Abstract
Objective
To improve the diagnosis and treatment of Penicilliosis marneffei without human immunodeficiency virus infection.
Methods
Analyze and review the clinical features, diagnosis and treatment of six cases of P. marneffei without human immunodeficiency virus infection at The First Affiliated Hospital of Fujian Medical University.
Results
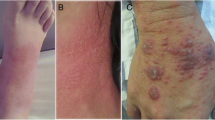
Two cases were diagnosed in the ENT Department, three cases in the respiratory department and one case in the dermatological department. Penicillium marneffei infection was confirmed by sputum culture, blood culture and tissue biopsy. After definite diagnosis, one refused further treatment, and others showed significant improvement.
Conclusion
Penicilliosis marneffei is insidious onset and easy to be escaped and misdiagnosed. To achieve early diagnosis and appropriate treatment, doubtful cases should be alerted for the diagnoses as P. marneffei.




Similar content being viewed by others
References
Hu Y, Zhang J, Li X, et al. Penicillium marneffei infection: an emerging disease in mainland China. Mycopathologia. 2013;175(1–2):57–67.
Devi KR, Singh LR, Rajkumari R, et al. Penicillium marneffei—an indicator disease of AIDS: a case report. Indian J Pathol Microbiol. 2007;50(3):674–6.
Xie Y, Li Y, Hu C, et al. The analysis of risk factors and the immune status in Penicillium marneffei in patients without human immunodeficiency virus infection. Chin Mycol. 2016;11(3):174–7.
Yulan L, Bin Y, Yongxu J, et al. A case report of disseminated Penicillium marneffei without HIV infection. Int J Lab Med. 2012;33(10):1196–9.
Cooper CR Jr, Haycocks NG. Penicillium marneffei: an insurgent species among the penicillin. Eukaryot Microbiol. 2000;47(1):24–8.
Tsui WM, Ma KF, Tsang DN. Disseminated Penicillium marneffei infection in HIV-infected subject. Histopathology. 1992;20:287–93.
Lu ZH, Liu HR, Xie XL, et al. Infection of Penicillium marneffei. [Zhonghua bing li xue za zhi] Chin J Pathol. 2004;33(6):536–40 (in Chinese).
Vanittanakom N, Cooper CR Jr, Fisher MC, et al. Penicillium marneffei infection and recent advances in the epidemiology and molecular biology aspects. Clin Microbiol Rev. 2006;19(1):95–110.
Mo Z. Two Penicillium marneffei infant with HIV-negative, cases report and literature review[J]. J Youjiang Med Univ Natl. 2015;37(5):737–9.
Su X, Zhang N, Liu C, et al. Disseminated Penwillium marneffei infection in immunocompetent patients: one case report and literature review. Chin J Respir Crit Care Med. 2013;12(3):244–8.
Kawila R, Chaiwarith R, Supparatpinyo K. Clinical and laboratory characteristics of Penicilliosis marneffei among patients with and without HIV infection in Northern Thailand: a retrospective study. BMC Infect Dis. 2013;13:464.
Qiu Y, Liao H, Zhang J, et al. Differences in clinical characteristics and prognosis of Penicilliosis among HIV-negative patients with or without underlying disease in Southern China: a retrospective study. BMC Infect Dis. 2015;15:525.
Li L, Tang X, Cai W. The clinical research of 101 AIDS combined with Penicilliosis marneffei. Chin AIDS. 2008;14(1):12–4.
Li HJ, Zhang YJ, et al. CT manifestation of Penicillium marneffei pneumonia in AIDS patients. Fang she xue shi jian Radiol Pract. 2009;24(9):952–4.
Bo L, Ping F. Research progress of Penicilliosis marneffei. Dermatol Venereol. 2010;3(1):26–8.
Liyan X, Changming L, Xianyi Z, et al. Fifteen cases of penicilliosis in Guangdong, China. Mycopathologia. 2004;158(2):151–5.
Wanshan C, Xiaoping T, Yecheng L, et al. In vitro susceptibilities of 5 antifungal agents against 52 strains of Penicillium marneffei. Chin J Infect Dis. 2008;26(3):143–5.
Ye R, Song W, Qiu X, et al. Analysis of fungus infection and drug sensitivity in AIDS patients. Guangdong Med. 2007;28(5):783–5.
Zhang Q, Liang L, Cao C, et al. Effects of amphotericin B and voriconazole on ultrastructure of a clinical isolate of Penicillium marneffei. Chin J Dermatol. 2015;8:572–5.
Xie L, Wang J, Zhang J, et al. Identification and in vitro antifungal susceptibility of Penicillium marneffei in yeast phase. Chin J Infect Control. 2016;15(12):934–8.
Cristina M, Patriza P, Alessanda G, et al. Discontinuation of primary prophylaxis for Pneumocystis carinii pneumonia and toxoplasmic encephalitis in human immunodeficiency virus type-1 infections: the charges in opportunistic prophylaxis study. Infect Dis. 2000;18(5):1635–42.
Acknowledgements
Authors thank professor Lin Qi-chang, Department of Respiration, the First Affiliated Hospital of Fujian Medical University, for his kind of offering the cases of respiratory department. We also thank our colleagues of clinical laboratory for their assistance of fungal identification.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The research has no conflicts of interest.
Ethical Standard
The research was compliance with ethical standards, and all the patients involved were informed consent.
Rights and permissions
About this article
Cite this article
Wang, Yg., Cheng, Jm., Ding, Hb. et al. Study on the Clinical Features and Prognosis of Penicilliosis marneffei Without Human Immunodeficiency Virus Infection. Mycopathologia 183, 551–558 (2018). https://doi.org/10.1007/s11046-017-0236-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-017-0236-3