Abstract
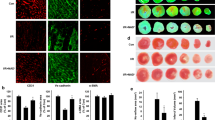
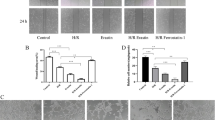
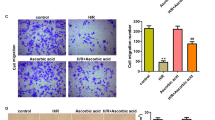
Endothelial-to-mesenchymal transition (EndMT) has been reported as a key factor in myocardial fibrosis. Acetylcholine (ACh), a neurotransmitter of the vagus nerve, has been confirmed to exert cardio-protective properties with unclear mechanisms. In this study, the specific markers of cell injury, EndMT, inflammation, and autophagy were measured. We found that treatment with ACh prevented hypoxia-induced cell viability reduction and apoptosis in human cardiac microvascular endothelial cells (HCMECs). Additionally, our results indicate that pre-treatment with ACh significantly suppresses hypoxia-induced EndMT and NF-κB activation in HCMECs. ACh also reduced hypoxia-inducible factor (HIF)-1ɑ protein levels under hypoxia. Knock down of HIF-1ɑ enhanced the inhibitory effect of ACh on NF-κB activation. The NF-κB-specific small molecule inhibitor BAY 11-7082, prostaglandin E2, and LY294002 prevented hypoxia-induced EndMT. Moreover, our data show that hypoxia triggers autophagy in HCMECs, and ACh significantly upregulates autophagy activity. Pre-treatment of HCMECs with 3-methyladenine or chloroquine partially reversed ACh-induced EndMT inhibition. These results suggest that ACh may confer protection against hypoxia-induced EndMT through the inhibition of NF-κB and the induction of autophagy.




Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
Abbreviations
- α-SMA:
-
α-Smooth muscle actin
- Ach:
-
Acetylcholine
- AMI:
-
Acute myocardial infarction
- ECM:
-
Extracellular matrix
- EMT:
-
Epithelial-to-mesenchymal transition
- EndMT:
-
Endothelial-to-mesenchymal transition
- HCAECs:
-
Human coronary artery endothelial cells
- HCMECs:
-
Human cardiac microvascular endothelial cells
- HUVECs:
-
Human umbilical vein endothelial cells
- MF:
-
Myocardial fibrosis
- PBS:
-
Phosphate buffered saline
- PECAM-1:
-
Platelet endothelial cell adhesion molecule-1
- TEM:
-
Transmission electron microscopy
- VE-cad:
-
Vascular endothelial cadherin
References
Heusch G, Libby P, Gersh B, Yellon D, Böhm M, Lopaschuk G, Opie L (2014) Cardiovascular remodelling in coronary artery disease and heart failure. Lancet 383:1933–1943. https://doi.org/10.1016/S0140-6736(14)60107-0
Tissier A, Morgan JA, Dudareva N (2017) Plant volatiles: going 'In' but not 'Out' of trichome cavities. Trends Plant Sci 22:930–938. https://doi.org/10.1016/j.tplants.2017.09.001
Allawadhi P, Khurana A, Sayed N, Kumari P, Godugu C (2018) Isoproterenol-induced cardiac ischemia and fibrosis: plant-based approaches for intervention. Phytother Res 32:1908–1932. https://doi.org/10.1002/ptr.6152
Chen PY, Qin L, Baeyens N, Li G, Afolabi T, Budatha M, Tellides G, Schwartz MA, Simons M (2015) Endothelial-to-mesenchymal transition drives atherosclerosis progression. J Clin Invest 125:4514–4528. https://doi.org/10.1172/JCI82719
Correia AC (2016) Moonen J-RAJ, Brinker MGL, Krenning G, FGF2 inhibits endothelial-mesenchymal transition through microRNA-20a-mediated repression of canonical TGF-beta signaling. J Cell Sci 129:569–579. https://doi.org/10.1242/jcs.176248
Flier SN, Tanjore H, Kokkotou EG, Sugimoto H, Zeisberg M, Kalluri R (2010) Identification of epithelial to mesenchymal transition as a novel source of fibroblasts in intestinal fibrosis. J Biol Chem 285:20202–20212. https://doi.org/10.1074/jbc.M110.102012
Kisanuki YY, Hammer RE, Miyazaki J, Williams SC, Richardson JA, Yanagisawa M (2001) Tie2-Cre transgenic mice: a new model for endothelial cell-lineage analysis in vivo. Dev Biol 230:230–242. https://doi.org/10.1006/dbio.2000.0106
Chen PY, Simons M (2016) When endothelial cells go rogue. Embo Mol Med 8:1–2. https://doi.org/10.15252/emmm.201505943
Arciniegas E, Frid MG, Douglas IS, Stenmark KR (2007) Perspectives on endothelial-to-mesenchymal transition: potential contribution to vascular remodeling in chronic pulmonary hypertension. Am J Physiol Lung Cell Mol Physiol 293:L1–L8. https://doi.org/10.1152/ajplung.00378.2006
Peinado H, Olmeda D, Cano A (2007) Snail, Zeb and bHLH factors in tumour progression: an alliance against the epithelial phenotype? Nat Rev Cancer 7:415–428. https://doi.org/10.1038/nrc2131
Xu X, Tan X, Tampe B, Sanchez E, Zeisberg M, Zeisberg EM (2015) Snail is a direct target of hypoxia-inducible factor 1alpha (HIF1alpha) in hypoxia-induced endothelial to mesenchymal transition of human coronary endothelial cells. J Biol Chem 290:16653–16664. https://doi.org/10.1074/jbc.M115.636944
Fleenor BS, Marshall KD, Rippe C, Seals DR (2012) Replicative aging induces endothelial to mesenchymal transition in human aortic endothelial cells: potential role of inflammation. J Vasc Res 49:59–64. https://doi.org/10.1159/000329681
Kroemer G, Marino G, Levine B (2010) Autophagy and the integrated stress response. Mol Cell 40:280–293. https://doi.org/10.1016/j.molcel.2010.09.023
Zou J, Liu Y, Li B, Zheng Z, Ke X, Hao Y, Li X, Li X, Liu F, Zhang Z (2017) Autophagy attenuates endothelial-to-mesenchymal transition by promoting Snail degradation in human cardiac microvascular endothelial cells. Biosci Rep. https://doi.org/10.1042/BSR20171049
Liu Y, Zou J, Li B, Wang Y, Wang D, Hao Y, Ke X, Li X (2017) RUNX3 modulates hypoxia-induced endothelial-to-mesenchymal transition of human cardiac microvascular endothelial cells. Int J Mol Med 40:65–74. https://doi.org/10.3892/ijmm.2017.2998
Good RB, Gilbane AJ, Trinder SL, Denton CP, Coghlan G, Abraham DJ, Holmes AM (2015) Endothelial to mesenchymal transition contributes to endothelial dysfunction in pulmonary arterial hypertension. Am J Pathol 185:1850–1858. https://doi.org/10.1016/j.ajpath.2015.03.019
Sena CM, Pereira AM, Seica R (1832) Endothelial dysfunction—a major mediator of diabetic vascular disease. Biochim Biophys Acta 2013:2216–2231. https://doi.org/10.1016/j.bbadis.2013.08.006
Lee JG, Ko MK, Kay EP (2012) Endothelial mesenchymal transformation mediated by IL-1β-induced FGF-2 in corneal endothelial cells. Exp Eye Res 95:35–39. https://doi.org/10.1016/j.exer.2011.08.003
Kanaji N, Sato T, Nelson A, Wang X, Li Y, Kim M, Nakanishi M, Basma H, Michalski J, Farid M, Chandler M, Pease W, Patil A, Rennard SI, Liu X (2011) Inflammatory cytokines regulate endothelial cell survival and tissue repair functions via NF-κB signaling. J Inflamm Res 4:127–138. https://doi.org/10.2147/JIR.S19461
Maleszewska M (2013) Moonen J-RAJ, Huijkman N, van de Sluis B, Krenning G, Harmsen MC, IL-1β and TGFβ2 synergistically induce endothelial to mesenchymal transition in an NFκB-dependent manner. Immunobiology 218:443–454. https://doi.org/10.1016/j.imbio.2012.05.026
Song S, Ji Y, Zhang G, Zhang X, Li B, Li D, Jiang W (2018) Protective effect of atazanavir sulphate against pulmonary fibrosis in vivo and in vitro. Basic Clin Pharmacol Toxicol 122:199–207. https://doi.org/10.1111/bcpt.12871
Semenza GL (2001) HIF-1, O(2), and the 3 PHDs: how animal cells signal hypoxia to the nucleus. Cell 107(1):1–3. https://doi.org/10.1016/s0092-8674(01)00518-9
Krieg T, Qin Q, Philipp S, Alexeyev MF, Cohen MV, Downey JM (2004) Acetylcholine and bradykinin trigger preconditioning in the heart through a pathway that includes Akt and NOS. Am J Physiol Heart Circ Physiol 287:H2606–H2611. https://doi.org/10.1152/ajpheart.00600.2004
Cockman ME, Lancaster DE, Stolze IP, Hewitson KS, McDonough MA, Coleman ML, Coles CH, Yu X, Hay RT, Ley SC, Pugh CW, Oldham NJ, Masson N, Schofield CJ, Ratcliffe PJ (2006) Posttranslational hydroxylation of ankyrin repeats in IkappaB proteins by the hypoxia-inducible factor (HIF) asparaginyl hydroxylase, factor inhibiting HIF (FIH). Proc Natl Acad Sci USA 103:14767–14772. https://doi.org/10.1073/pnas.0606877103
Cummins EP, Berra E, Comerford KM, Ginouves A, Fitzgerald KT, Seeballuck F, Godson C, Nielsen JE, Moynagh P, Pouyssegur J, Taylor CT (2006) Prolyl hydroxylase-1 negatively regulates IkappaB kinase-beta, giving insight into hypoxia-induced NFkappaB activity. Proc Natl Acad Sci USA 103:18154–18159. https://doi.org/10.1073/pnas.0602235103
Netea-Maier RT, Plantinga TS, van de Veerdonk FL, Smit JW, Netea MG (2016) Modulation of inflammation by autophagy: consequences for human disease. Autophagy 12:245–260. https://doi.org/10.1080/15548627.2015.1071759
Kroemer G, Marino G, Levine B (2010) Autophagy and the integrated stress response. Mol Cell 40:P280–P293. https://doi.org/10.1016/j.molcel.2010.09.023
Wu X, He L, Chen F, He X, Cai Y, Zhang G, Yi Q, He M, Luo J (2014) Impaired autophagy contributes to adverse cardiac remodeling in acute myocardial infarction. PLoS ONE 9:e112891. https://doi.org/10.1371/journal.pone.0112891
Kanamori H, Takemura G, Goto K, Maruyama R, Tsujimoto A, Ogino A, Takeyama T, Kawaguchi T, Watanabe T, Fujiwara T, Fujiwara H, Seishima M, Minatoguchi S (2011) The role of autophagy emerging in postinfarction cardiac remodelling. Cardiovasc Res 91:330–339. https://doi.org/10.1093/cvr/cvr073
Roy A, Guatimosim S, Prado VF, Gros R, Prado MA (2015) Cholinergic activity as a new target in diseases of the heart. Mol Med 20:527–537. https://doi.org/10.2119/molmed.2014.00125
Hoover DB, Ganote CE, Ferguson SM, Blakely RD, Parsons RL (2004) Localization of cholinergic innervation in guinea pig heart by immunohistochemistry for high-affinity choline transporters. Cardiovasc Res 62:112–121. https://doi.org/10.1016/j.cardiores.2004.01.012
Kakinuma Y, Tsuda M, Okazaki K, Akiyama T, Arikawa M, Noguchi T, Sato T (2013) Heart-specific overexpression of choline acetyltransferase gene protects murine heart against ischemia through hypoxia-inducible factor-1alpha-related defense mechanisms. J Am Heart Assoc 2:e004887. https://doi.org/10.1161/JAHA.112.004887
Zhang R, Wugeti N, Sun J, Yan H, Guo Y, Zhang L, Ma M, Guo X, Jiao C, Xu W, Li T, Liu H, Ma Y (2014) Effects of vagus nerve stimulation via cholinergic anti-inflammatory pathway activation on myocardial ischemia/reperfusion injury in canine. Int J Clin Exp Med 7:2615–2623
Acknowledgements
This work was supported by the National Natural Science Foundation of China (Grant No. 81860052, 81871113).
Author information
Authors and Affiliations
Contributions
All the authors participated in the design, interpretation of the data, drafting and review of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, Z., Li, X., Zhu, Y. et al. Protective effects of acetylcholine on hypoxia-induced endothelial-to-mesenchymal transition in human cardiac microvascular endothelial cells. Mol Cell Biochem 473, 101–110 (2020). https://doi.org/10.1007/s11010-020-03811-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-020-03811-w