massachusetts General Hospital and Partners HealthCare in accordance with their conflict of interest policies. CorticoMetrics did not sponsor any part of this research. The other authors declare that they have no conflict of interest.
Ethical standard
Experiments comply with the current laws of the country in which they were performed.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Reuter, M., Gerstner, E.R., Rapalino, O. et al. Impact of MRI head placement on glioma response assessment. J Neurooncol 118, 123–129 (2014). https://doi.org/10.1007/s11060-014-1403-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-014-1403-8