Abstract
Background
Low birth weight (LBW) is associated with significant mortality and morbidity and remains a significant preventable problem. Risk factors include socioeconomic, demographics, and characteristics of the environment. Spatial analysis can uncover unusual frequencies of health problems in neighborhoods, eventually leading to insights for targeted interventions.
Objectives
This study's goals were to 1. Evaluate the geographic distribution of spatial clusters of LBW births and maternal risk factors. 2. Determine the spatial relationship between risk factors and LBW.
Methods
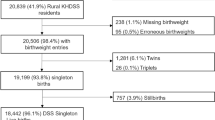
This study obtained data on LBW newborns and risk factors from 19,013 births over 5 years (2012–2016) for Escambia County Census Tracts, extracted from FloridaCharts.com. Software was used to detect significant spatial clusters; these clusters were then plotted on a map. Poisson regression determined the statistical relationship between Census Tract risk factors and LBW. A separate analysis of the LBW cluster controlling for risk factors was also performed.
Results
All risk factor clusters resided in similar locations as the LBW cluster. The multiple Poisson regression model containing all risk factors fully explained the LBW cluster. On bivariate Poisson regression all risk factors in the Census Tract were significantly related to LBW whereas in multivariable Poisson regression, the proportion of births to African American women in the Census Tract remained significant after adjusting for other risk factors (p < 0.001).
Conclusions for Practice
Clusters of LBW and risk factors were located in the same region of the county, with the proportion of births to African American women in the Census Tract remaining significant on multiple Poisson Regression. Targeted interventions should be directed at the geographic level.


Similar content being viewed by others
References
Agrawal, A., Scherrer, J. F., Grant, J. D., Sartor, C. E., Pergadia, M. L., Duncan, A. E., et al. (2010). The effects of maternal smoking during pregnancy on offspring outcomes. Preventive Medicine,50, 1–2.
Anthopolos, R., James, S. A., Gelfand, A. E., & Miranda, M. L. (2011). A spatial measure of neighborhood level racial isolation applied to low birthweight, preterm birth, and birthweight in North Carolina. Spat Spatiotemporal Epidemiol.,2, 235–246.
Buekens, P., Wilcox, A. J., Kiely, J., & Masuy-Stroobant, G. (1995). Birthweight, preterm births and neonatal mortality in Belgium and the United States. Paediatric and Perinatal Epidemiology,9, 273–280.
Buka, S., Brennan, R., Rich-Edwards, J., Raudenbush, S., & Earls, F. (2003). Neighborhood support and birth weight of urban infants. American Journal of Epidemiology, 157, 1–8.
Cnattingius, S. (2004). The epidemiology of smoking during pregnancy: Smoking prevalence, maternal characteristics, and pregnancy outcomes. Nicotine Tob Res. Suppl,2, S125–S140.
Cromley, R. G., & Cromley, E. K. (2009). Choropleth map legend design for visualizing community health disparities. Int J of Health Geogr.,8, 52.
David, R. J. (1980). The quality and completeness of birthweight and gestational age data in computerized birth files. American Journal of Public Health,70, 964–973.
Daw, J. R., & Sommers, B. D. (2018). Association of the affordable care act dependent coverage provision with prenatal care use and birth outcomes. JAMA,319, 579–587.
English, P. B., Kharrazi, M., Davies, S., Scalf, R., Waller, L., & Neutra, R. (2003). Changes in the spatial pattern of low birth weight in a southern California county: The role of individual and neighborhood level factors. Social Science and Medicine,1982(56), 2073–2088.
Grady, S. C. (2010). Racial residential segregation impacts on low birth weight using improved neighborhood boundary definitions. Spat Spatiotemporal Epidemiol.,1, 239–249.
Grossman, D. C., Baldwin, L. M., Casey, S., Nixon, B., Hollow, W., & Hart, L. G. (2002). Disparities in infant health among American Indians and Alaska natives in US metropolitan areas. Pediatrics,109, 627–633.
Healthy People 2020: Maternal and Child Health. Published website: https://www.healthypeople.gov/2020/topics-objectives/topic/maternal-infant-and-child-health/objectives.
Herbst, M. A., Mercer, B. M., Beazley, D., Meyer, N., & Carr, T. (2003). Relationship of prenatal care and perinatal morbidity in low-birth-weight infants. American Journal of Obstetrics and Gynecology,189, 930–933.
Insaf, T. Z., & Talbot, T. (2016). Identifying areas at risk of low birth weight using spatial epidemiology: A small area surveillance study. Preventive Medicine,88, 108–114.
Kotelchuck, M. (1994). An evaluation of the Kessner Adequacy of Prenatal Care Index and a proposed Adequacy of Prenatal Care Utilization Index. American Journal of Public Health, 84(9), 1414–1420.
Kulldorff, M., Huang, L., & Konty, K. (2009). A scan statistic for continuous data based on the normal probability model. International Journal of Health Geographics, 8, 58.
Kulldorff, M. (2018). SaTScan™ version 9; Software for the spatial and space-time scan statistics. https://www.SaTScan.org.
Lee, H., Yoon, S. J., Ahn, H., Ha, M., Koh, K. S., & June, K. J. (2004). A survey on prenatal environmental risk factors for mothers of low birth weight infants in Asian-city. J Prev Med Public Health,37, 11–16.
Liu, L., Johnson, H. L., Cousens, S., Perin, J., Scott, S., Lawn, J. E., et al. (2012). Global, regional, and national causes of child mortality: An updated systematic analysis for 2010 with time trends since 2000. Lancet,379, 2151–2161.
Michielutte, R., Ernest, J., Moore, M., Meis, P., Sharp, P., Wells, J., & Buescher, P. (1992). A comparison of risk assessment models for term and preterm low birthweight. Preventive Medicine, 21(1), 98–109.
Mkandawire-Valhmu, L., Lathen, L., Baisch, M. J., Cotton, Q., Dressel, A., Antilla, J., … Hess, A. (2018). Enhancing Healthier Birth Outcomes by Creating Supportive Spaces for Pregnant African American Women Living in Milwaukee. Matern Child Health J, 22(12), 1797-1804.https://doi.org/10.1007/s10995-018-2580-4
Moore, M. L., Michielutte, R., Meis, P. J., Ernest, J. M., Wells, H. B., & Buescher, P. A. (1994). Etiology of low-birthweight birth: A population-based study. Preventive Medicine,23(6), 793–799.
Mustafa, G., & David, R. J. (2001). Comparative accuracy of clinical estimates versus menstrual gestational age in computerized birth certificates. Public Health Reports,116, 15–21.
Ncube, C. N., Enquobahrie, D. A., Albert, S. M., Herrick, A. L., & Burke, J. G. (2016). Association of neighborhood context with offspring risk of preterm birth and low birthweight: A systematic review and meta-analysis of population-based studies. Social Science and Medicine,1982(153), 156–164.
Nowak, A. L., & Giurgescu, C. (2017). The built environment and birth outcomes: A systematic review. MCN; American Journal of Maternal Child Nursing,42(1), 14–20. https://doi.org/10.1097/nmc.0000000000000299.
Ohlsson, A., & Prakeshkumar, S. (2008). Determinants and Prevention of Low Birth Weight. A Synopsis of the Evidence. Edmonto: Institute of Health Economics (IHE).
Pillas, D., Marmot, M., Naicker, K., Goldblatt, P., Morrison, J., & Pikhart, H. (2014). Social inequalities in early childhood health and development: A European-wide systematic review. Pediatric Research,76(5), 418–424. https://doi.org/10.1038/pr.2014.122.
Ruiz, M., Goldblatt, P., Morrison, J., Kukla, L., Svancara, J., Riitta-Jarvelin, M., … Pikhart, H. (2015). Mother's education and the risk of preterm and small for gestational age birth: a DRIVERS meta-analysis of 12 European cohorts. J Epidemiol Community Health, 69(9), 826-833.https://doi.org/10.1136/jech-2014-205387
Schaaf, J. M., Liem, S. M., Mol, B. W., Abu-Hanna, A., & Ravelli, A. C. (2013). Ethnic and racial disparities in the risk of preterm birth: A systematic review and meta-analysis. American Journal of Perinatology,30, 433–450.
Schoen, C. N., Tabbah, S., Iams, J. D., Caughey, A. B., & Berghella, V. (2015). Why the United States preterm birth rate is declining. American Journal of Obstetrics and Gynecology,213, 175–180.
Tayebi, T., Hamzehgardeshi, Z., Ahmad, S. M., Dayhimi, M., & Danesh, M. (2014). Relationship between Revised Graduated Index (R-GINDEX) of prenatal care utilization & preterm labor and low birth weight. Glob J Health Sci.,6, 131–137.
Veisani, Y., Jenabi, E., Delpisheh, A., & Khazaei, S. (2019). Effect of prenatal smoking cessation interventions on birth weight: meta-analysis. J Matern Fetal Neonatal Med,32(2), 332–338. https://doi.org/10.1080/14767058.2017.1378335.
Vintzileos, A., Ananth, C. V., Smulian, J. C., Scorza, W. E., & Knuppel, R. A. (2002). The impact of prenatal care on postneonatal deaths in the presence and absence of antenatal high-risk conditions. American Journal of Obstetrics and Gynecology,187, 1258–1262.
Xaverius, P., Alman, C., Holtz, L., & Yarber, L. (2016). Risk factors associated with very low birth weight in a large urban area, stratified by adequacy of prenatal care. Mat Child Health Journal,20, 623–629.
Yaya, S., Bishwajit, G., Ekholuenetale, M., & Shah, V. (2017). Inadequate utilization of prenatal care services, socioeconomic status, and educational attainment are associated with low birth weight in zimbabwe. Front Public Health,5, 35.
Acknowledgements
We appreciate the collaboration between the authors and Theresa Chmiel BA, Executive Director at Escambia County Healthy Start Coalition.
Funding
The authors do not have any financial relationship with any industry and no industry sponsored this research. This research had no funding other than time provided by the University of Florida College of Medicine.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Burns, J.J., Livingston, R. & Amin, R. The Proximity of Spatial Clusters of Low Birth Weight and Risk Factors: Defining a Neighborhood for Focused Interventions. Matern Child Health J 24, 1065–1072 (2020). https://doi.org/10.1007/s10995-020-02946-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-020-02946-y