Abstract
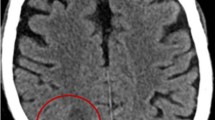
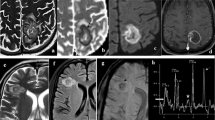
Scedosporium apiospermum is a saprobic fungus responsible for many different clinical manifestations. Although it affects mostly immunocompromised patients, pulmonary and disseminated scedosporiosis have also been reported in immunocompetent subjects. It often causes subcutaneous mycetoma, despite its preferential tropism to CNS. The authors describe a fatal case of a S. apiospermum brain abscess in a 58-year-old female. She was affected by chronic liver disease and idiopathic pulmonary fibrosis and had been treated with corticosteroid therapy for a long time. She recovered in a neurosurgery unit, wherein TC scan and cerebral MRI revealed an expansive left temporo-parietal process with vasogenic oedema. A stereotactic puncture of the lesion was carried out, and pus of brain abscess was evacuated. Empirical antifungal therapy was initiated with liposomal amphotericine B based on the clinical suspicion of Zygomycetes infection; after 3 days, posaconazole was added. The correct aetiological diagnosis arrived too late and the patient was treated with no specific therapy. This fatal case confirms the necessity of having a fast and correct aetiological diagnosis to improve the patient’s outcome.



Similar content being viewed by others
References
Cortez KJ, Roilides E, Quiroz-Telles F, Meletiadis J, Antachopoulos C, Knudsen T, Buchanan W, Milanovich J, Sutton DA, Fothergill A, Rinaldi MG, Shea YR, Zaoutis T, Kottilil S, Walsh TJ. Infections caused by Scedosporium spp. Clin Microbiol Rev. 2008;21:157–97.
Tintelnot K, Wagner N, Seibold M, de Hoog GS, Horrè R. Re-identification of clinical isolates of the Pseudallescheria boydii-complex involved in near-drowning. Mycoses. 2008;51:11–6.
Wilichowski E, Christen HJ, Schiffmann H, Schulz-Schaeffer W, Behrens-Baumann W. Fatal Pseudallescheria boydii panencephalitis in a child after near-drowning. Pediatr Infect Dis J. 1996;15:365–70.
Katragkou A, Dotis J, Kotsiou M, Tamiolaki M, Roilides E. Scedosporium apiospermum infection after near-drowning. Mycoses. 2007;50:412–21.
Poza G, Montoya J, Redondo C, Ruiz J, Vila N, Rodriguez-Tudela JL, Cerón A, Simarro E. Meningitis caused by Pseudallescheria boydii treated with voriconazole. Clin Infect Dis. 2000;30:981–2.
Tadros TS, Workowski KA, Siegel RJ, Hunter S, Schwartz DA. Pathology of hyalohyphomycosis caused by Scedosporium apiospermum (Pseudallescheria boydii): an emerging mycosis. Hum Pathol. 1998;29:1266–72.
De Hoog G, Guarro J, Gené J, Figueras MJ. Atlas of clinical fungi, 2nd edn, Utrecht: Centraalbureau voor Schimmelcultures, 2000.
Clinical and Laboratory Standard Institute. Reference method for broth dilution antifungal susceptibility testing of filamentous fungi; Approved standard—2nd edn. CLSI Document M38-A2. Wayne, PA. Clinical and Laboratory Standard Institute, 2008.
Pfaller MA, Diekema DJ, Jones RN, Sader HS, Fluit AC, Hollis RJ, Messer SA. SENTRY participant group. International surveillance of bloodstream infections due to Candida species: frequency of occurrence and in vitro susceptibilities to fluconazole, ravuconazole, voriconazole of isolates collected from 1997 through 1999 in the SENTRY antimicrobial surveillance program. J Clin Microbiol. 2001;39:3254–59.
Diekema DJ, Messer SA, Boyken LB, Hollis RJ, Kroeger J, Tendolkar S, Pfaller MA. In vitro activity of seven systemically active antifungal agents against a large global rare Candida species as determined by CLSI broth microdilution methods. J Clin Microbiol. 2009;47:3170–7.
Gilgado F, Cano J, Gené J, Sutton DA, Guarro J. Molecular and phenotypic data supporting distinct species statuses for Scedosporium apiospermum and Pseudallescheria boydii and the new species Scedosporium dehoogii. J Clin Microbiol. 2008;46:766–71.
Gilgado F, Genè J, Cano J, Guarro J. Heterothallism in Scedosporium apiospermum and description of its teleomorph Pseudallescheria apiospermum sp. nov. Med Mycol. 2010;48:122–8.
Kowacs PA, Soares Silvado CE, Monteiro de Almeida S, Ramos M, Abrão K, Madaloso LE, Pinheiro RL, Werneck LC. Infection of CNS by Scedosporium apiospermum after near-drowning. Report of a fatal case and analysis of its confounding factors. J Clin Pathol. 2004;57:205–7.
Guarro J, Kantarcioglu AS, Horré R, Rodriguez-Tudela JL, Cuenca Estrella M, Berenguer J, de Hoog GS. Scedosporium apiospermum changing clinical spectrum of a therapy-refractory opportunist. Med Mycol. 2006;44:295–327.
Alastruey-Izquierdo A, Cuenca-Estrella M, Monzón A, Rodriguez-Tudela JL. Prevalence and susceptibility testing of new species of Pseudallescheria and Scedosporium in a collection of clinical mold isolates. Antimicrob Agents Chemother. 2007;51:748–51.
Cuenca-Estrella M, Gomez-Lopez A, Mellado E, Buitrago MJ, Monzon A, Rodriguez-Tudela JL. Head-to-head comparison of the activities of currently available antifungal agents against 3, 378 Spanish clinical isolates of yeasts and filamentous fungi. Antimicrob Agents Chemother. 2006;50:917–21.
Thornton CR. Tracking the emerging human pathogen Pseudallescheria boydii by using highly specific monoclonal antibodies. Clin Vaccine Immunol. 2009;16:756–64.
Zhou X, Kong F, Sorrell TC, Wang H, Duan Y, Chen SC. Practical method for detection and identification of Candida, Aspergillus, and Scedosporium spp by use of rolling-circle amplification. J Clin Microbiol. 2008;46:2423–7.
Acknowledgments
We thank the BCCM/IHEM Culture Collection for the molecular identification of strain IHEM 24840.
Conflict of Interest
The authors have no conflict of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Caggiano, G., Cantisani, P., Rolli, M. et al. The Importance of a Proper Aetiological Diagnosis in the Management of Patients with Invasive Mycoses: A Case Report of a Brain Abscess by Scedosporium apiospermum . Mycopathologia 172, 317–322 (2011). https://doi.org/10.1007/s11046-011-9436-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-011-9436-4