Abstract
Introduction
Pregnant women initiating antiretroviral therapy (ART) in sub-Saharan Africa have been shown to have sub-optimal engagement in care, particularly after delivery, and interventions to improve engagement in care for this unique population are urgently needed.
Methods
We enrolled 25 pregnant women living with HIV at each of two large antenatal clinics in Johannesburg and Cape Town, South Africa (n = 50), and conducted in-depth interviews. We assessed participants’ reported acceptability of the following proposed interventions to improve engagement in care and retention monitoring data systems: financial incentives, educational toys, health education, combined maternal/infant visits, cell phone text reminders, mobility tracking, fingerprint/biometric devices, and smartcards.
Results
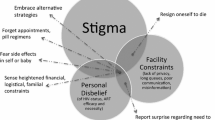
Acceptability overall for interventions was high, with mixed responses for some interventions. Overall themes identified included (i) the intersection of individual and facility responsibility for a patient’s health, (ii) a call for more health education, (iii) issues of disclosure and concerns about privacy, and (iv) openness to interventions that could improve health systems.
Discussion
These findings provide insight into the preferences and concerns of potential users of interventions to improve engagement in HIV care for pregnant women, and support the development of tools that specifically target this high-risk group.
Similar content being viewed by others
References
Ambia, J., & Mandala, J. (2016). A systematic review of interventions to improve prevention of mother-to-child HIV transmission service delivery and promote retention. Journal of the International AIDS Society, 19(1), 20309.
An, S. J., George, A. S., LeFevre, A., Mpembeni, R., Mosha, I., Mohan, D., et al. (2015). Program synergies and social relations: Implications of integrating HIV testing and counselling into maternal health care on care seeking. BMC Public Health, 15(1), 24. https://doi.org/10.1186/s12889-014-1336-3.
Bandura, A. (2001). Social cognitive theory: An agentic perspective. Annual Review of Psychology, 52(1), 1–26.
Bärnighausen, T., Chaiyachati, K., Chimbindi, N., Peoples, A., Haberer, J., & Newell, M.-L. (2011). Interventions to increase antiretroviral adherence in sub-Saharan Africa: A systematic review of evaluation studies. The Lancet Infectious Diseases, 11(12), 942–951.
Bogart, L. M., Chetty, S., Giddy, J., Sypek, A., Sticklor, L., Walensky, R. P., et al. (2012). Barriers to care among people living with HIV in South Africa: Contrasts between patient and healthcare provider perspectives. AIDS Care, 25(7), 843–853.
Chaiyachati, K. (2014). Interventions to improve adherence to antiretroviral therapy: A rapid systematic review. AIDS, 28, S187–S204. https://doi.org/10.1097/QAD.0000000000000252ISSN.
Chamie, G., Schaffer, E. M., Ndyabakira, A., Emperador, D. M., Kwarisiima, D., Camlin, C. S., et al. (2018). Comparative effectiveness of novel nonmonetary incentives to promote HIV testing. AIDS, 32(11), 1443–1451.
Clouse, K., Mongwenyana, C., Musina, M., Bokaba, D., Long, L., Maskew, M., et al. (2018). Acceptability and feasibility of a financial incentive intervention to improve retention in HIV care among pregnant women in Johannesburg, South Africa. AIDS Care, 30(4), 453–460.
Clouse, K., Pettifor, A., Shearer, K., Maskew, M., Bassett, J., Larson, B., et al. (2013). Loss to follow-up before and after delivery among women testing HIV positive during pregnancy in Johannesburg, South Africa. Tropical Medicine and International Health, 18(4), 451–460.
Clouse, K., Schwartz, S., Van Rie, A., Bassett, J., Yende, N., & Pettifor, A. (2014). What they wanted was to give birth; nothing else: Barriers to retention in option B + HIV care among postpartum women in South Africa. Journal of Acquired Immune Deficiency Syndromes, 67(1), e12–e18.
Clouse, K., Vermund, S. H., Maskew, M., Lurie, M. N., MacLeod, W., Malete, G., et al. (2017). Mobility and clinic switching among postpartum women considered lost to HIV care in South Africa. Journal of Acquired Immune Deficiency Syndromes, 74(4), 383–389.
Colvin, C. J., Konopka, S., Chalker, J. C., Jonas, E., Albertini, J., Amzel, A., et al. (2014). A systematic review of health system barriers and enablers for antiretroviral therapy (ART) for HIV-infected pregnant and postpartum women. PLoS ONE, 9(10), e108150.
Dapaah, J. M., & Senah, K. A. (2016). HIV/AIDS clients, privacy and confidentiality; the case of two health centres in the Ashanti Region of Ghana. BMC Medical Ethics, 17(1), 41.
El-Sadr, W. M., Donnell, D., Beauchamp, G., Hall, H. I., Torian, L. V., Zingman, B., et al. (2017). Financial incentives for linkage to care and viral suppression among HIV-positive patients. JAMA Internal Medicine, 177(8), 1083–1092.
Fox, M. P., Bor, J., Brennan, A. T., MacLeod, W. B., Maskew, M., Stevens, W. S., et al. (2018). Estimating retention in HIV care accounting for patient transfers: A national laboratory cohort study in South Africa. PLoS Medicine, 15(6), e1002589.
Geldsetzer, P., Yapa, H. M. N., Vaikath, M., Ogbuoji, O., Fox, M. P., Essajee, S. M., et al. (2016). A systematic review of interventions to improve postpartum retention of women in PMTCT and ART care. Journal of the International AIDS Society, 19(1), 20679.
Geng, E. H., Glidden, D. V., Emenyonu, N., Musinguzi, N., Bwana, M. B., Neilands, T. B., et al. (2010). Tracking a sample of patients lost to follow-up has a major impact on understanding determinants of survival in HIV-infected patients on antiretroviral therapy in Africa. Tropical Medicine and International Health, 15(Suppl 1), 63–69.
Gourlay, A., Birdthistle, I., Mburu, G., Iorpenda, K., & Wringe, A. (2013). Barriers and facilitating factors to the uptake of antiretroviral drugs for prevention of mother-to-child transmission of HIV in sub-Saharan Africa: A systematic review. Journal of the International AIDS Society, 16(1), 18588.
Govindasamy, D., Ford, N., & Kranzer, K. (2012). Risk factors, barriers and facilitators for linkage to antiretroviral therapy care: A systematic review. AIDS, 26(16), 2059–2067.
Greene, E., Pack, A., Stanton, J., Shelus, V., Tolley, E. E., Taylor, J., et al. (2017). It makes you feel like someone cares; acceptability of a financial incentive intervention for HIV viral suppression in the HPTN 065 (TLC-Plus) study. PLoS ONE, 12(2), e0170686.
Haas, A. D., Tenthani, L., Msukwa, M. T., Tal, K., Jahn, A., Gadabu, O. J., et al. (2016). Retention in care during the first 3 years of antiretroviral therapy for women in Malawi’s option B+ programme: An observational cohort study. The Lancet HIV, 3(4), e175–e182.
Hodgson, I., Plummer, M. L., Konopka, S. N., Colvin, C. J., Jonas, E., Albertini, J., et al. (2014). A systematic review of individual and contextual factors affecting ART initiation, adherence, and retention for HIV-infected pregnant and postpartum women. PLoS ONE, 9(11), e111421.
Joint United Nations Programme on HIV/AIDS (UNAIDS). (2016a). On the Fast-track to an AIDS-free Generation. Geneva.
Joint United Nations Programme on HIV/AIDS (UNAIDS). (2016b). Prevention Gap Report. Geneva.
Kemp, C. G., Weiner, B. J., Sherr, K. H., Kupfer, L. E., Cherutich, P. K., Wilson, D., et al. (2018). Implementation science for integration of HIV and non-communicable disease services in sub-Saharan Africa. AIDS, 32, S93–S105.
Knettel, B. A., Cichowitz, C., Ngocho, J. S., Knippler, E. T., Chumba, L. N., Mmbaga, B. T., et al. (2018). Retention in HIV care during pregnancy and the postpartum period in the option B+ era. Journal of Acquired Immune Deficiency Syndromes, 77(5), 427–438. https://doi.org/10.1097/QAI.0000000000001616.
Kohler, P. K., Ondenge, K., Mills, L. A., Okanda, J., Kinuthia, J., Olilo, G., et al. (2014). Shame, guilt, and stress: Community perceptions of barriers to engaging in prevention of mother to child transmission (PMTCT) programs in western Kenya. AIDS Patient Care and STDs, 28(12), 643–651.
Linnemayr, S., Stecher, C., & Mukasa, B. (2017). Behavioral economic incentives to improve adherence to antiretroviral medication. AIDS, 31(5), 719–726.
MacPhail, C., Adato, M., Kahn, K., Selin, A., Twine, R., Khoza, S., et al. (2013). Acceptability and feasibility of cash transfers for HIV prevention among adolescent South African women. AIDS and Behavior, 17(7), 2301–2312.
Maughan-Brown, B., Smith, P., Kuo, C., Harrison, A., Lurie, M. N., Bekker, L.-G., et al. (2018). A conditional economic incentive fails to improve linkage to care and antiretroviral therapy initiation among HIV-positive adults in Cape Town, South Africa. AIDS Patient Care and STDs, 32(2), 70–78.
Merten, S., Kenter, E., McKenzie, O., Musheke, M., Ntalasha, H., & Martin-Hilber, A. (2010). Patient-reported barriers and drivers of adherence to antiretrovirals in sub-Saharan Africa: A meta-ethnography. Tropical Medicine and International Health, 15(Suppl 1), 16–33.
Mills, E. J., Nachega, J. B., Bangsberg, D. R., Singh, S., Rachlis, B., Wu, P., et al. (2006). Adherence to HAART: A systematic review of developed and developing nation patient-reported barriers and facilitators. PLoS Medicine, 3(11), e438.
Musoke, P., Gakumo, C. A., Abuogi, L. L., Akama, E., Bukusi, E., Helova, A., et al. (2018). A text messaging intervention to support option B+ in kenya: A qualitative study. Journal of the Association of Nurses in AIDS Care, 29(2), 287–299.
Myer, L., & Phillips, T. K. (2017). Beyond “Option B+”. Journal of Acquired Immune Deficiency Syndromes, 75, S115–S122.
Myer, L., Phillips, T. K., Zerbe, A., Ronan, A., Hsiao, N.-Y., Mellins, C. A., et al. (2016). Optimizing antiretroviral therapy (art) for maternal and child health (MCH). JAIDS Journal of Acquired Immune Deficiency Syndromes, 72(Suppl 2), S189–S196.
Nachega, J., Skinner, D., Jennings, L., Magidson, J., Altice, F., Burke, J., et al. (2016). Acceptability and feasibility of mHealth and community-based directly observed antiretroviral therapy to prevent mother-to-child HIV transmission in South African pregnant women under Option B+ : An exploratory study. Patient Preference and Adherence, 10, 683.
Phillips, T. K., Clouse, K., Zerbe, A., Orrell, C., Abrams, E. J., & Myer, L. (2018). Linkage to care, mobility and retention of HIV-positive postpartum women in antiretroviral therapy services in South Africa. Journal of the International AIDS Society, 21 e25114.
Phillips, T. K., McNairy, M. L., Zerbe, A., Myer, L., & Abrams, E. J. (2015). Implementation and operational research: postpartum transfer of care among HIV-infected women initiating antiretroviral therapy during pregnancy. Journal of Acquired Immune Deficiency Syndromes, 70(3), e102–e109.
Phillips, T. K., Thebus, E., Bekker, L.-G., Mcintyre, J., Abrams, E. J., & Myer, L. (2014). Disengagement of HIV-positive pregnant and postpartum women from antiretroviral therapy services: A cohort study. Journal of the International AIDS Society, 17, 19242.
Posse, M., Meheus, F., van Asten, H., van der Ven, A., & Baltussen, R. (2008). Barriers to access to antiretroviral treatment in developing countries: A review. Tropical Medicine and International Health, 13(7), 904–913.
Ronen, K., Unger, J. A., Drake, A. L., Perrier, T., Akinyi, P., Osborn, L., et al. (2018). SMS messaging to improve ART adherence: perspectives of pregnant HIV-infected women in Kenya on HIV-related message content. AIDS Care, 30(4), 500–505.
Schwartz, S. R., Clouse, K., Yende, N., Van Rie, A., Bassett, J., Ratshefola, M., et al. (2015). Acceptability and feasibility of a mobile phone-based case management intervention to retain mothers and infants from an option B+ program in postpartum HIV care. Maternal and Child Health Journal, 19(9), 2029–2037.
Serwaa-Bonsu, A., Herbst, A. J., Reniers, G., Ijaa, W., Clark, B., Kabudula, C., et al. (2010). First experiences in the implementation of biometric technology to link data from Health and Demographic Surveillance Systems with health facility data. Global Health Action, 3(1), 2120.
Shubber, Z., Mills, E. J., Nachega, J. B., Vreeman, R., Freitas, M., Bock, P., et al. (2016). Patient-reported barriers to adherence to antiretroviral therapy: A systematic review and meta-analysis. PLoS Medicine, 13(11), e1002183.
Sibanda, E. L., Tumushime, M., Mufuka, J., Mavedzenge, S. N., Gudukeya, S., Bautista-Arredondo, S., et al. (2017). Effect of non-monetary incentives on uptake of couples’ counselling and testing among clients attending mobile HIV services in rural Zimbabwe: A cluster-randomised trial. The Lancet Global Health, 5(9), e907–e915.
Sikombe, K., Kadota, J. L., Simbeza, S., Eshun-Wilson, I., Beres, L., Moore, C. B., Geng, E. H. (2018). Understanding patient mobility in HIV-positive adults across multiple clinics in Zambia. In Conference on Retroviruses and Opportunistic Infections. Boston, MA.
Sindelar, J. L. (2008). Paying for performance: the power of incentives over habits. Health Economics, 17(4), 449–451.
Stern, E., Colvin, C., Gxabagxaba, N., Schutz, C., Burton, R., & Meintjes, G. (2017). Conceptions of agency and constraint for HIV-positive patients and healthcare workers to support long-term engagement with antiretroviral therapy care in Khayelitsha, South Africa. African Journal of AIDS Research, 16(1), 19–29.
Tolley, E. E., Taylor, J., Pack, A., Greene, E., Stanton, J., Shelus, V., et al. (2018). The role of financial incentives along the antiretroviral therapy adherence continuum: A qualitative sub-study of the HPTN 065 (TLC-Plus) study. AIDS and Behavior, 22(1), 245–257.
Tong, A., Sainsbury, P., & Craig, J. (2007). Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. International Journal for Quality in Health Care, 19(6), 349–357.
Venables, E., Edwards, J. K., Baert, S., Etienne, W., Khabala, K., & Bygrave, H. (2016). They just come, pick and go. The acceptability of integrated medication adherence clubs for HIV and non communicable disease (ncd) patients in Kibera, Kenya. PloS ONE, 11(10), e0164634.
Wall, K. M., Kilembe, W., Inambao, M., Chen, Y. N., Mchoongo, M., Kimaru, L., et al. (2015). Implementation of an electronic fingerprint-linked data collection system: A feasibility and acceptability study among Zambian female sex workers. Global Health, 11(1), 27.
World Health Organization. (2015). Guideline on when to start antiretroviral therapy and on pre-exposure prophylaxis for HIV. Geneva
Yotebieng, M., Thirumurthy, H., Moracco, K. E., Edmonds, A., Tabala, M., Kawende, B., et al. (2016). Conditional cash transfers to increase retention in PMTCT Care, Antiretroviral adherence, and postpartum virological suppression. Journal of Acquired Immune Deficiency Syndromes, 72 S124–S129.
Acknowledgments
We would like to acknowledge the contributions of the study participants and study site staff, without whom this research would not have been possible. This publication is based on research that has been supported in part by the University of Cape Town’s Research Committee (URC).
Funding
This work was supported by the US National Institutes of Health under grant K01 MH107256 (Clouse, PI) and grant UL1TR002243 to the Vanderbilt CTSA. This content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH or the US Government.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Phillips, T.K., Bonnet, K., Myer, L. et al. Acceptability of Interventions to Improve Engagement in HIV Care Among Pregnant and Postpartum Women at Two Urban Clinics in South Africa. Matern Child Health J 23, 1260–1270 (2019). https://doi.org/10.1007/s10995-019-02766-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-019-02766-9