Abstract
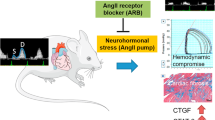
To determine whether therapy with the angiotensin II type 1 receptor blocker (ARB) candesartan and the comparator angiotensin-converting-enzyme inhibitor (ACEI) enalapril during healing after reperfused ST-elevation myocardial infarction (RSTEMI) limit adverse remodeling of infarct zone (IZ) collagens and left ventricular (LV) diastolic dysfunction, we randomized 24 dogs surviving anterior RSTEMI (90-min coronary occlusion) to placebo, candesartan, and enalapril therapy between day 2 and 42. Six other dogs were sham. We measured regional IZ and non-infarct zone (NIZ) collagens (hydroxyproline; types I/III; cross-linking), transforming growth factor-β (TGF-β) and topography at 6 weeks, and hemodynamics, LV diastolic and systolic function, and remodeling over 6 weeks. Compared to sham, placebo-RSTEMI differentially altered regional collagens, with more pronounced increase in TGF-β, hydroxyproline, and type I, insoluble, and cross-linked collagens in the IZ than NIZ, and increased IZ soluble and type III collagens at 6 weeks, and induced persistent LV filling pressure elevation, diastolic and systolic dysfunction, and LV remodeling over 6 weeks. Compared to placebo-RSTEMI, candesartan and enalapril limited adverse regional collagen remodeling, with normalization of type III, soluble and insoluble collagens and decrease in pyridinoline cross-linking in the IZ at 6 weeks, and attenuation of LV filling pressure, diastolic dysfunction, and remodeling over 6 weeks. The results suggest that candesartan and enalapril during healing after RSTEMI prevent rather than worsen adverse remodeling of IZ collagens and LV diastolic dysfunction, supporting the clinical use of ARBs and ACEIs during subacute RSTEMI.






Similar content being viewed by others
References
Kloner RA, Ellis SG, Lange R et al (1983) Studies of experimental coronary artery reperfusion: effects on infarct size, myocardial function, biochemistry, ultrastructure and microvascular damage. Circulation 68(suppl I):I8–15
Murakami T, Kusachi S, Murakami M et al (1998) Time-dependent changes of serum carboxy-terminal peptide of type I procollagen and carboxy-terminal telopeptide of type I collagen concentrations in patients with acute myocardial infarction after successful reperfusion: correlation with left ventricular volume indices. Clin Chem 44:2453–2461
Frangogiannis NG, Mendoza LH, Lindsey ML et al (2000) IL-10 is induced in the reperfused myocardium and may modulate the reaction to injury. J Immunol 165:2798–2808
Jugdutt BI (1997) Effect of reperfusion on ventricular mass, topography and function during healing of anterior infarction. Am J Physiol 272:H1205–H1211
Zhao MJ, Zhang H, Robinson TF et al (1987) Profound structural alterations of the extracellular collagen matrix in postischemic dysfunctional (“stunned”) but viable myocardium. J Am Coll Cardiol 10:1322–1334
Sawicki G, Menon V, Jugdutt BI (2004) Improved balance between TIMP-3 and MMP-9 after regional myocardial ischemia-reperfusion during AT1 receptor blockade. J Card Fail 10:442–449
Connelly CM, Vogel WM, Wiegner AW et al (1985) Effects of reperfusion after coronary artery occlusion on post-infarction scar tissue. Circ Res 57:562–577
Boyle MP, Weisman HF (1993) Limitation of infarct expansion and ventricular remodeling by late reperfusion. Study of time course and mechanism in a rat model. Circulation 88:2872–2883
Bolognese L, Neskovic AN, Parodi G et al (2002) Left ventricular remodeling after primary coronary angioplasty: patterns of left ventricular dilation and long-term prognostic implications. Circulation 106:2351–2357
The SOLVD Investigators (1991) Effect of enalapril on survival in patients with reduced left ventricular ejection fractions and congestive heart failure. N Engl J Med 325:293–302
Pfeffer MA, Swedberg K, Granger CB et al;CHARM Investigators and Committees (2003) Effects of candesartan on mortality and morbidity in patients with chronic heart failure: the CHARM-Overall programme. Lancet 362:759–766
Pfeffer MA, Braunwald E, Moye LA et al (1992) Effect of captopril on mortality and morbidity in patients with left ventricular dysfunction after myocardial infarction. The SAVE Investigators. N Engl J Med 327:669–677
St John Sutton M, Pfeffer MA, Plappert T et al for the SAVE Investigators (1994) Quantitative two-dimensional echocardiographic measurements are major predictors of adverse cardiovascular events after acute myocardial infarction. The protective effects of captopril. Circulation 89:68–75
Pfeffer MA, McMurray JJ, Velazquez EJ et al;Valsartan in Acute Myocardial Infarction Trial Investigators (2003) Valsartan, captopril, or both in myocardial infarction complicated by heart failure, left ventricular dysfunction, or both. N Engl J Med 349:1893–1906
Solomon SD, Skali H, Anavekar NS et al (2005) Changes in ventricular size and function in patients treated with valsartan, captopril, or both after myocardial infarction. Circulation 111:3411–3419
Jugdutt BI, Lucas A, Khan MI (1997) Effect of ACE inhibition on infarct collagen deposition and remodeling during healing after transmural canine myocardial infarction. Can J Cardiol 13:657–668
van Krimpen C, Schoemaker RG, Cleutjens JP et al (1991) Angiotensin I converting enzyme inhibitors and cardiac remodeling. Basic Res Cardiol 86:149–155
Jugdutt BI (2003) Ventricular remodeling postinfarction and the extracellular collagen matrix. When is enough enough? Circulation 108:1395–1403
Smits JF, van Krimpen C, Schoemaker RG et al (1992) Angiotensin II receptor blockade after myocardial infarction in rats: effects on hemodynamics, myocardial DNA synthesis, and interstitial collagen content. J Cardiovasc Pharmacol 20:772–778
Schoemaker RG, Debets JJ, Struyker-Boudier HA et al (1991) Delayed but not immediate captopril therapy improves cardiac function in conscious rats, following myocardial infarction. J Mol Cell Cardiol 23:187–197
Diez J, Querejeta R, Lopez B et al (2002) Losartan-dependent regression of myocardial fibrosis is associated with reduction of left ventricular chamber stiffness in hypertensive patients. Circulation 105:2512–2517
Yoshida J, Yamamoto K, Mano T et al (2004) AT1 receptor blocker added to ACE inhibitor provides benefits at advanced stage of hypertensive diastolic heart failure. Hypertension 43:686–691
Jugdutt BI, Menon V, D. Kumar et al (2002) Vascular remodeling during healing after reperfused myocardial infarction in the dog model. Effects of reperfusion, amlodipine and enalapril. J Am Coll Cardiol 39:1538–1545
Jugdutt BI, Xu Y, Balghith M et al (2001) Cardioprotective effects of angiotensin II type 1 receptor blockade with candesartan after reperfused myocardial infarction: role of angiotensin II type 2 receptor. JRAAS 2:S162–S166
Jugdutt BI, Khan MI, Jugdutt SJ et al (1995) Effect of enalapril on ventricular remodeling and function during healing after anterior myocardial infarction in the dog. Circulation 91:802–812
Jugdutt BI (1997) Effect of amlodipine versus enalapril on left ventricular remodeling after anterior reperfused myocardial infarction. Can J Cardiol 13:945–954
Jugdutt BI, Joljart MJ, Khan MI (1996) Rate of collagen deposition during healing after myocardial infarction in the rat and dog models: mechanistic insights into ventricular remodeling. Circulation 94:94–101
Klotz S, Foronjy RF, Dickstein ML et al (2005) Mechanical unloading during left ventricular assist device support increases left ventricular collagen cross-linking and myocardial stiffness. Circulation 112:364–374
Miller EJ, Rhodes RK (1982) Preparation and characterization of the different types of collagen. Method Enzymol 82(Pt A):33–64
Stegemann H, Stalder K (1967) Determination of hydroxyproline. Clin Chim Acta 18:267–273
Laurent GJ, Cockerill P, McAnulty RJ et al (1981) A simplified method for quantitation of the relative amounts of type I and type III collagen in small tissue samples. Anal Biochem 113:301–312
Cleutjens JP, Verluyten MJ, Smits JF et al (1995) Collagen remodeling after myocardial infarction in the rat heart. Am J Pathol 147:325–338
Sekita S, Katagiri T, Sasai Y et al (1985) Studies on collagen in the experimental myocardial infarction. Jpn Circ J 49:171–178
Whittaker P, Boughner DR, Kloner RA (1989) Analysis of healing after myocardial infarction using polarized light microscopy. Am J Pathol 134:879–893
Yu CM, Tipoe GL, Wing-Hon Lai K et al (2001) Effects of combination of angiotensin-converting enzyme inhibitor and angiotensin receptor antagonist on inflammatory cellular infiltration and myocardial interstitial fibrosis after acute myocardial infarction. J Am Coll Cardiol 38:1207–1215
Sun Y, Zhang JQ, Zhang J et al (1998) Angiotensin II, transforming growth factor-beta1 and repair in the infarcted heart. J Mol Cell Cardiol 30:1559–1569
Eghbali M, Tomek R, Sukhatme VP et al (1991) Differential effects of transforming growth factor-beta 1 and phorbol myristate acetate on cardiac fibroblasts. Regulation of fibrillar collagen mRNAs and expression of early transcription factors. Circ Res 69:483–490
Balghith M, Jugdutt BI (2002) Assessment of diastolic dysfunction after acute myocardial infarction using Doppler Echocardiography. Can J Cardiol 18:69–77
Acknowledgments
A grant to B. Jugdutt from the Canadian Institutes of Health Research, Ottawa, ON supported this work. We thank AstraZeneca and Merck-Frosst for gifts of candesartan and enalapril, respectively, technicians with data collection, and Catherine Graham with manuscript preparation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jugdutt, B.I., Idikio, H. & Uwiera, R.R.E. Angiotensin receptor blockade and angiotensin-converting-enzyme inhibition limit adverse remodeling of infarct zone collagens and global diastolic dysfunction during healing after reperfused ST-elevation myocardial infarction. Mol Cell Biochem 303, 27–38 (2007). https://doi.org/10.1007/s11010-007-9452-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-007-9452-3