Abstract
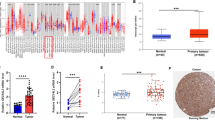
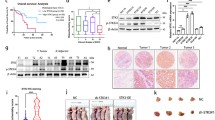
This study intended to investigate the expression of the ZEB1 and E-cadherin proteins in lung squamous cell carcinoma (LSCC) tissues and to examine the clinicopathological correlation between protein levels and LSCC. RT-PCR and Western blot were used to examine the expression of ZEB1 and E-cadherin mRNAs and proteins in LSCC tissues as well as in adjacent normal tissues, and then analyze the relationship between the clinicopathological characteristics and the expression changes of ZEB1 and E-cadherin mRNAs in LSCC. In addition, RNAi was used to knockdown the expression of the ZEB1 gene in Human HCC827 cells; subsequently, changes in the invasive ability of the resultant cells were studied. The positive rates of ZEB1 and E-cadherin mRNAs in LSCC tissues were 69.2 and 38.5 %, respectively. They differed significantly from the corresponding positive rates in the adjacent normal lung tissues (15.4 and 80.8 %, p < 0.05). There was a negative correlation between the protein levels of ZEB1 and E-cadherin in LSCC tissues (r = -0.714, p < 0.001); in addition, it was found that ZEB1 protein expression in LSCC tissues was significantly higher than that in the neighboring normal lung tissues (p < 0.05), and its expression was also significantly higher in patients with lymph node metastases and distant metastases compared to those patients without metastatic disease (p < 0.05). On the contrary, E-cadherin expression was significantly lower in LSCC tissues than that in the neighboring normal tissue (p < 0.05). It was lower in patients with lymph node metastasis and distant metastasis compared to patients without metastatic disease (p < 0.05). However, the expression of ZEB1 and E-cadherin was independent of gender, age, tumor size, or tumor differentiation level (p > 0.05). Transfection of ZEB1 siRNA into HCC827 cells significantly reduced the ZEB1 protein level (p < 0.01) and significantly elevated E-cadherin levels (p < 0.01). Moreover, significantly less ZEB1 siRNA-transfected cells migrated through Transwell chambers in the LSCC tissue than that in the control groups (untransfected or transfected with control siRNA, p < 0.01). The expression of the ZEB1 gene in LSCC tissues is downregulated with the expression of E-cadherin. On the other hand, the expression of siRNA against ZEB1 promotes E-cadherin expression and suppresses the invasive ability conferred by E-cadherin. In conclusion, our data suggested that overexpression of the ZEB1 gene is possibly associated with the occurrence, development, invasion of LSCC.


Similar content being viewed by others
References
Giangreco A, Groot KR, Janes SM (2007) Lung cancer and lung stem cells: strange bedfellows? Am J Respir Crit Care Med 175:547–553
Shao WL, Wang DY, He JX (2010) The role of gene expression profiling in early-stage non-small cell lung cancer. J Thorac Dis 2:89–99
Yang HH, Zhang Q, He JX, Lu WJ (2010) Regulation of calcium signaling in lung cancer. J Thorac Dis 2:52–56
Xiao DK, He JX (2010) Epithelial mesenchymal transition and lung cancer. J Thorac Dis 2:154–159
Korpanty G, Smyth E, Carney DN (2011) Update on anti-angiogenic therapy in non-small cell lung cancer: Are we making progress? J Thorac Dis 3:19–29
Shash E, Peccatori FA, Azim HA Jr (2011) Optimizing the use of epidermal growth factor receptor inhibitors in advanced non-small-lung cancer (NSCLC). J Thorac Dis 3:57–64
McKeage MJ, Jameson MB (2010) AS1404–201 study group investigators. Comparative outcomes of squamous and non-squamous non-small cell lung cancer (NSCLC) patients in phase II studies of ASA404 (DMXAA)—retrospective analysis of pooled data. J Thorac Dis 2:199–204
Yang P, Xu XY, Liu XJ, Gong JS (2011) The value of delayed 18F FDG-PET imaging in diagnosis of solitary pulmonary nodules: a preliminary study on 28 patients. Quant Imaging Med Surg 1:31–34
Stridh P, Thessen Hedreul M, Beyeen AD, Adzemovic MZ, Laaksonen H, Gillett A, Ockinger J, Marta M, Lassmann H, Becanovic K et al (2010) Fine-mapping resolves Eae23 into two QTLs and implicates ZEB1 as a candidate gene regulating experimental neuroinflammation in rat. PLoS ONE 5:e12716
Prager GW, Poettler M, Unseld M, Zielinski CC (2012) Angiogenesis in cancer: anti-VEGF escape mechanisms. Transl Lung Cancer Res 1:14–25
Vandewalle C, Comijn J, De Craene B, Vermassen P, Bruyneel E, Andersen H, Tulchinsky E, Van Roy F, Berx G (2005) SIP1/ZEB2 induces EMT by repressing genes of different epithelial cell–cell junctions. Nucleic Acids Res 33:6566–6578
Postigo AA, Depp JL, Taylor JJ, Kroll KL (2003) Regulation of Smad signaling through a differential recruitment of coactivators and corepressors by ZEB proteins. EMBO J 22:2453–2462
Hidaka T, Nakahata S, Hatakeyama K, Hamasaki M, Yamashita K, Kohno T, Arai Y, Taki T, Nishida K, Okayama A et al (2008) Down-regulation of TCF8 is involved in the leukemogenesis of adult T-cell leukemia/lymphoma. Blood 112:383–393
Postigo AA, Dean DC (1999) Independent repressor domains in ZEB regulate muscle and T-cell differentiation. Mol Cell Biol 19:7961–7971
Williams TM, Moolten D, Burlein J, Romano J, Bhaerman R, Godillot A, Mellon M, Rauscher FJ III, Kant JA (1991) Identification of a zinc finger protein that inhibits IL-2 gene expression. Science 254:1791–1794
Hsu FM, Zhang S, Chen BP (2012) Role of DNA-dependent protein kinase catalytic subunit in cancer development and treatment. Transl Cancer Res 1:22–34
Fontemaggi G, Gurtner A, Strano S, Higashi Y, Sacchi A, Piaggio G, Blandino G (2001) The transcriptional repressor ZEB regulates p73 expression at the crossroad between proliferation and differentiation. Mol Cell Biol 21:8461–8470
Putzke AP, Ventura AP, Bailey AM, Akture C, Opoku-Ansah J, Celiktas M, Hwang MS, Darling DS, Coleman IM, Nelson PS et al (2011) Metastatic progression of prostate cancer and e-cadherin regulation by zeb1 and SRC family kinases. Am J Pathol 179:400–410
Argast GM, Krueger JS, Thomson S, Sujka-Kwok I, Carey K, Silva S, O’Connor M, Mercado P, Mulford IJ, Young GD et al (2011) Inducible expression of TGFbeta, Snail and Zeb1 recapitulates EMT in vitro and in vivo in a NSCLC model. Clin Exp Metastasis 28(7):593–614
Lorenzatti G, Huang W, Pal A, Cabanillas AM, Kleer CG (2011) CCN6 (WISP3) decreases ZEB1-mediated EMT and invasion by attenuation of IGF-1 receptor signaling in breast cancer. J Cell Sci 124:1752–1758
Bao B, Wang Z, Ali S, Kong D, Li Y, Ahmad A, Banerjee S, Azmi AS, Miele L, Sarkar FH (2011) Notch-1 induces epithelial-mesenchymal transition consistent with cancer stem cell phenotype in pancreatic cancer cells. Cancer Lett 307:26–36
van Roy F, Berx G (2008) The cell–cell adhesion molecule E-cadherin. Cell Mol Life Sci 65:3756–3788
Rachagani S, Senapati S, Chakraborty S, Ponnusamy MP, Kumar S, Smith LM, Jain M, Batra SK (2011) Activated Kras (G12D) is associated with invasion and metastasis of pancreatic cancer cells through inhibition of E-cadherin. Br J Cancer 104:1038–1048
Erdem H, Gundogdu C, Sipal S (2011) Correlation of E-cadherin, VEGF, COX-2 expression to prognostic parameters in papillary thyroid carcinoma. Exp Mol Pathol 90(3):312–317
Saad AA, Awed NM, Abd Elkerim NN, El-Shennawy D, Alfons MA, Elserafy ME, Darwish YW, Barakat EM, Ezz-Elarab SS (2010) Prognostic significance of E-cadherin expression and peripheral blood micrometastasis in gastric carcinoma patients. Ann Surg Oncol 17:3059–3067
Muller A, Homey B, Soto H, Ge N, Catron D, Buchanan ME, McClanahan T, Murphy E, Yuan W, Wagner SN et al (2001) Involvement of chemokine receptors in breast cancer metastasis. Nature 410:50–56
Prager GW, Poettler M, Unseld M, Zielinski CC (2012) Angiogenesis in cancer: anti-VEGF escape mechanisms. Transl Lung Cancer Res 1:14–25
Lee JM, Dedhar S, Kalluri R, Thompson EW (2006) The epithelial-mesenchymal transition: new insights in signaling, development, and disease. J Cell Biol 172:973–981
Gemmill RM, Roche J, Potiron VA, Nasarre P, Mitas M, Coldren CD, Helfrich BA, Garrett-Mayer E, Bunn PA, Drabkin HA (2011) ZEB1-responsive genes in non-small cell lung cancer. Cancer Lett 300:66–78
Bateman G, Ricketts DN, Saunders WP (2003) Fibre-based post systems: a review. Br Dent J 195:43–48
Yu HG, Li JY, Yang YN, Luo HS, Yu JP, Meier JJ, Schrader H, Bastian A, Schmidt WE, Schmitz F (2003) Increased abundance of cyclooxygenase-2 correlates with vascular endothelial growth factor-A abundance and tumor angiogenesis in gastric cancer. Cancer Lett 195:43–51
Qian Y, Corum L, Meng Q, Blenis J, Zheng JZ, Shi X, Flynn DC, Jiang BH (2004) PI3 K induced actin filament remodeling through Akt and p70S6K1: implication of essential role in cell migration. Am J Physiol Cell Physiol 286:C153–C163
Eger A, Aigner K, Sonderegger S, Dampier B, Oehler S, Schreiber M, Berx G, Cano A, Beug H, Foisner R (2005) DeltaEF1 is a transcriptional repressor of E-cadherin and regulates epithelial plasticity in breast cancer cells. Oncogene 24:2375–2385
Adachi Y, Takeuchi T, Nagayama T, Ohtsuki Y, Furihata M (2009) Zeb1-mediated T-cadherin repression increases the invasive potential of gallbladder cancer. FEBS Lett 583:430–436
Postigo AA (2003) Opposing functions of ZEB proteins in the regulation of the TGFbeta/BMP signaling pathway. EMBO J 22:2443–2452
Nakahata S, Yamazaki S, Nakauchi H, Morishita K (2010) Downregulation of ZEB1 and overexpression of Smad7 contribute to resistance to TGF-beta1-mediated growth suppression in adult T-cell leukemia/lymphoma. Oncogene 29:4157–4169
Chung JH, Rho JK, Xu X, Lee JS, Yoon HI, Lee CT, Choi YJ, Kim HR, Kim CH, Lee JC (2011) Clinical and molecular evidences of epithelial to mesenchymal transition in acquired resistance to EGFR-TKIs. Lung Cancer 73(2):176–182
Guo BH, Feng Y, Zhang R, Xu LH, Li MZ, Kung HF, Song LB, Zeng MS (2011) Bmi-1 promotes invasion and metastasis, and its elevated expression is correlated with an advanced stage of breast cancer. Mol Cancer 10:10
Author information
Authors and Affiliations
Corresponding authors
Additional information
Jiaxing Zhang and Chenhui Lu contributed equally to this study.
Rights and permissions
About this article
Cite this article
Zhang, J., Lu, C., Zhang, J. et al. Involvement of ZEB1 and E-cadherin in the invasion of lung squamous cell carcinoma. Mol Biol Rep 40, 949–956 (2013). https://doi.org/10.1007/s11033-012-2136-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-012-2136-4